* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Presentation Slides - AAFP Learning Link
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Jatene procedure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Discovery and development of direct thrombin inhibitors wikipedia , lookup
Antihypertensive drug wikipedia , lookup
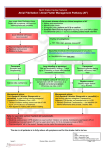
Evidence-based Recommendations The practice recommendations in this presentation are from: European Society of Cardiology Source: Guidelines for the Management of Atrial Fibrillation. European Heart Journal 2010;31:2369-429. Website: http://www.escardio.org/guidelines-surveys/escguidelines/GuidelinesDocuments/guidelines-afib-FT.pdf Strength of Evidence: The strength of evidence is indicated following each recommendation. Evidence-based Recommendations American College of Cardiology, American Heart Association Task Force on Practice Guidelines and European Society of Cardiology Committee for Practice Guidelines Source: ACC/AHA/ESC 2006 Guidelines for the Management of Patients with Atrial Fibrillation. Circulation 2006;114:e257-e354. Website: http://circ.ahajournals.org/cgi/content/full/114/7/e257 Strength of Evidence: The strength of evidence is indicated following each recommendation. Evidence-based Recommendations American College of Cardiology Foundation, American Heart Association Task Force on Practice Guidelines Source: 2011 ACCF/AHA/HRS Focused Update on the Management of Patients with Atrial Fibrillation (Updating the 2006 Guideline). Circulation 2011;123:104-23. Website: http://circ.ahajournals.org/cgi/content/short/123/1/104 Strength of Evidence: The strength of evidence is indicated following each recommendation. Evidence-based Recommendations American College of Cardiology Foundation, American Heart Association Task Force on Practice Guidelines Source: 2011 ACCF/AHA/HRS Focused Update on the Management of Patients with Atrial Fibrillation (Update on Dabigatran). J Am Coll Cardiol 2011;57:1330-7. Website: http://content.onlinejacc.org/cgi/content/full/j.jacc.2011.01.010 Strength of Evidence: The strength of evidence is indicated following each recommendation. Evidence-based Recommendations American College of Chest Physicians Source: Antithrombotic Therapy in Atrial Fibrillation. Chest 2008;133(Suppl 6):546S-92S. Website: http://chestjournal.chestpubs.org/content/133/6_suppl/546S.full Strength of Evidence: The strength of evidence is indicated following each recommendation. To Anticoagulate or Not to Anticoagulate? Module 1 Case 1 55-year-old male with lone atrial fibrillation Case 1 • 55-year-old male comes to the office stating that he has had two days of palpitations. He denies chest pain or shortness of breath. • Past medical history: negative • Medications: none • Family history: father died of an MI at 80 years of age; mother is alive and well Case 1 (continued) • Social history: works as a financial advisor, no tobacco use, social drinker (few drinks a week) • Physical exam: – – – – – Pulse: 105 irregular BP: 130/74 mm Hg Respiratory rate: 14 CV: irregularly irregular without murmurs Lungs: clear • Electrocardiogram: atrial fibrillation at rate of 104 Case 1: ECG CHADS2 Scoring Points C CHF 1 H Hypertension 1 A Age ≥75 1 D Diabetes 1 S Stroke or TIA 2 CHF = congestive heart failure; TIA = transient ischemic attack. Information from Gage BF, et al. JAMA 2001;285:2864-70. CHADS2 Application CHADS2 Score Adjusted Stroke Rate (per 100 patient years) 95% Confidence Interval 0 1.9 1.2-3.0 1 2.8 2.0-3.8 2 4.0 3.1-5.1 3 5.9 4.6-7.3 4 8.5 6.3-11.1 5 12.5 8.2-17.5 6 18.2 10.5-27.4 Information from Gage BF, et al. JAMA 2001;285:2864-70. CHADS2 and Recommended Therapy CHADS2 Score 0 1 ≥2 Recommended Therapy Aspirin (75 mg-325 mg daily) Aspirin (75 mg-325 mg daily) or Warfarin (INR 2.0-3.0) Warfarin (INR 2.0-3.0) Aspirin or no therapy is acceptable for patients less than 60 years of age with no heart disease (lone AF). Singer DE, et al. Chest 2008;133(suppl 6):546S-92S. Aspirin • Stroke reduction compared with placebo – Aspirin: 14% to 22% – Warfarin: 62% • Bleeding risk – Aspirin: 1.3 per 100 patient years (lethal bleeding = 0.2) – Warfarin: 2.2 per 100 patient years (lethal bleeding = 0.4) Hart RG, et al. Ann Intern Med 1999;131:492-501. EAFT Study Group. Lancet 1993;342:1255-62. Petersen P, et al. Lancet 1989;333:175-9. Van Walraven C, et al. JAMA 2002;288:2441-8. Gulløv AL, et al. Arch Intern Med 1999;159:1322-8. Evidence-based Recommendations Recommendation #1: The CHADS2 score is recommended as a simple initial means of assessing stroke risk in nonvalvular atrial fibrillation (AF). (I A) Recommendation #2: Patients with no risk factors (essentially patients aged <65 years with lone AF, with none of the risk factors) are at low risk of stroke. In these patients, the use of aspirin, 75 mg–325 mg daily, or no antithrombotic therapy, is recommended. (I B) ESC. European Heart Journal 2010;31:2369-429. Evidence-based Recommendation Recommendation #3: Antithrombotic therapy to prevent thromboembolism is recommended for all patients with AF, except those with lone AF or contraindications. (I A) ACC/AHA/ESC. Circulation 2006;114:e257-354. Choice of Anticoagulant Module 2 Case 2 65-year-old male with hypertension Case 2 • 65-year-old male with a history of hypertension presents for routine follow-up and is noted to have an irregular pulse. He denies chest pain or shortness of breath. • Past medical history – Hypertension – Peptic ulcer disease treated approximately 5 years ago – Intermittent GERD • Medications – Hydrochlorothiazide, 12.5 mg daily – Lisinopril, 5 mg daily – Omeprazole OTC, 10 mg as needed Case 2 (continued) • Social history: retired schoolteacher, denies tobacco use, rare alcohol use • Physical exam: – – – – General: alert, oriented, comfortable Pulse: 95 BP: 138/86 mm Hg CV: irregularly irregular with 2/6 systolic blowing murmur at the apex • Electrocardiogram: atrial fibrillation with a heart rate of 95, possible left ventricular hypertrophy Case 2: ECG Cumulative Mortality (%) Mortality: Rhythm vs. Rate Control (AFFIRM trial) 30 P=0.08 25 20 Rhythm Control 15 Rate Control 10 5 0 0 1 2 3 4 5 Years AFFIRM = Atrial Fibrillation Follow-up Investigation of Rhythm Management. Reprinted with permission from Wyse DG, et al. N Engl J Med 2002;347:1825-33. Management with the rhythm-control strategy offers no survival advantage over the rate-control strategy, and there are potential advantages, such as a lower risk of adverse drug effects, with the rate-control strategy. CHADS2 and Recommended Therapy CHADS2 Score 0 1 ≥2 Recommended Therapy Aspirin (75 mg-325 mg daily) Aspirin (75 mg-325 mg daily) or Warfarin (INR 2.0-3.0) Warfarin (INR 2.0-3.0) Aspirin or no therapy is acceptable for patients less than 60 years of age with no heart disease (lone AF). Singer DE, et al. Chest 2008;133(suppl 6):546S-92S. Cumulative Hazard Rate Stroke/Systemic Embolization: Dabigatran vs. Warfarin Figure shows data from the RE-LY study, displaying cumulative hazard rates for the primary outcome of stroke or systemic embolism. 