* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Placenta - Academics
High-altitude adaptation in humans wikipedia , lookup
Acute respiratory distress syndrome wikipedia , lookup
Circulatory system wikipedia , lookup
Cushing reflex wikipedia , lookup
Homeostasis wikipedia , lookup
Hemodynamics wikipedia , lookup
Biofluid dynamics wikipedia , lookup
Common raven physiology wikipedia , lookup
Intracranial pressure wikipedia , lookup
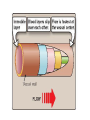
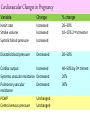
Maternal Physiology Dr Kapila Hettiarachchi Consultant Anaesthetist SBSCH – Peradeniya Sri Lanka Hemodynamic Changes Systemic vascular resistance Falls steadily over the first 20 weeks primary cause Erosion of maternal resistance vessels by the fetal placenta Progesterone Dilate cutaneous and renal vascular Cardiac output Cardiac output increase by 40-50% Stroke Volume - 20-30% Heart rate - 10-15% Cardiac output Stroke Volume begins to rise very early (20–30%) in pregnancy, mediated by an increase in preload and contractility Preload Na+ and water retention Placental hormones potentiate Renin– angiotensin–aldosterone system and thirst Contractility Sustained increases in cardiac output Stimulate ventricular hypertrophy • The heart is physiologically dilated and displaced in both cephalad and lateral directions. • A normal pregnancy ECG may have 15 – 200 left axis deviation and T waves may be inverted in lateral leads and lead III mimicking left ventricular hypertrophy and other structural disease. Mean arterial pressure Diastolic blood pressure falls Pulse pressure widens 1. CO 2. Heart rate 3. Mean arterial pressure 4. Systemic vascular resistance Increased diastolic runoff Blood escapes the arterial system more easily during diastole Windkessel Effect Evens out pressure and flow through the vasculature over time C. Physiologic anaemia Plasma volume increase by 40%–50% Red blood cell increase by 25%–35% Physiologic benefit Reduces blood viscosity So, reduces shear stress Shear stress high velocity to support the sustained increases in cardiac out put High-velocity flow increases shear stress on the vascular lining, where it could become damaging Shear stress When blood velocity and viscosity increases Shear stress is increased Reynolds equation Haematocrit is the primary determinant of blood viscosity Anaemia reduces shear stress levels and lessens the risk of vascular endothelial damage Reynolds equation The likelihood of turbulence can be predicted NR is Reynolds number, v is mean blood velocity, d is vessel diameter, ρ (rho) is blood density, η is blood viscosity. 2. Murmurs Functional murmurs Venous hum Cardiovascular Changes in Pregnancy Variable Heart rate Stroke volume Systolic blood pressure Change Increased Increased Increased % change 20–30% 10–15% 2nd trimester Diastolic blood pressure Decreased 20–50% Cardiac output Systemic vascular resistance Pulmonary vascular resistance PCWP Central venous pressure Increased Decreased Decreased 40–50% by 3rd trimest 20% 30% Unchanged Unchanged Aortocaval Compression Compensation occurs through sympathetic stimulation and collateral venous return via vertebral plexus and azygous veins Aortocaval Compression • By 38–40 weeks gestational age, there is a 25 – 30% decrease in CO when turning from the lateral to the supine position. Blood flow to the nasal mucosa is increased Increase in blood flow to the skin, resulting in warm, clammy hands and feet Dissipate heat from the metabolically active feto-placental unit oEdema Fetus, placenta, and amniotic fluid = ~8–10 kg at term compresses inferior vena cava and other smaller veins oEdema Compression causes venous pressures in the lower extremities to rise This causes Increases mean capillary pressure and Increases net fluid filtration from blood to the interstitium oEdema Fall in colloid osmotic pressure by 30%– 40% during pregnancy (from ~25 mm Hg prior to pregnancy to ~15 mm Hg postpartum) Respiratory system O2 demands of the mother and growing fetus increase rapidly during pregnancy O2 consumption at term is increased ~ 30% Progesterone exerts a stimulant action on the respiratory centre and carotid body receptors Respiratory system Progressive increase in minute ventilation to ~50% over non-pregnant values during the second trimester Respiratory system What is minute ventilation ? Respiratory system Minute ventilation increase is mainly by An increase in tidal volume and Small or no rise in respiratory rate (2–3 breaths/min) Respiratory system Net effect is that PaO2 rises by ~10 mm Hg, and PaCO2 falls by ~8 mm Hg, causing a slight respiratory alkalosis (<0.1 pH ) Respiratory system 20% decrease in Functional residual capacity (FRC) Expiratory reserve capacity (ERC) Residual volume (RV) caused by a rise in the diaphragm Changes in Respiratory Function in Pregnancy Variable Non-Pregnant Term Pregnancy Tidal volume ↑ 450 mL 650 mL Respiratory rate 16 min–1 