* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download DRUG - ichapps.com
Survey
Document related concepts
Orphan drug wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Plateau principle wikipedia , lookup
Compounding wikipedia , lookup
Psychopharmacology wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Theralizumab wikipedia , lookup
Drug design wikipedia , lookup
Pharmacognosy wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Prescription costs wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug discovery wikipedia , lookup
Transcript
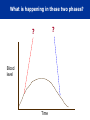
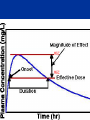
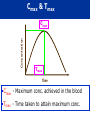
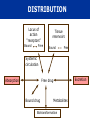
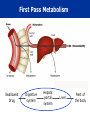
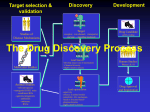
Let’s learn PHARMACOLOGY PHARMACOLOGY Greek Word Pharmacon Drug Logos Science Science of drugs- dealing with the study of Desirable and Undesirable effects. Pharmacology is the study of drugs and their actions on the body What is PHARMACOLOGY ? Pharmacokinetics What the body does to drug Pharmacodynamics What the drug does to body Pharmacology Pharmacotherapeutics The study of the use of drugs Pharmacy Preparing suitable dosage forms Toxicology PHARMACY It is the science of: •Identification •Selection •Preservation •Standardization •Compounding, •Dispensing and of medicinal substances PHARMACOPOEIA • It is an official code containing a selected list of the established drugs and medicinal preparations physical with properties descriptions and tests identity, purity and potency. USP, etc. IP: Indian Pharmacopoeia BP: British Pharmacopoeia USP: United states Pharmacopoeia of their for their e.g. IP, BP, DRUG “ Drug is any substance or product that is used or is intended to be used to modify physiological systems or pathological states for the benefit of the recipient .” “Poisons in small doses are the best medicines; and useful medicines in too large doses are poisonous” William Withering 1789 DRUG NAMES • Chemical…states its chemical composition and molecular structure. • Generic…usually manufacturer. suggested • Official…as listed (I.P., B.P., U.S.P.) in the by the Pharmacopoeia. • Brand…the trade or proprietary name. DRUG NAMES Chemical Name 1,4 benzodiazepine analog Generic Name Alprazolam Official Name Alprazolam, USP Brand Name Alprax® THE NATURE AND SOURCES OF DRUGS • Mineral • Liquid paraffin, magnesium sulfate, etc • Animal • Insulin, Thyroid, etc. • Plant • Morphine, Quinine etc • Synthetic • Aspirin, Sulfonamides, etc. • Micro-organisms • Penicillin & other antibiotics. • Drugs produced by genetic engineering • Human insulin, human growth, hormone etc. DRUG DEVELOPMENT PROCESS Chemistry Synthesis & Purification Formulation Animal Pharmacology Animal Toxicity (Short / Long term) Studies in Humans Drug Authorities Market DRUG DEVELOPMENT PROCESS DOSE Vs DOSAGE • Dose: The quantity of drug administered at one time • 500mg of Paracetamol • Dosage: The amount of the drug that should be given over time • 500 mg Paracetamol TID for 3 days DRUG DOSAGE FORMS Tablets Capsule Aerosol Injection Suspension Infusion Cream Solution ROUTES OF DRUG ADMINISTRATION How the drug is given Enteral 1. Oral 2. Sublingual 3. Rectal Parenteral (injectable) 1. Intravenous 2. Intramuscular 3. Subcutaneous Topical 1. Intranasal 2. Inhalation 3. Intravaginal PHARMACOKINETICS • The study of what the body does to the drug • It is the study of absorption, distribution, metabolism and excretion (ADME) of drugs • “Fate of drug” PHARMACOKINETICS •Absorption How the drug is moved into blood stream from the site of administration ? • Distribution How much drug is moved to various body Depends on blood flow through tissue tissues / organs ? • Metabolism How the drug is altered – broken down ? • Excretion How much of the drug is removed from the body ? ABSORPTION Site of Administration DRUG Vascular System Drug Absorption of Various Dosage Forms Oral Preparations Liquids, elixirs, syrups Suspension solutions Powders Capsules Tablets Coated tablets Enteric-coated tablets Fastest Slowest IV Route What would the graph of blood level against time look like? Blood level Time ORAL Route What would the graph of blood level against time look like? Blood level Time What is happening in these two phases? ? ? Blood level Time Absorption and Distribution Metabolism and Excretion Blood level Time BIOAVAILABILITY • Bioavailability is a fraction of administered dose of a drug that reaches the systemic circulation in the unchanged form. • Bioavailability of IV route : 100 % BIOAVAILABILITY Destroyed in gut Dose Not absorbed Destroyed Destroyed by gut wall by liver to systemic circulation BIOAVAILABILITY Factors influencing bioavailability • Dosage forms • Chemical form • Dissolution & Absorption of drug • Route of administration • Presence of food/drugs in GI tract • First pass effect • Extent of drug metabolism before reaching systemic circulation MSC MEC Concept of Critical Threshold • MEC (Minimum Effective Concentration): The minimum level of