* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download A or V
Heart failure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
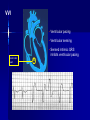
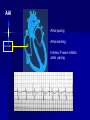
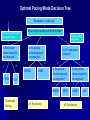
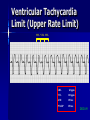
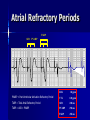
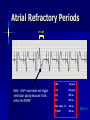
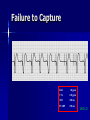
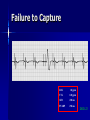
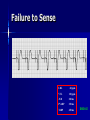
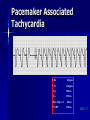
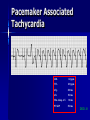
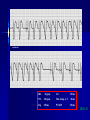
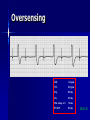
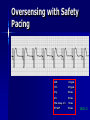
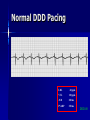
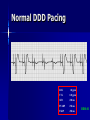
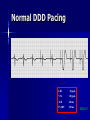
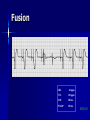
Pacemakers Jonathan MacCabe November 15, 2004 Pacemaker Indications Acquired A/V block in Adults – Class I: There is general agreement that permanent pacemakers should be implanted. Complete heart block, permanent or intermittent, at an anatomic level associated with any on of the following complications: – Symptomatic bradycardia. In the presence of complete heart block symptoms must be presumed to be due the heart block unless proved otherwise – Congestive heart failure – Ectopic rhythms and other medical conditions that require drugs that suppress the automaticity of escape rhythms and result in symptomatic bradycardia. – Documented periods of asystole >= 3.0 s or any escape rate <40/min. in symptom free patients – Confusional states that clear with temporary pacing – Post A/V junctional ablation, myotonic dystrophy Pacemaker Indications Acquired A/V block in Adults – Class I: There is general agreement that permanent pacemakers should be implanted. Second degree A/V block permanent or intermittent, regardless of the type or the site of the block, with symptomatic bradycardia. Atrial fibrillation, Atrial flutter and rare cases of SVT with complete or advanced A/V block, bradycardia and any of the conditions in A1. The bradycardia must be unrelated to digitalis or drugs known to impair A/V conduction. Pacemaker Indications Acquired A/V block in Adults – Class II: Conditions in which permanent pacemakers are frequently used but there is some divergence of opinion about whether they are needed. Asymptotic complete heart block, permanent or intermittent, at any anatomic site, with ventricular rates of 40/min. or faster Asymptomatic type ll second degree block, permanent or intermittent Asymptomatic type I second degree block at intra-His or infra-His levels. – Class III: Conditions in which there is general agreement that pacemakers are not necessary. First degree A/V block Asymptomatic type 1 second degree A/V block at the suprahis level. Pacemaker Indications AV Block Associated with Myocardial Infarction: – Class I: There is general agreement that permanent pacemakers should be implanted. Persistent advanced second degree A/V block or complete heart block after acute myocardial infarction with block in he His-Purkinje system Patients with transient advanced A/V block and associated bundle branch block Pacemaker Indications AV Block Associated with Myocardial Infarction: – Class II: Conditions in which permanent pacemakers are frequently used but there is some divergence of opinion about whether they are needed. Patients with persistent advanced block in the A/V node – Class III: Conditions in which there is general agreement that pacemakers are not necessary. Transient A/V conduction disturbances in the absence of intraventricular conduction defects Transient A/V block in the presence of isolated left anterior hemiblock Acquired left anterior hemiblock in the absence of A/V block. Pacemaker Indications Bifasicular and Trifasicular Block (chronic) – Class I: There is general agreement that permanent pacemakers should be implanted. Bifasicular block with intermittent complete heart block associated with symptomatic bradycardia Bifasicular or Trifasicular block with intermittent type ll second degree A/V block without symptoms attributable to the heart block. Pacemaker Indications Bifasicular and Trifasicular Block (chronic) – Class II: Conditions in which permanent pacemakers are frequently used but there is some divergence of opinion about whether they are needed. Bifasicular or trifasicular block with syncope that is not proved to be due to complete heart block, but other possible causes for syncope are not identifiable Markedly prolonged HV (>100ms) Pacing-induced infra-His block – Class III: Conditions in which there is general agreement that pacemakers are not necessary. Fasicular block without A/V block or symptoms Fasicular block with first degree block without symptoms Pacemaker Indications Sinus Node Dysfunction: – Class I: There is general agreement that permanent pacemakers should be implanted. Sinus node dysfunction with documented symptomatic bradycardia. In some patients this will occur as a consequence of long-term (essential) drug therapy of type and dose for which there are no acceptable alternatives. – Class II: Conditions in which permanent pacemakers are frequently used but there is some divergence of opinion about whether they are needed. Sinus node dysfunction occurring spontaneously or as a result of necessary drug therapy, with heart rates <40/min. when a clear association between significant symptoms consistent with bradycardia and the actual presence of bradycardia has not been documented. Pacemaker Indications Sinus Node Dysfunction: – Class III: Conditions in which there is general agreement that pacemakers are not necessary. Sinus node dysfunction in asymptomatic patients including those in whom substantial sinus bradycardia (heart rate < 40/min.) is a consequence of long-term drug treatment Sinus node dysfunction in patients in whom symptoms suggestive of bradycardia are clearly documented not to be associate with a slow heart rate. Pacemaker Indications Hypersensitive Carotid Sinus and Neurovascular Syndromes – Class I: There is general agreement that permanent pacemakers should be implanted. Recurrent syncope associates with clear, spontaneous events provoked by carotid sinus stimulation; minimal carotid sinus pressure induces asystole of >3 sec. duration in the absence of a medication that depresses the sinus node or A/V node – Class II: Conditions in which permanent pacemakers are frequently used but there is some divergence of opinion about whether they are needed. Recurrent syncope without clear, provocative events and with a hypersensitive cadrioinhibitory response. Syncope with associated bradycardia reproduced by a headup tilt with or without isoproterenol or other forms of provocative maneuvers and in which a temporary pacemaker and second provocative test can establish the likely benefits of a permanent pacemaker Pacemaker Indications Hypersensitive Carotid Sinus and Neurovascular Syndromes – Class III: Conditions in which there is general agreement that pacemakers are not necessary. A hyperactive cardioinhibitory response to carotid sinus stimulation in the absence of symptoms. Vague symptoms, such s dizziness or light-headedness or both, with a hyperactive cardioinhibitory response to carotid sinus stimulation. Recurrent syncope, light-headedness or dizziness in the absence of a cardioinhibitory response. The NASPE / BPEG Generic (I.C.H.D.) The NASPE/BPEG Generic (NBG) Code Position I II III IV V Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Programmability, rate modulation Antitachyarrhythmia Function(s) Letters Used O-None O-None O-None A-Atrium A-Atrium V-Ventricle V-Ventricle D-Dual (A+V) D-Dual (A+V) T-Triggered P-Simple P-Pacing Programmable (antitachyI-Inhibited arrhythmia) M-MultiD-Dual Programmable S-Shock (T+I) C-Communicating D-Dual (P+S) R-Rate modulation S- Single (A or V) S- Single (A or V) Manufacturer’s Designation Only O-None O-None Codes Are Combined To Describe: The mode of pacing The mode of sensing How the pacemaker will respond to the presence or absence of intrinsic beats - AOO - AAI - VOO - VVI The NASPE/BPEG Generic (NBG) Code Position I II III IV V Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Programmability, rate modulation Antitachyarrhythmia Function(s) Letters Used O-None O-None O-None A-Atrium A-Atrium V-Ventricle V-Ventricle D-Dual (A+V) D-Dual (A+V) T-Triggered P-Simple P-Pacing Programmable (antitachyI-Inhibited arrhythmia) M-MultiD-Dual