* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 2-L2 new chronic pain
Survey
Document related concepts
Transcript
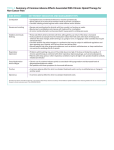
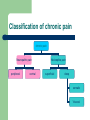
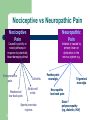
Chronic Pain Dr. Muhannad Y. Al-Muhanna What is Chronic Pain? Chronic pain is persistent or recurrent pain, lasting beyond the usual course of acute illness or injury, or more than 3 - 6 months, and adversely affecting the patient’s wellbeing. Pain that continues when it should not. Acute vs Chronic Pain Characteristic Acute Pain Chronic Pain Cause Generally known Often unknown Duration of pain Short, well-characterized Persists after healing, 3 months Treatment approach Resolution of underlying cause, usually selflimited Often not cure by treating the underlying cause Classification of chronic pain chronic pain Neuropathic pain peripheral central Nociceptive pain superficial deep somatic Visceral Nociceptive vs Neuropathic Pain Nociceptive Pain Neuropathic Pain Caused by activity in neural pathways in response to potentially tissue-damaging stimuli Postoperative pain Initiated or caused by primary lesion or dysfunction in the nervous system e.g. Arthritis Mechanical low back pain Sickle cell crisis Sports/exercise injuries *Complex regional pain syndrome Postherpetic neuralgia Trigeminal neuralgia Neuropathic low back pain Distal polyneuropathy (eg, diabetic, HIV) Pathophysiology of chronic pain Persistent activation of nociceptive transmission to the dorsal horn may induce a pain wind-up phenomenon. (Pain wind-up: is a frequency-dependent increase in the excitability (hyperexcitability) of spinal cord neurons, evoked by electrical stimulation of afferent C-fibers. It occurs due to sustained and repeated state of excitation of the projection neurons. Causing the dorsal horn neuron to transmit progressively increasing numbers of pain impulses. Pathophysiology of chronic pain This induces pathological changes that lower the threshold for pain signals to be transmitted. It may generate non-nociceptive nerve fibers to respond to pain signals. In chronic pain this process is difficult to reverse or eradicate once established. Central pain Central pain state: a neurological condition caused by damage or malfunction in the NS which causes a sensitization of the pain system. It is almost always generated by wind-up of the projection neurons of the spinothalamic and spinoreticular pathways. The extent of pain and the areas affected are related to the cause of the injury . Central (thalamic) pain syndrome Dejerine–Roussy syndrome is a condition developed after a thalamic stroke, a stroke causing damage to the thalamus. An initial lack of sensation and tingling in the opposite side of the body. Weeks to months later, numbness can develop into severe and chronic pain that is not proportional to an environmental stimulus, called dysaesthesia or allodynia. Chronic Pain Syndrome Chronic Pain Syndrome (CPS) is a common problem that is complex in nature of poor etiology and poor response to therapy. Most consider ongoing pain of 3~6 months are diagnostic. Two or more co-existing pain conditions or widespread generalized pain. Although CPS has been known to resolve completely with (and very rarely without) treatment, it is uncommon for full relief to be achieved Management of pain Opioids act on GPCRs: act by closing calcium channels or opening potassium channels. Opioids receptors are present centrally and peripherally. WHO Analgesic ladder: 1- start with non-opioid analgesics. 2- weak opioids. 3- strong opioids. Basic nerve conduction study MOTOR CONDUCTION STUDIES The compound muscle action potential (CMAP) is a biphasic potential with an initial negativity, or upward deflection from the baseline. For each stimulation site: the latency, amplitude, duration, and area of the CMAP are measured . A motor conduction velocity can be calculated after two sites of stimulation, one distal and one proximal. It’s called M response CMAP The active recording electrode is placed on the center of the muscle belly (over the motor endplate), and the reference electrode is placed distally about 3:4 cm The stimulator then is placed over the nerve that supplies the muscle, with the cathode placed closest to the recording electrode. As current is slowly increased from a baseline: more of the underlying nerve fibers are brought to action potential, and subsequently more muscle fiber action potentials are generated. The recorded potential, known as the compound muscle action potential (CMAP), represents the summation of all underlying individual muscle fiber action potentials. When the current is increased to the point that the CMAP no longer increases in size the supramaximal stimulation has been achieved. Latency Latency measurements usually are made in milliseconds (ms). The latency is the time from the stimulus to the initial negative deflection from baseline. The only major difference between CMAPs produced by proximal and distal stimulations is the latency. Conduction Velocity It’s measurement of the speed of the fastest conducting nerve axons. It is calculated by dividing the change in distance (between proximal stimulation site & distal stimulation site in mm) by the latency (time) difference (in ms) Conduction Velocity Amplitude it is most commonly measured from baseline to the negative peak (baseline-topeak) and less commonly peak-to-peak. CMAP amplitude reflects the number of muscle fibers that depolarize. low CMAP amplitudes most often result from loss of axons (as in a typical axonal neuropathy)