drug concentration needed for the desired therapeutic effect to be present. • MSC (Maximum Safe Concentration): The maximum level of drug concentration above which toxic effects occurs. OR • MTC (Minimum Toxic Concentration): The minimum level of drug concentration that produces toxic effects. •Maximal Effect: Greatest response that can be produced by a drug, above which no further response can be created (sometimes called “peak effect”) •Onset: How long before a drug is able to exert a therapeutic effect •Duration: How long a drug effect lasts DRUG HALF-LIFE (t1/2 ) • Half life is the time required to reduce the plasma concentration to 50% of its original value • Will determine dosing requirements / how long a drug will remain in the body • Used in determining dosing interval • Goal - Plateau DRUG HALF-LIFE (t1/2 ) 110 100 Concentration (m g/L) 90 80 70 60 50 40 30 20 10 0 0 1 2 3 4 5 6 7 8 9 Tim e (hours) Half-life is the time taken for the concentration of drug in blood to fall by a half Half-life is 2 hrs DRUG HALF-LIFE (t1/2 ) • 1t 1/2 - 50 % drug is eliminated • 2 t1/2 - 50+25 (75 %) drug is eliminated • 3 t1/2 - 50+25 +12.5 (87.5 %) drug is eliminated • 4 t1/2 - 50+25 eliminated +12.5+6.25 (93.7 %) drug is Thus, nearly complete drug elimination occurs in 4-5 half lives. DRUG HALF-LIFE (t1/2 ) 50 25 12.5 6.25 3.12 1.56 Cmax & Tmax Concentration Cmax Tmax Time •Cmax - Maximum conc. achieved in the blood •Tmax - Time taken to attain maximum conc. AUC (Area Under Curve) AUC • AUC is the area under the plot of plasma concentration of drug against time after drug administration. DISTRIBUTION Distribution is a branch of pharmacokinetics which describes the reversible transfer of drug from one location to another within the body. DISTRIBUTION Locus of action “receptors” Bound Tissue reservoirs Free Bound Free Systemic circulation Absorption Free drug Bound drug Metabolites Biotransformation Excretion Excretion Plasma- Protein Binding • Many drugs bound to circulating plasma proteins such as albumin, lipoproteins, glycoprotein, globulins etc. • Free form • Pharmacologically active • Bound form • Pharmacologically inactive Receptor Site Protein-bound drug Free Drug Dosing • Dosing Interval - How often the drug should be given • Loading dose – Which puts the plasma concentration in the therapeutic range • Maintenance dose - Routine smaller doses to maintain the steady state (Plateau) METABOLISM Metabolism = change / biotransformation The conversion from one chemical form to another Site of drug biotransformation • Liver - cytochrome P450 pathways OR microsomal P450 pathways are used to metabolize most agents • Enzymatic alteration of drug structure Effect of metabolism 80% of drugs become inactive Inactive drug becomes active: Prodrug Some drugs do not get metabolised at all METABOLISM Majority of drugs are metabolized in liver by enzymes – Cytochrome P 450 Drugs may induce (activate) or inhibit these enzymes Drug – Drug interactions First Pass Metabolism The first-pass metabolism (also known as first-pass effect or presystemic metabolism) is a phenomenon of drug metabolism whereby the concentration of a drug is greatly reduced before it reaches the systemic circulation. First Pass Metabolism Swallowed Drug Digestive system Hepatic portal system Liver Rest of the body First Pass Metabolism Systems that affect the first pass effect of the drug, • • • • Enzymes of the gastro intestinal lumen Gut wall enzyme Bacterial enzymes Hepatic enzymes First Pass Metabolism Effect of first pass metabolism Part of administered dose made inactive ↓ bioavailability Drug converted into its active form • Nitroglycerin when given orally • Totally inactivated in the liver • 100% first pass effect • Always given sublingually Prodrug Administered After in an inactive form administration converted into their active form usually in liver Designed to improve bioavailability Examples Enalapril – Enalaprilate Ramipril - Ramiprilate METABOLISM Factors affecting metabolism : 1. Age – Children / Elderly 2. Disease condition – e.g. Liver disease 3. Induction of drug metabolizing enzymes 4. First-pass effect – Nitroglycerin 5. Competition between drugs 6. Genetics 7. Environment e.g. Smoking Excretion Drugs &/or its metabolites eliminated from the body • Elimination of the drug • Unchanged (Parent form) • Metabolites • Routes of excretion • Kidneys – Urine • GIT – Stools • Skin - Perspiration • Eyes - Tears are irreversibly PHARMACODYNAMICS • The study of what the drug does to the body • It is the quantitative study of the biological and therapeutic effects of drugs. PHARMACODYNAMICS Drug actions: • The cellular processes involved in the drug and cell interaction Drug effect: • The physiologic reaction of the body to the drug PHARMACODYNAMICS Onset • The time it takes for the drug to elicit a therapeutic response Peak • The time it takes for a drug to reach its maximum therapeutic response Duration • The time a drug concentration is sufficient to elicit therapeutic response Four targets of drug action on cells • Receptors • Ach