* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Hypertrophic Cardiomyopathy - Carolinas HealthCare System
Survey
Document related concepts
Baker Heart and Diabetes Institute wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
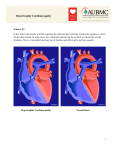
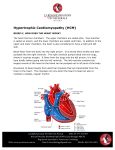
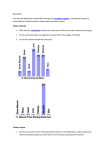
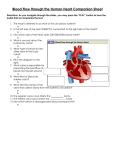
The www.sangerheart.org Hypertrophic Cardiomyopathy John D. Symanski, MD, FACC, FASE Adult Cardiologist Hypertrophic cardiomyopathy fibrosis [see Figure 2].6 The (HCM) is defined as excessive ven- characteristic symptoms of tricular hypertrophy with a nondilated HCM (shortness of breath, chest ventricle in the absence of the typical discomfort and syncope) are provocative factors [see Figure 1]. related to several pathophysiologic HCM is the most common genetic processes, including: 1) obstruction cause of heart disease, with an auto- of blood flow through the narrowed somal dominant mode of inheritance left ventricular outflow tract in most cases. This disorder affects (LVOTO), 2) disturbance of the approximately one out of 500 individ- mitral valve apparatus with uals in the general population. HCM resultant mitral regurgitation, is highly variable in terms of disease 3) subendocardial ischemia and penetrance and clinical expression. 4) abnormal LV relaxation (diastolic Age at onset, distribution of ventricu- dysfunction) [see Figure 3].7 lar hypertrophy, symptom status and Larry T. Watts, MD, FACS Cardiothoracic Surgeon Cardiac rhythm disturbances sudden death risk are unique to each including atrial fibrillation and patient and may be related to an ventricular tachyarrhythmias may also individual’s specific gene mutation as contribute to symptom production, well as modifying factors.1-5 cardiac morbidity and mortality. It is important to understand that the Disease characteristics source of symptoms in any given Histopathologically, HCM is patient may result from any one of characterized by malalignment of these factors or the combination of cardiac muscle fibers (myocyte several pathophysiologic processes. disarray), dysplastic intramyocardial arterioles and excessive myocardial Continued on page 3 SPRING 2011 | Vol. 2 | issue 1 NEW! FREE ONLINE CME Free CME credit is now available for noted presentations. Visit www.sangerheart.org and click on the “Charlotte AHEC Connect” logo to find archived and live CME presentations. sign up to Receive The Sanger Report via e-mail If you’re interested in receiving a copy of The Sanger Report via e-mail, visit www.sangerheart.org and fill out the short sign-up form located on our home page. Privacy policy: Your information will not be used for third-party distribution. Inside ... Hypertrophic Cardiomyopathy continued PAGE 3 Cardiovascular Disease: Women’s Initiative PAGE 5 How Common is Venous Disease? PAGE 6 The latest news and best practices from Sanger Heart & Vascular Institute Fighting Cardiovascular Disease Sanger Heart & Vascular Institute Awards Jan. 6, 2011 marked the 25th anni- featured in the ACC’s magazine versary of the first heart transplant and on its website for his leader- performed in Charlotte, NC, by ship role. Francis Robicsek, MD. Since then, Welcome to the second volume of Sanger Heart & Vascular Institute Samuel H. Zimmern, MD, was The Sanger Report. This is our first issue for 2011, (SHVI) physicians have performed published in the HeartRhythm featuring three clinical articles from our adult cardiology more than 470 heart transplants, Society Journal in December 2010, and cardiothoracic surgery teams. with our most recent mortality for his article titled “Mutations statistics second to none. “We in the Cardiac L-Type Calcium Adult Cardiology, and Larry T. Watts, MD, from the John D. Symanski, MD, from the Department of couldn’t have made it this far Channel Associated with Inherited Department of Cardiothoracic Surgery, explain hypertro- without the dedication and sup- J-Wave Syndromes and Sudden phic cardiomyopathy (HCM), the most common genetic port of both Carolinas HealthCare Cardiac Death.” Dr. Zimmern cause of heart disease and sudden cardiac death in System and Sanger Heart & Vascular recently chaired the 8th annual children and athletes. They