* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Fetal CHF
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Jatene procedure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
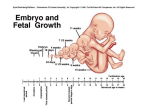
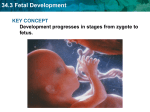
Fetal Congestive Heart Failure Shabib Alhadheri, MD Fetal Anatomy & Physiology • Brain and heart get highest oxygenated blood (from UV) • Lower body gets less oxygenated blood (from RV) • Pulmonary = systemic pressure • Lowest flow at aortic isthmus • Both lungs receive only 10% of CO and have the highest vascular resistance • Since the blood is oxygenated in the placenta, the O2 sat in the IVC (70%) is higher than that in the SVC (40%) • The highest pO2 is found in the umbilical vein (32 mmHg) Fetal Circulation • Parallel circulations • Mixing of venous returns • High resistance of the pulmonary circulation • Low resistance of the placental circulation • Presence of shunts • Right ventricular dominance • Non-compliant behavior of ventricular filling in utero • Limited range of HR over which CO can be maintained Fetal Circulation Fetal Myocardium • Fetal myocardial fibers generate less active tension when compared to adults • Resting tension is higher in fetal cells • Higher proportion of non-contractile proteins in fetal cells Fetal Myocardium • The RV is the dominant ventricle ejecting the combined CO into the descending aorta • The LV supplies a more highly saturated yet smaller proportion of combined CO to coronaries, head, brain and forelimbs • The fetal ventricles are limited in their ability to increase stroke volume in response to increased HR Fetal Hemodynamics • Fewer contractile elements affects diastolic performance • Atrioventricular valve E:A ratio – < 1 in utero – ~ 1 near term – > 1 postnatally • Maturation improves ventricular relaxation Foramen Ovale Restriction • • • • Progressive right atrial enlargement RV dilation and hypertrophy, MPA/DA enlargement Reduced growth of the left heart PDA Constriction • May occur naturally but more commonly seen in maternal prostaglandin inhibitors ingestion • Results in RV pressure overload, hydrops fetalis • On Echo: – elevated peak systolic flow velocities across DA (> 1m/s); associated high diastolic flow velocity – Associated with TR; increased MPA pressure • Severity related to amount of elevated diastolic velocity of the pulmonary artery Transitional Circulation • Cord is clamped, baby cries – Systemic vascular resistance (SVR) jumps – LV end diastolic pressure (LVEDP) increases – Lungs expand – Pulmonary capillaries see high pO2 – Pulmonary vascular resistance (PVR) falls – Ductus arteriosus constricts Causes of Fetal CHF Fetal tachy/bradyarrhythmias Anemia/hemoglobinopathy Fetal systemic infection/myocarditis (parvovirus) Congenital heart disease with valvular regurgitation • Non-cardiac malformations e.g. diaphragmatic hernia or cystic hygroma • Twin-twin transfusion recipient volume and pressure overload • Atrioventricular fistula with high cardiac output • • • • What You Need To Know? Fetal heart rate Cardiomegaly Myocardial function Pulsed Doppler evaluation of the IVC Pulsed Doppler of the umbilical cord Color and pulsed Doppler of the cardiac valves • Evidence for hydrops fetalis • • • • • • Fetal Heart Rate • Bradycardia – Mechanical PR interval – Complete heart block • Tachycardia – SVT – Atrial flutter HR… M-Mode HR… Doppler Study Supraventricular Tachycardia (SVT) Atrial Flutter Complete Heart Block Cardiomegaly • The most common cardiac chamber to show enlargement is the right atrium • C/T area ratio = cardiac area/chest area (normal 0.25-0.35) • C/T circumference ratio = cardiac circ/chest circ (normal <0.5) Myocardial function • Decreased fractional shortening • Valvular regurgitation Myocardial Performance Index (MPI) (Tei Index) • Using the