receptors / Epinephrine receptors • Ion Channels •Voltage gated Na+ / K+ / Ca++ • Enzymes •Cyclooxygenase / Acetylcholine esterase • Carriers •Na+/ K+ pump / Proton Pump Receptors • Specific macromolecular components of the cell which when binds with ligand produces positive or negative biological response • Situated - on the surface / inside the cell • Affinity: Inherent ability of the drug to bind with the receptor • Efficacy (Intrinsic activity): Inherent ability of the drug to induce a physiological response • Potency: An expression of the activity of the drug, in terms of the concentration or amount needed to produce a defined effect What drug can do? All that drugs can do is, • Mimic the physiological activity of the body’s own molecules • Block the physiological body’s own molecules activity of the Drug at Receptor • Agonist : It activates a receptor to produce an effect similar to that of the physiological signal molecule • Antagonist : It prevents the action of an agonist on a receptor but does not have any effect of its own • Partial agonist : It activates a receptor to produce sub maximal effect but antagonizes the action of full agonist. Agonist v/s Antagonist • Drug + Receptor EFFECT • Drug + Receptor Maximum Effect • Drug = complete or full agonist • Drug + Receptor Less than maximal effect • Drug = partial agonist • Drug + Receptor Block effect • Drug = Antagonist Effects of combination of drug • Addition 1+1=2 • Response elicited by combined drugs is equal to the combined response of the individual drugs • Synergism 1+1=3 • Two drugs with the same effect are given together and produce a response greater than the sum of their individual responses Effects of combination of drug • Potentiation 0+1=2 • A drug which has no effect enhances the effect of a second drug • Antagonism 1+1=0 • Drug inhibits the effect of another drug. Usually, the antagonist has no inherent activity Factors affecting drug response • Pharmacological •Dose & Route of administration •Duration of treatment •Co-administration of other drugs • Individual •Age & Weight •Gender •Pathology •Diet Indication & Contraindication • Indication: A clinical circumstance indicating that the use of a particular intervention would be appropriate • Contraindication: Any condition which renders a particular line of treatment improper or undesirable. Adverse drug reaction What does the term adverse reaction refer to? A. A life-threatening response to a drug B. A drug-induced allergy C. A harmful, noxious, unintended & undesirable response to a drug D. An unpredictable response to a drug Adverse drug reactions Side effect Toxicity – overdose Allergic reaction Physical dependence Carcinogenic effect PLACEBO: Drug devoid of intrinsic pharmacological activity and it works by psychological means. USES : ?????? PHASES OF CLINICAL DEVELOPMENT • Phase 1: Clinical pharmacology • Phase 2: Clinical investigation • Phase 3: Formal therapeutic trials • Phase 4: Post licensing (marketing) studies Pregnancy Considerations • Increased maternal HR, CO and blood volume • May affect absorption, distribution, effectiveness • Drugs may cross placenta • Drugs may cross into breast milk • Tertatogens Pregnancy Categories • A: controlled studies in pregnancy (<1 %). • B: animal studies show no risk; Inadequate human data. • C: animal studies show risk, inadequate human data. • D: human data show risk, benefit may outweigh risk. • X: animal or human data positive for risk. Use unwarranted. Pediatric Considerations • Oral absorption • Thinner skin ( topical absorption) • Plasma protein concentration • Free protein-bound drug availability • Extracellular fluid in neonate • Altered metabolic rates • Elimination/metabolism • BSA/weight based dosing important! Geriatric Considerations • Oral absorption • Plasma protein concentration • Muscle mass, body fat • Liver/renal function • Multiple drugs • Multiple diseases FUNDAMENTALS OF PHARMACOLOGY • The rational pharmacological treatment of any patient requires adequate knowledge about : The disease process, Pharmacodynamic properties drug(s) selected, and The individual’s handling [pharmacokinetics]. of the of the drug(s) OPTIMUM DRUG CONCENTRATION • The concentration must not be too low, nor too high. • In the former case, therapeutic failure may occur, while in the later, adverse effects may prove troublesome to the patient. FUNDAMENTALS OF PHARMACOLOGY • Drugs act by affecting biochemical or physiological process in the body. Most drugs act at specific receptors. • The action of a drug is characterized by two variables: The magnitude of the response and The concentration required to produce the response. FUNDAMENTALS OF PHARMACOLOGY • A specific drug acts only at one receptor but may produce multiple effects due to the location of the receptor in various organs. • A selective drug acts on one receptor in a particular tissue at concentrations that produce little effect on the receptor in other organs. • Most drugs have multiple actions and it is usually preferable to use more specific or more selective agents THANK YOU