* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The effect of Steroids in DBA
Blood donation wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Autotransfusion wikipedia , lookup
Hemolytic-uremic syndrome wikipedia , lookup
Plateletpheresis wikipedia , lookup
Men who have sex with men blood donor controversy wikipedia , lookup
Jehovah's Witnesses and blood transfusions wikipedia , lookup
Hemorheology wikipedia , lookup
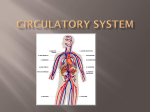
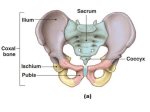
Investigation of blood cell production and the effect of steroids in Diamond-Blackfan Anaemia Deena Iskander, Clinical Research Fellow Centre for Haematology, Faculty of Medicine, Hammersmith Hospital, Imperial College London Paediatric Haematology and Bone Marrow Transplantation Unit, St Mary’s Hospital, Imperial College Healthcare NHS Trust, London, UK Imperial Molecular Pathology Laboratory, Hammersmith Hospital, Imperial College Healthcare Trust DBA Family Weekend, May 2016 Plan • • • • • • Background to project Aims Experimental design Results Conclusions Further work Diamond-Blackfan Anaemia Inherited bone marrow failure disease 5-10 per million babies born Low haemoglobin: ANAEMIA requiring blood transfusions Other blood count abnormalities e.g. low white blood cell count Physical changes arising at birth e.g. heart problems, kidney problems, joint problems Problems developing throughout life e.g. slow growth, infections Vlachos A et al. Expert Rev Hematol, 2014 Narla A & Ebert B, Blood 2010 DBA is a caused by a change in the genetic code -a ‘mutation’- that leads to half the normal amount of one ribosomal protein Small ribosomal subunit Large ribosomal subunit Slavov et al Cell Reports 2015 Mutation inherited from one parent in 35% patients and arises ‘out of the blue’ in 65% The same mutation can cause different effects in different people dad 11y son Preterm birth with poor growth and low birth weight Diagnosed at birth (mother known to have DBA) RPL11 mutation Transfusions needed for first few years Steroids aged 5y– initial response but loss of response by 10y Second steroid trial no response Resistant to steroids mum 30y old mum Diagnosed aged 7y RPL11 mutation Blood transfusions needed in pregnancy Treated with steroids Responsive to steroids- no further blood transfusions needed Some of family details changed DBA is characterised by absent or reduced red blood cell precursors in the bone marrow Non-DBA child BM DBA BM How red blood cells develop in the bone marrow Red blood cell ‘parents’ Red blood cell precursor Red blood cells Stem cells What is the identity of the ‘parents’/progenitors of red cells in humans? ‘Invisible’ Bone marrow Blood Different blood cell defects are implicated in DBA • Absent progenitors in 7 relapsed patients with DBA (Nathan D JCI 1978) • Normal progenitor numbers with impaired development of progenitors to red blood cells (Lipton J et al Blood 1989) What is the origin of red blood cell failure in DBA? Management of DBA Diagnosis Steroid responsive 80% Dose weaned/stopped Steroid resistant 20% Steroid resistant 40% Prednisolone steroid tablets - high dose Blood transfusions /Bone marrow transplantation Ultimately only 40% patients can use steroids in the long-term How do steroids work in DBA? • Act directly on DNA • Increase haemoglobin • Increase the number of times that red blood cell progenitors divide, leading to more and more red blood cells How do steroids affect red blood cell progenitors in DBA? Aims 1 a) Define the identities of red blood cell progenitors in human bone marrow b) Describe early blood cell development in DBA 2 Understand how steroids improve anaemia in DBA by studying the cells and genes that are affected by steroids in human red blood cell progenitors Experimental design Bone marrow from patients with DBA and healthy children after consent Isolation of cells of interest Looing at the cells directly isolated from bone marrow Growing the cells in a ‘soup’ that promotes red blood cell development Samples labelled anonymously once they arrive in the lab Clinical information accompanying each sample stored confidentially Investigation of - the markers on the outside of red blood cell progenitor populations - How the cells grow - What genes the