* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 4 Infectious Diseases
Middle East respiratory syndrome wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Henipavirus wikipedia , lookup
Onchocerciasis wikipedia , lookup
Sarcocystis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Anaerobic infection wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Leptospirosis wikipedia , lookup
West Nile fever wikipedia , lookup
Trichinosis wikipedia , lookup
Epidemiology of HIV/AIDS wikipedia , lookup
Diagnosis of HIV/AIDS wikipedia , lookup
Hepatitis C wikipedia , lookup
Marburg virus disease wikipedia , lookup
Oesophagostomum wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Schistosomiasis wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Hepatitis B wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
Herpes simplex wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Herpes simplex virus wikipedia , lookup
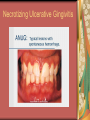
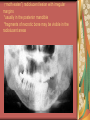
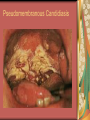
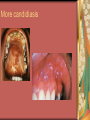
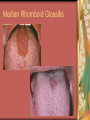
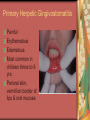
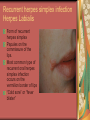
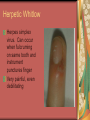
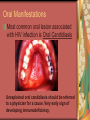
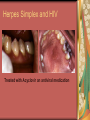
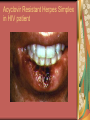
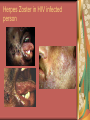
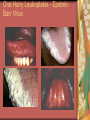
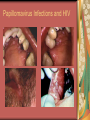
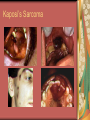
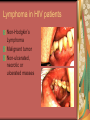
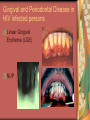
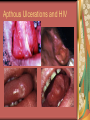
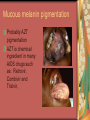
Chapter 4 Infectious Diseases Bacterial Infections Inflammatory and immune response to infection Inflammatory response is a nonspecific response and results in edema and the accumulation of a large number of white blood cells ate the site Immune system response is highly specific Specific antibodies are formed in response to specific antigens Microorganisms are antigens Opportunistic infection Decrease in salivary flow Antibiotic administration Immune system alterations Change oral flora so that organisms that are usually nonpathogenic are able to cause disease Impetigo Skin infection – caused by Streptococcus pyogenes and Staphylococcus aureus May itch (pruritus) Regional lymphadenopathy may be present Normally found on skin (non-intact skin is necessary to contract Oral manifestation - resembles recurrent herpes simplex Tuberculosis Infectious chronic granulomatous disease Usually caused by Mycobacterium tuberculosis Primary infection of the lung Inhaled droplets containing bacteria lodge in the alveoli of the lungs Ulcerations can appear when organisms are carried in sputum to oral cavity Routine dental treatment is deferred for patients with active TB An antigen called Purified Protein Derivative (PPD) is injected into the skin Actinomycosis Infection caused by a filamentous bacterium called Actinomyces israelii Formation of abscesses that tend to drain by the formation of sinus tracts Organisms are common inhabitants of the oral cavity…predisposing factors are unknown Syphilis Caused by the spirochete Treponema pallidum. Transmitted by direct contact Can penetrate mucous membranes, but needs a break in tissue to penetrate it Usually transmitted through sexual contact with a partner with active lesions Blood or transplacental innoculation Syphilis Stages of Syphilis: (1) Primary - oral lesion - chancre (2) Secondary- oral lesion - mucous patch (3) Latent - no oral lesion (4) Tertiary - oral lesion - gumma Necrotizing Ulcerative Gingivitis Necrotizing Periodontal Diseases NUG- an acute infection isolated in the gingiva (formerly known as ANUG) NUP – is a similar infection that has progressed to include attached periodontal ligament and bone loss (AAP, 2000) Necrotizing Periodontal Diseases Signs and symptoms Gingiva is painful and erythematous Necrosis of interdental papillae (blunted) Foul odor Metallic taste Sloughing of the necrotic tissue presents as a pseudomembrane over the tissues Necrotizing Periodontal Diseases Unique in their clinical presentation, etiology and pathogenesis If NUP is combined with HIV marginal necrosis of the gingiva and a very rapid loss of alveolar bone is seen severe pain and bleeding without any provocation perhaps because of immunodeficiency there have been reports of tooth loss in only three to six months after onset Necrotizing Periodontal Diseases NUG Acute recurring gingival infection of complex etiology Characterized by necrosis of the papillae often described as “punched-out” Spontaneous bleeding and pain Pain is what make necrotizing periodontal diseases very different from plaqueinduced gingivitis and periodontitis NUG 1. 