Programmable S-Shock (T+I) C-Communicating D-Dual (P+S) R-Rate modulation S- Single (A or V) S- Single (A or V) Manufacturer’s Designation Only O-None O-None The NASPE/BPEG Generic (NBG) Code Position I II III IV V Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Programmability, rate modulation Antitachyarrhythmia Function(s) Letters Used O-None O-None O-None A-Atrium A-Atrium V-Ventricle V-Ventricle D-Dual (A+V) D-Dual (A+V) T-Triggered P-Simple P-Pacing Programmable (antitachyI-Inhibited arrhythmia) M-MultiD-Dual Programmable S-Shock (T+I) C-Communicating D-Dual (P+S) R-Rate modulation S- Single (A or V) S- Single (A or V) Manufacturer’s Designation Only O-None O-None The NASPE/BPEG Generic (NBG) Code Position I II III IV V Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Programmability, rate modulation Antitachyarrhythmia Function(s) Letters Used O-None O-None O-None A-Atrium A-Atrium V-Ventricle V-Ventricle D-Dual (A+V) D-Dual (A+V) T-Triggered P-Simple P-Pacing Programmable (antitachyI-Inhibited arrhythmia) M-MultiD-Dual Programmable S-Shock (T+I) C-Communicating D-Dual (P+S) R-Rate modulation S- Single (A or V) S- Single (A or V) Manufacturer’s Designation Only O-None O-None The NASPE/BPEG Generic (NBG) Code Position I II III IV V Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Programmability, rate modulation Antitachyarrhythmia Function(s) Letters Used O-None O-None O-None A-Atrium A-Atrium V-Ventricle V-Ventricle D-Dual (A+V) D-Dual (A+V) T-Triggered P-Simple P-Pacing Programmable (antitachyI-Inhibited arrhythmia) M-MultiD-Dual Programmable S-Shock (T+I) C-Communicating D-Dual (P+S) R-Rate modulation S- Single (A or V) S- Single (A or V) Manufacturer’s Designation Only O-None O-None VOO • Ventricular pacing • No sensing • Ventricular asynchronous pacing at lower programmed pacing rate Ventricular lead * AOO • Atrial pacing Atrial lead * • No sensing • Atrial asynchronous pacing at lower programmed pacing rate VVI • Ventricular pacing • Ventricular sensing • Sensed intrinsic QRS inhibits ventricular pacing Ventricular lead * AAI • Atrial pacing • Atrial sensing Atrial lead * • Intrinsic P wave inhibits atrial pacing Dual Chamber Pacing DDD • Pacing in both the atrium and ventricle Atrial lead Ventricular Lead T/I I • Sensing in both the atrium and ventricle * • Intrinsic P wave and intrinsic QRS can inhibit pacing * • Intrinsic P Wave can “trigger” a paced QRS DDD pacing Dual-chamber pacing capable of pacing and sensing in both the atrial and ventricular chambers of the heart 4 distinct patterns can be observed with DDD pacing – Sensing in the atrium and sensing in the ventricle – Pacing in the atrium and sensing in the ventricle – Sensing in the atrium and pacing in the ventricle (“P wave tracking”) – Pacing in the atrium and pacing in the ventricle DDD pacing Example of sensing in both the atrium and the ventricle (inhibiting in both the atrium and the ventricle) DDD pacing Example of pacing in the atrium with sensing (inhibition of pacing) in the ventricle DDD pacing Example of sensing in the atrium (inhibition of atrial pacing) and pacing in the ventricle Also known as “P wave tracking” DDD pacing Example of atrial pacing and ventricular pacing (no inhibition of pacing) DDD Pacing Adapts to changes post-implant May resemble AAI, VAT, VDD, DVI modes Will strive to maintain AV synchrony with variable atrial rates and AV conduction AV Synchrony Cardiac Output = Stroke Volume x Heart Rate Facilitates venous return Increases LVEDP Maintains appropriate opening and closing of A-V valves Pacemaker Syndrome Loss of AV Synchrony Shortness of breath Fatigue Headache Syncope Vertigo CHF, Pulmonary Edema Dizziness Palpitations Pulsations in the neck Chest pain Near Syncope Confusion Hemodynamic Penalties From Loss Of AV Synchrony Loss of atrial contribution Decrease in stroke volume Decrease in cardiac output Decrease in cerebral perfusion Decrease in coronary blood flow Treatment of Pacemaker Syndrome Dual-chamber pacing Normal atrial sensing & capture Appropriate AV Delay Goals of Choosing a Pacing Mode Desire to maintain AV synchrony – DDD mode is best to provide AV synchrony Preservation of AV synchrony requires: – Viable atrium and – Patient must not have chronic/permanent atrial