* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Week-4
Survey
Document related concepts
History of psychiatry wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Abnormal psychology wikipedia , lookup
Posttraumatic stress disorder wikipedia , lookup
History of mental disorders wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Transcript
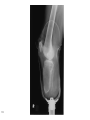
WEEK 4: FEDERAL & STATE REHABILITATION LAWS, RULES, REGULATIONS & GUIDELINES AS THEY APPLY TO WORKING AS A VRC IN THE VA SYSTEM. Special Topics in Rehabilitation: REH 6560 Assignment 4 Assignment 4 has been posted to the Course Website Reading Assignment for Week 4 has been posted to the Course Website Amputations Acquired condition that results in the loss of a limb 3 Amputations: Causes 4 Trauma: Severance of a body part due to sudden severe trauma Severe open fractures with arterial and nerve damage can be treated; however, treatment is at a high cost, and multiple surgeries are required The result is often a limb that is painful, nonfunctional, and less efficient than a prosthesis Amputation: Location 5 Below-Knee Amputation (B/K): This is an amputation above the ankle, but below the knee Full knee use is retained, but it is hard for these amputees to put weight on the stump Amputation: Location 6 Above Knee Amputation (A/K): This is an amputation in the thigh The whole body weight can't be held on the stump, but a person is able to sit with this amputation Amputation: Location 7 Hip Disarticulation (H/D): This involves removing the entire leg bone, but surgeons like to leave the upper femur for stability and a place or a prosthetic device Amputation: Location 8 Wrist Disarticulation (W/D): This is a removal of the hand, but at the wrist joint Plastic sockets are now made to serve as wrists Amputation: Location 9 Elbow Disarticulation (E/D): This is the removal of the whole forearm at the elbow This amputation creates a bulb shaped stump that can hold weight Amputation: Possible Functional Limitations 10 Upper Extremity: Grasping Pinching Bimanual Carrying Lifting Holding Pushing activities 11 Amputation: Possible Functional Limitations 12 Lower Extremity: Balancing Climbing Walking Stooping Pushing Lifting Jumping / Pulling 13 Prosthetics 14 Fit Training Comfort Stump Care Things To Ask About… 15 Frontal Lobe Injury Alterations in personality Occipital Lobe Injury Visual disturbances Things To Ask About… 16 Cortical Disruption Reduce mental status or Amnesia Retrograde Unable to recall events before injury Antegrade Unable to recall events after trauma “Repetitive Questioning” The Effects of a TBI Depend on: 17 Number of injuries Severity of injuries Time since injury(s) Areas of injury Age the injury(s) occurs The Effects of a TBI Depend on: 18 Status of the person before injury What happens after the injury to re-establish previous abilities Effects of Injury 19 The effects of the injury will not be uniform or necessarily stable. Impaired skills in one area does not necessarily mean impaired skills in another area. Strengths and weaknesses may change over time, especially with more recent injuries. Simplified Brain Behavior Relationships Frontal Lobe • Initiation • Problem solving • Judgment • Inhibition of behavior • Planning/anticipation • Self-monitoring • Motor planning • Personality/emotions • Awareness of abilities/limitations • Organization • Attention/concentration • Mental flexibility • Speaking (expressive language) 20 Parietal Lobe Frontal Lobe Occipital Lobe Temporal Lobe Parietal Lobe • Sense of touch • Differentiation: size, shape, color • Spatial perception • Visual perception Occipital Lobe • Vision Cerebellum Brain Stem Temporal Lobe Brain Stem • Memory • Hearing • Understanding language (receptive language) • Organization and sequencing • Breathing • Heart rate • Arousal/consciousness • Sleep/wake functions • Attention/concentration Cerebellum • Balance • Coordination • Skilled motor activity Types of TBI: Open 21 Skull compromised and brain exposed Head Trauma - 21 Types of TBI: Closed 22 Skull not compromised and brain not exposed Head Trauma - 22 Brain Injury 23 As defined by the National Head Injury Foundation “a traumatic insult to the brain capable of producing physical, intellectual, emotional, social and vocational changes.” Brain’s Response to Injury Swelling of brain Vasodilatation Increased 24 with increased blood volume ICP Head Trauma - 24 Brain’s Response to Injury 25 Decreased blood flow to brain Perfusion decreases Cerebral ischemia (hypoxia) Signs & Symptoms of Brain Injury: Altered Mental Status 26 Altered orientation Alteration in personality Amnesia Retrograde Antegrade Signs & Symptoms of Brain Injury 27 Cushing’s Reflex Increased BP Bradycardia Erratic respirations Signs & Symptoms of Brain Injury 28 Vomiting Without nausea Projectile Body temperature changes Changes in pupil reactivity Direct VS. Indirect Brain Injuries 29 Direct Primary injury caused by forces of trauma Indirect Secondary injury caused by factors resulting from the primary injury Brain Injury: Direct Brain