* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Infective Endocarditis
Remote ischemic conditioning wikipedia , lookup
Jatene procedure wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Myocardial infarction wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Artificial heart valve wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Mitral insufficiency wikipedia , lookup
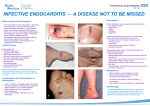
Endocarditis Endocarditis Chapter 3 Infective Endocarditis: Imaging to Improve Detection Rates Abdelhai Abdelqader1*, Chanukya Dahagam1, Aditya Goud1, Ramez Jabaji1, Gabriel Soudry2 and Sriram Padmanabhan3 Department of Internal Medicine, MedStar Franklin Square Hospital Center, USA 2 Department of Nuclear Medicine, MedStar Franklin Square Hospital Center, USA 3 Department of Cardiology, MedStar Franklin Square Hospital Center, USA Copyright: © 2016 Abdelhai Abdelqader, et al. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source. 1 Corresponding Author: Abdelhai Abdelqader, 9000 Franklin Square Drive, Baltimore, MD 21237, USA, Tel: 443-777-6346; Fax: 443-777-8155; Email: [email protected] * First Published September 10, 2016 All authors contributed equally to the creation of this manuscript. A Abdelqader is the article guarantor. Informed Consent: Informed consent was obtained from the patient for educational use of the below mentioned data and no personal patient information has been disclosed. 2 www.avidscience.com Introduction Infective endocarditis (IE) is an infection of the endocardium, but can involve any structure of the heart including prosthetic valves and implanted devices [1-4]. IE is a fatal disease with an in-hospital mortality rate up to 26% with half of patients having surgery during their hospital stay [1-4]. Echocardiography has played a key role in diagnosing IE, evaluating response to treatment, and predicting prognosis, however, has its own limitations. The limited anatomical information provided and lack of molecular activity monitoring has brought into question the use of other imaging modalities. Our aim is to discuss the roles of current imaging modalities can have in the diagnosis of IE. Imaging Modalities Echocardiogram is an essential imaging technique in diagnosing and managing IE. Echocardiography provides prognostic evaluation, follow-up during therapy and usewww.avidscience.com 3 Endocarditis Endocarditis ful in the perioperative period. Before and during surgery, transesophageal echocardiography (TEE) plays a crucial role [5]. Our aims of this review is to discuss the supplementary role in the diagnosis and possibly follow up care in IE with the use of multislice computerized tomography (CT), magnetic resonance imaging (MRI) and nuclear imaging. Echocardiography Echocardiography is the image test of choice to diagnose IE and plays a major role in the management and the follow up care in these patients. Echocardiography must be done without delay when IE is suspected. The diagnosis currently relies on clinical, microbiological and morphological criteria included in the modified Duke classification [5]. A strong understanding of the cardiothoracic anatomy is essential for understanding and analyzing echocardiographic findings. The initial test is a transthoracic echocardiography (TTE), that if negative in low-risk patients the IE is unlikely diagnosis. TTE is superior to TEE for detecting anterior cardiac abscesses and for assessing valvular function (Figure 1). If TTE is negative and high suspicion for IE exists, it should be followed up by TEE. A TEE should be done when a TTE is nondiagnostic, e.g. operator expertise, intracardiac device, distorted intra-thoracic or chest wall anatomy. 4 www.avidscience.com Figure 1: TTE of a patient with mitral valve IE due to Staphylococcus aureus with showing dynamic flow from the peri-valvular abscess seen at the center. www.avidscience.com 5 Endocarditis Endocarditis Figure 3: TEE of a large anterior mitral valve with IE. Figure 2: TTE of mitral valve IE due to Staphylococcus aureus. 