* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Definitions
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Electrocardiography wikipedia , lookup
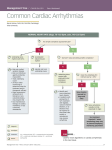
Pathway for Diagnosis / Referral of Adults with Palpitations presenting in Primary Care Symptoms Present at time of consultation NO YES History, Exam ECG, TFT, FBC Associated with Presyncope / Syncope, Chest Pain or SOB Delta wave on ECG (WPW) REFER CARDIOLOGY PAF See AF Management High Cardiac Risk Abnormal ECG Chest pain / SOB / Syncope YES NO Call 999 or Cardiac Arrest Protocol 12 lead ECG Sinus tachycardia (<120bpm) Investigate for underlying cause Not sinus rhythm or AF Atrial fibrillation Try vagal manoeuvres See AF Management YES REFER CARDIOLOGY NO Normal ECG etc Single Episode Reversion to sinus rhythm REFER CARDIOLOGY Consider medication if recurrent Recurrent Episodes Continuing Tachycardia NO FURTHER ACTION REQUIRED Symptoms < once a day Symptoms daily REQUEST OPEN ACCESS MEMO if available * OR REFER CARDIOLOGY REQUEST OPEN ACCESS 24-HOUR TAPE if available * OR REFER CARDIOLOGY Single Ectopics only with no other symptoms – REASSURE Couplets / Triplets / Salvos – REFER CARDIOLOGY URGENT MEDICAL ADMISSION Note: Recurrent worrying symptoms unexplained by this pathway: Cardiology advice can be sought PAF - See AF Management SVT REFER CARDIOLOGY Sinus Rhythm with no other symptoms - REASSURE ECN DS/SH FINAL 140907 8 pages * Open access memo or tape If available locally, an aid to the correct device is given in the accompanying guidelines Definitions Palpitation: is the uncomfortable awareness of the heart rhythm. Normal palpitations occur with exercise, emotion and stress or after taking substances that increase adrenergic activity or decrease vagal activity. Abnormal palpitations may occur for no reason and may be fast or strongand-slow. Palpitations may point to cardiac arrhythmia; however many with rhythm disturbances will not have palpitations, instead experiencing syncope, shock and chest pain. Syncope: is a sudden but brief loss of consciousness that is caused by inadequate blood supply to the brain. Recovery is spontaneous and rapidly complete. Syncope is common, disabling and possibly associated with sudden cardiac death. Vertigo: is a hallucination of movement of the environment about the patient, or of the patient with respect to the environment. It is not synonymous with dizziness. It may be central - due to a disorder of the brainstem or the cerebellum - or peripheral - due to a disorder in the inner ear or the Vlllth cranial nerve. Always would suggest ENT review prior to cardiac review unless associated with palpitations or chest pain High Risk Factors: Pre existing structural heart disease History of heart failure History of syncope or presyncope FH of Sudden Cardiac Death under the age of 40yrs Exertion cardiac symptoms (including exertional palpitations) Resting 12 lead ECG abnormality (pre excitation, old MI, LBBB) Vagal Manoeuvres: Valsalva Manoeuvre Carotid Sinus Massage (if practitioner feels competent and no bruits present) Face immersion in cold Water Common Situations: Palpitations as missed beats or non sustained runs occurring predominately at rest or at night are suggestive of PVE needing no intervention if there are no other risk factors of cardiac disease If the attacks are occurring less than once a week without associated 'High Risk Factors' ambulatory monitoring is unlikely to be of assistance. If High Risk Factors are present formal referral is suggested. • Asymptomatic bradycardia in the elderly (resting heart rate in mid 40s) do not need intervention Syncope without preceding palpitation, or occurring less then once a week, investigation with a 24hr ECG is rarely helpful Investigation of symptoms - Cardiomemo or 24 hour tape? A cardiomemo is a patient activated event recording device that is generally provided for 5 to 7 days. It is helpful for infrequent symptoms and is recommended for patients who have symptoms less than once a day but more frequent than once a fortnight A 24 hours tape allows continuous heart rhythm monitoring for 24 hours. It is indicated where there are symptoms on a daily, or near daily, basis ECN DS/SH FINAL 140907 8 pages Atrial Fibrillation accounts for approximately 70% of all Arrhythmia Presentation in Essex. Therefore it was felt essential to include all types of presentations of AF in the following pathways. The guidance includes advice on Risk stratification and Rate versus Rhythm Control. New Diagnosis Atrial Fibrillation Care Pathway Page 4 Treatment Strategy