Injury 30 o Immediate damage due to force o Coup and contracoup o Fixed at time of injury Head Trauma - 30 Direct Brain Injury Types 31 Coup Injury at site of impact Contrecoup Injury on opposite side from impact 32 Coup Contrecoup Indirect Brain Injury 33 o o o Results from hypoxia or decreased perfusion Response to primary injury Develops over hours Head Trauma - 33 Blast Injuries 34 Secondary blast injury (caused by flying debris and fragments) Tertiary blast injury (caused by being thrown by blast wind) from penetrating and blunt trauma that is not unlike head injuries from causes other than explosions Blast Injuries 35 There is some controversy whether the brain is vulnerable to primary blast injury (caused by the overpressurization wave), animal models suggest that it is. Shear and stress waves from the overpressurization could potentially cause TBI directly (e.g., concussion, hemorrhage, edema, diffuse axonal injury). PTSD 36 Post-traumatic stress disorder (PTSD) is a mental health condition that's triggered by a terrifying event Symptoms may include flashbacks, nightmares and severe anxiety, as well as uncontrollable thoughts about the event Summary 37 The frontal lobe of the brain is most commonly injured. Therefore, deficits in executive functioning and self-regulation are frequently observed after TBI Summary 38 Self-regulation is at the core of who we are, how we respond to different situations, and how well we are able to move toward the completion of our long-term goals. Summary 39 Self-regulation deficits can interfere with the effective provision of treatment and other services Many individuals with TBI have additional disorders associated with impaired selfregulation. The effects of such co-occurring disorders are not yet well-understood Secondary Effects of Impaired Executive Functioning/Self-Regulation 40 Decreased automatic responses Slowed processing More effort required to learn and respond Self-Regulation 41 Using the cognitively-based executive functions to manage one’s own responses to different situations Being able to make decisions based on long-term goals rather than immediate desires Impulsivity/Disinhibition 42 Performing a response without considering the longterm consequences of that action Lack of Initiation 43 Problems with “starting”--cannot initiate behaviors consistent with the achievement of one’s goals How would this impact looking for a job? Deficits in Self-Regulation are also Observed in Persons with: 44 Substance use disorders Attention deficit disorder Various psychiatric disorders And all are more prone to having a TBI. TBI: POSSIBLE FUNCTIONAL LIMITATIONS 45 Balancing, lifting, walking Strength, coordination Vision, hearing, communication skills Pain and headaches Possible Functional Limitations: TBI 46 Memory, organizational and planning ability, concrete thinking Attention span/distractibility Writing skills, reading skills, visual-spatial skills Lack of initiative, inflexibility, irritability TBI: Psychosocial Considerations 47 Social judgment, maturity Social awkwardness Feelings of isolation, impulsiveness, aggressiveness Anger, depression, anxiety, low self-esteem Noise-Induced Hearing Loss (NIHL) 48 Sound is measured in units called decibels. The humming of a refrigerator is 45 decibels, normal conversation is approximately 60 decibels, and the noise from heavy city traffic can reach 85 decibels. Noise-Induced Hearing Loss (NIHL) 49 Long or repeated exposure to sounds at or above 85 decibels can cause hearing loss. People usually experience pain at about 130 dB 50 51 52 Stats 1.6 million troops deployed to OEF/OIF to date Approximately 40% have accessed VA care Three most common presenting problems: Musculoskeletal Ailments Mental Disorders (PTSD, SA/D, Depressive) “Symptoms, Signs, and Ill Defined Cond.” PTSD and Mild Traumatic Brain Injury (TBI) Slightly more than half of combat injuries early in OIF came from explosions 29% evacuated from combat theater to WRAMC had evidence of TBI (Jan 2003-Feb 2007) Approximately 15% of all wounded vets have suffered TBI (4,471 cases diagnosed between October 2001 and September 2007) TBI Physical damage by external blunt or penetrating trauma Acceleration-Deceleration Movement (whiplash) resulting in tearing or nerve fibers, bruising/contusion of brain Scraping of brain across bony base of skull leading to olfactory, oculomotor, acoustic nerve damage. Loss of sense of smell and reduction of taste (anosmia), double and/or blurred vision, dizziness or vertigo Usually remit after several days or weeks (nerves recover or regenerate) Levels of TBI Mild LOC for less then 30 minutes w/normal CT and/or MRI Altered mental state: “dazed,” “confused,” “seeing stars” PTA less then 24 hours (unable to store or retrieve new information) Glasgow Coma Scale (GCS): 13-15 Levels of TBI Moderate LOC less than six hours w/abnormal CT and/or MRI PTA less than seven days GCS: 9-12 Severe LOC greater than six hours w/abnormal CT and/or MRI PTA greater than seven days GCS: 1-8 Post-Concussion Syndrome (PCS) Symptoms immediately post-injury