* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Spontaneous baroreflex control of cardiac output during dynamic
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
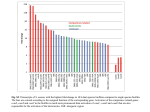
Am J Physiol Heart Circ Physiol 294: H1310–H1316, 2008. First published January 11, 2008; doi:10.1152/ajpheart.01187.2007. Spontaneous baroreflex control of cardiac output during dynamic exercise, muscle metaboreflex activation, and heart failure Masashi Ichinose,1,3 Javier A. Sala-Mercado,1 Donal S. O’Leary,1 Robert L. Hammond,1,2 Matthew Coutsos,1 Tomoko Ichinose,1,4 Marco Pallante,5 and Ferdinando Iellamo5,6 Departments of 1Physiology and 2Surgery, Wayne State University School of Medicine, Detroit, Michigan; 3Laboratory for Applied Human Physiology, Faculty of Human Development, Kobe University, Kobe, Japan; 4Laboratory for Human Performance Research, Osaka International University, Osaka, Japan; and 5Dipartimento Medicina Interna, Universita di Roma Tor Vergata, and 6Instituto di Ricovero e Cura a Carattere Scientifico San Raffaele Pisana, Roma, Italy Submitted 11 October 2007; accepted in final form 16 December 2007 THE ARTERIAL BAROREFLEX is considered the main mechanism of arterial blood pressure regulation in the short-term control of the cardiovascular system (30). Changes in arterial pressure result in baroreflex-mediated reciprocal changes in heart rate (HR) and sympathetic activity. During exercise, the baroreflex is reset to operate around the higher-prevailing blood pressure and HR (7, 13, 26, 28). In addition to resetting during exercise, arterial baroreflex sensitivity in the control of HR during rapid spontaneous changes in blood pressure decreases during exercise as workload rises (3, 14, 23, 31). The reduction of baroreflex HR sensitivity during exercise is thought to be associated with vagal withdrawal, inasmuch as these rapid baroreflex changes in HR are mediated by changes in parasympathetic tone (23). Recently, it has been demonstrated (31) in dogs that imposed muscle metaboreflex activation during dynamic exercise also reduces spontaneous baroreflex HR sensitivity, which is even further suppressed in these settings in subjects with congestive heart failure (HF) (16). Although the spontaneous baroreflex HR technique has often been used to study baroreflex control of HR (2, 3, 14, 23, 29), Sala-Mercado et al. (33a) in the accompanying article have shown that these baroreflex-mediated changes in HR do not always cause changes in cardiac output (CO) due to changes in stroke volume (SV). This study showed that in the normal dog at rest, ⬃44% of the changes in HR caused changes in CO (HR-CO translation or coupling). In addition, HF significantly decreased this coupling such that changes in CO were more related to changes in SV than to changes in HR. Whether dynamic exercise with and without muscle metaboreflex activation alters the ability of spontaneous baroreflex-mediated changes in HR to cause changes in CO is unknown, as is whether these relationships are affected by HF. Since exercise changes cardiac autonomic balance, markedly increasing baseline HR and decreasing spontaneous baroreflex HR sensitivity (15), we hypothesized that the ability of the baroreflex HR responses to elicit compensatory changes in CO would also be decreased. Although spontaneous baroreflex HR sensitivity decreases further with metaboreflex activation (31), substantial increases in ventricular contractility also occur (6, 21, 33), which could attenuate any further loss of coupling between the HR and CO responses. However, in subjects with HF, muscle metaboreflex-induced increases in ventricular contractility are severely impaired (5, 32). Therefore, we also hypothesized that muscle metaboreflex activation would not decrease the coupling between changes in HR and CO in normal subjects, but with the impaired ventricular performance in HF, we hypothesized that metaboreflex activation in this setting would induce further decreases in the ability of changes in HR to elicit changes in CO. Address for reprint requests and other correspondence: D. S. O’Leary, Dept. of Physiology, Wayne State Univ. School of Medicine, 540 E. Canfield Ave., Detroit, MI 48201 (e-mail: [email protected]). The costs of publication of this article were defrayed in part by the payment of page charges. The article must therefore be hereby marked “advertisement” in accordance with 18 U.S.C. Section 1734 solely to indicate this fact. arterial baroreflex sensitivity; exercise reflexes; pressor response; impaired cardiac performance H1310 0363-6135/08 $8.00 Copyright © 2008 the American Physiological Society http://www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 Ichinose M, Sala-Mercado JA, O’Leary DS, Hammond RL, Coutsos M, Ichinose T, Pallante M, Iellamo F. Spontaneous baroreflex control of cardiac output during dynamic exercise, muscle metaboreflex activation, and heart failure. Am J Physiol Heart Circ Physiol 294: H1310–H1316, 2008. First published January 11, 2008; doi:10.1152/ajpheart.01187.2007.