filling time of AV valve and ejection time of the ventricle Normal values at 18-31 weeks gestation -TI 0.53+/- 0.13 -ICT 43+/- 14ms -IRT 48+/- 13ms -ET 173+/- 16 ms Friedman et al; Ultrasound in Obst & Gyn, Vol 21 issue 1, 33-36, Jan 2003 Myocardial Performance Index (MPI) • A ventricular geometry-independent measure of combined systolic and diastolic ventricular performance • Obtained by Doppler sampling of inflow and outflow across the ventricle measuring the time intervals relating to isovolumic contraction (ICT), isovolumic relaxation (IRT), and ventricular ejection (ET) Tricuspid Regurgitation • The true BP and ventricular cavity pressure in the human fetus is unknown • The typical peak systolic pressure for a newborn premature infant born at 24 weeks’ gestation is ~ 30-40 mmHg • The normal fetal heart in series with the low placental vascular resistance, the fetal pressure should be less • Therefore, elevated RVp reflects increased vascular resistance Pulsatility Index • A Doppler-derived measure of placental vascular resistance (PVR) • Obtained by Doppler interrogation of the umbilical artery • Calculated as maximum systolic – end-diastolic velocity/ mean velocity (normal mean 2.46 +/0.52) • When there is a low, absent, or even reversed diastolic flow velocity at end-diastole, this suggests a very high PVR Abnormal Doppler Pattern • As the ventricles become more stiff (less compliant), the Doppler parameters of ventricular filling begin to change • The normal double-peak inflow pattern (passive filling “E wave” and active atrial filling “A wave”) fuse into a singlepeak Abnormal Venous Doppler • Reversal away from the heart during atrial contraction is a sign of increased end-diastolic pressure in the ventricles of the failing heart • Increased atrial reversal in the inferior vena cava • Ductus venosus atrial reversal • Umbilical venous atrial pulsations (diastolic block… predicts perinatal mortality) Abnormal Doppler Pattern • Ductus venosus flow during atrial contraction diminishes, often becoming absent or reversed in case of a very stiff, noncompliant right ventricle • Pulsations in the umbilical vein reflects a severe degree of impediment to ventricular filling (diastolic dysfunction) Inferior Vena Cava Flow Normal fetus with a small amount of flow reversal A fetus with poor RV compliance showing an increased degree of flow reversal Ductus Venosus Flow Normal flow pattern with continuous forward flow Some reversal flow (arrows), suggesting a stiff abnormal heart Umbilical Cord Doppler Normal pattern - Pulsatile umbilical artery flow - Continuous venous flow UA UV Decreased diastolic velocity with reversal flow (arrows) with pulsatile venous flow, suggestive of elevated placental vascular resistance Inflow Patterns Fetal Post-Natal Inflow Pattern Double-peak Single-peak TV Hydrops Fetalis • Imbalance between supply and demand • Development of abnormal fluid collection in the fetus, in more than one site – Abdomen (ascites) – Pleural or pericardial space (effusion) – Skin (subcutaneous edema “>5mm thickness”) Non-Immune Hydrops Fetalis… Causes Etiology / Pathogenesis: Percent Cardiovascular ( NIHF via CHF) Chromosomal abnormalities 17 – 35 % 14 – 16 % (e.g. Turner, Noonan syndromes) 4 – 12 % Hematologic (NIHF 20 severe fetal anemia leading to high output cardiac failure) Norton et al., 1994 Fetal Hydrops-Pleural/Pericardial Effusions Fetal Hydrops-Ascites Fetal Hydrops-IVC flow reversal Fetal Hydrops-UV pulsations Summary • Redistribution of cardiac output – Absent end diastolic flow in umbilical artery with brain sparing • Cardiomegaly • Abnormal venous Doppler – Flow reversal in IVC – Umbilical venous pulsations • Abnormal myocardial function – Decreased shortening fraction – Valvular regurgitation James Huhta, Seminars in Fetal & Neonatal Medicine (2005) 10, 542-552 Thank You