2. 3. 4. 5. 6. Known by many names over the years Trench mouth Vincent’s infection Fuso-spirochetal gingivitis ANUG (misnomer b/c “acute” is clinical description) No chronic form of NUG Recurrence NUP Progression of NUG into the underlying attached gingiva causing periodontal pocketing Bone loss May occur if # of recurrences of NUG or underlying systemic conditions such as AIDS AIDS/NUP originally called HIV_P If associated with recurrences conservative treatment is very successful No so with AIDS patients NPD One of the few “emergency” dental hygiene appointments Extreme pain Gross debridement Anesthetic helps ease pain during procedure Sonic or ultrasonic Education about the cause of the disease Nutritional counseling Vitamin recommendations Oral hygiene instruction No antibiotics Pericoronitis Inflammation of the mucosa around the crown of a partially erupted or impacted tooth Trauma from an opposing molar and impaction of food under the soft tissue flap (operculum) covering the distal portion of the third molar Treatment includes mechanical debridement and irrigation of the pocket and systemic antibiotics. Extraction of the impacted molar is usually necessary to prevent recurrence. Osteomyelitis An inflammatory process within medullary (trabecular) bone that involves the marrow spaces No change is seen on the radiograph unless the disease has been present for more than one week *(“moth eaten”) radiolucent lesion with irregular margins *usually in the posterior mandible *fragments of necrotic bone may be visible in the radiolucent areas Tonsillitis and Pharyngitis Inflammatory conditions of the tonsils and pharyngeal mucosa Can be caused by different organisms Streptococcal bacterial infection closely resembles tonsillitis and pharyngitis that are caused by viruses Strep throat caused by group A, beta hemolytic streptococci are significant Strep throat Scarlet fever - usually occurs in children Tonsillitis and pharyngitis Fever, red skin rash, petechiae on the soft palate and “strawberry tongue” Rheumatic Fever - childhood disease that follows strep infection Inflammatory reaction involving heart, joints, and CNS Heart valve damage…bacterial endocarditis prophylactic pre-medication is necessary Fungal Infections Candidiasis Moniliasis (“Thrush”) Overgrowth the yeast-like fungus Candida albicans Encompasses a group of mucosal and cutaneous conditions with a common etiologic agent from the Candida genus of fungi; most common oral mycotic infection Part of the normal oral flora especially if dentures are worn Candida albicans overgrowth can result from many different conditions Antibiotic therapy Cancer chemotherapy Corticosteroid therapy Dentures Diabetes Mellitus HIV infection Hypoparathyroidism Infancy Multiple Myeloma Primary T-lymphocyte deficiency Xerostomia Types of Oral Candidiasis Pseudomembranous Erythematous Chronic atrophic (denture stomatitis) Chronic hyperplastic (candidal leukoplakia) Angular cheilitis Pseudomembranous Candidiasis More candidiasis Angular Cheilitis Candida organism most often causes Appears as erythema and/or fissuring at the labial commissures Can be caused by other factors (e.g., nutritional, factitial) Angular cheilitis Condition is most often bilateral Median Rhomboid Glossitis An asymptomatic, elongated, erythematous patch of atrophic mucosa of the mid-dorsal surface of the tongue due to a chronic Candida albicans infection Central Papillary Atrophy of the Tongue Median Rhomboid Glossitis Viral Infections Papillomavirus infection HPV’s identified in oral lesions, normal mucosa and implicated in neoplasia Verruca vulgaris or common wart autoinoculation