16 min–1 Vital capacity 3200 mL 3200 mL Inspiratory reserve volume 2050 mL 2050 mL Expiratory reserve volume ↓ 700 mL 500 mL Functional residual capacity ↓ 1600 mL 1300 mL Residual volume ↓ 1000 mL 800 mL PaO2 slight ↑ 11.3 kPa 12.3 kPa PaCO2 ↓ 4.7–5.3 kPa 4 kPa pH slightly ↑ 7.40 7.44 Renal blood flow is increased Renal Glomerular Filtration Rate (GFR) rises steadily to ~50% above normal values at 16 weeks’ gestation Renal Changes in Pregnancy Parameter NonPregnant Pregnant Urea (mmol L 2.5–6.7 2.3–4.3 70–150 50–75 200–350 150–350 22–26 18–26 −1) Creatinine (μmol L−1) Urate (μmol L −1) Bicarbonate (mmol L −1) Aldosterone • Action is enhanced to increase water absorption causing increase in volume of distribution. Gastrointestinal Changes Heart burn due to reduction in lower oesophageal sphincter tone (but not upper oesophageal sphincter) and cephalad passage of acidic gastric content. Increase in intragastric pressure and altered axis due to upward movement of gravid uterus. Gastrointestinal Changes Gastrointestinal motility decreases but gastric emptying is not delayed during pregnancy However, it is delayed during labour but returns to normal by 18 h after delivery GI effects return to pre-pregnancy level in 24-48hrs Liver Function Changes in Pregnancy Parameter Change in Pregnancy Albumin Decreased Alkaline phosphatase Increased (from placenta) ALT/AST No change Plasma cholinesterase Decreased NO increase in Liver blood flow Pregnancy induces a hypercoagulable state Coagulation Changes in Late Pregnancy Fibrinolysis – increased Platelet function not changed Haematological Changes Associated with Pregnancy Variable NonPregnant Pregnant Haemoglobin 14 g dL–1 12 g dL–1 Haematocrit 0.40–0.42 0.31–0.34 Red cell count 4.2 × 1012 L–1 3.8 × 1012 L–1 White cell count 6.0 × 109 L–1 9.0 × 109 L–1 ESR 10 58–68 Platelets 150–400 × 109 L–1 120–400 × 109 L–1 Haematological changes Fibrinogen increased from 2.5 (non-pregnant value) to 4.6–6.0 g L–1 Factor II slightly increased Factor V slightly increased Factor VII increased 10-fold Factor VIII increased – twice non-pregnant state Factor IX increased Factor X increased Factor XII increased 30–40% Plasminogen unchanged Plasminogen activator reduced Plasminogen inhibitor increased Fibrinogen-stabilizing factor falls gradually to 50% of non-pregnant value Factor XI decreased 60–70% Factor XIII decreased 40–50% Antithrombin IIIa decreased slightly 23. Features of Mendelson’s syndrome include: a) Urticarial rash b) Bronchospasm c) Hypoxia d) Hypotension e) Aspiration of at least 100 ml of gastric contents • 23. FTTFF 2. Physiology of pregnancy: clinical anaesthetic implications Compared with the non-gravid state, increased cardiac output in pregnancy: 1. Occurs as a result of a high-flow, high-resistance circulation. 2. Is likely to lead to non-pathological systolic and diastolic murmurs. 3. Is associated with an electrocardiogram (ECG) that is similar to that during pulmonary embolism. 4. Is likely to be reduced by aortocaval compression in the first, second and third trimesters. 5. Combined with an altered haemoglobin concentration, leads to an increase in oxygen delivery. FTFTT 18. Appropriate statements regarding the respiratory system in pregnant patients compared with non-pregnant patients include: 1. There is a reduction in airway resistance. 2. Reduced functional residual capacity (FRC) increases alveolar dead space. 3. Reduced FRC is expected to be associated with a reduction in the rate of increase in concentration of volatile anaesthetic agents. 4. Increased minute ventilation during labour can cause acidaemia in the fetus. 5. During preoxygenation, denitrogenation is likely to occur quickly. • TFFTT 19. During pregnancy: 1. Urine glucose is helpful in assessing diabetic control in pregnancy. 2. Thyroid function testing should include both thyroid-stimulating hormone and free thyroxine. 3. Raised alkaline phosphatase is usually indicative of liver disease. 4. Having normal renal functions is clinically significant in pregnancy. 5. Proton pump inhibitors (PPIs) are contraindicated. 19. • • • • • 1. F 2. T 3. F 4. T 5. F 20. The following physiological changes occur in normal pregnancy: (a) Progesterone increases the sensitivity of the respiratory center to carbondioxide. (b) Systemic vascular resistance is increased in trimesters I and II. (c) Central venous pressure increases. (d) Gastric emptying is delayed. (e) FRC decreases to 80% of pre-pregnancy values. 20. The following physiological changes occur in normal pregnancy: (a) True; (b) False; (c) False; (d) False; (e) True (a) It also acts as a primary respiratory stimulant and the effects are enhanced by oestrogen. (b) Systemic vascular resistance decreases by 25--30%, the effect mediated by progesterone, prostacyclin and oestrogen. (c) Central venous pressure and pulmonary artery pressure are unchanged during normal pregnancy. During labour each uterine contraction expels 500 ml of blood into the circulation which produces an increase in central venous pressure of 4--6 cm H2O. 21. Pregnancy-induced changes in lung volumes cause: • (a) Desaturation to occur more rapidly than in non-pregnant patients. • (b) Pre-oxygenation to be more effective. • (c) A fall in minute ventilation due to restricted diaphragmatic excursion. • (d) Airway closure in the erect position in 50% of parturients at term. • (e) An increase in PaCO2. 