* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Where There Is Blood, There Is a Way
Survey
Document related concepts
Transcript
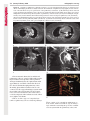
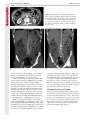
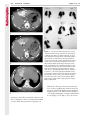
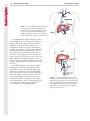
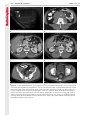
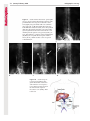
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT 67 Where There Is Blood, There Is a Way: Unusual Collateral Vessels in Superior and Inferior Vena Cava Obstruction1 Online-Only CME See www.rsna .org/education /rg_cme.html LEARNING OBJECTIVES After reading this article and taking the test, the reader will be able to: ■■List the common collateral pathways in patients with SVC or IVC obstruction. ■■Discuss the uncommon collateral pathways in patients with SVC or IVC obstruction. ■■Describe the imaging features of the uncommon collateral pathways in SVC or IVC obstruction. Sangita Kapur, MD • Eugene Paik, MD • Ario Rezaei, MD Doan N.Vu, MD Obstruction of the superior vena cava (SVC) or inferior vena cava (IVC) is most commonly an acquired condition, typically caused by malignancy, benign conditions such as mediastinal fibrosis, and iatrogenic causes such as venous catheterization. In the event of chronic occlusion, collateral pathways must develop to maintain venous drainage. The major collateral pathways seen with SVC or IVC obstruction are well described and include the azygos-hemiazygos, internal and external mammary, lateral thoracic, and vertebral pathways. In addition, several unusual collateral pathways may be seen with SVC or IVC obstruction; these include systemic-to-pulmonary venous, cavoportal, and intrahepatic collateral pathways. In patients with systemic-to-pulmonary venous collateral vessels, the systemic veins drain directly into the left side of the heart, resulting in a right-to-left shunt. The collateral veins consist of mediastinal connections between the innominate veins and the superior pulmonary veins through bronchial venous plexuses around the airways, hilar vessels, and pleura. The cavoportal collateral pathways consist of collateral formation between the SVC or IVC and a tributary to the portal system. They include the caval-superficial-umbilical-portal pathway, caval-mammary-phrenic–hepatic capsule–portal pathway, caval-mesenteric-portal pathway, caval-renal-portal pathway, caval-retroperitonealportal pathway, and intrahepatic cavoportal pathway. These types of collateral pathways may result in unusual enhancement patterns in the liver. An understanding of these unusual collateral pathways is essential in a patient with caval occlusion who presents with signs and symptoms of a right-to-left shunt or has unusual enhancing lesions in the liver. © RSNA, 2010 • radiographics.rsna.org Abbreviations: IVC = inferior vena cava, SVC = superior vena cava RadioGraphics 2010; 30:67–78 • Published online 10.1148/rg.301095724 • Content Code: From the Department of Radiology, University of Cincinnati Medical Center, 234 Goodman Street, Cincinnati, OH 45267-0761 (S.K., A.R., D.N.V.); and the Department of Radiology, Christ Hospital, Cincinnati, Ohio (E.P.). Received April 3, 2009; revision requested May 29 and received July 31; accepted September 15. All authors have no financial relationships to disclose. Address correspondence to S.K. (e-mail: [email protected]). 1 The Editor has no relevant financial relationships to disclose. © RSNA, 2010 68 January-February 2010 Introduction Obstruction of the superior vena cava (SVC) or inferior vena cava (IVC) is typically an acquired condition. SVC syndrome is most commonly associated with metastatic pulmonary or mediastinal malignancy (1). Benign causes include infection, idiopathic mediastinal fibrosis, retrosternal thyroid, aortic aneurysm, benign tumors, mediastinal hematoma, sarcoidosis, radiation fibrosis, and iatrogenic causes (2–5). Thrombosis of the SVC is a well-known complication of central venous catheter placement (2,3). Thrombosis is a major cause of IVC obstruction and often results from superior extension of lower extremity or pelvic deep venous thrombosis (6). Causes such as dehydration, sepsis, pelvic inflammatory disease, coagulopathy, congestive heart failure, trauma, immobility, severe exertion, or iatrogenic causes (eg, placement of an IVC filter) may also result in IVC thrombosis. Other less common causes of IVC obstruction include tumor invasion, extrinsic compression, and intrinsic caval disease, (eg, congenital membranes or primary caval tumors) (6). In the event of chronic occlusion, collateral pathways must develop to maintain venous drainage (1,2,5,6) The pattern of collateral pathways can be predicted on the basis of the level of obstruction. The following four major collateral pathways are commonly reported in SVC or IVC obstruction (1,2,5,6). 