cells express Patients with DBA compared with healthy children Non-DBA (18 people) DBA (15 people) Average age (range) 6y7m (1y6m-43y) 6y (10m-17y) Reason for bone marrow Donating their bone marrow for a bone marrow transplant 13 for follow-up, 1 for low blood counts, 1 for diagnosis of DBA Treatment NA 10 on regular blood transfusions (2 steroids not yet tried, 8 resistant to steroid) 5 steroid responsive Diagnosis of DBA by DNA sequencing Not detected RPS19 RPL5 RPS26 RPS24 RPL11 RPL35a RPS7 RPL15 RPS29 RPS10 RPS17 RPS15 RPL36 Under investigation A ribosomal protein mutation likely to be causing DBA has been identified by sequencing in 69% (68/99) patients tested. 1 Gerrard G, Valgañón M, En Foong H et al. British Journal Haematol. 2013 Results Aim 1a: What is the identity of the ‘parents’/progenitors of red cells? Characterisation of red blood cell progenitors using protein labels on their surface Early red cell progenitors Late red cell progenitors x10 x10 A B Hypotheses: A cells are early red blood cell progenitors B cells are late red blood cell progenitors Iskander D et al, Blood, 2015 Indeed we found that these newly defined progenitors look different….. Sorted A EEP Sorted B LEP 50mm …..and express different genes GATA-1 GATA-2 Gene expression relative to GAPDH 100 80 60 40 20 5 4 3 2 1 0 2.0 1.5 1.0 0.5 G M P EB P B LE P A EE EP M G M P EB P B LE P A EE EP 0.0 M Gene expression relative to GAPDH P G M EB P B LE P A EE EP M Gene expression relative to GAPDH CD36 500 400 300 200 100 20 15 10 5 0 N=3 Iskander D et al, Blood, 2015 Conclusions I: Normal blood cell production We have identified the early and late red blood cell progenitor populations in the bone marrow of healthy children. The same populations were also found in adult bone marrow. The above findings have since been corroborated by other groups. (Mori Y, PNAS, 2015) This is important because it means we can capture these cells from human bone marrow samples and study them in health and diseases, which should lead to understanding these diseases better. Results II Aim 1b: Describe early blood cell development in DBA Aim 2: Understand how steroids improve anaemia in DBA DBA progenitors do not grow normally Non-DBA x10 No. colonies/100 cells 60 * 50 40 30 BFU-E CFU-E CFU-G/M/GM Erythroid clusters Erythroid clusters DBA 20 10 x20 0 CON DBA CON DBA CON DBA CMP MEP GMP N=4 CON N=5 DBA Iskander D et al, Blood, 2015 Transfusion-dependent (TD) versus steroid-responsive (SR) patients DBA TD CON NON-DBA CD71 10 5 10 4 10 3 10 2 DBA SR 5 10 78.8% 90.7% 9.48% 104 3 10 102 0 0 0 10 3 10 4 CD41a CD105 10 10 5 5 10 4 10 3 0 10 LEP 0.9% EEP 2.8% 10 2 0 0 10 3 10 4 5 104 105 5 10 4 10 3 10 2 LEP 1.7% LEP 0.0% EEP 6.9% EEP 0.7% 0 10 103 0 10 3 10 4 10 5 CD36 Iskander D et al, Blood, 2015 Conclusions II: DBA blood cell production • In transfusion-dependent DBA – There are fewer red blood cell progenitors and they don’t work normally • Red blood cell progenitor abnormalities are restored in steroid-responsive DBA Summary of progress and future work We have identified the early and late red blood cell progenitor populations in the bone marrow of healthy children. We have used these definitions to identify the places in red cell production where things are going wrong in DBA. We will continue to study these cells with the aim of identifying why things go wrong in DBA and how steroids can help. The overall aim of this work is to find new approaches and gene targets that we can use to treat DBA. Acknowledgements Tassos Karadimitris Irene Roberts Josu de la Fuente Beth Psaila, Valentina Caputo, Aris Chaidos, Katerina Goudevenou, Andi Roy Qais Al-Oqaily, Neha Bhatnagar, Joana Costa, Maialen Lasa, Kalliopi Makarona, David O’Connor, Kyriake Petivi, Kanagaraju Ponnusamy, Antonella Rotolo, Nikolaos Trasanidis Mauritius Kleijnen, David Pitcher Holger Auner, Sandra Loaiza, Katarzyna Parzych Niklas Feldhahn, Bryant Boulianne Paediatric Haematology team, St Mary’s Hospital Yvonne Harrington, SpRs Mark Layton, Hammersmith Hospital The patients and their familiesAll of you! NIHR BRC Imaging and FACS Facility, Imperial College John Goldman Centre for Cellular Therapy Imperial Molecular Pathology lab Letizia Foroni, Jamshid Khorashad, Gareth Gerrard, Hui en Foong , Sandra Hing