* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Indication
Neuropsychopharmacology wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Drug discovery wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Pharmacognosy wikipedia , lookup
Prescription costs wikipedia , lookup
Psychopharmacology wikipedia , lookup
Drug interaction wikipedia , lookup
Ciprofloxacin wikipedia , lookup
Discovery and development of cephalosporins wikipedia , lookup
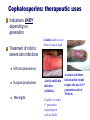
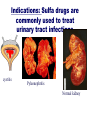
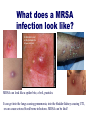
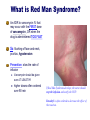
Antibiotics: Part II Introduction to Antibiotics: Part II • Cephalosporins 1st generation 2nd generation 3rd generation 4th generation Sulfonamides Lincosamides Aminoglycosides Fluroquinolones Oxazolodinoes Miscellaneous Vancomycin Metronidazole Drugs to Know Cephalosporins Sulfonamides Lincosamides Aminoglycosides Narrow spectrum Narrow spectrum Antibacterial & antiprotozoa Very potent Serious SE! clindamycin (Cleocin) po, IV Neomycycin Effective against bacteria AND protozoa amikacin (Amikin) IV beta lactam abx 4 generations cephalexin (Keflex) PO 1st trimethoprim + sulfisoxazole (TMP/SMP, Bactrim) po cefazolin Ancef IV 1st garamycin/Gentamicin cefuroxime Ceftin PO 2nd cefoxitin Mefoxin IM/IV 2nd cefixime Suprax PO 3rd cefitraxone Rocephin IM/IV 3rd cefepime Maxipime IV 4th NARROW THERAPEUTIC INDEX ` More Drugs to Know Fluoroquinolones Oxazolidinones Misc Agents ciprofloxacin (Cipro) IV/PO linezolid (Zyvox) vancomycin (Vancocin) levofloxacin (Levaquin) IV/PO IV / PO Considered the “last line drug” IV/po Formerly the “last line drug” Requires ‘peak & trough’ levels metronidazole (Flagyl) IV/PO Abx and antiparasitic CEPHALOSPORINS The cephalosporins are divided into four generations which progressively become broader spectrum Look for “cef” prefix Like penicillins, many cephalosporins have a beta-lactam structure The first generations of cephalosporins are sensitive to betalactamase producing bacteria Thus, these drugs are RENDERED INEFFECTIVE by bacteria that produce betalactamase Adverse Reactions: Cephalosporins (all generations) Low toxicity, well tolerated Adverse Reactions Hypersensitivity (similar Increased bleeding by interfering with vitamin K metabolism. Monitor PT/INR may occur up to 72H after last dose (delayed reaction) to and 10% cross-reactive with penicillin hypersensitivity) *GI (N-V-D) ANTABUSE EFFECT (interaction with ETOH) Nephrotoxicity Adverse reactions Prolonged use may cause a superinfection What is the Antabuse Effect? disulfiram/Antabuse Is a drug that increases the sensitivity to alcohol Discovered in the 1920’s Used to support the treatment of chronic alcoholism Blocks the processing of alcohol in the body by inhibiting acetaldehyde dehydrogenase Causes INTENSE negative effects of alcohol N/V, H/A, dizziness Some drugs (cephalosporins and Flagyl) may cause this same effect when taken with ETOH Cephalosporins: therapeutic uses Indications VARY depending on generation Treatment of mild to severe skin infections Cellulitis–mild to severe Often d/t strep or staph URI and pneumonia Surgical prophylaxis Meningitis A fairly mild skin infection (cellulitus) Could be tx with a 1st generation cephalosporin such as Keflex A serious soft tissue infection that would require the use of 2nd generation such of Mefoxin 1st Generation Cephaloporins 1st generation NARROW SPECTRUM Good gram (+) coverage. Poor gram (-) coverage MINIMALLY effective against betalactamase producing bacteria Indications: Used to treat UTIs, SIMPLE skin infections, strep throat Can be used for surgical prophylaxis ALTERNATIVE TO PENICILLIN (mild allergy only) for staph and strep infections (Keflex) cefazolin sodium (Ancef) PO: cephalexin IM/IV: 2nd Generation Cephalosporons 2nd generation BROADER SPECTRUM good gram (+) AND good gram (-) coverage But limited application b/c NOT effective against betalactamase producing bacteria Indications: Used to treat septicemia, bone and joint infections, and respiratory infections PO: cefuroxime (Ceftin) otitis, sinusitis, and