—We have previously shown that spontaneous baroreflex-induced changes in heart rate (HR) do not always translate into changes in cardiac output (CO) at rest. We have also shown that heart failure (HF) decreases this linkage between changes in HR and CO. Whether dynamic exercise and muscle metaboreflex activation (via imposed reductions in hindlimb blood flow) further alter this translation in normal and HF conditions is unknown. We examined these questions using conscious, chronically instrumented dogs before and after pacing-induced HF during mild and moderate dynamic exercise with and without muscle metaboreflex activation. We measured left ventricular systolic pressure (LVSP), CO, and HR and analyzed the spontaneous HR-LVSP and CO-LVSP relationships. In normal animals, mild exercise significantly decreased HR-LVSP (⫺3.08 ⫾ 0.5 vs. ⫺5.14 ⫾ 0.6 beats 䡠 min⫺1 䡠 mmHg⫺1; P ⬍ 0.05) and CO-LVSP (⫺134.74 ⫾ 24.5 vs. ⫺208.6 ⫾ 22.2 ml 䡠 min⫺1 䡠 mmHg⫺1; P ⬍ 0.05). Moderate exercise further decreased both and, in addition, significantly reduced HR-CO translation (25.9 ⫾ 2.8% vs. 52.3 ⫾ 4.2%; P ⬍ 0.05). Muscle metaboreflex activation at both workloads decreased HR-LVSP, whereas it had no significant effect on CO-LVSP and the HR-CO translation. HF significantly decreased HR-LVSP, CO-LVSP, and the HR-CO translation in all situations. We conclude that spontaneous baroreflex HR responses do not always cause changes in CO during exercise. Moreover, muscle metaboreflex activation during mild and moderate dynamic exercise reduces this coupling. In addition, in HF the HR-CO translation also significantly decreases during both workloads and decreases even further with muscle metaboreflex activation. H1311 BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS Table 1. Hemodynamic values at rest, during mild exercise and MRA at mild exercise, in N and in the same animals after induction of HF Condition, Setting HLBF, l/min LVSP, mmHg CO, l/min SV, ml N, rest N, mild free-flow exercise N, mild exercise ⫹ MRA HF, rest HF, mild free-flow exercise HF, mild exercise ⫹ MRA 0.81⫾0.09 1.17⫾0.11† 0.63⫾0.05‡ 0.47⫾0.07* 0.76⫾0.08*† 0.60⫾0.07‡ 131.8⫾5.4 133.4⫾5.4 178.3⫾5.5‡ 102.0⫾5.5* 109.4⫾4.8* 140.0⫾6.8*‡ 4.52⫾0.32 6.06⫾0.45† 7.33⫾0.52‡ 3.46⫾0.31* 4.32⫾0.33*† 4.60⫾0.47* 42.2⫾3.4 46.7⫾3.6† 48.7⫾3.8‡ 27.0⫾2.5* 27.7⫾2.8* 24.9⫾2.4*‡ CO-LVSP SV-LVSP HR, beats/ HR-LVSP Incidence, Incidence, Incidence, min sequences/100 beats sequences/100 beats sequences/100 beats 108⫾5 131⫾3† 152⫾5‡ 130⫾6* 159⫾7*† 184⫾7*‡ 9.3⫾1.5 6.5⫾1.1† 6.2⫾0.9 6.1⫾0.8* 3.0⫾0.6*† 2.7⫾0.6* 6.3⫾0.9 4.6⫾0.4† 4.5⫾0.4 3.8⫾0.6* 3.0⫾0.5* 2.9⫾0.5* 1.6⫾0.2 1.8⫾0.4 2.1⫾0.5 2.8⫾0.4* 2.9⫾0.6* 3.0⫾0.2* MATERIALS AND METHODS Experiments were performed on eight adult, mongrel dogs (weight, ⬃20 –25 kg) of either sex, selected for their willingness to run on a motor-driven treadmill. The protocols employed in the present study conform with the National Institutes of Health guidelines and were reviewed and approved by the Wayne State University Animal Investigation Committee. Surgical preparation and procedures. All animals were accustomed to human handling and trained to run freely on a motor-driven treadmill before they were surgically instrumented in two different procedures (sternotomy and left flank abdominal surgery). The first surgical session with its pre- and postpharmachological treatments have been previously described in detail by Sala-Mercado et al. (33a). Briefly, under sterile conditions, a midline sternotomy was performed. A telemetered blood pressure transducer (model PAD-70, Data Sciences International) was placed subcutaneously on the left side of the chest. Its catheter was tunneled into the thoracic cavity and located inside the left ventricle for measuring left ventricular pressure (LVP). A 20- or 24-mm blood flow transducer (Transonic Systems) was placed around the ascending aorta to measure CO, and three stainless steel ventricular pacing electrodes (O-Flexon, Ethicon) were sutured to the right ventricular free wall. For studies unrelated to the present investigation, vascular occluders were placed on the superior and inferior venous cava and two pairs of sonomicrometry crystals were placed on the left ventricular endocardium. The pericardium was reapproximated loosely, and the chest was closed in layers. After at least 10 days (recovery period), a second surgical intervention was performed through a left abdominal retroperitoneal approach (33a). A 10-mm blood flow probe (Transonic Systems) was placed on the terminal aorta to measure blood flow to the hindlimbs (HLBF). A hydraulic vascular occluder (DocXS Biomedical Products) was placed on the terminal aorta just distal to the flow probe. All arteries branching from the aorta between the iliac arteries and the HLBF probe were ligated and severed, and a catheter was placed through a lumbar artery proximal to the HLBF probe and occluder to measure mean arterial pressure (MAP). All cables, wires, occluder tubings, and the aortic catheter were tunneled subcutaneously and exteriorized between the scapulae. Experimental procedures. Experiments were performed after the animals had recovered completely (i.e., alert, afebrile, active, and of good appetite) from the second surgical session (7 days). Before every experiment, each animal was