21. Pregnancy-induced changes in lung volumes cause: (a) True; (b) False; (c) False; (d) False; (e) False • (a,b) The residual volume and the functional residual capacity are reduced in pregnancy causing a decrease in the O2 storage capacity. Thus, desaturation occurs much faster and pre-oxygenation, although still recommended, is less effective. • (c) Although the diaphragm is displaced in later pregnancy, an increase in the diameter of the chest ensures increased minute volumes. • (d) Airway closure occurs in the supine position. (e) PaCO2 decreases as a result of an increased minute ventilation. 22. In the third trimester of pregnancy: • (a) A mild elevation of g-GT and ALT is abnormal. • (b) Alkaline phosphatase plasma concentrations return to normal. • (c) A plasma creatinine concentration of 120 μmol l–1 is a normal finding. • (d) A plasma urate concentration of 0.5 mmol l–1 is consistent with the diagnosis of pre-eclampsia. • (e) The platelet count is frequently slightly decreased. 22. In the third trimester of pregnancy: (a) False; (b) False; (c) False; (d) True; (e) True • (a) Mildly elevated liver enzymes are a normal finding throughout pregnancy. • (b) Alkaline phosphatase is produced in the placenta and is often increased 2-fold compared with non-pregnant women. • (d) The upper normal limit for urate in pregnancy is 0.35 mmol l–1 and urate is frequently elevated in preeclampsia. • (e) The platelet count tends to be slightly lower than in non-pregnant women. 23. Aortocaval compression: • (a) Does not occur before the end of the first trimester. • (b) Is symptomatic in about 10% of parturients in the third trimester. • (c) Can be unmasked by the institution of effective epidural analgesia. • (d) May occur on induction of general anaesthesia despite a wedge under the parturients right hip. • (e) Can cause fetal hypoxaemia. 23. Aortocaval compression: (a) False; (b) True; (c) True; (d) True; (e) True • (a) Aortocaval compression usually occurs after 20 weeks’ gestation but may occur before. (b–e) Aortocaval compression is only symptomatic in about 10% of parturients but may be unmasked by general, spinal anaesthesia, epidural anaesthesia and sedation.A 15° left lateral tilt or a wedge under the right hip have been described to treat symptomatic aortocaval compression but manual displacement of the uterus may occasionally be necessary to treat its symptoms. Untreated it will eventually lead to fetal hypoxaemia. 24. The following changes occur in the gastro-intestinal system during pregnancy: • (a) Gastric emptying is delayed in the third trimester. • (b) Lower oesophageal sphincter pressure decreases as a result of progesterone-mediated smooth muscle relaxation. • (c) Upper oesophageal sphincter pressure decreases as a result of progesterone-mediated smooth muscle relaxation. • (d) Gastric volume increases in labour. • (e) 80% of term parturients suffer from gastrooesophageal reflux. 24. The following changes occur in the gastro-intestinal system during pregnancy: (a) False; (b) True; (c) False; (d) True; (e) True • (a) Although this has been claimed in the past, a review of the literature reveals no evidence to support this. (b–e) Gastro-oesophageal reflux is due to the relaxation of the lower oesophageal sphincter.The upper oesophageal sphincter is made up from striated muscle which is not affected by progesterone and therefore maintains its tone. Only under sedation or general anaesthesia and muscle relaxation is upper oesophageal sphincter tone lost and aspiration of gastric contents becomes a danger. 25. The following changes to the coagulation system are normal in pregnancy: • (a) The platelet count decreases to 50 000 mm–3. • (b) Parturients are hypercoagulable. • (c) There is decreased fibrinolysis. • (d) Platelet function increases in pregnancy. • (e) Clotting screens will usually be reported as normal. 25. The following changes to the coagulation system are normal in pregnancy: (a) False; (b) True; (c) False; (d) False; (e) True • (a) Although the platelet count decreases in pregnancy it is only <100 000 mm–3 in 2% of parturients. • (b–e) There is an increase in most coagulation factors and the coagulation system is activated. As a result of increased coagulation, there has to be increased fibrinolysis. Platelet function remains normal throughout pregnancy. It is activity and consumption that are increased. In routine clotting tests, the changes to the coagulation system are not detected.