review the pathophysiology, Institute,” says SHVI President Cardiology Update for Primary Care diagnosis and management of patients with HCM. Paul G. Colavita, MD. “Since the Physicians, held in Charlotte, NC. Cheryl A. Russo, MD, from the Department of Adult first transplant, we have developed a Cardiology, outlines our current women’s initiative. dedicated Heart Failure/Transplant Sherry J. Saxonhouse, MD, from Dr. Russo brings new perspective to the topic of heart Clinic, a Pediatric Cardiac the Division of Electrophysiology, disease as the leading cause of death among American Transplant Program and expanded was selected to serve on the ACC’s women. She highlights the evidence-based guidelines our LVAD Program to include Accreditation Council for Continuing for cardiovascular disease prevention and the expanding destination therapy.” Medical Education and as associ- literature in the area of cardiovascular disease diagnosis ate editor of Cardiac Arrhythmia Thomas V. Johnson, MD, is for CardioSource. Dr. Saxonhouse leading the effort with SHVI to also has been selected to serve on Division of Vascular Medicine and Surgery, discusses participate in the American College the ACC’s ABIM Board Question venous disease, specifically varicose veins. The causes of Cardiology’s (ACC’s) FOCUS Writing Committee. of varicose veins and the treatment options available for Program. FOCUS is a national this very common disease are also detailed. in women. In our closing article, Felipe Navarro, MD, from the quality improvement initiative that Kevin W. Lobdell, MD, from As you can see from this issue and those before helps cardiovascular professionals the Department of Cardiothoracic it, Sanger Heart & Vascular Institute is committed to best use Appropriate Use Criteria Surgery, was published in The providing high quality, evidence-based care for a broad and ultimately reduce inappropriate Annals of Thoracic Surgery in spectrum of cardiovascular concerns—from congenital imaging. Dr. Johnson was recently January 2011, for his article titled, heart disease to transplants. We will continue to be on “Effect of Body Mass Index on the forefront in the fight against cardiovascular disease, Outcomes after Cardiac Surgery: and will continue to highlight our progress in the coming Is There an Obesity Paradox?” issues of The Sanger Report. Francis Robicsek, MD, and Sincerely, the International Medical Outreach Program recently received the highest recognition for humanitarian Paul G. Colavita, MD, FACC and medical achievements in Central President America. Sanger Heart & Vascular Institute 2 The Sanger Report | www.sangerheart.org Trophy image © 2011 Thinkstock Rodolfo Robles Award, the Hypertrophic Cardiomyopathy Continued from page 1 Disease diagnosis The diagnosis of HCM may initially be suspected based on characteristic symptoms such as: an abnormal ECG a systolic murmur on cardiac auscultation a history of a family member with premature sudden death Confirmation of the diagnosis usually involves cardiac imaging with either ultrasound (echocardiography) or MRI. Genetic testing is now commercially available and assuming an increasingly important role in diagnosis confirmation and family screening.8,9 HCM remains the most common cause of sudden death in young athletes. Although the frequency of this dreaded complication is low, F igure 1 Normal heart (left) and heart in HCM (right). HCM is characterized by a nondilated ventricular cavity with excessive ventricular wall thickening. LVH may be diffuse (concentric) or preferentially involve the ventricular septum, LV free wall, or apex.3 identification and management of high-risk patients remains an important clinical challenge.6,10 Preventing sudden cardiac death in high-risk HCM patients associated with an increased sudden on Holter monitoring or exercise stress death risk include: testing a family history of HCM-related an abnormal or attenuated BP sudden cardiac death response a history of recent syncope or Specific HCM gene mutations sudden death and presence of myocardial fibrosis feared complication of the disease and extreme hypertrophy (greater than (as identified by delayed gadolinium may strike at any time in previously 3-cm wall thickness on echo or MRI) enhancement on cardiac