* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download toxoplasmosis new
Lyme disease wikipedia , lookup
Henipavirus wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Anaerobic infection wikipedia , lookup
Hookworm infection wikipedia , lookup
Herpes simplex wikipedia , lookup
Cysticercosis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Tuberculosis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
West Nile fever wikipedia , lookup
Chagas disease wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Brucellosis wikipedia , lookup
Hepatitis C wikipedia , lookup
Plasmodium falciparum wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Leishmaniasis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Hepatitis B wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Neonatal infection wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Trichinosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Leptospirosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Fasciolosis wikipedia , lookup
Toxoplasma gondii wikipedia , lookup
Toxoplasmosis wikipedia , lookup
Sarcocystis wikipedia , lookup
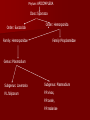
Phylum: APICOMPLEXA
Class: Sporozoa
Order: Eucoccida
Family: Hemosporidae
Order: Hemosporida
Family:Piroplasmidae
Genus: Plasmodium
Subgenus: Laverania
Subgenus: Plasmodium
P.L.faliparum
P.P.vivax,
P.P.ovale,
P.P.malariae
Order Eucocoida
Suborder Adeleina Eimeriina
haemosporina
Family Eimeridae
Eimeria
Isospora
Toxoplasma
Isospora belli
Toxoplasma gondii
What is toxoplasmosis?
A Zoonotic Infection of Humans
Toxoplasma gondii is a sporazoan of the
subclass Coccidia. The only species is Gondii.
It is a common intracellular protozoan which
infects most species of warm-blooded animals
Toxoplasmosis is an infection that can threaten
the health of an unborn child
Morphology
It exists in three forms—
tachyzoites (trophozoites),
tissue cysts,
oocytes.
Sources of infection
Source of all oocytes ...
– Domestic (cats,dogs) and wild (zoo) cats
( Cats are the only known full-life-cycle host of
the protozoan) parasite
– Rodents :rats
Persist in environment (soil)
– reservoir of infective oocytes
if moist
Many intermediate hosts
– reservoir of infective tissue cysts( farm
animals— cattle, sheep, rabbit)
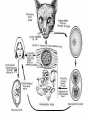
Life cycle – Enteroepithelial /
enteric
•
asexual and sexual division is intracellular in
epithelial cells of small intestine (ileum)
Oocytes
•
oocytes become infective after passage in feces
(Oocytes do not become infectious until they
sporulate. Depending on conditions such as
temperature, sporulation occurs 2 to 21 days
after the oocyte is excreted in the feces )
Sporoblast formation
2 sporocysts in each Mature oocyte
Infect cats
Sporozoites liberated in intestine
Intracellular multiplication in ileum
Endozoite formation
Gametogony – micro & Macrogamete
formation
Fertilization – zygote – Oocyte
Few endozoites enter extraintestinal
tissues & form tissue cysts
Life cycle in Humans
Ingestion of Oocytes
Sporozoites liberated in small intestine
Intracellular multiplication – endozoites
Infect intestinal & other tissues /
transplacental infection
Pseudocyst
Endozoites – bradyzoites – Tissue cyst
Clinical features
Toxoplasma gondii can cause a wide spectrum of
disease after infecting a new host, including
acute, latent, and reactivated disease as well as
congenital disease
Congenital toxoplasmosis
Maternal toxoplasmosis
+ inapparent—subclinical--usually is asymptomatic —
most of cases
+apparent ( 10-20 %)—not specific
Generalized
—flue like illness- fever,fatigue,weakness,malaise
Lymphatic
-
fever,
(retroperitoneal,
generalised
mesentric
lymphadenopathy
{abdominal
pain},
lumbar, occiptal), liver and spleen enlargement The
lymphadenitis may wax and wane for months and
finally
resolve
spontaneously.
It
is
mistaken with infectious mononucleosis).
commonly
neurological --- encephalopathy,
chorioretinitis
Exanthematous -- generalized
maculopapular erythramatous patches
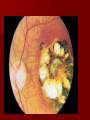
Ocular --- eye pain, Photophobia,
blurred vision, scotoma
("blind
spot"), chorioretinitis, Retinitis,
blindness
The
acute acquired form however,
can be a fulminating disease with an
erythematous rash, fever, malaise,
myositis, dyspnea, acute
myocarditis,and encephalitis.