for Atrial Fibrillation Page 5 Rate versus Rhythm Control Page 6 Stroke Risk Stratification Page 6 Primary Care Management Guideline for Permanent Atrial Fibrillation with Known Aetiology Page 7 Haemodynamically Unstable & Acute Onset Atrial Fibrillation Page 8 3 ECN DS/SH FINAL 140907 8 pages New Diagnosis Atrial Fibrillation Care Pathway If Previous Diagnosis of AF – see Treatment Strategy No symptoms – opportunistic case-finding leads to clinical suspicion of new AF Symptomatic presentation and clinical suspicion of new AF Confirm Diagnosis History Examination Manual Pulse 12 lead ECG Emergency referral to A&E If patient is Haemodynamically unstable Start treatment if ventricular Rate > 90 bpm For Example Beta Blockers Rate Limiting Calcium Antagonist Digoxin Referral to Local Rapid Access Arrhythmia Clinic or Equivalent ECHO (if appropriate) FBC, UE, LFT & Thyroid function Stroke Risk Stratification Management Plan Follow Up Sinus Rhythm Assess need for further maintenance / monitoring Continued AF Continued FU / Monitoring Return of symptoms / AF Referral for further Electrophysiology Advice 4 ECN DS/SH FINAL 140907 8 pages Treatment Strategy for Atrial Fibrillation Confirmed Diagnosis of Atrial Fibrillation Further investigations and clinical assessment including Stroke Risk Stratification Paroxysmal AF Persistant AF Permanent AF OR Rate Control Refer to permanent AF with Known Aetiology Rhythm Control Continued Symptoms or Failure of Rate or Rhythm Control EP Consultant Referral Classifications: All AF lasting greater than 30 seconds should be described as: Paroxysmal – if self terminating within 7 days Persistent – if cardioverted to Sinus Rhythm by any means or lasts >7days regardless of how it terminates Permanent – if it does not terminate or relapses within 24 hrs of cardioversion 5 ECN DS/SH FINAL 140907 8 pages Rate versus Rhythm Control Rate Control Rhythm Control Contraindication to Cardioversion Patients over 65 Presenting for the first time with lone AF Contraindications to anticoagulation Patients with coronary heart disease Younger patients Structural heart disease that precludes long term maintenance of sinus rhythm Long duration of AF ( > 12 months ) Multiple failed attempts of cardioversion Ongoing but reversible cause Patients unsuitable for cardioversion Patients with Congestive heart failure Patients with contraindications to antiarrhythmic drugs On going symptomatic patients despite rate management Without congestive heart failure Patients with AF secondary to a treated/corrected precipitant Stroke Risk Stratification – there are two systems of risk evaluation The CHAD2 score-if the score is over 2 formal Anticoagulation suggested CHAD2 Item Congestive Heart Failure Hypertension Age over 75 Diabetes Prior cerebral ischaemia The NICE Guidance – 2006 6 ECN DS/SH FINAL 140907 8 pages Points 1 1 1 1 2 Primary Care Management Guideline for Permanent Atrial Fibrillation with Known Aetiology Annual Drug Review Warfarin Ensure NO side-effects and possible drug interactions eg. Non-steroidals, Aspirin and Clopidogrel * Medication for Rate Control Those on Long Term Amiodarone should have a recorded reason documented from a cardiologist or AF Clinic, as this drug is rarely given to patients with permanent AF. Amiodarone Those on Amiodarone long term require: 6 monthly TFT Annual opticians eye screen and refer if corneal microdeposits develop CXR if respiratory symptoms develop Associated hepatotoxicity - advise at least annual LFT. Stop amiodarone if develop signs of liver disease *Patient’s on Aspirin, Clopidogrel and Warfarin should be reviewed by a cardiologist to see if all three need to be continued Annual Rate & Rhythm Review Check Heart Rate & Rhythm with Annual ECG Atrial Fibrillation Sinus Rhythm Target Rate Control = 60-80 bpm at rest 1st Line: Beta-Blockers 2nd Line: Diltiazem / Verapamil Digoxin: First line for sedentary patients Exclude Paroxysmal AF with Cardiomemo. If results show Sinus Rhythm throughout consider stopping Warfarin. Check that Cardiologist or AF clinic hasn’t suggested Long Term Warfarin. 7 ECN DS/SH FINAL 140907 8 pages Haemodynamically Unstable & Acute Onset Atrial Fibrillation Patients with acute haemodynamic instability secondary to AF Is the situation life – threatening ? NO YES Is Duration of AF > 48 Hrs ? NO Emergency Electrical Cardioversion YES Consider Pharmacological or Electrical Cardioversion + Stroke Risk Stratification Pharmacological rate – control + Stroke Risk Stratification Refer to Local Rapid Access Arrhythmia Clinic or Equivalent 8 ECN DS/SH FINAL 140907 8 pages