occurs through finger contact…looks like a papilloma Primary Herpetic Gingivostomatitis Painful Erythematous Edematous Most common in children 6mos to 6 yrs. Perioral skin, vermillion border of lips & oral mucosa Recurrent herpes simplex infection Herpes Labialis Form of recurrent herpes simplex Papules on the commissure of the lips. Most common type of recurrent oral herpes simplex infection occurs on the vermilion border of lips “Cold sore” or “fever blister” Recurrent herpes simplex infection Intraorally - occurs on keratinized mucosa that is fixed to bone Most commonly hard palate and gingiva Tiny clusters of vesicles or ulcers that can coalesce to form a single ulcer with an irregular border Prodromal symptoms = pain, burning, tingling Heal without scarring in 1-2 weeks Transmitted by direct contact Primary infection occurs at the site of inoculation Amount of virus is highest in vesicle stage Herpetic Whitlow Herpes simplex virus. Can occur when fulcruming on same tooth and instrument punctures finger Very painful, even debilitating Herpes simplex can also spread to eyes. Inform patients with herpes to be very careful not to self inoculate. If they have open vesicles it can be spread to other areas of the body such as eyes or mucous membranes around genitalia. Learn table 4-2 on differences between aphthous ulcers and herpes simplex (page 142) Herpes Zoster Caused by the Varicella-Zoster virus Common name is Shingles Respiratory aerosols and contact with secretions from skin lesions transmit the virus Unilateral distribution of oral and skin lesions Painful vesicles that progress to ulcers Same virus that causes Chicken Pox (Varicella) Epstein-Barr Virus Infection Infectious Mononucleosis Most common in late adolescents and young adults in upper socioeconomic classes (transmitted by close contact) Hairy Leukoplakia Most common in HIV infected people Nasopharyngeal carcinoma - rare neoplasm Burkitt’s Lymphoma - rare neoplasm Coxsackievirus infections Herpangia - vesicles on the soft palate *fever, malaise, sore throat, difficulty swallowing (dysphagia)…erythematous pharyngitis Mild to moderate and resolves in less than 1 week Hand-Foot and Mouth Disease - occurs in epidemics in children less that 5 years of age Painful vesicles and ulcers anywhere in mouth Lesions resolve spontaneously within 2 weeks Human Immunodeficiency Virus (HIV) & Acquired immunodeficiency syndrome (AIDS) Most individuals experience an acute disease that occurs shortly after infection with HIV Sexual contact, blood or blood product contact, infant to mother Acute disease resolves and no signs or symptoms of disease exist for some time Most patients eventually have a progressive immunodeficiency HIV & AIDS # of CD4 lymphocytes decreases Fatigue, opportunistic infections (oral candidiasis) As the immune system becomes profoundly deficient, life threatening opportunistic infections and neoplasms occur Most severe result of infection with HIV is AIDS AIDS Diagnosis See table 4-3 (page 147) Severe CD4 lymphocyte depletion Pneumocystic carinii pneumonia Esophageal candidiasis Kaposi’s sarcoma Pulmonary tuberculosis Recurrent pneumonia Invasive cervical cancer Oral Manifestations Most common oral lesion associated with HIV infection is Oral Candidiasis Unexplained oral candidiasis should be referred to a physician for a cause. Very early sign of developing immunodeficiency. Herpes Simplex and HIV Treated with Acyclovir an antiviral medication Acyclovir Resistant Herpes Simplex in HIV patient Herpes Zoster in HIV infected person Oral Hairy Leukoplakia - EpsteinBarr Virus Papillomavirus Infections and HIV Kaposi’s Sarcoma Opportunistic neoplasm that occurs in patients with HIV infections HHV-8 associated with this neoplasm Neoplasm is a mass of newly formed tissue in which the growth of tissue is uncontrolled and progressive Kaposi’s Sarcoma Lymphoma in HIV patients Non-Hodgkin’s Lymphoma Malignant tumor Non-ulcerated, necrotic or ulcerated masses Gingival and Periodontal Disease in HIV infected persons Linear Gingival Erythema (LGE) NUP Apthous Ulcerations and HIV Mucous melanin pigmentation Probably AZT pigmentation AZT is chemical ingredient in many AIDS drugs such as: Retrovir, Combivir and Trizivir,