6 www.avidscience.com www.avidscience.com 7 Endocarditis Endocarditis Major echocardiographic findings in diagnosing IE include vegetation, abscess or pseudoaneurysm and new dehiscence of a prosthetic valve [2,6,7]. With TEE, the diagnosis may remain very challenging in the setting of intracardiac device, pre-existing mitral valve prolapsed or degenerative calcified valves, prosthetic valves, vegetations <2 mm, or even non-vegetant IE (Figure 2). Threedimensional (3D) TEE superior to two-dimensional TEE in being able to identify and localize vegetations to better estimate risk of embolism as well as identifying complications such as abscesses, perforationsor ruptured chordate [8] (Figure 3). This is often used in many centers and is a reasonable technique that can complement standard echocardiography. In addition to diagnosis, echocardiography identifies prognostic signs that directly impact management of IE. The three most frequent and severe complications of IE are heart failure, perivalvular extension and embolic events. Heart failure is a major indication for emergent (within 24 hours) or urgent (few days) surgery [2]. TEE is excellent at identifying acute valvular regurgitation, valve obstruction or intracardiac fistula. TTE can demonstrate hemodynamic changes such as increased left and right diastolic pressures, pulmonary arterial pressures and ventricular dysfunction. Perivalvular extensions can be a precursor to heart failure via fistula or prosthetic valve dehiscence, complete heart block and persistent infection. In general, perivalvular extension is best seen with TEE, while TTE 8 www.avidscience.com is best to demonstrate anterior abscess of the aortic annulus [9]. Embolic events are common and symptomatic in 25% of cases with half incidentally found [10,11]. The risk of embolization is related to vegetation size. There is strong evidence that early surgery helps reduces embolic risk. When a vegetation is > 10mm there is high risk for embolization and when associated with complications (heart failure, infection refractory to therapy, abscess or prosthetic valve) or simply vegetation > 15mm it needs urgent surgery. If possible, valves should be surgically repaired especially mitral valves [2]. One of the challenges in managing IE is improving the diagnosis of IE to start treatment at an early stage [12]. The sensitivity of diagnosing vegetations in native and prosthetic valves for TTE is 70% and 50%, respectively and with TEE is 96% and 92%, respectively [6,7]. A negative echocardiography is observed in 15% of IE cases. False negatives that occur with echocardiography include intracardiac devices, valvular prosthesis, pre-existing severe valvular disease, very small vegetations, abscess or lack of vegetations. Identifying these lesions early in the disease can be difficult [13]. Conversely, false positive with echocardiography include thrombi that mimic vegetations, prolapsed cusp, intracardiac tumors, myxomatous changes, Lambl’s excresences or strands [13]. Hence, results can be misleading, even in the hands of an experienced person. We will now explore other imaging modalities that may improve the diagnosis of IE for earlier appropriate therapy. www.avidscience.com 9 Endocarditis Endocarditis Multislice Computed Tomography Multislice CT (MSCT) is a non-invasive test that provides detailed demonstration of not only coronary anatomy, but valvular and perivalvular damage through high temporal and spatial resolution and multiplanar reconstruction [14]. In identifying valvular and perivalvular damage, ECG-gated 64-slice CT (the minimum slices) has a reported sensitivity of 97%, specificity of 88% and negative predictive value (NPV) 88% compared to TEE [15]. Although MSCT misses small leaflet perforations, it is able to detect vegetations in prosthetic valve IE. MSCT can detect abscesses and pseudoaneurysms as accurate as TEE and superior in providing information on extent and consequences of any perivalvular extension, anatomy of abscesses, pseudoaneurysms, and fistulae [13,15]. Cardioembolic events can occur throughout the body, but most frequently the brain and spleen. For cerebral emboli, MRI is certainly superior, however, in critically ill patients MSCT serves a sensitive non-invasive diagnostic tool. If MSCT is negative for IE or IE complications, but clinical suspicion remains high the test is readily available to repeat. Splenic infarcts appear as triangular hypodensities on contrast CT, but are nonspecific for IE. The use of contrast offers high sensitivity and specificity in detecting systemic abscesses, but differentiation from infarct is a challenge. Administering intravenous contrast in a patient receiving potentially nephrotoxic an10 www.avidscience.com tibiotics and possible septic renal emboli should be done on case-by-case situation. Comparing