transported to the laboratory and allowed to roam freely for 15–30 min and then was directed to the treadmill. The CO and HLBF transducers were connected to the flow meters (Transonic System). HR was computed by a cardiotachometer triggered by the CO signal. The LVP signal was checked, and the arterial catheter was connected to a pressure transducer (Transpac IV, Abbott). All data were recorded on analog-to-digital recording systems for subsequent off-line analyses. For a given experimental session, data were collected at rest and then at a randomly selected workload (mild exercise, 3.2 km/h, 0% grade elevation; or moderate exercise, 6.4 km/h, 10% grade elevation). Only one workload was performed on any experimental day. All animals ran freely with only positive verbal encouragement. Steady-state data were recorded at rest while the animal was standing on the treadmill, during exercise with unrestricted blood flow to the hindlimbs and after metaboreflex activation elicited by reductions in HLBF achieved by partial inflation of the terminal aortic occluder as previously described (37). Each dog completed several experiments at both workloads. After the completion of the control experiments, modest congestive HF was induced via rapid ventricular pacing as previously described by us and others (25, 32). Briefly, the heart was paced at 240 –250 beats/min for ⬃ 30 days, and the experiments were repeated while in modest HF conditions [defined as resting tachycardia, reduced CO, SV, and maximum Table 2. Hemodynamic values at rest, during moderate exercise and MRA at moderate exercise, in N and in the same animals after induction of HF Condition, Setting HLBF, l/min LVSP, mmHg CO, l/min SV, ml HR, beats/min HR-LVSP Incidence, sequences/ 100 beats N, rest N, moderate free-flow exercise N, moderate exercise ⫹ MRA HF, rest HF, moderate free-flow exercise HF, moderate exercise ⫹ MRA 0.81⫾0.09 2.55⫾0.15† 1.87⫾0.14‡ 0.47⫾0.07* 1.92⫾0.19*† 1.55⫾0.19‡ 131.8⫾5.4 147.9⫾5.9† 186.3⫾6.9‡ 102.0⫾5.5* 132.6⫾7.3*† 160.5⫾12.0*‡ 4.52⫾0.32 8.84⫾0.55† 10.16⫾0.63‡ 3.46⫾0.31* 6.80⫾0.59*† 7.14⫾0.78* 42.2⫾3.4 48.3⫾3.8† 52.4⫾4.1‡ 27.0⫾2.5* 35.2⫾3.1*† 34.2⫾3.5* 108⫾5 186⫾7† 197⫾7‡ 130⫾6* 194⫾3*† 208⫾4*‡ 9.3⫾1.5 6.0⫾0.8† 4.9⫾0.7 6.1⫾0.8* 1.8⫾0.2*† 2.4⫾0.3* CO-LVSP Incidence, sequences/ 100 beats SV-LVSP Incidence, sequences/ 100 beats 6.3⫾0.9 3.6⫾0.4† 3.3⫾0.3 3.8⫾0.6* 2.2⫾0.4* 2.2⫾0.2* 1.6⫾0.2 2.2⫾0.3 2.3⫾0.2 2.8⫾0.4* 2.9⫾0.1* 3.4⫾0.7* Values are means ⫾ SE; number of animals are the same as in Table 1. *P ⬍ 0.05, HF vs. N; †P ⬍ 0.05, free-flow exercise vs. rest; ‡P ⬍ 0.05, free-flow exercise ⫹ MRA vs. free-flow exercise. AJP-Heart Circ Physiol • VOL 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 Values are means ⫾ SE. MRA, metaboreflex activation; HF, heart failure; HLBF, hindlimb blood flow; LVSP, left ventricular systolic pressure; CO, cardiac output; SV, stroke volume; HR-LVSP incidence, number of spontaneous baroreflex HR sequences; CO-LVSP incidence, number of spontaneous CO-LVSP relationships; SV-LVSP incidence, number of spontaneous SV-LVSP relationships. For HLBF, n ⫽ 7 animals; for all other values, n ⫽ 8 normal animals (N) and n ⫽ 7 HF animals. *P ⬍ 0.05, HF vs. N; †P ⬍ 0.05, free-flow exercise vs. rest; ‡P ⬍ 0.05, free-flow exercise ⫹ MRA vs. free-flow exercise. H1312 BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS RESULTS Fig. 1. Average values of heart rate (HR)-left ventricular systolic pressure (LVSP) (A), cardiac output (CO)-LVSP (B), and stroke volume (SV)-LVSP (C) at rest and during mild and moderate (Mod) exercise with and without muscle metaboreflex activation (MRA) in normal (N) and heart failure (HF) condition. *P ⬍ 0.05, significant difference between N and HF; †P ⬍ 0.05, free-flow exercise vs. rest; ‡P ⬍ 0.05 exercise ⫹ MRA vs. free-flow exercise. and minimum first derivative of left ventricular pressure, as described in our previous studies (11, 16, 32)]. Data analysis. Each animal served as its own control. During the experiments, beat-to-beat CO, HLBF, HR, MAP, and LVP were collected continuously. Data were recorded for 3 to 5 steady-state min to include several respiratory cycles. In the companion article by Sala-Mercado et al. (33a), we have described in detail how we assessed the HR-LVSP and CO-LVSP. Briefly, since left ventricular systolic pressure (LVSP) is virtually identical to the aortic arch systolic blood pressure, we used LVSP as the input to the arterial baroreflex. We searched for three or more consecutive beats (sequences) in which the LVSP and HR or CO of the following beat changed in the opposite directions. Subsequently, a linear regression was applied to each individual sequence, and only those in which r2 was ⬎0.85 were accepted and a slope was calculated. By averaging all slopes, we obtained the mean slope of the HR-LVSP and COLVSP relationships within a given test period. By computing the overlap between HR sequences and CO sequences, we examined the AJP-Heart Circ Physiol • VOL Table 1 shows the average values of HLBF, LVSP, CO, SV, HR, and normalized number of spontaneous baroreflex HR, CO, and SV-LVSP sequences (HR-, CO-, SV-LVSP incidences) at rest and during mild workload before (free flow) and after muscle metaboreflex activation in normal and HF conditions. Table 2 shows the same measurements during moderate exercise. The cardiovascular responses to exercise and muscle metaboreflex activation before and after induction of HF were essentially the same as we have reported in previous studies (1, 10, 32). Briefly, metaboreflex activation caused substantial increases in HR, CO, and LVSP at both workloads. After the induction of HF, CO and LVSP were significantly depressed Fig. 2. The relationship between HR-LVSP and CO-LVSP in N and HF conditions. Group average data during each setting in N condition (F) and group average data during each setting in HF condition (E) are shown. The lines represent the regression line. 