1. The azygos-hemiazygos pathway includes the azygos, hemiazygos, intercostal, and lumbar veins. 2. The internal and external mammary pathway includes the internal mammary, superior epigastric, and inferior epigastric veins and superficial veins of the thorax. radiographics.rsna.org 3. The lateral thoracic pathway uses the lateral thoracic, thoracoepigastric, superficial circumflex, long saphenous, and femoral veins to collateralize to the IVC. 4. The vertebral pathway uses the innominate, vertebral, intercostal, lumbar, and sacral veins to collateralize to the azygos and internal mammary pathways. The azygos-hemiazygos pathway predominates unless it is poorly developed or obstruction blocks the azygos vein confluence with the SVC (2,6,7). In addition, gonadal and periureteric veins can also function as collateral vessels in infrarenal IVC obstruction (Fig 1) (6). Certain unusual collateral circulations may also develop with SVC or IVC obstruction. In this article, the systemic-to-pulmonary venous collateral pathway, cavoportal collateral pathway, and intrahepatic collateral pathway are discussed. Unusual Collateral Pathways Systemic-to-Pulmonary Venous Collateral Pathway The systemic-to-pulmonary venous collateral pathway is an uncommon result of SVC obstruction (1,2,5,8–11). The presence of such collateral vessels results in a right-to-left shunt, subsequently leaving the patient susceptible to stroke, brain abscess, and a high cardiac output state (4). This pathway is usually the result of SVC obstruction from malignant causes, but it may rarely be caused by benign conditions (8). The pathway consists of mediastinal connections between the innominate veins and the superior pulmonary veins via the bronchial venous plexuses around the airways, hilar vessels, and pleura (8) (Fig 2). These shunts may be further categorized as anatomic, congenital, or acquired (8). Teaching Point Teaching Point RG • Volume 30 Number 1 Kapur et al 69 Figure 1. Cavocaval collateral vessels in a 61-year-old woman with a primary leiomyosarcoma of the IVC. The leiomyosarcoma produced obstruction below the level of the renal veins and resulted in cavocaval collateralization through the left gonadal vein. (a–c) Axial (a, b) and coronal (c) contrast material–enhanced computed tomographic (CT) images (a obtained at a higher level than b) show a large IVC mass (arrowheads) that causes IVC obstruction. A large left gonadal vein (arrows) acts as a collateral vessel between the IVC below the mass and the IVC above the mass. (d, e) Images from venography performed with a right common femoral approach show the IVC obstruction (arrowheads in d) and unnamed small collateral vessels (arrowheads in e) between the right common iliac vein and the left gonadal vein (arrows). LIV in e = left common iliac vein. 70 January-February 2010 radiographics.rsna.org Figure 2. Systemic-to-pulmonary collateral vessels in a 37-year-old woman with a history of end-stage renal disease and multiple placements of dialysis catheters. She underwent CT pulmonary angiography because of shortness of breath. There was poor opacification of the pulmonary vasculature. (a, b) CT images show collateral vessels around the left pulmonary artery (arrow in a) and the left main-stem bronchus (arrow in b). (c) Coronal multiplanar reformation image shows systemic-to-pulmonary collateral vessels (arrows) surrounding the left pulmonary artery and left main-stem bronchus with opacification of the left superior pulmonary vein (arrowhead). (d) Coronal maximum intensity projection image shows stenosis of the left brachiocephalic vein (arrow) and collateral vessels at the left pulmonary hilum (arrowhead). (e) Volume-rendered image shows collateral vessels at the left pulmonary hilum (arrow) and a pericardiophrenic collateral vessel (arrowhead). 1. In an anatomic shunt, the bronchial and pulmonary veins are connected through preexisting bronchial venous plexuses. These plexuses drain predominantly into the right atrium, with approximately one-third of their flow directed into the left atrium through pulmonary veins. Normally, pleurohilar bronchial veins are also connected to the azygos-hemiazygos system with intervening valves. If systemic venous pressure rises, as in caval obstruction, the valves can become incompetent with resultant reversal of flow and a right-to-left shunt. 2. There are three types of congenital systemic-to-pulmonary venous collateral pathways. These consist of (a) anomalous pulmonary venous return, with reversed flow; (b) an embryologic remnant connecting the posterior cardinal venous system with the pulmonary veins; and RG • Volume 30 Number 1 Kapur et al 71 Figure 3. Spontaneous cavoportal collateral vessel in a 45-year-old man. Axial (a) and coronal (b, c) contrast-enhanced CT images show a spontaneous collateral vessel (white arrow in c), which connects the IVC circulation (arrowheads in c) with the inferior mesenteric vein (ie, portal) circulation (black arrows). (c) a persistent left SVC, which may occasionally be a thin channel that drains into the left superior pulmonary vein or left atrium. 