MRI) are asymptomatic patients. Factors nonsustained ventricular tachycardia gaining broader recognition in Sudden death in HCM is the most Continued on page 4 F igure 2 Microscopic and histologic features of HCM include myocyte disarray (left), abnormally thickened walls of intramyocardial arterioles with narrowed vessel lumen (center) and patchy replacement of myocardial fibers with fibrosis (right).7 www.sangerheart.org | The Sanger Report 3 Hypertrophic Cardiomyopathy Continued from page 3 F igure 3 In approximately two-thirds of patients with HCM, prominent septal hypertrophy results in systolic left ventricular outflow tract obstruction (LVOTO; white arrow) and distortion of the mitral valve apparatus with resultant regurgitation (yellow arrow).3 has become less popular due to the with severe LVOTO since the 1960s. existence of more effective treatment [See Figure 5.] Surgical decision-making options. Alcohol septal ablation is is tailored by thorough preoperative favored at some institutions due to echocardiographic analysis including 3D its less invasive nature. Complete reconstruction where specific attention heart block necessitating pacemaker is paid to the septal thickness/extent, implantation, ventricular septal defects aortic valvular abnormalities and other and intractable ventricular arrhythmias associated defects. Careful analysis may complicate this procedure. The must be made of the mitral valve and time-honored surgical treatment option its subvalvular apparatus looking for for patients who have obstructive HCM fusion or thickening of the papillary is septal myectomy. muscles with potential attachments to the free wall, excessive papillary muscle determination of high-risk individuals [see Figure 4].6 Automatic implantable cardioverter-defibrillator (AICD) therapy Surgical therapy of HCM Transaortic septal myectomy has clearly been demonstrated to save has been the standard surgical lives in high-risk HCM patients.4-6,10 procedure for symptomatic patients hypertrophy with anterior displacement, abnormal chordae tendinae or accessory Continued on page 8 Managing HCM Traditionally, medical therapies including beta-blockers, calcium channel blockers, disopyramide and amiodarone have been used alone or in combination in HCM patients to ameliorate symptoms and lessen the frequency of ventricular and supraventricular arrhythmias.2-5 For those in whom symptoms are due principally to LVOTO and who don’t respond or are intolerant to conventional medical therapies, mechanical interventions to expand the LV outflow tract may be pursued. Dual-chamber pacing he time-honored surgical “ Ttreatment option for patients who have obstructive HCM is septal myectomy. ” 4 The Sanger Report | www.sangerheart.org F igure 4 Gadolinium-enhanced MRI indicates regions of myocardial fibrosis (arrows) involving the midventricular septum.11 Cardiovascular Disease: Women’s Initiative Images on pages 1 & 6 © iStockphoto/DSGpro • Image on page 5 © iStockphoto/ranplett • Image on page 6 © iStockphoto/Dorling_Kindersley Cheryl A. Russo, MD, FACC Adult Cardiologist Heart disease is the leading during pregnancy, increasing cause of death among American a patient’s risk of CVD in the women, accounting for greater than future. Finally, a woman’s one in four deaths in this population. childbearing status must In the United States, more women be considered not only in die of cardiovascular disease (CVD) prevention, but also in than do their male counterparts diagnosis and treatment. each year. Among minority popula- In addition to preven- tions, disease disparities are even tion, the expanded literature greater. These facts don’t represent has increased our knowledge in a recent trend, rather one that has diagnosing CVD. We’ve learned been apparent for decades. Only in that a woman’s presentation with the last 10 to 15 years has significant CVD often differs significantly from to taking the lead in understanding awareness been brought to the sub- that of a man. Women more often CVD in women. We’re striving to pro- ject of CVD in women. As recently as present with chest pain, as compared vide the women of our community 1997, a mere 30 percent of women to a specific acute coronary event. and beyond with the highest level of polled were