MSCT to TEE, we are able to extract more information in a shorter time, but their utility remains case dependent (Table 1). The major limitations of MSCT are potential artifacts from metal and lack of hemodynamic assessment. Table 1: Comparing MSCT to TEE. Hemodynamics Vegetations and perforations TEE Accurate for evaluating hemodynamics Can be inaccurate in very severe acute lesions Excellent to detecting small vegetations and perforations Difficult to identify in PVE or calcified valves Difficult to identify leaflet perforation in AV IE CT Limited due to static image Difficult to demonstrate vegetations <2 mm Preferred method to demonstrate prosthetic valve vegetations Well demonstrates valular and perivalvular extension Difficult to demonstrate leaflet perforations Abscesses Difficult to identify in early IE Very operator dependent Fistulae Coronary anatomy Excellent demonstration of abscesses, aneurysms, and pseudoaneurysms Visualize mediastinal structures Can be combined with PET Excellent visualization Well visualized, but operator dependent Can demonstrate stenosis of ostial coronary artery Excellent visualization of coronary artery anatomy Wall motion abnormalities suggestive of ischemia or infarction Possible avoidance of pre-operative cardiac catherization in high-risk cases RCA may be difficult to visualize in presence of AVR Extra-cardiac signs An enlarged aortic root may prevent visualization of anomalous coronary arteries Ascending aorta well demonstrated Extra-cardiac shunts poorly seen Peripheral embolization not well seen www.avidscience.com Excellent demonstration of neurologic, pulmonary, and systemic embolizations and abscesses Extra-cardiac shunts well seen, but may not indicate infection 11 Endocarditis Endocarditis Magnetic Resonance Imaging Several studies have investigated the role of MRI in IE diagnosis and management and have made remarkable findings. Yet, the most plausible role of MRI in IE is detecting cerebral complications of embolic IE. MRI of the brain during acute IE has reported lesions in about 60% of cases [10,11,16]. Most cardioembolic strokes were ischemic, often with small infarcts than large infarcts. Studies have suggested< 10% of patients have lesions associated with parenchymal or subarachnoid hemorrhages, abscesses or mycotic aneurysms [10,11,16,17]. Compared to CT, MRI is a more sensitive test that can better characterize cerebrallesions in patients with IE, but its impact on IE diagnosis is reflected in adding one minor Duke criterion in patients with cerebral lesions without clinically evident neurologic deficits [11]. A prospective study by Duval et al. reported MRI brain upgraded the diagnosis of IE in a fourth of patients who presented with suspected IE, leading to an earlier diagnosis [10]. This study excluded microhemorrhages since they are nonspecific for IE-related cardioembolism [10,19]. Abdominal MRI detects a third of patients with lesions, often ischemic, but has no impact on diagnosis of IE compared to brain MRI [16,20]. Cardiac MRI has been shown to detect contrast enhancement in the late phase for irreversible myocardial damage and fibrosis. IE can result in myocarditis or coronary artery embolization leading to myocardial damage 12 www.avidscience.com and fibrosis. These can be detected with delayed phase enhancement MRI [21]. Delayed contrast enhancement MRI on the paravlavular tissues has been shown to detect paravalvular extension, a predictor for further complications such as paravalvular abscess, endothelial erosion, mycotic aneurysm, intracardiac fistula [21]. Unfortunately, limitations to cardiac MRI include artifacts due to prosthetic valves. This limits diagnostic information and lower spatial resolution, but is a nonionizing study. Given the information cardiac MRI provides despite its limitations, it may have a role in IE, albeit limited. Nuclear Imaging In an effort to accelerate the diagnostic phase if IE, focus has shifted from anatomical to functional at the molecular level. The most recently studied new nuclear imaging tool for use in IE has been positron emission tomography (PET-CT). The predominant utility in using this modality is to increase detection of IE in those with unclear diagnosis when using modified Duke criteria, peripheral emboli and inflammatory disease [22]. PET/CT uses 18 fluorodeoxyglucose (18F-FDG) that is injected and taken up in vivo by metabolically active cells. Images