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 translation or coupling of baroreflex HR responses into CO responses. We consider complete overlap when HR and CO sequences completely overlapped, and partial overlap when the sequences overlapped by at least two beats (thus partial overlap includes those which completely overlapped). The proportion of complete and partial overlap to the total number of HR and CO sequences was calculated, respectively. We also calculated the spontaneous changes in SV and the percentage of CO sequences that completely or partially overlapped with SV sequences. Since not all baroreflex HR responses caused compensatory changes in CO due to reciprocal changes in SV, we further analyzed each baroreflex sequence and calculated within each sequence the absolute amount of reciprocal change in SV per change in HR (expressed as ml/beat) and the percentage of the HR sequences associated with the reciprocal changes in SV at each setting in normal and HF conditions. Statistical analysis. With the use of the averaged responses for each animal, statistical analyses were performed on the data with Systat software (Systat 11.0). An ␣-level of P ⬍ 0.05 was set to determine statistical significance. Two-way analysis of variance for repeated measures was used for comparing hemodynamic data obtained at rest [resting data before moderate exercise; those data at rest before mild exercise were used in the accompanying article (33a)], during each workload before and after muscle metaboreflex activation, in normal and HF conditions. If a significant interaction term was found, a test for simple effects post hoc analysis (CMatrix) was performed to determine significant group mean differences. In figures and text, data are expressed as means ⫾ SE and reflect data from eight animals in normal state, with n ⫽ 7 animals in HF. BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS setting. Mild and moderate exercise decreased both HR-LVSP and CO-LVSP as in normal animals. In HF, muscle metaboreflex activation caused a further slight yet significant decrease in HR-LVSP, whereas it did not alter CO-LVSP at both workloads. SV-LVSP was low and did not vary across settings or in HF. Figure 2 shows that there were close linear relationships between HR-LVSP and CO-LVSP, both before and after induction of HF; however, the slope of the linear regression line in HF was markedly diminished compared with that in the normal state, indicating that even at the same HR-LVSP, the CO-LVSP was smaller in HF. Figure 3 shows the percentage of partial and complete overlap of HR sequences with CO sequences (Fig. 3, A and B), of CO sequences with HR sequences (Fig. 3, C and D), and of CO sequences with SV sequences (Fig. 3, E and F) at each setting before and after induction of HF. The same conclusions Fig. 3. The proportion of the overlap among HR, CO, and SV sequences. HR-CO partial overlap (A), proportion of the HR sequences overlapped at least 2 beats with CO sequences; HR-CO complete overlap (B), proportion of the HR sequences completely overlapped with CO sequences; CO-HR partial overlap (C), proportion of the CO sequences overlapped at least 2 beats with HR sequences; CO-HR complete overlap (D), proportion of CO sequences completely overlapped with CO sequences; CO-SV partial overlap (E), proportion of the CO sequences overlapped at least 2 beats with SV sequences; CO-SV complete overlap (F), proportion of CO sequences completely overlapped with SV sequences. *P ⬍ 0.05 between N and HF; †P ⬍ 0.05 vs. rest; ‡P ⬍ 0.05 vs. mild exercise; §P ⬍ 0.05 vs. moderate exercise. AJP-Heart Circ Physiol • VOL 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 and the animals were tachycardic. Metaboreflex activation in HF still caused a tachycardia; however, the fall in SV markedly limited any reflex increase in CO. Exercise decreased the incidence of HR-LVSP sequences with no further change with metaboreflex activation both before and after the induction of HF. The incidence of HR-LVSP and CO-LVSP sequences was significantly less in all settings in HF. The SV-LVSP incidence was quite low and did not vary significantly with exercise and metaboreflex activation, although it was significantly increased in all settings in HF. Figure 1 shows the HR-LVSP (Fig. 1A), CO-LVSP (Fig. 1B), and SV-LVSP (Fig. 1C) in each setting. In normal animals, both HR-LVSP and CO-LVSP significantly decreased