aware that heart disease There may be a variance in the cardiovascular care. Recognizing that was the No. 1 threat to their lives. quality of pain as well as atypical the risk of CVD is a spectrum along Over the next decade, awareness symptoms such as fatigue or dysp which all women have a place, we‘re nearly doubled. During this period, nea. There’s an awareness that prepared to guide women at all stages the scientific literature grew exponen- the sensitivity and specificity of of their lives and personalize their tially and confirmed the differences diagnostic and prognostic studies care. We have assembled a team of between genders in all aspects of are not equal between the genders. specialists who focus on the cardio- Finally, much data has been vascular needs of women, including gathered regarding the treatment primary and secondary prevention, of CVD in women. Studies reveal disease diagnosis and delivery of evidence-based guidelines for CVD that women are less likely than men care to assure optimal outcomes. prevention in women were updated to be referred for appropriate We also offer Heart of a Woman in 2007 to incorporate this new data. therapeutic procedures. We’ve Support Group, a joint effort between Some noteworthy advancements learned that as compared to men, SHVI and Carolinas HealthCare within these guidelines include: women’s in-hospital mortality after System. Our goal is to unite women generalizing the approach to risk myocardial infarction is higher and who have survived a cardiac event assessment, which now reflects a overall survival is lower. Some of with women who are striving to woman’s high lifetime risk of CVD these differences in outcomes may prevent similar experiences. Through augmenting risk assessment with be explained by confounding education, sharing of information nontraditional risk factors factors, such as older age at and encouragement, participants updating recommendations for presentation and higher number are empowered with the knowledge hormonal and aspirin therapy of comorbidities in women. required to begin or maintain a However, the difference is clear. heart-healthy lifestyle. For more infor- CVD, including prevention, diagnosis, treatment and outcomes. The American Heart Association’s Also unique to preventing CVD in the female patient is consideration of comorbidities that may occur At Sanger Heart & Vascular Institute (SHVI), we’re committed mation, visit www.sangerheart.org or call 704-373-0212. www.sangerheart.org | The Sanger Report 5 How Common is Venous Disease? Experts estimate that between 5 and 30 percent of the American population suffers Felipe Navarro, MD, FACC, FSVM Vascular Interventionalist What causes varicose veins? Contracting calf muscles propel are usually aggravated by prolonged standing or sitting (due to the immobility of muscle pump in the calves). from chronic varicose veins. blood against gravity. The venous Female patients may experience more Venous disease often results valves are one-way valves that pro- pronounced symptoms during their in symptoms such as achiness, mote blood flow toward the heart. menses. fatigue, swelling and pain in As the weakened venous walls cause the legs. These symptoms can venous dilatation (most commonly However, left untreated, varicose interfere with a patient’s activities in the greater saphenous vein), the veins can lead to complications of daily life. At least 20 percent of valvular leaflets no longer meet such as: patients with venous disease will properly, thereby becoming incom- Stasis pigmentation. This condi- develop leg ulcers due to greater petent. This allows reflux in the tion presents as a discoloration of saphenous vein reflux disease. venous segment, which subsequently the skin, often with swelling. most common “ Triskhe factor for developing varicose veins in females is the presence of progesterone, which is thought to weaken the venous walls. ” Most varicose veins are benign. further dilates the vein. Reflux is Stasis dermatitis. Commonly then further propagated distally mistaken for infectious cellulitis and along the vein and its tributaries, treated unsuccessfully with antibiotics, becoming visible varicose veins. stasis dermatitis often presents as an erythematous patch of skin that’s