respiratory tract infections IM/IV: cefoxitin sodium (Mefoxin) infections abdominal and pelvic 3rd Generation Cephalosporins 3rd generation: NARROW spectrum Good for gram (-) infections only nosocomial infections mostly d/t gram (-) infections able to penetrate the CSF (meninigitis) MINIMALLY effective against beta-lactamase bacteria DOES CROSS BLOOD BRAIN BARRIER!! PO: cefixime (Suprax) IM/IV: ceftriaxone (Rocephin) Rocephin has a long half life and can be given once or twice a day 4th generation Cephalosprins 4th generation: BROADEST spectrum Effective against MOST gram (+) and gram AND… Able to resist MOST beta-lactamase producing bacteria CROSSES BLOOD BRAIN BARRIER!! Is effective against MRSA and enterobacter IM/IV: cefepime (Maxipime) IV SULFONAMIDES Indications: Sulfonamides are commonly Rx for UTIs MOA - inhibit the synthesis of folic acid Achieve high concentration in the KIDNEYS (UTI’s) May be used as an alternative for clients allergic to penicillin Bacteria use folic acid to synthesize their DNA Indications: Sulfa drugs are commonly used to treat urinary tract infections cystitis Pyleonephritis Normal kidney Sulfonamides Indications: Narrow spectrum Most common – UTI’s and Chlamydia, pneumocytis carinii pneumonia, rheumatic fever Caution: cross sensitivity with THIAZIDES and SULFONYLUREAS **Patient allergic to sulfa antibiotics may also be allergic to thiazides and/or diabetic sulfa containing drugs Sulfonamides Common drugs: Trimethomprim Bacteriostatic when used alone Commonly used WITH SULFA for synergistic effect rendering them bacterocidal * trimethroprim + sulfisoxazole (Septra , Bactrim) (TMP/SMP) SULFONAMIDES Adverse Effects *Anorexia, N-V-D photosensitivity Crystalluria (kidney stones can form) Interactions: displaces protein bound anticoagulants clotting times (PTINR) toxic to the kidney (need to drink lots!) Bone marrow suppression, hemolytic anemia Renal failure Skin rashes Hypersensitivity – vascular lesions, rash, eruptions, drug fever Encourage lots of water Sulfa drugs can be toxic to the kidney. Lincosamide clindamycin/Cleocin is effective against BOTH bacteria and PROTOZOA such as trichomoniasis Indications: Used to tx diseases of the skin, vagina, resp tract and abdomen Is effective against skin infections d/t MRSA! Is a powerful inhibitor of toxin synthesis Often used WITH a bacteriocidal agent As the bacteriocidal agent and toxins are released the clindamycin inhibits the toxin formation SE: Frequently causes C. diff colitis!! Lincosamides MOA: inhibits bacterial protein synthesis Bacterostatic at low doses and bacterocidal at higher doses clindamycin (Cleocin) NARROW SPECTRUM Indications: Used to treat gram (+) infection, including staph, and anaerobic organisms SE: *N-V-D Rash Colitis (c dif) and anaphylactic shock What does a MRSA infection look like? MRSA can look like a spider bite, a boil, pustules. It can get into the lungs causing pneumonia, into the bladder/kidney causing UTI, or can cause serious blood borne infections. MRSA can be fatal! AMINOGLYCOSIDES Destroy bacteriatrue bactericidal agents IV only Cannot be given po d/t poor absorption Indications: Used to treat SERIOUS INFECTIONS d/t aerobic bacilli and gram (-) organisms *Very potent and capable of serious side effects!! Nursing Alert: Do not mix in the same container with penicillins and cephalosporins Aminoglycosides MOA: Inhibits bacterial protein synthesis Bactericidal NARROW SPECTRUM Only active against gram (-) bacteria Pseudomonas Indication: Primarily used in nosocomial infections Aminoglycosides (cont) Do not penetrate CSF Cross the blood brain barrier in children but not adults Excreted RENALLY by glomerular filtration **Narrow therapeutic index drug** *Requires constant monitoring “PEAK/TROUGH LEVELS” What is a Peak and Trough level? PEAK = greatest concentration of the drug in the BLOOD (30 min AFTER infusion) TROUGH = greatest concentration of the drug in the TISSUE (30 min PRIOR to next infusion) Therapeutic levels are desired Risk for serious SE increases with high trough levels High trough levels? – the next dose may be held and peak and trough