Outcome can be fatal, but this form
of toxoplasmosis is rare
Congenital infections
in unexposed mother with an active primary
infection during pregnancy or previously
exposed mother before pregnancy with immune
compromise eg : (AIDS ) very rare
tachyzoites cross placental barrier
fetus becomes infected only about 40% of time
when mothers are infected in the first trimester,
15 percent of fetuses become infected,as
compared to 30 percent in the second trimester
and 65 percent in the third trimester.
the earlier in pregnancy the infection occurs, the
more severe the fetal infection.
Congenital Toxoplasmosis
Two types:
Asymptomatic (inapparent) Congenital Toxo
60% of infected
may suffer from Long Term Sequella
up to 90 percent of infected babies appear normal at
birth,
80 to 90 percent will develop sight-threatening eye
infections months to years after birth.
About 10 percent will develop hearing loss and/or
learning disabilities
Symptomatic Congenital Toxo
40% of infected—
About one in 10 infected
These newborns often have severe eye infections,
an enlarged liver and spleen, jaundice (yellowing
of the skin and eyes), pneumonia and other
problems.
Some die within a few days of birth.
Those who survive sometimes suffer from mental
retardation, severely impaired eyesight, cerebral
palsy, seizures and other problems.
more likely if mother infected in 1st/2nd Trimester
Severe damage to fetus = stillbirth or abortion
Lab Diagnosis
Morphologic
– tachyzoites in circulating WBC, bone marrow, lung,
spleen, brain ?
– histopathologic examination
Culture or animal inoculation (rare)
Isolation of parasites from blood or other body fluids, by
intraperitoneal inoculation into mice or tissue culture.
The mice should be tested for the presence of
Toxoplasma organisms in the peritoneal fluid 6 to 10 days
post inoculation; if no organisms are found, serology can
be performed on the animals 4 to 6 weeks post
inoculation.
Pseudocyst
Serologic Diagnosis of Toxo
unreliable in immunodeficient (AIDS) pts
normally IgM and IgG rise simultaneously
– IgG - persists for years
– IgM - undetectable after “cure”
elevated IgM titer is diagnostic of recent infection in persons
with normal immunity
disseminated infection may exist in AIDS pts without
demonstrable titer
A negative IgG or IgM test excludes Diagnosis
– both should be + if acutely infected
If IgG screening is + then do IgM test
– a + IgM test confirms acute toxoplasmosis or current Toxoplasma
infection
Tests which employ whole parasites include
the dye test (Sabin-Feldman Dye Test (DT)
direct agglutination and the fluorescent
antibody test,
whilst tests that use disrupted parasites as
an antigen source include ELISA, latex
agglutination, indirect haemagglutination
and complement fixation.
Polymerase Chain Reaction
(PCR)
PCR amplification is used to detect T. gondii
DNA in
body fluids and tissues
brain tissue
cerebrospinal fluid (CSF)
vitreous and aqueous fluid
bronchoalveolar lavage (BAL) fluid
urine
amniotic fluid
peripheral blood.
Treatment:
No treatment in Asymptomatic Because it is self
limiting disease Except in children to prevent retinal
inflammation
In healthy people, infection with Toxoplasma gondii,
leads to the production of sarcocysts in various tissues
and immunity to additional infections. Thus, an infected
but asymptomatic person in good health generally does
not need treatment.
Treatment of pregnant women is controversy because
of toxicity of medication but is still advocated
Treatment of Infected Newborns
Infected babies should be treated as soon
as possible after birth with pyrimethamine
and sulfadiazine which, as mentioned
earlier, can help prevent or reduce the
disabilities associated with toxoplasmosis.
Treatment
pyrimethamine + sulfadiazine
– High-dose therapy is continued for 4-6 weeks, and
lower dose maintenance therapy is given thereafter.