What are the risk factors? intensely pruritic. The most common risk factor Stasis ulcerations. These are for developing varicose veins in extremely painful and difficult to females is the presence of proges- treat. Successful treatment includes terone, which is thought to weaken compressive therapy coupled with the venous walls. Pregnancy intensi- elimination of refluxing superficial fies the progesterone surge, causes veins, if present. About 0.4 percent venous hypertension and increases of venous ulcers transform into venous capacity. Other risk factors malignant lesions. include prolonged standing, hered- Varicose veins can also bleed, ity, obesity and aging. In some either spontaneously or as a result patients, several risk factors are of direct trauma. present; the female hairdresser, for example (gender and prolonged standing), with a family history of varicose veins. What are the treatment options? Medical management reduces symptoms and prevents the develop- What are the symptoms? Patients most often complain of 6 The Sanger Report | www.sangerheart.org ment of secondary complications. Initial treatment options usually achiness and a feeling of heaviness in include compression therapy with their legs. Other symptoms include graded elastic compression stock- restless legs, focal burning or pruritis ings. Leg elevation can help alleviate and leg swelling. A patient’s symptoms edema and lower hydrostatic surgical ligation and stripping, B EFORE both treatments are equally efficient in eliminating greater saphenous reflux, alleviating symptoms and signs of saphenous varicosities and improving quality of life. Other studies suggest that ablation results in an earlier return to normal activity. References 1. Beebe-Dimmer JL, Pfeifer JR, Engle JS, et al. The epidemiology of chronic venous insufficiency and varicose veins. Ann Epidemiol. 2005;15(3):175–184. a fter 2. Min RJ, Khillnani N, Zimmet SE. Endovenous laser treatment of saphenous vein reflux: Long-term results. J Vasc Intervent Radiol. 2003;14(8):991–996. pressure. A graded exercise program introduced into the distal aspect of 3. Kabnick LS. Outcome of different endovenous helps rehabilitate muscle pump and the refluxing vein and fed proximally laser wavelengths for great saphenous vein improves symptoms of venous insuf- to within 2 cm of the saphenofemoral ficiency in varicose veins. ablation. J Vasc Surg. 2006;43(1):88–88.e7. or saphenopopliteal junction. The 4. Merchant RF, Pichot O. Closure Study Group. Many interventional treat- procedure is performed with tumes- Long-term outcomes of endovenous radiofrequency ment options are also available. cent anesthesia, which is a mixture obliteration of saphenous reflux as a treatment of Sclerotherapy is one option that of 0.1 percent lidocaine in saline. helps obliterate telangiectases, This provides a heat sink to reduce reticular veins and varicose veins. skin burns, helps to collapse the vein 5. Rasmussen LH, Bjoern L, Lawaetz M, et al. In the United States, sodium around the catheter and eliminates Randomized trial comparing endovenous laser tetradecyl sulfate and sodium procedural pain. morrhuate are approved for treat- superficial venous insufficiency. J Vasc Surg. 2005;42:502–509. ablation of the great saphenous vein with high Laser treatment with an 810-nm, ligation and stripping in patients with varicose veins. J Vasc Surg. 2007;46(2):308–315. ment of varicose veins. The use of a 940-nm or a 980-nm diode has these agents in a foam preparation shown excellent results with saphe- 6. Lurie F, Creton D, Eklof B, et al. Prospective has not been approved by the FDA. nous vein obliteration in 93 percent randomized study of endovenous radiofrequency Endovenous radiofrequency and laser ablation therapies are of cases at one and two years. Radiofrequency treatment yields recent advances in the treatment complete occlusion in 87.2 percent of varicose veins. They’re useful in of cases and a reflux-free rate of treating varicose veins that arise 83.8 percent of cases after a five- from refluxing greater or lesser year follow-up period. When com- saphenous veins. Catheters are paring endovenous ablation with obliteration (closure) versus ligation and vein stripping (EVOLVeS): Two-year follow-up. Eur J Vasc Endovasc Surg. 2005;29(1):67–73. 