with mild and moderate exercise. Although muscle metaboreflex activation at both workloads caused a further decrease in HR-LVSP, it had no obvious effect on CO-LVSP. In HF, both HR-LVSP and CO-LVSP were significantly attenuated at each H1313 H1314 BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS AJP-Heart Circ Physiol • VOL Fig. 4. A: percentage of HR sequences associated with reciprocal changes in SV. B: average absolute amount of change in SV per beat (in the HR baroreflex sequences) at each setting in N and HF conditions. *P ⬍ 0.05 between N and HF; †P ⬍ 0.05 vs. rest; ‡P ⬍ 0.05 vs. mild exercise; §P ⬍ 0.05 vs. moderate exercise. DISCUSSION To our knowledge, this is the first study to investigate to what extent the spontaneous baroreflex-induced changes in HR translate into functional changes in CO during dynamic exercise. Furthermore, we investigated the effects of muscle metaboreflex activation on this coupling and how these relationships are affected after the induction of congestive HF. Cardiac baroreflex responses during dynamic exercise and metaboreflex activation in normal subjects. Our results confirm previous studies showing that dynamic exercise attenuates spontaneous baroreflex control of HR (3, 14, 23, 31) and furthermore show that dynamic exercise progressively decreases both HR-LVSP and CO-LVSP as exercise intensity increases. In addition to the attenuation in the gain of cardiac baroreflex responses, we found that dynamic exercise reduces the coupling of the HR responses into CO responses. This reduction in the ability of HR responses to elicit effective changes in CO was due to simultaneous reciprocal changes in SV; that is, as HR increased, often SV fell (and the magnitude of the fall in SV per beat increased), such that CO remained relatively unchanged. The progressive decrease in baroreflex control of HR together with the fewer number of HR responses actually causing effective changes in CO suggests that the contribution of baroreflex-mediated CO responses to blood pressure regulation progressively declines as exercise intensity increases. 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 are reached using either partial or complete overlap. In agreement with the companion article by Sala-Mercado et al. (33a), in normal animals, at rest, ⬃50% of HR sequences overlapped with CO sequences, whereas most of CO sequences overlapped with HR sequences. The CO sequences (either partial or complete) overlapped with SV sequences were around 10% at rest. When compared with rest, HR-CO overlap and CO-HR overlap slightly decreased during mild exercise but significantly decreased with moderate exercise intensity, whereas CO-SV overlap slightly increased at mild exercise and significantly increased at moderate exercise. Furthermore, muscle metaboreflex activation during mild and moderate exercise showed no significant change in HR-CO overlap with respect to the values during exercise before hindlimb ischemia. Muscle metaboreflex activation at mild exercise significantly decreased the CO-HR overlap seen during free-flow exercise, but during moderate exercise muscle, metaboreflex activation had no effect on the CO-HR overlap. Moreover, CO-SV overlap rose significantly during muscle metaboreflex activation at both mild and moderate exercise compared with free-flow exercise. In HF, the HR-CO overlap and CO-HR overlap were significantly decreased and the CO-SV overlap was significantly increased at all settings. HR-CO overlap slightly decreased during mild exercise and significantly decreased at moderate exercise. CO-HR overlap significantly decreased during both mild and moderate exercise. CO-SV overlap progressively increased as exercise intensity increased. Muscle metaboreflex activation during both workloads significantly decreased HR-CO overlap and also tended to decrease CO-HR overlap. In contrast, CO-SV overlap significantly increased during muscle metaboreflex activation at both mild and moderate exercise intensities in HF. Both before and after the induction of HF, HR sequences overlapped with SV sequences were ⬍10% in all the settings, and we observed neither significant changes between settings nor a significant difference between normal and HF states. Figure 4 shows the percentage of the HR sequences associated with reciprocal changes in SV at each setting before and after induction of HF (Fig. 4A), in addition to the change in SV (absolute amount) per beat within the baroreflex sequences (Fig. 4B). In normal animals, from rest to mild exercise, no significant changes occurred. Muscle metaboreflex activation tended to increase both values. Muscle metaboreflex activation significantly increased the percentage of HR sequences that showed reciprocal changes in SV compared with the resting situation. In contrast, moderate exercise significantly increased the percentage of overlap (HR with reciprocal changes in SV) and the quantity that SV changed. Muscle metaboreflex activation at this workload had no further effect. In accordance with the companion article by Sala-Mercado et al. (33a), the percentage of the HR-LVSP sequences in which reciprocal changes in SV occurred was