– Spiramycin
• pyrimethamine + clindamycin or dapsone
Prophylaxis –in the primary prevention of
toxoplasmosis in persons with HIV who have
dormant or latent infection
TMP-SMX - trimethoprim-sulfamethoxazole
• pyrimethamine plus folinic acid
• dapsone + pyrimethamine
Prevention of Toxoplasmosis
education
avoiding exposure to the parasite, mostly
by simple hygienic measures.
avoid exposure to oocyte
– wash hands carefully after handling raw meat, fruit,
vegetables, and soil
Babesiosis
• Babesiosis (piroplasmosis) is a hemolytic
disease similar to malaria but without an
exoerythrocytic cycle.
• Disease caused by B. divergens can be
severe, even fatal, in splenectomized and
debilitated patients (Most patients are
older than 50 years of age).
• B. microti causes a self-limiting febrile
disease characterized by fatigue and
anorexia.
Babesia
• There are >100 species of this intracellular parasite.
• The disease caused by Babesia known as Babesiosis
• The disease distribute all over the world where there is
tick available.
• Babesia microti is the predominant human pathogen,
endemic to the NE and Midwest.
• Natural parasite reservoir is rodents
• Its common among dogs, cattle , goats, sheep, horses
and rodents
• Human infect during cattle (B. bovis) rodent (B. microti)
• Carried by the hard-bodied Ixodes tick.
• more severe in patients who are immunosuppressed,
splenectomized, and/or elderly
B. bigemina
Cattel
B. motasi
Sheep
B. equi
Horses
B. Caballi
Horses
The parasites reproduce by binary fission inside the
R.B.Cs, after transmission with the tick saliva.
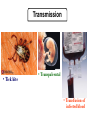
Transmission
• Tick bite
• Transpalcental
• Transfusion of
infected blood
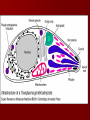
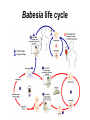
Babesia life cycle
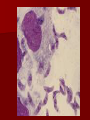
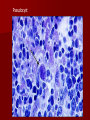
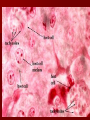
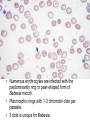
• Numerous erythrocytes are infected with the
predominantly ring or pear-shaped form of
Babesia microti.
• Pleomorphic rings with 1-3 chromotin dots per
parasite.
• 3 dots is unique for Babesia.
Clinical Symptoms
• Ranges from asymptomatic infection to fatal
illness (rare)
• More severe infection tends to occur in
immunnocompromised, elderly, and the very
young.
• The extreme end of the spectrum is often
described as a malaria-like infection; symptoms
may include
Fever, sweating, chills, headache, anemia,
jaundice, malaise, haemoglobinuria &
Weakness.
Diagnosis
• Diagnosis is based on clinical suspicion and history of
exposure.
• Thick and thin smears remain most clinically used
• However, it is necessary to examine 200 to 300 oil
immersion fields before declaring a specimen
negative.
• Various PCR detection assays are available for
detection of B microtic and other species.
• More sensitive but also more time consuming and
expensive.
• Indirect fluorescent antibody test can also be used as
a confirmatory test.
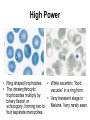
High Power
• Ring shaped trophozites
• White eccentric “food
• The intraerythrocytic
vacuole” in a ring form.
trophozoites multiply by
• Very transient stage in
binary fission or
Malaria. Very rarely seen.
schizogony, forming two to
four separate merozoites. .
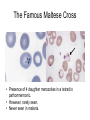
The Famous Maltese Cross
• Presence of 4 daughter merozoites in a tetrad is
pathomnemonic.
• However, rarely seen.
• Never seen in malaria.
Multiply Infected RBCs
• RBCs can be infected with multiple organisms at the same
time. Up to 12 parasites may infect a single RBC.
• Plasmodium has up to 3 parasites/RBC.
Control and prevention
1. One should avoid tick exposure and, if bitten,
remove the tick from the skin immediately.
2. Treatment of infected animals with available
drugs .
3. Use of the Acaricides regularly & periodically
in the endemic area.