7. Darwood RJ, Theivacumar N, Dellagrammaticas D, et al. Randomized clinical trial comparing endovenous laser ablation with surgery for the treatment of primary great saphenous varicose veins. Br J Surg. 2008;95(3):294–301. www.sangerheart.org | The Sanger Report 7 e-logo_2options_v2.ai The The Sanger Report 1001 Blythe Blvd. Suite 300 Charlotte, NC 28203 Printed With Soy Ink PRSRT STD U.S. POSTAGE PAID Sanger Heart & Vascular Institute Printed With Soy Ink Please Recycle This Publication Please Recycle This Publication Printed With Soy Ink Please Recycle This Publication Copyright © 2011 Sanger Heart & Vascular Institute Printed With Soy Ink Please Recycle This Publication www.sangerheart.org Hypertrophic Cardiomyopathy 3. Nishimura RA, Ommen SR, Tajik AJ. Continued from page 4 Hypertrophic cardiomyopathy: A patient perspective. Circulation. 2003;108:e133–e135. papillary muscles. These anomalies contribute to LVOTO and residual Reduced outflow Mitral regurgitation Septal myectomy obstruction, if not addressed. 4. Spirito P, Seidman CE, McKenna WJ, et al. The management of hypertrophic cardiomyopathy. N Eng J Med. Increased outflow Surgical techniques include 1997;336(11):775–785. extensive resection from trigone 5. Nishimura RA, Holmes DR. [Clinical Practice] to trigone, extending deep in the Hypertrophic obstructive cardiomyopathy. ventricular cavity to the base of both papillary muscles. Care is taken to avoid injury to the aortic valve or N Eng J Med. 2004;350(13):1320–1327. Incision line through hypertrophied basal septum 6. Maron BJ. Contemporary insights conduction tissue or creation of a F igure 5 ventricular septal communication. Surgical septal and prevention of sudden death Residual systolic anterior motion over reoperation for residual myectomy in hypertrophic cardiomyopathy. the medial papillary muscle of the or recurrent obstruction mitral valve and midcavitary residual is less than 10 percent at eight to 10 7. Fifer MA, Vlahakes GJ. Management of symp- obstruction can be avoided by years. Importantly, symptomatic status toms in hypertrophic cardiomyopathy. Circulation. adequate resection. Barring intrinsic is dramatically improved, with more 2008;117(3):429–439. pathology, mitral valve intervention than 50 percent of patients reporting can be avoided with the expectation functional Class I status after surgery of improvement of mitral insufficiency and the remainder improving one to on postoperative studies. two functional classes.2,3,5 In experienced hands, with proper and strategies for risk stratification 5 Circulation. 2010;121(3):445–456. 8. Force T, Bonow RO, Houser SR, et al. Research priorities in hypertrophic cardiomyopathy. Report of a working group of the National Heart, Lung, and Blood Institute. Circulation. 2010;122:1130-1133. For more information about the myocardial protection, surgical risks services available at Sanger Heart & 9. Bos JM, Towbin JA, Ackerman MJ. Diagnostic, are minimal with an initial mortality Vascular Institute or to schedule an prognostic and therapeutic implications of genetic of less than 1 percent and successful appointment, call 877-999-SHVI (7484) testing for hypertrophic cardiomyopathy. J Am Coll relief of LVOTO with absent gradients. or visit www.sangerheart.org. Surgical pacemaker placement is necessary in only about 3 percent of patients with normal conduction References 1. Maron BJ. Hypertrophic cardiomyopathy: A systematic review. JAMA. 2002;287(10):1308–1320. preoperatively but increases to 30 percent if there is intraventricular conduction delay or 70 percent if right bundle branch block is present prior to myectomy. Risk of Cardiol. 2009;54(3):201–211. 10. Maron BJ, Estes NAM III, Maron MS, et al. Primary prevention of sudden death as a novel treatment strategy in hypertrophic cardiomyopathy. Circulation. 2003;107(23):2872–2875. 2. Maron BJ, McKenna WJ, Danielson GK, et al. American College of Cardiology/European Society 11. Maron MS, Maron BJ, Harrigan C, et al. of Cardiology, Clinical expert consensus document Hypertrophic cardiomyopathy phenotype revisited on hypertrophic cardiomyopathy. J Am Coll Cardiol. after 50 years with cardiovascular magnetic 2003;42(9):1687–1713. resonance. J Am Coll Cardiol. 2009;54(3):220–228.