3. The acquired type of systemic-to-pulmonary venous collateral system is inflammatory in origin and results in newly formed vessels bridging subpleural pulmonary veins and intercostal veins through pleural adhesions. The formation of this systemic-to-pulmonary shunt is theorized to arise from adhesions between the chest wall and lung, allowing bridging veins to develop across the pleural space (8,9). Fibrosing mediastinitis, adhesions, radiation fibrosis, and chronic inflammation have been postulated as contributing factors (9–12). Methods for depicting right-to-left shunts include scintigraphy (eg, technetium 99m [99mTc] macroaggregated albumin scanning), venography, and helical CT. CT venography has recently been explored for depiction of such shunts (9), as multidetector CT and three-dimensional reformation can aid in delineation and diagnosis of this complex anatomy (Fig 2). CT can also help identify the underlying cause of obstruction, its exact level, and other potential collateral pathways. Keys to visualization of these vessels at cross-sectional imaging include presence of extensive obstruction, use of dynamic high-contrast spiral CT technique, and abundant collateral vessels (11). Cavoportal Collateral Pathway Another unusual but important collateral pathway is the cavoportal collateral pathway, whereby flow is directed from the vena cava to the portal vein (13). In contradistinction, portocaval collateral vessels are frequently visualized with portal hypertension, where blood flow is hepatofugal (13). On occasion, cavoportal collateral vessels may form spontaneously (Fig 3). 72 January-February 2010 Teaching Point A brief review of the developmental embryology will facilitate a better understanding of these collateral pathways. The developing visceral veins consist of the right and left vitelline veins from the yolk sac and the right and left umbilical veins from the placenta. These veins open into corresponding horns of the sinus venosus. The vitelline veins anastomose with each other around the developing duodenum and pass through the septum transversum (the primitive liver) to the sinus venosus. In the primitive liver, these veins are broken up into sinusoids. The left vitelline vein disappears, and blood is redistributed to a now enlarged right vitelline vein. The vitelline system gives rise to the suprahepatic IVC, the hepatic veins, and the portal vein (14,15). The umbilical veins carry oxygenated blood to the embryo. The right umbilical vein and the portion of the left umbilical vein between the liver and the sinus venosus degenerate. The remainder of the left umbilical vein then carries all the blood from the placenta to the fetus. A large channel known as the ductus venosus develops in the liver and connects the umbilical vein with the IVC, bypassing the sinusoidal circulation of the liver (14,15). The complicated development of the cardinal system and the close relationship of its development with that of the vitelline and umbilical veins may explain the occurrence of congenital portosystemic anastomoses (14). The normal existence of portosystemic connections was observed by Ruysch in 1738 (16). Madden identified preexisting portosystemic connections in 50% of normal individuals after death (17). Two embryologic hepatofugal collateral channels were observed by McIndoe (17). 1. One is at the site of the obliterated fetal circulation in the falciform ligament comprising the umbilical and paraumbilical veins. 2. Another is at areas where the gastrointestinal tract becomes retroperitoneal developmentally (ie, where the bare areas come in contact with somatic tissues): the duodenum, pancreas, spleen, colon, and liver. The presumed basis for intrahepatic portosystemic shunts is a persistent communication between the vitelline veins of the omphalomesenteric system and the sinus venosus owing to a focal absence of sinusoid formation (14). radiographics.rsna.org Figure 4. Caval-superficial-umbilical-portalpathway. Diagram shows SVC or IVC obstruction and cavoportal collateral pathways. The epigastric venous tributaries of the caval circulation anastomose with a recanalized paraumbilical vein, which in turn drains into the left portal vein. EMV = external mammary vein, EV = epigastric vein, IEV = inferior epigastric vein, IMV = internal mammary vein, SEV = superior epigastric vein. The term downhill varices was used by Felson and Lessure (18) to describe a type of cavoportal collateral pathway in the case of SVC obstruction. The lower part of the esophageal venous plexus communicates with the coronary vein of the portal system inferiorly, while superiorly it communicates with the azygos system. Thus, the lower esophageal veins join the azygos system with the portal system. In patients with SVC obstruction below the azygos vein entry, this communication can divert blood to the portal system, with the flow directed toward the portal system or “downhill” (18). Four cavoportal collateral pathways have been identified. 