substantially increased at rest in HF. In addition, the changes in HR were accompanied by larger changes in SV, not only at rest but at each setting. Although, when in HF, neither mild nor moderate exercise before and after muscle metaboreflex activation altered the percentage of overlap, larger reciprocal changes in SV per beat occurred with each workload before and after muscle metaboreflex activation. BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS AJP-Heart Circ Physiol • VOL CO occur. These results suggest that the depressed dynamic baroreflex control of CO in HF is induced by both a decreased baroreflex chronotropic response (i.e., diminished HR baroreflex gain) and an impaired inotropic state of the heart (i.e., reduced SV). In addition, in HF, a higher percentage of CO responses were associated with spontaneous baroreflex-like changes in SV. The increased contribution of SV changes to CO responses seen in HF might reflect a higher afterload sensitivity of the left ventricle in HF subjects (32). Accordingly, baroreflex-mediated blood pressure regulation relies less on CO control and is more dependent on peripheral vascular regulation in HF (17, 24). Limitations of the study. Our approach employed to evaluate arterial baroreflex control of HR and CO (based on spontaneous fluctuations in blood pressure, HR and CO) has several advantages and disadvantages that we have previously described in detail (14, 16, 31). Briefly, the reduction in spontaneous baroreflex HR sensitivity seen with exercise and with muscle metaboreflex activation may be due to a shift of the operating point to a lower sensitivity portion of the entire stimulus response relationship (9, 27). In addition, the autonomic mechanisms mediating these rapid baroreflex changes in HR and CO are likely confined to the parasympathetic component of baroreflex (22, 23). The spontaneous baroreflex technique does, however, enable a qualitative and quantitative estimate of the integrated baroreceptor-cardiac response relationships during the spontaneous blood pressure fluctuations that characterize both the resting and exercise conditions, without the necessity of any pharmacological or mechanical interventions. This aspect is particularly relevant in HF conditions, in which, for example, sympathostimulatory reflexes by stretch of cardiac chambers after phenylephrine-induced increase of afterload or a direct -adrenergic stimulation at the sinus node level by high doses of the drug superimposed to the already heightened blood pressure of exercise may affect baroreflex responses. Conclusions. We found that dynamic exercise decreases both HR-LVSP and CO-LVSP and the translation of the HR responses into CO responses. Muscle metaboreflex activation further decreases HR-LVSP, whereas it has no significant effect on CO-LVSP and the translation of HR responses into CO responses in normal animals. After the induction of congestive HF, HR-LVSP, CO-LVSP, and the translation of HR responses into CO responses decreased significantly at rest, during dynamic exercise with and without muscle metaboreflex activation, further supporting the concept that in HF baroreflex-mediated blood pressure regulation relies less on CO control and is more dependent on peripheral vascular regulation. ACKNOWLEDGMENTS We thank Erin Krengel, Sue Harris, Jaime Rodriguez, and Dominic Fano for expert technical assistance and care of the animals and also Dr. Jong-Kyung Kim for assistance with the surgeries. GRANTS M. Ichinose and T. Ichinose are recipients of research fellowships of the Japan Society for the Promotion of Science for Young Scientists. This research was supported by a National Heart, Lung, and Blood Institute Grant HL-55473 and by a Agenzia Spaziale Italiana, Disturbi del Controllo Motorio e Cardiorespiratorio project, Grant ASI I/006/06/0 (to F. Iellamo). 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 Previous studies demonstrated that the muscle metaboreflex and the arterial baroreflex interact to regulate cardiovascular responses during exercise (13, 18 –20, 34, 36). A recent study from our laboratory showed that muscle metaboreflex activation in normal dogs during dynamic exercise resets the arterial baroreflex to higher blood pressure and HR and reduces HRLVSP (31), which we also observed in the present study. The mechanism(s) responsible for the decrease in HR-LVSP by muscle metaboreflex activation during dynamic exercise are surely complex, as discussed in our previous studies (16, 31). A likely cause of the decrease in HR-LVSP is the alteration in the balance of autonomic activity to the heart during muscle metaboreflex activation, mainly a further enhancement in sympathetic activity (11, 22). In contrast, to the decrease in HRLVSP, muscle metaboreflex activation had no obvious effect on CO-LVSP and on the translation of HR responses into CO responses. One likely explanation is that the muscle metaboreflex activation-induced increase in SV via augmented ventricular performance (33) coupled with central blood mobilization (35) would work to maintain CO-LVSP in the face of a decreased baroreflex HR response. Therefore, despite the decreased baroreflex