0.05 0.04 Dabigatran 110 mg 0.03 Warfarin Primary outcome results Warfarin = 1.69% per year Dabigatran (150 mg twice daily) = 1.11% per year 0.02 Dabigatran 150 mg 0.01 0.00 0 6 12 18 Months 24 30 RE-LY = The Randomized Evaluation of Long-Term Anticoagulation Therapy. Reprinted with permission from Connolly S, et al. N Engl J Med 2009;361:1139-51. (P<0.001 for superiority; RR: 0.66) Rates of major bleeding Warfarin = 3.36% per year Dabigatran (150 mg twice daily) = 3.11% per year (P=0.31) Comparing Dabigatran and Warfarin Characteristic Dabigatran Warfarin Dosing Twice daily According to INR Monitoring Half-life Yes Mean: 40 hours Elimination No 13 hours (normal renal function) Renal Drug-drug interactions Few Numerous Drug-food interactions None noted in the prescribing information Numerous U.S. prescribing information for dabigatran and warfarin, 2010. Hepatic Evidence-based Recommendation Recommendation #4: Anticoagulation is recommended for patients with more than one moderate risk factor. Such risk factors include age 75 years or greater, hypertension, heart failure, impaired left ventricular systolic function (ejection fraction 35% or less, or fractional shortening less than 25%), and diabetes mellitus. (I A) ACC/AHA/ESC. Circulation 2006;114:e257-354. Case 3 70-year-old female The Impact of Patient Factors on Choice of Anticoagulant Module 3 Case 3 • 70-year-old female presents with two weeks of palpitations without shortness of breath or chest pain. • Past medical history – Hypertension – Hypercholesterolemia – Congestive heart failure (ejection fraction: 35%) • Medications – Metoprolol, 50 mg twice daily – Lisinopril, 20 mg daily – Atorvastatin, 20 mg daily Case 3 (continued) • Social history: lives with her husband, neither drives; does not smoke or use alcohol • Physical exam: – – – – – – General: alert, interactive, comfortable BP: 128/78 mm Hg Pulse: 80 RR: 16 Lungs: clear CV: irregularly irregular with II/VI systolic murmur left upper sternal border • Electrocardiogram: atrial fibrillation with rate 76 Rate vs. Rhythm Control in CHF Kaplan–Meier Estimates of Death from Cardiovascular Causes (Primary Outcome) Survival Rate (%) 100 Rate Control • Similar outcomes to AFFIRM • No evidence-based benefit of rhythm control over rate control in CHF - No survival advantage - No outcomes advantage 80 Rhythm Control 60 P=0.59 40 20 0 0 12 24 36 48 Months of Follow-up 60 Reprinted with permission from Roy D, et al. N Engl J Med 2008;358:2667-77. Dabigatran: Practical Aspects • Dosing and creatinine clearance >30 ml/min: 150 mg twice daily 15-30 ml/min: 75 mg twice daily <15 ml/min: Do not use • No need for blood level monitoring • Therapeutic level reached within 30 minutes to 2 hours U.S. prescribing information for dabigatran, 2010. Dabigatran: Practical Aspects (continued) • Switching from warfarin to dabigatran – Not much guidance yet available – Wait until INR is below 2.0, then start dabigatran • Surgery – Creatinine clearance ≥50 ml/min: Skip doses for 1-2 days before surgery – Creatinine clearance <50 ml/min: Skip doses for 3-5 days before surgery U.S. prescribing information for dabigatran, 2010. Evidence-based Recommendation Recommendation #5: In patients with atrial fibrillation (AF), including those with paroxysmal AF, who have two or more of the following risk factors for future ischemic stroke, the guidelines recommend longterm anticoagulation with an oral vitamin K antagonist, such as warfarin, targeted at an INR of 2.5 (range: 2.0 to 3.0) because of the increased risk of future ischemic stroke faced by this set of patients. (1A) Risk factors: Age >75 years, history of hypertension, diabetes mellitus, and moderately or severely impaired left ventricular systolic function and/or heart failure ACCP. Chest 2008;133(Suppl 6):546S-92S. Evidence-based Recommendation Recommendation #6: Dabigatran is useful as an alternative to warfarin for the prevention of stroke and systemic thromboembolism in patients with paroxysmal to permanent atrial fibrillation and risk factors for stroke and systemic thromboembolism who do not have a prosthetic heart valve or hemodynamically significant valve disease, severe renal failure (creatinine clearance <15ml/min), or advanced liver disease (impaired baseline clotting function). (I B) ACCF/AHA/HRS. J Am Coll Cardiol 2011;57:1330-7. Balancing Benefit and Risk Module 4 Case 4 85-year-old female with multiple comorbidities Case 4 • 85-year-old female presents for routine physical exam. She has no complaints, and denies chest pain or shortness of breath. • Past medical history – – – – Hypertension Coronary artery disease Congestive heart failure Degenerative joint disease with ambulatory dysfunction Case 4 (continued) • Medications – – – – Atenolol, 25 mg daily Lisinopril, 10 mg daily Hydrochlorothiazide, 12.5 mg daily Aspirin, 81 mg daily • Social history: lives in assisted living and has had numerous falls in past six months; does not smoke or drink alcohol Case 4 (continued) • Physical exam - General: comfortable and interactive BP: 130/80 mm Hg Pulse: 80 Lungs: clear CV: irregularly irregular with I/VI systolic murmur • Electrocardiogram: atrial fibrillation with rate 104 Aspirin Plus Clopidogrel (ACTIVE A Trial) • Aspirin (75 mg-100 mg daily) plus clopidogrel (75 mg daily) reduced stroke risk by 28% - Aspirin stroke risk: 3.3% per year - Combination therapy stroke risk: 2.4% per year Cumulative Incidence 1.0 0.8 0.6 • 2.0% per year incidence of major bleeding (vs. 1.3% with aspirin alone) 0.4 P<0.001 0.2 0.0 Aspirin Only Clopidogrel Plus Aspirin 0 1 2 3 4 Years Adapted with permission from Connolly S. N Engl J Med 2009;360:2066-78. Evidence-based Recommendation Recommendation #7: The selection of antithrombotic agent should be based on the absolute risks of stroke and bleeding, and the relative risk and benefit for a given patient. (I A) ACC/AHA/ESC. Circulation 2006;114:e257-354. Evidence-based Recommendation Recommendation #8: The addition of clopidogrel to aspirin to reduce the risk of major vascular events, including stroke, might be considered in patients with atrial fibrillation in whom oral anticoagulation with warfarin is considered unsuitable due to patient preference or physician assessment of the patient’s ability to safely sustain anticoagulation. (IIb B) ACCF/AHA/HRS. Circulation 2011;123:104-23. Final Comments: Rate vs. Rhythm • There is no significant difference in outcomes for patients, either with or without congestive heart failure, with a strategy of either rate control or rhythm control. Roy D, et al. N Engl J Med 2008;358:2667-77. Wyse DG, et al. N Engl J Med 2002;347:1825-33. Final Comments: Thromboprophylaxis • Assess ALL patients with atrial fibrillation for risk of stroke - Patients with low risk of stroke (CHADS2 score = 0): do not need anticoagulation and may be managed with an antiplatelet agent - All others need anticoagulation, unless there are contraindications - Patients with moderate risk (CHADS2 score = 1): either an antiplatelet or anticoagulation agent is appropriate Thromboprophylaxis (continued) • For patients in whom anticoagulation is contraindicated, an antiplatelet agent is recommended: - Either aspirin or clopidogrel - There may also be a place for the combination of aspirin plus clopidogrel - Combination decreases risk of stroke but increases risk of major bleeds compared to aspirin alone (Connolly S. N Engl J Med 2009;360:2066-78.) Thromboprophylaxis (continued) • Patients with CHADS2 score ≥2 – or patients with score of 1 in whom anticoagulation is indicated – two anticoagulant agents are available. - Dabigatran - Warfarin Thromboprophylaxis (continued) • Decision of which anticoagulant medication to use should be made on an individual basis - Dabigatran has lower risk of stroke and systemic embolism compared with warfarin - Same major bleeding risk at 150 mg twice daily Connolly SJ, et al. N Engl J Med 2009;361:1139-51. Wann LS, et al. Circulation 2011;123:1144-50.