are taken approximately one hour after injection. The radioactive tracer, 18F-FDG, is taken up by inflammatory cells, which aggregate at sites of active infection [21]. Cases have been reported where PET/CT has detected www.avidscience.com 13 Endocarditis Endocarditis periprosthetic valve abscesses, while the initial echocardiography was negative. In following patients diagnosed with IE, PET/CT has revealed clinically silent cardioembolic events in a third of cases [23,24]. For PET/CT, cerebral septic emboli may be obscured as this tracer has high physiological uptake in the brain. Metastatic infections (generally <5 mm), may be below the threshold of detectability for PET/CT scanners [23,24]. For patients with recent implantation of the prosthetic valve, postoperative inflammation results in usually low grade tracer uptake of variable duration. FDG PETCT may also provide adequate differentiation between post-operative inflammation and active infection in patients with cardiovascular implantable electronic devices [23,25]. Additionally, a number of other conditions can imitate 18F-FDG uptake seen in IE, such as active thrombi, soft atherosclerotic plaques, vasculitis, primary cardiac tumors or cardiac metastasis from non-cardiac tumor, post-surgical inflammation, and foreign body reactions [23]. There is increasing interest in using PET/CT in established IE to monitor antibiotic responses, but currently there is insufficient data to make any recommendations. There is limited data exploring PET/CT in IE with native valves, impact of hyperglycemia, and cost analysis. 14 www.avidscience.com Conclusion In summary, review of recent data, the United States Task Force proposes three additions to the diagnostic criteria [18]: 1. Identifying paravalvular lesions by cardiac CT to be considered a major criterion. 2. When IE is not clear on a prosthetic valve, abnormal nuclear uptake around the valve site by 18FFDG PET CT if implanted >3 months or cardiac MRI should be considered a major criterion. 3. Identifying recent silent embolic events or infectious aneurysms by imaging only should be considered minor criterion. Echocardiography serves a major role in diagnosis and management of IE. Recent data suggests other imaging tools, namely MSCT, cerebral MRI and 18F-FDP PET CT can be used to improve detection rate of silent vascular phenomena and endocardial lesions in IE. In combination, these imaging tools may have use for diagnosis, follow up and diagnostically challenging cases of IE. References 1. Habib G. Embolic risk in subacute bacterial endocarditis: determinants and role of transesophageal echocardiography. Current cardiology reports. 2003; 5: 129-136. www.avidscience.com 15 Endocarditis Endocarditis 2. Habib G, Hoen B, Tornos P, Thuny F, Prendergast B, et al. Guidelines on the prevention, diagnosis, and treatment of infective endocarditis (new version 2009): the Task Force on the Prevention, Diagnosis, and Treatment of Infective Endocarditis of the European Society of Cardiology (ESC). Endorsed by the European Society of Clinical Microbiology and Infectious Diseases (ESCMID) and the International Society of Chemotherapy (ISC) for Infection and Cancer. Eur Heart J. 2009; 30: 2369-2413. 5. Saby L, Laas O, Habib G, Cammilleri S, Mancini J, et al. Positron Emission Tomography/Computed Tomography for Diagnosis of Prosthetic Valve Endocarditis: Increased Valvular F-Fluorodeoxyglucose Uptake as a Novel Major Criterion. Journal of the American College of Cardiology. 2013; 61: 2374-2382. 3. Tornos P, Iung B, Permanyer-Miralda G, Baron G, Delahaye F, et al. Infective endocarditis in Europe: lessons from the Euro heart survey. Heart. 2005; 91: 571-575. 7. Mügge A, Daniel WG, Frank G, Lichtlen PR. Echocardiography in infective endocarditis: reassessment of prognostic implications of vegetation size determined by the transthoracic and the transesophageal approach. Journal of the American College of Cardiology. 1989; 14: 631-638. 4. Baddour LM, Wilson WR, Bayer AS, Fowler VG Jr, Bolger AF, et al. Infective endocarditis diagnosis, antimicrobial therapy, and management of complications: a statement for healthcare professionals from the committee on rheumatic fever, endocarditis and Kawasaki disease, council on cardiovascular disease in the young, and the councils on clinical cardiology, stroke, and cardiovascular surgery and anesthesia, American Heart Association: endorsed by the Infectious Diseases Society of America. Circulation. 