* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Acute visual loss
Visual impairment wikipedia , lookup
Photoreceptor cell wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
Visual impairment due to intracranial pressure wikipedia , lookup
Diabetic retinopathy wikipedia , lookup
Retinal waves wikipedia , lookup
Macular degeneration wikipedia , lookup
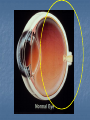
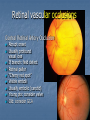
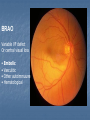
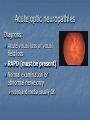
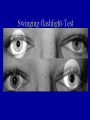
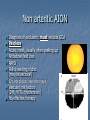
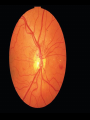
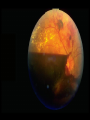
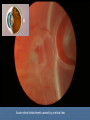
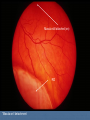
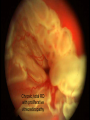
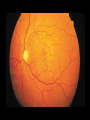
Acute visual loss: Emergency room perspective Dr.Ehud Zamir Acute visual loss Unilateral RETINAL ARTERIAL OCCLUSIONS AION VITREORETINAL Bilateral OPTIC NEURITIS Hemorrhagic AMD TOXIC ISCHEMIC OR OTHER CORTICAL DAMAGE Acute visual loss: history How acute?: seconds/minutes? Hours? Is it really acute? ACUTE VISUAL LOSS UNILATERAL RETINAL ARTERIAL OCCLUSIONS AION VITREORETINAL BILATERAL OPTIC NEURITIS Hemorrhagic AMD TOXIC ISCHEMIC OR OTHER CORTICAL DAMAGE History Associated symptoms Underlying risk factors Flashing lights, floaters, shadow/curtain Jaw claudication, scalp tenderness , temple pain, loss of weight Diplopia , other neurological symptoms Peripheral vascular disease, hypertension, diabetes, cholesterol Known embolic sources Risk factors for retinal detachment: myopia, family history Complete ophthalmic, systemic, family and drug history Acute unilateral visual loss Retinal vascular occlusions Central Retinal Artery Occlusion Abrupt onset Usually profound visual loss If branch: field defect Retinal pallor “Cherry red spot” Visible emboli Usually embolic (carotid) Young pts: consider valve Old: consider GCA BRAO Variable VF defect Or central visual loss • Embolic • Vasculitic • Other autoimmuune • Hematological Examination Generally very poor vision RAPD Retinal whitening and pallor typically less than counting fingers vision severe visual field constriction Compare with the other eye Carotid bruit / murmurs? Temporal artery tenderness Treatment No treatment proven consistently to be of value Theoretically should be given ASAP Irreversible ischaemic damage probably after 90 minutes Modalities: AC paracenthesis Ocular massage Diamox CO2 enriched oxygen (carbogen) Hyperbaric oxygen Selective ophthalmic artery catheterisation, TPA Always consider GCA: Hx, ESR, CRP Acute optic neuropathies Diagnosis: Acute visual loss or visual field loss RAPD (must be present) Normal examination or abnormal nerve only retina and media usually OK Acute optic neuropathy (schematic approach) Old: AION Sick: GCA (arteritic) Young: Optic neuritis Well: Non arteritic (crowded disk) Acute optic neuropathy Young: Optic neuritis Optic neuritis 20-50 years old, more in females Preceded/accompanied by pain on eye movements Dyschromatopsia: red desaturation test RAPD Reduced brightness VF defect VA: ANY Disc: 2/3 are normal (hence retrobulbar ON) or disc swelling. Haemorrhage is atypical. Optic neuritis Diagnosed clinically Most commonly due to demyelination DD: vasculitis, neoplasia, syphilis MRI of prognostic value re: MS Treatment with high dose I.V methylprednisolone has some early benefit 1 gram I.V. per day for 3d, then pred 1mg/kg/day for 11d then 4d taper Oral prednisolone (previously standard Rx) associated with more attacks! Treatment only hastens recovery; has no influence over long-term visual outcome Usually untreated; even after treatment some deficit often remains Acute optic neuropathy (schematic approach) Old: AION 10% Sick, older (>80): GCA (arteritic) 90% Well: Non arteritic Non arteritic AION Diagnosis of exclusion: must exclude GCA Painless Acute onset, usually when waking up Altitudinal field loss RAPD Pallid swelling of disc (may be sectoral) Crowded disc (see other eye) Vascular risk factors (DM, HTN, hypotension) No effective therapy Arteritic AION Should always be considered in AION Constitutional symptoms Combined ESR and CRP very sensitive and specific (97% for ESR>47, CRP>2.45) If suspected: admission for IV steroids and early temporal artery biopsy. Contralateral involvement in 50-90% of untreated patients! Vitreoretinal Vitreous haemorrhage: Retinal tear / detachment Proliferative diabetic retinopathy Retinal vein occlusion Retinal macroaneurysms (hypertension) Posterior vitreous detachment Vitreous haemorrhage The retina has to be evaluated through dilated fundoscopy Ultrasound B-scan if no fundal view If retinal detachment: urgent surgical repair may be required (macula on RD) Otherwise: later treatment or surgery (vitrectomy) depending on aetiology of the vitreous haemorrhage Retinal detachment Typically causing visual loss over days Starts as a dark curtain over part of field Often preceded by photopsias Family history, myopia, trauma, intraocular surgery may be risk factors Requires surgical repair The longer the delay in surgery the less chance the retina will return to function normally Acute retinal detachment caused by a retinal tear Macula still attached (on) RD “Macula-on” detachment Chronic, total RD with proliferative vitreoretinopathy Age related macular degeneration Most common reason for blindness in Western world Wet form: neovascular membrane bleeds/leaks, thus affecting macular function Treatment with intravitreal anti-VEGF injections Prognosis guarded Monitor for distortion (metamorphopsia) Questions?