chronotropic response, cardiac baroreflexmediated blood pressure regulation would be maintained via an inotropic response during metaboreflex activation. Cardiac baroreflex responses during dynamic exercise and metaboreflex activation in HF. HF is characterized by increased sympathetic activity, depressed vagal tone, and an attenuated baroreflex control of HR (8, 12). In addition, this increased sympathetic activity is further augmented during dynamic exercise (11). In this context, an enhanced muscle metaboreflex-induced sympathetic activation has been proposed as a key factor in the evolution and worsening of HF (4). In HF, the ability of the metaboreflex to improve ventricular function is virtually abolished (5, 32) and the pressor response occurs via peripheral vasoconstriction. Iellamo et al. (16) have recently reported that HR-LVSP is significantly depressed at rest and during dynamic exercise before and after muscle metaboreflex activation in subjects with HF. In addition, in the companion article, Sala-Mercado et al. (33a) showed that HF also decreased CO-LVSP and the ability of baroreflex changes in HR to cause changes in CO. In the present study we observed that HF significantly decreased CO-LVSP and HR-LVSP not only at rest but also during both mild and moderate exercise before and after muscle metaboreflex activation. Furthermore, in HF, significantly fewer HR responses caused CO responses in each setting. This markedly reduced ability of changes in HR to elicit effective changes in CO was due to the significantly larger reciprocal changes in SV that occurred during HR-LVSP sequences (Fig. 4). Indeed, at the highest workload with metaboreflex activation, over a twofold greater fall in SV occurred with increases in HR, thereby markedly limiting the ability of increases in HR to elicit increases in CO. Thus, whereas in normal subjects it is likely that the increased ventricular contractility induced by metaboreflex activation acts to sustain CO-LVSP, the impaired ability to improve ventricular function in HF likely contributed in an important manner to the further decrease in CO-LVSP in this setting. In addition, the marked decrease in the slope of the linear regression between HR-LVSP and CO-LVSP in HF indicates that even at the same baroreflex HR sensitivity, smaller changes in H1315 H1316 BAROREFLEX HR-CO OVERLAP: EXERCISE, N, AND HF CONDITIONS REFERENCES AJP-Heart Circ Physiol • VOL 294 • MARCH 2008 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.32.247 on June 17, 2017 1. Ansorge EJ, Augustyniak RA, Perinot RL, Hammond RL, Kim JK, Sala-Mercado JA, Rodriguez J, Rossi NF, O’Leary DS. Altered muscle metaboreflex control of coronary blood flow and ventricular function in heart failure. Am J Physiol Heart Circ Physiol 288: H1381–H1388, 2005. 2. Bertinieri G, Di Rienzo M, Cavallazzi A, Ferrari AU, Pedotti A, Mancia G. Evaluation of baroreceptor reflex by blood pressure monitoring in unanesthetized cats. Am J Physiol Heart Circ Physiol 254: H377– H383, 1988. 3. Burger HR, Chandler MP, Rodenbaugh DW, Dicarlo SE. Dynamic exercise shifts the operating point and reduces the gain of the arterial baroreflex in rats. Am J Physiol Regul Integr Comp Physiol 275: R2043– R2048, 1998. 4. Coats AJ, Clark AL, Piepoli M, Volterrani M, Poole-Wilson PA. Symptoms and quality of life in heart failure: the muscle hypothesis. Br Heart J 72: S36 –S39, 1994. 5. Crisafulli A, Salis E, Tocco F, Melis F, Milia R, Pittau G, Caria MA, Solinas R, Meloni L, Pagliaro P, Concu A. Impaired central hemodynamic response and exaggerated vasoconstriction during muscle metaboreflex activation in heart failure patients. Am J Physiol Heart Circ Physiol 292: H2988 –H2996, 2007. 6. Crisafulli A, Salis E, Pittau G, Lorrai L, Tocco F, Melis F, Pagliaro P, Concu A. Modulation of cardiac contractility by muscle metaboreflex following efforts of different intensities in humans. Am J Physiol Heart Circ Physiol 291: H3035–H3042, 2006. 7. Dicarlo SE, Bishop VS. Onset of exercise shifts operating point of arterial baroreflex to higher pressures. Am J Physiol Heart Circ Physiol 262: H303–H307, 1992. 8. Eckberg DL. Baroreflex inhibition of the human sinus node: importance of stimulus intensity, duration, and rate of pressure change. J Physiol 269: 561–577, 1977. 9. Eiken O, Convertino VA, Doerr DF, Dudley GA, Morariu G, Mekjavic IB. Characteristics of the carotid baroreflex in man during normal and flow-restricted exercise. Acta Physiol Scand 144: 325–331, 1992. 10. Hammond RL, Augustyniak RA, Rossi NF, Churchill PC, Lapanowski K, O’Leary DS. Heart failure alters the strength and mechanisms of the muscle metaboreflex. Am J Physiol Heart Circ Physiol 278: H818 –H828, 2000. 11. Hammond RL, Augustyniak RA, Rossi NF, Lapanowski K, Dunbar JC, O’Leary DS. Alteration of humoral and peripheral vascular responses during graded exercise in heart failure. J Appl Physiol 90: 55– 61, 2001. 12. Higgins CB, Vatner SF, Eckberg D, Braunwald E. Alterations in the baroreceptor reflex in conscious dogs with heart failure. J Clin Invest 51: 715–724, 1972. 