2005; 111: e394e434. 16 www.avidscience.com 6. Habib G, Badano L, Tribouilloy C, Vilacosta I, Zamorano JL, et al. Recommendations for the practice of echocardiography in infective endocarditis. Eur J Echocardiogr. 2010; 11: 202-219. 8. Berdejo J, Shibayama K, Harada K, Tanaka J, Mihara H, et al. Evaluation of Vegetation Size and Its Relationship With Embolism in Infective Endocarditis A Real-Time 3-Dimensional Transesophageal Echocardiography Study. Circulation: Cardiovascular Imaging. 2014; 7: 149-154. 9. Graupner C, Vilacosta I, SanRomán J, Ronderos R, Sarriá C, et al. Periannular extension of infective endocarditis. J Am Coll Cardiol. 2002; 39: 1204-1211. www.avidscience.com 17 Endocarditis Endocarditis 10.Duval X, Iung B, Klein I, Brochet E, Thabut G, et al. Effect of early cerebral magnetic resonance imaging on clinical decisions in infective endocarditis: a prospective study. Annals of Internal Medicine. 2010; 152: 497-504. 11.Cooper HA, Thompson EC, Laureno R, Fuisz A, Mark AS, et al. Subclinical brain embolization in left-sided infective endocarditis: results from the evaluation by MRI of the brains of patients with left-sided intracardiac solid masses (EMBOLISM) pilot study. Circulation. 2009; 120: 585-591. 12.Habib G, Avierinos JF, Thuny F. Aortic valve endocarditis: is there an optimal surgical timing? Current opinion in cardiology. 2007; 22: 77-83. 13.Grob A, Thuny F, Villacampa C, Flavian A, Gaubert JY, et al. Cardiac multidetector computed tomography in infective endocarditis: a pictorial essay. Insights Imaging. 2014; 5: 559-570. 14.Thuny F, Gaubert JY, Jacquier A, Tessonnier L, Cammilleri S, et al. Imaging investigations in infective endocarditis: current approach and perspectives. Arch Cardiovasc Dis. 2013; 106: 52-62. 15.Feuchtner GM, Stolzmann P, Dichtl W, Schertler T, Bonatti J, et al. Multislice computed tomography in infective endocarditis: comparison with transesophageal echocardiography and intraoperative findings. J Am CollCardiol. 2009; 53: 436444. 18 www.avidscience.com 16.Snygg-Martin U, Gustafsson L, Rosengren L, Alsiö A, Ackerholm P, et al. Cerebrovascular complications in patients with left-sided infective endocarditis are common: a prospective study using magnetic resonance imaging and neurochemical brain damage markers. Clinical infectious diseases. 2008; 47: 23-30. 17.Okazaki S, Yoshioka D, Sakaguchi M, Sawa Y, Mochizuki H, et al. Acute ischemic brain lesions in infective endocarditis: incidence, related factors, and postoperative outcome. Cerebrovascular Diseases. 2013; 35: 155-162. 18.Li JS, Sexton DJ, Mick N, Nettles R, Fowler VG Jr, et al. Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis. 2000; 30: 633-638. 19.Klein I, Iung B, Labreuche J, Hess A, Wolff M, et al. Cerebral microbleeds are frequent in infective endocarditis: a case-control study. Stroke. 2009; 40: 3461-3465. 20.Bernard Iung, Isabelle Klein, Bruno Mourvillier, Jean-Marc Olivot, Delphine De´taint et al. Respective effects of early cerebral and abdominal magnetic resonance imaging on clinical decisions in infective endocarditis. European Heart JournalCardiovascular Imaging. 2012; 13: 703-710. 21.Dursun M, Yılmaz S, Yılmaz E, Yılmaz R, Onur İ, et al. The utility of cardiac MRI in diagnosis of www.avidscience.com 19 Endocarditis Endocarditis infective endocarditis: preliminary results. Diagn Interv Radiol. 2015; 21: 28-33. 22.Palestro CJ, Manuel L Brown, Lee A Forstrom, Bennett S Greenspan, John G McAfee, et al. Society of Nuclear Medicine Procedure Guideline for 99mTc-exametazime (HMPAO)-labeled leukocyte scintigraphy for suspected infection/inflammation, version 3.0. 2004. 23.Van Riet J, Hill EE, Gheysens O, Dymarkowski S, Herregods MC, et al. (18)F-FDG PET/CT for early detection of embolism and metastatic infection in patients with infective endocarditis. Eur J Nucl Med Mol Imaging. 2010; 37: 1189-1197. 24.Sarrazin JF, Philippon F, Tessier M, Guimond J, Molin F, et al. Usefulness of fluorine-18 positron emission tomography/computed tomography for identification of cardiovascular implantable electronic device infections. J Am CollCardiol. 2012; 59: 1616-1625. 25.Erba PA, Conti U, Lazzeri E, Sollini M, Doria R, et al. Added value of 99mTc-HMPAO-labeled leukocyte SPECT/CT in the characterization and management of patients with infectious endocarditis. J Nucl Med. 2012; 53: 1235-1243. 20 www.avidscience.com www.avidscience.com 21