repeated Aminogylcosides Potential Serious Adverse Effects Ototoxicity – vestibular and auditory may be irreversible Nephrotoxicity – potentially reversible BUN & Creatinine Both toxicities dependent on HIGH “TROUGH” LEVELS Aminoglycosides *gentamicin sulfate (Garamycin) – available in topical, opthalmic, and IV forms amikacin (Amikin): (IV only) – often used to rx infections resistant to gentamicin, little resistance so far to Amikin neomycin (Mycifradin) – a milder aminoglycoside Indications: suppress GI bacteria pre-op (colon surgery) a topical agent to treat wound infections Pseudomonas infection: serious infections Pseudomonas infections are resistant to many antibiotics Quinolones/Fluoroquinolones MOA: interfere with bacterial DNA Bacteriocidal Quinolones developed first Have a narrow spectrum Seldom used today Fluoroquinolones developed by adding a fluorine atom to basic quinolone structure BROADER SPECTRUM What infections are floroquinolones commonly prescribed for? Indications: Many gram (-), some anerobes, atypicals Good for people allergic to erythromycin (EES) UTIs, bone and joint infections, bronchitis, pneumonia, gonorrhea Enterobacter, Pseudomonas, MRSA Now seeing FQRP (fluoquinolone resistant pseudomonas) Accumulates well in urine and prostate Florquinolones Adverse Effects: Both serious and bothersome: N-V-D, dyspepsia H/a, dizziness, rashes Hepatotoxicity (LFTs) Drug Interactions Can inhibit theophylline and warfarin metabolism increasing the levels of these drugs Fluoroquinolones Look for “floxacin” suffix Common drugs *ciprofloxacin (Cipro) PO and IV levofloxacin (Levaquin) PO and IV ** NURSING ALERT** IV Levaquin is sensitive to light and will break down if exposed to light use a brown plastic bag to cover IVPB What is the hype about Vancomycin? NARROW SPECTRUM GM (+) Vancomycin is used IV to treat serious infections (MRSA) and Enterococci Vancocin is used po to treat C. difficile colitis Was previously considered the LAST RESORT DRUG Resistance is now being noted to infections caused by Enterococcus (VRE) and staph aureus (VRSA) Super Bug is resistant to Vancomycin Miscellaneous Agent: Vancomycin vancomycin IV (Vancocin) PO A glycopeptide antibiotic structurally different from other available antibiotics SE: (potential and serious) Petechiae and Thrombocytopenia Ototoxicity and nephrotoxicity Peak and trough levels periodically monitored Rapid IV administration can cause “RED SYNDROME” MAN What is Red Man Syndrome? An ADR to vancomycin IV that may occur with the FIRST dose of vancomycin ,OR when the drug is administered TOO FAST Sx: flushing of face and neck, pruritus, hypotension Prevention: slow the rate of infusion Vancomycin should be given over AT LEAST lH higher doses often ordered over 90 min If Red Man Syndrome develops, the nurse should stop the infusion and notify the HCP. Benadryl is often ordered to decrease the effect of the reaction. Vancomycin Resistance Enterococci (VRE) Oxazolidinones Newer class of antibiotic Indication: Developed in 1999 primarily to treat vancomycin -resistant enterococcus (VRE) Enterococci is a gram (+) bacterium in our GI tract that can be highly aggressive , esp in post-op pts Enterococci causes UTI, septicemia, endocarditis and infects wounds Oxazolidinones are also used to treat infections d/t MRSA Is now considered “THE LAST LINE ANTIBIOTIC” Oxazolidinones linezolid (Zyvox) (po,IV) Inhibits bacterial protein synthesis New “Last line drug” Adverse effects: *Pseudomembranous colitis (C. Difficile colitis) Misc Antibiotic: metronidazole/Flagyl Flagyl is considered both an ANTIBIOTIC and an Anti-parasitic agent Indications: Flagyl is commonly prescribed to treat infections d/t anaerobic bacteria and some protozoa Also, commonly used for abdominal and pelvic infections; as well as liver abcess More Indications: metronidazole/Flagyl Indication: Flagyl is also the first line treatment for C. diff colitis an anerobic bacteria that causes profuse diarrhea in some patients who take certain antibiotics Adverse Reactions: Generally well tolerated Antabuse effect may occur if ETOH consumed while taking Flagyl.