13. Ichinose M, Saito M, Kondo N, Nishiyasu T. Time-dependent modulation of arterial baroreflex control of muscle sympathetic nerve activity during isometric exercise in humans. Am J Physiol Heart Circ Physiol 290: H1419 –H1426, 2006. 14. Iellamo F. Neural mechanisms of cardiovascular regulation during exercise. Auton Neurosci 90: 66 –75, 2001. 15. Iellamo F, Galante A, Legramante JM, Lippi ME, Condoluci C, Albertini G, Volterrani M. Altered autonomic cardiac regulation in individuals with Down syndrome. Am J Physiol Heart Circ Physiol 289: H2387–H2391, 2005. 16. Iellamo F, Sala-Mercado JA, Ichinose M, Hammond RL, Pallante M, Ichinose TK, Stephenson LW, O’Leary DS. Spontaneous baroreflex control of heart rate during exercise and muscle metaboreflex activation in heart failure. Am J Physiol Heart Circ Physiol 293: H1929 –H1936, 2007. 17. Kim JK, Augustyniak RA, Sala-Mercado JA, Hammond RL, Ansorge EJ, O’Leary DS. Heart failure alters the strength and mechanisms of arterial baroreflex pressor responses during dynamic exercise. Am J Physiol Heart Circ Physiol 287: H1682–H1688, 2004. 18. Kim JK, Sala-Mercado JA, Rodriguez J, Scislo TJ, O’Leary DS. The arterial baroreflex alters the strength and mechanisms of the muscle metaboreflex pressor response during dynamic exercise. Am J Physiol Heart Circ Physiol 288: H1374 –H1380, 2005. 19. McIlveen SA, Hayes SG, Kaufman MP. Both central command and exercise pressor reflex reset carotid sinus baroreflex. Am J Physiol Heart Circ Physiol 280: H1454 –H1463, 2001. 20. Nishiyasu T, Tan N, Morimoto K, Nishiyasu M, Yamaguchi Y, Murakami N. Enhancement of parasympathetic cardiac activity during activation of muscle metaboreflex in humans. J Appl Physiol 77: 2778 – 2783, 1994. 21. Nobrega ACL, Williamson JW, Garcia JA, Mitchell JH. Mechanisms for increasing stroke volume during static exercise with fixed heart rate in humans. J Appl Physiol 83: 712–717, 1997. 22. O’Leary DS. Autonomic mechanisms of muscle metaboreflex control of heart rate. J Appl Physiol 74: 1748 –1754, 1993. 23. Ogoh S, Fisher JP, Dawson EA, White MJ, Secher NH, Raven PB. Autonomic nervous system influence on arterial baroreflex control of heart rate during exercise in humans. J Physiol 566: 599 – 611, 2005. 24. Olivier NB, Stephenson RB. Characterization of baroreflex impairment in conscious dogs with pacing-induced heart failure. Am J Physiol Regul Integr Comp Physiol 265: R1132–R1140, 1993. 25. Patel HJ, Pilla JJ, Polidori DJ, Pusca SV, Plappert TA, Sutton MS, Lankford EB, Acker MA. Ten weeks of rapid ventricular pacing creates a long-term model of left ventricular dysfunction. J Thorac Cardiovasc Surg 119: 834 – 841, 2000. 26. Potts JT, Shi XR, Raven PB. Carotid baroreflex responsiveness during dynamic exercise in humans. Am J Physiol Heart Circ Physiol 265: H1928 –H1938, 1993. 27. Raven PB, Fadel PJ, Ogoh S. Arterial baroreflex resetting during exercise: a current perspective. Exp Physiol 91: 37– 49, 2006. 28. Rowell LB, O’Leary DS, Kellogg DL Jr. Integration of Cardiovascular Control Systems in Dynamic Exercise. New York: Oxford Press, 1996, p. 770 – 838. 29. Ryan S, Ward S, Heneghan C, McNicholas WT. Predictors of decreased spontaneous baroreflex sensitivity in obstructive sleep apnea syndrome. Chest 131: 1100 –1107, 2007. 30. Sagawa K. Baroreflex control of systemic arterial pressure and vascular bed. In: Handbook of Physiology. The Cardiovascular System. Peripheral Circulation and Organ Blood Flow. Bethesda, MD: Am. Physiol. Soc., 1983, sect. 2, vol. III, pt. 2, chapt. 14, p. 453– 496. 31. Sala-Mercado JA, Ichinose M, Hammond RL, Ichinose TK, Pallante M, Stephenson LW, O’Leary DS, Iellamo F. Muscle metaboreflex attenuates spontaneous heart rate baroreflex sensitivity during dynamic exercise. Am J Physiol Heart Circ Physiol 292: H2867–H2873, 2007. 32. Sala-Mercado JA, Hammond RL, Kim JK, McDonald PJ, Stephenson LW, O’Leary DS. Heart failure attenuates muscle metaboreflex control of ventricular contractility during dynamic exercise. Am J Physiol Heart Circ Physiol 292: H2159 –H2166, 2007. 33. Sala-Mercado JA, Hammond RL, Kim JK, Rossi NF, Stephenson LW, O’Leary DS. Muscle metaboreflex control of ventricular contractility during dynamic exercise. Am J Physiol Heart Circ Physiol 290: H751– H757, 2006. 33a.Sala-Mercado JA, Ichinose M, Hammond RL, Coustos M, Ichinose T, Pallante M, Iellamo F, O’Leary DS. Spontaneous baroreflex control of heart rate versus cardiac output: altered coupling in heart failure. Am J Physiol Heart Circ Physiol (January 11, 2008); doi:10.1152/ajpheart. 01186.2007. 34. Scherrer U, Pryor SL, Bertocci LA, Victor RG. Arterial baroreflex buffering of sympathetic activation during exercise-induced elevations in arterial pressure. J Clin Invest 86: 1855–1861, 1990. 35. Sheriff DD, Augustyniak RA, O’Leary DS. Muscle chemoreflex-induced increases in right atrial pressure. Am J Physiol Heart Circ Physiol 275: H767–H775, 1998. 36. Sheriff DD, O’Leary DS, Scher AM, Rowell LB. Baroreflex attenuates pressor response to graded muscle ischemia in exercising dogs. Am J Physiol Heart Circ Physiol 258: H305–H310, 1990. 37. Wyss CR, Ardell JL, Scher AM, Rowell LB. Cardiovascular responses to graded reductions in hindlimb perfusion in exercising dogs. Am J Physiol Heart Circ Physiol 245: H481–H486, 1983.