may include: Memory, attention, concentration deficits Fatigues, poor sleep, dizziness, headaches Irritability, depression Anxiety Most common: free-floating anxiety, fearfulness, intense worry, generalized uneasiness, social withdrawal, heightened sensitivity, related dreams Recovery (mild TBI) expected within 4-12 weeks; however, some symptoms may linger for months to years Assessment Post concussion Syndrome (PCS) Insomnia Memory Deficits Poor Concentration Depressed Mood Anxiety Irritability Headache Dizziness Fatigue Noise/Light Intolerance PTSD Insomnia Memory Deficits Poor Concentration Depressed Mood Anxiety Irritability Intrusive symptoms Emotional Numbing Hyperarousal Avoidance behavior Mild TBI among OIF Returnees (Hoge et al., 2008) 2,525 soldiers included in study (assessed 3-4 months post-deployment) 5% (124) reported injury with LOC (up to several minutes) 10% (260) reported injury with altered mental status w/out LOC Four soldiers reported LOC longer than 30 minutes 17% (435) reported other injuries TBI Among OIF Returnees (Hoge et al., 2008) Of those who reported LOC, 44% met criteria for PTSD, as compared to: -27% of those with altered mental state -16% of those with other injuries -9% of those with no injuries Blast Injuries Over 50% of combat injuries result from bombs, grenades, land mines, missles, mortar/artillery shells Account for majority of brain injury in theater with GSWs, falls, and MVAs close behind TBI among service members as high as 22% 2003-2008: over 6,600 TBI Four major polytrauma centers (MN, CA, FL, VA): 923 OEF/OIF patients with TBI Blast Injury Blast injuries results from pressure generated from an explosion which causes in overpressurization Air-filled organs (ears, lung, GI tract) and organs surrounded by fluid filled cavities (brain, spinal cord) susceptible Hoge et al. (2006) 01 May 2003 – 30 April 2004: OEF (Afghanistan) OIF (Iraq, Kuwait, Qatar) Other (Bosnia, Kosovo, etc.) N = 303,905 Marines and Soldiers OEF: 11.3% of 16,318 OIF: 19.1% of 222,620 Other: 8.5% of 64,967 Hoge at al. (2006) Combat Experiences: OEF OIF OTHER Any 46.0% 65.1% 7.4% Witnessed 38.1% 49.5% 5.3% Discharged 6.2% 17.8% 0.4% Felt in Danger 24.6% 50.3% 3.2% Suicidality and PTSD PTSD patients are 6 times more likely to attempt suicide than the general population PTSD has greater risk of increased number of suicide attempts than all other anxiety disorders Kessler R et al. Arch Gen Psychiatry 1999;56:617-626. Therapeutic Intervention Teach patients that PTSD Represent psychobiologic reaction to overwhelming stress Not character flaw or sign of weakness Fear that will be seen as “damaged” or emotionally unstable May lose right to carry weapon May be viewed as unstable Traumatized patients Notoriously reluctant to seek help Particularly from mental health professionals Therapeutic Intervention PTSD symptom relief Usually requires specialized techniques help patient confront fears and emotional responses to trauma in more structured format Without becoming overwhelmed Treatment involves Reducing level of distress associated with memories of event Quelling resultant physiological reactions Focus on behavioral outcomes rather than biomedical indices Therapeutic Intervention Effective Exposure Therapy Cognitive-Behavioral Therapy Helping confront painful thoughts and feelings Helping process thoughts and feelings Interpersonal therapies Understanding ways in which traumatic event continues to affect relationships and other aspects of their lives Group Therapy May also help reduce isolation and stigma Pharmacotherapy In PTSD, randomized trials have shown effectiveness of SSRIs TCAs MAOIs SSRIs 1st-line treatment safer and better tolerated Only FDA-approved drugs Sertraline (Zoloft) Paroxetine (Paxil) Pharmacotherapy -blockers May reduce peripheral sympathetic tone Perhaps, potential to worsen depression Beneficial effects of drug therapy May not be evident for 8 weeks or more Once drug a drug seems effective Continue for at least 12 months Summary Most people will gradually recover from psychological effects of traumatic event PTSD will develop in a substantial portion of subjects exposed to trauma PTSD Failure to recover from nearly universal set of emotions and reactions Typically manifested by Distressing memories or nightmares related to trauma Attempts to avoid reminders of trauma Heightened state of physiological arousal Summary Biologic mechanisms of PTSD Changes in brain regions Amygdala and hippocampus Associated with fear and memory Changes in systems involved in coordinating body’s response to stress Hormonal Neurochemical Physiological Summary Treatment Educate patient about nature of disorder Provide safe and supportive environment Discuss trauma and impact Relieve distress associated with Memories reminders of events Treatment strategies with variable success Exposure therapy Pharmacotherapy cognitive therapy Summary Pharmacotherapy SSRIs Effective and well tolerated Many with PTSD do not respond to drugs Need to better study this subset Pilot studies with propranolol Need confirmation