tachyarrhythmias Optimal Pacing Mode Decision Tree Pacemaker is indicated What is the condition of the SA Node? Chronic atrial fibrillation unexcitable atrium Normal or sinus bradycardia Is the patient chronotropically incompetent? Is the patient chronotropically incompetent? Y N N Y DDDR VVIR Is AV conduction adequate? DDD VVI Is the patient chronotropically incompetent? Y DDDR Ventricular Pacing AV Synchrony Y N N DDD Is the patient chronotropically incompetent? Y AAIR AV Synchrony N AAI AV Synchrony - DDD(R) Pacemaker is indicated • Benefits – AV synchrony – Normal sinus response • Risks – Loss of AV conduction What is the condition of the SA node?? Normal or sinus bradycardia Is AV conduction adequate? N Is the patient chronotropically incompetent? Y DDDR N DDD Ventricular Pacing Pacemaker is indicated Chronic atrial fibrillation unexcitable atrium Is the patient chronotropically incompetent? Y VVIR N VVI What is the condition of the SA node? • Benefits – Maintain minimum cardiac output – Single-lead implantation • Risks – Loss of AV synchrony – Retrograde conduction – Increased incidence of atria arrhythmias Rate Modulation/Rate Responsive Mode Rate Responsiveness/AdaptiveRate Pacing In Rate Responsive pacing (modes ending with “R”), sensor(s) in pacemaker are used to detect changes in physiologic needs and increase the pacing rate accordingly The sensor – Sensors are used to detect changes in metabolic demand – Sensors sense motion (piezoelectric crystal or accelerometer) or use a physiologic indicator, e.g., minute ventilation The algorithm – Within the software of the pacemaker – Uses the input from the sensor to determine the appropriate paced heart rate for the activity DDDR Pacing Example of Dual-Chamber RateResponsive pacing DDDR A DDDR pacemaker has two or more indicators of a patient’s metabolic need: – Sinus node – the best indicator, as it is physiologic – Input from the sensor(s) within the pacemaker Pacemaker Timing and Function Lower Rate Limit LRL LRL LRL LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms Ventricular Tachycardia Limit (Upper Rate Limit) VTL VTL VTL LRL 60 ppm VTL 120 ppm AVD 150 ms PVARP 250 ms DDD-09 A-V Delay AVD AV AV AVD AVD AV LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms A-V Delay AV p AV s LRL 60 ppm VTL 120 ppm AVp 200 ms Avs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms Atrial Refractory Periods TARP AVD PVARP LRL 60 ppm PVARP = Post Ventricular Activation Refractory Period VTL 120 ppm TARP = Total Atrial Refractory Period AVD 200 ms TARP = AVD + PVARP PVARP 250 ms TARP 450 ms Atrial Refractory Periods PVARP Note: this P wave does not trigger ventricular pacing because it falls within the PVARP LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-16 Pacemaker Malfunctions Failure to Capture LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms DDD-22 Failure to Capture LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms DDD-23 Failure to Sense LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms TARP 450 ms DDD-02 Pacemaker Associated Heart Block LRL 60 ppm VTL 120 ppm AVD 150 ms PVARP 350 ms DDD-12 Pacemaker Associated Heart Block Note: AVD is extended to preserve the upper rate limit LRL 60 ppm VTL 120 ppm AVD 150 ms PVARP 250 ms DDD-14 “Pacemaker Wenkebach” LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-15 Pacemaker Associated Tachycardia LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-17 Pacemaker Associated Tachycardia LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-18 continuous LRL 60 ppm AVs VTL 100 ppm Min. Adap. A-V AVp 200 ms PVARP 150 ms 88 ms 250 ms DDD-19 Oversensing LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-20 Oversensing with Safety Pacing LRL 60 ppm VTL 120 ppm AVp 200 ms AVs 150 ms Min. Adap. A-V PVARP 88 ms 250 ms DDD-21 Is This a Pacemaker Malfunction? Normal DDD Pacing LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms DDD-08 Normal DDD Pacing LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms TARP 450 ms DDD-01 Normal DDD Pacing LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms DDD-07 Fusion LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms DDD-05 Safety Pacing LRL 60 ppm VTL 120 ppm AVD 200 ms PVARP 250 ms TARP 450 MS DDD-04 The End