* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download ECG Basics
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Atrial fibrillation wikipedia , lookup
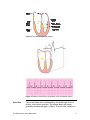
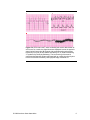
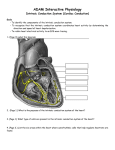
ECG Basics © 2006 American Heart Association Introduction Review ECG Basics to increase your knowledge of the electrocardiogram (ECG). In the PALS Provider Course you must be able to identify core rhythms during the case simulations and core case tests. Electrocardiogram Normal Cardiac Cycle The surface ECG is a graphic representation of the sequence of myocardial depolarization and repolarization. Each normal cardiac cycle (Figure 1) consists of a • P wave • QRS complex • T wave Electrical depolarization begins in the sinoatrial node at the junction of the superior vena cava and right atrium and advances through atrial tissue to the atrioventricular (AV) node, where conduction velocity slows temporarily. It then progresses via the bundle of His and the Purkinje system to depolarize the ventricular myocardium (Figure 2). The first deflection on the surface ECG (P wave) represents depolarization of both atria. The time required for depolarization to pass through the atria, the AV node, and the His-Purkinje system is represented by the PR interval. The QRS complex represents depolarization of the ventricular myocardium. Ventricular repolarization is characterized on the surface ECG as the ST segment and T wave (Figure 3). Figure 1. The electrocardiogram © 2006 American Heart Association 2 Figure 2. The cardiac conduction system. Figure 3. Relation of the ECG to the anatomy of the conduction system. Heart Rate The normal heart rate is influenced by the child's age, level of activity, and clinical condition. The normal heart rate range gradually declines with age1-5 (Table). There is wide variation in © 2006 American Heart Association 3 the normal heart rate within every age group. The child's temperature, emotional state, and sleep-awake state also influence heart rate. Table 1. Normal Heart Rates by Age Cardiac Monitoring Children with evidence of respiratory or cardiovascular instability should have continuous ECG monitoring. When arrhythmias are present, a 12-lead ECG is often necessary to supplement continuous bedside (3-lead) monitoring. Monitoring heart rate and rhythm can be helpful in both selection and modification of therapy: • Appropriate changes in heart rate or rhythm following interventions may indicate that the patient is responding to therapy. • Lack of change or worsening of heart rate or arrhythmia can indicate deterioration in the patient's condition and the need to modify therapy. Good Quality ECGs The ECG impulse is conducted from the patient to the cardiac monitor through cables attached to the patient with disposable adhesive monitoring pads or metal electrodes and straps. On a normal ECG of good quality, • the P waves, QRS complexes, and T waves are visible • the tachometer is triggered by the R wave but not the T wave • artifact is absent Placement of Electrodes Place conventional electrodes at the periphery of the anterior chest to avoid interference with cardiopulmonary examination and chest compressions should these become necessary. Typically you should place electrodes on the shoulders or the © 2006 American Heart Association 4 lateral chest surfaces and on the abdomen or thigh (Figure 4). ECG tracings also can be obtained through transcutaneous monitor/defibrillation/pacing adhesive electrodes on most monitor/defibrillators and some AEDs. Figure 4. Placement of electrodes for ECG monitoring. ECG Artifact Common Artifacts The ECG provides information about the electrical activity of the heart but not the effectiveness of myocardial contractility or quality of tissue perfusion. Therapy must always be guided by clinical assessment (eg, evaluation of responsiveness, capillary refill, end-organ perfusion, blood pressure) correlated with information derived from the ECG. Artifacts and electrode misplacement or displacement may account for discrepancies between the clinical examination and ECG data. Five of the most common ECG artifacts are the following: • A straight line (resembling asystole) or a wavy line (resembling coarse fibrillation) may be caused by a loose wire or monitoring electrode. • A tall T wave may be mistaken by the heart rate monitor for an R wave, causing the heart rate to be “double counted” so that the digital heart rate displayed on the monitor will be twice the intrinsic heart (and pulse) rate (Figure 5A). • Incorrect lead placement may obscure the P waves (may resemble heart block). • Muscle or 60-cycle electrical interference artifact (resembling VF (Figure 5B). • Motion artifact (chest percussion/physiotherapy or patting the infant can mimic ventricular arrhythmia [Figure 5C]). © 2006 American Heart Association 5 Figure 5. A, ECG with a tall T wave counted by the monitor tachometer as an R wave. As a result, the digital heart rate displayed is twice the patient’s actual intrinsic heart rate. B, Asystole with superimposed muscle artifact followed by 60-cycle (60 Hz) artifact resembling VF. C, Artifact resembling VT produced by chest physiotherapy. The lower tracing of the arterial waveform demonstrates pulses associated with an underlying sinus rhythm but the ECG artifact caused by chest physiotherapy resembles VT. © 2006 American Heart Association 6 References 1. 2. 3. 4. 5. Alimurung MM, Joseph LG, Nadas AS, et al. Unipolar precodial and extremity electrocardiogram in normal infants and children. Circulation. 1951;4:420-429. Ziegler RF. Electrocardiographic Studies in Normal Infants and Children. Springfield, IL: Charles C. Thomas Publishing; 1951. Furman RA, Halloran WR. Electrocardiogram in the first two months of life. J Pediatr. 1951;39:307-319. Tudbury PB, Atkinson DW. Electrocardiograms of 100 normal infants and young children. J Pediatr. 1950;34:466-481. Gillette PC, Garson A Jr, Porter CJ, et al. Dysrhythmias. In: Adams FH, Emmanouildies GC, Riemenschneider TA, eds. Moss' Heart Disease in Infants, Children and Adolescents. 4th ed. Baltimore, MD: Williams & Wilkins; 1989:725-741. © 2006 American Heart Association 7