1. Caval-superficial-umbilical-portal pathways may be seen with either SVC or IVC obstruction (Fig 4). The superficial, superior, and inferior epigastric veins anastomose with external or internal RG • Volume 30 Number 1 Kapur et al 73 Figure 5. Cavoportal collateral vessels in a 21-yearold woman with end-stage renal disease and a history of multiple placements of dialysis catheters. (a) Contrast-enhanced CT image shows wedge-shaped hyperenhancement of segment IV of the liver, prominent collateral vessels in the anterior abdominal wall (arrowheads), and a recanalized paraumbilical vein (arrow). (b) Contrast-enhanced CT image shows the recanalized paraumbilical vein communicating with a portal vein branch (arrowhead). (c) Contrast-enhanced CT image shows reflux of contrast material into hepatic veins (arrow). (d) Multiple images from the perfusion portion of a 99mTc macroaggregated albumin ventilation-perfusion study show increased uptake in segment IV of the liver (arrow). LAO = left anterior oblique, L lat = left lateral, LPO = left posterior oblique, RAO = right anterior oblique, RPO = right posterior oblique, Rt lat = right lateral. fashion into the left portal vein (13). The presence of such a pathway may result in a hot spot at hepatic segment IV during nuclear medicine studies, such as 99mTc sulfur colloid scanning or 99m Tc lung scintigraphy, or in hyperenhancement at venography or CT (Fig 5) (4,5,7,12,19–22). mammary veins. These superficial collateral veins then communicate with a recanalized paraumbilical vein, which in turn drains in a hepatopetal 74 January-February 2010 radiographics.rsna.org Figure 6. Caval-mammary-phrenic–hepatic capsule–portal pathway. Diagram shows SVC obstruction. There is collateral formation between the internal mammary vein (IMV) and hepatic capsular veins, which ultimately drain into the portal venous system. 2. Caval-mammary-phrenic–hepatic capsule– portal pathways are seen with SVC obstruction. In this pathway, blood flows from the internal mammary vein to the inferior phrenic vein. The inferior phrenic vein then communicates with hepatic capsular veins, which in turn drain into the intrahepatic portal tributaries (Fig 6). A focal hot spot may be visualized on nuclear medicine scans along the anterior and superior aspect of the liver, near the bare area. Focal contrast enhancement along the superior aspect of the liver and enlarged inferior phrenic veins and hepatic capsular collateral vessels can be seen at CT (13). 3. Caval-mesenteric-portal pathway: In IVC obstruction, venous blood may drain from the internal iliac veins to the hemorrhoidal plexus. From there, blood flow can ascend through the inferior mesenteric vein to the portal vein (Fig 7). Thus, the pathway is located between the superior rectal branches of the inferior mesenteric vein and the middle and inferior rectal branches of the internal iliac veins (13). This pathway may be visualized with CT (Fig 8), magnetic resonance imaging, or angiography (Fig 9). Figure 7. Caval–inferior mesenteric–portal pathway. Diagram shows IVC obstruction and collateral vessels from the caval system (internal iliac vein [IIV]) and the hemorrhoidal venous plexus, which drain into the portal venous system. IMV = inferior mesenteric vein, SMV = superior mesenteric vein. RG • Volume 30 Number 1 Kapur et al 75 Figure 8. Caval–inferior mesenteric–portal pathway in a 35-year-old man with testicular cancer, retroperitoneal adenopathy, IVC thrombosis, and formation of cavoportal collateral vessels. (a) Longitudinal ultrasonographic image of the right testicle shows a mass (arrow) and a dystrophic calcification (arrowhead). (b) Contrast-enhanced CT image shows retroperitoneal adenopathy (arrow). (c) Contrast-enhanced CT image shows unopacified blood from the inferior mesenteric vein (arrowhead) draining into the splenic vein (arrow). (d) Contrastenhanced CT image shows unopacified blood in the inferior mesenteric vein (arrow). (e) Contrast-enhanced CT image shows the hemorrhoidal vein and collateral vessels (arrow). (f) Contrast-enhanced CT image shows hemorrhoidal collateral vessels (arrow). 76 January-February 2010 radiographics.rsna.org Figure 9. Caval–inferior mesenteric–portal pathway in a 45-year-old woman with occlusion of the proximal IVC and cavoportal collateral vessels. Venography was performed with a left common iliac approach. (a, b) Venograms show superior hemorrhoidal collateral vessels (arrow in a), which drain into the inferior mesenteric vein (arrow in b). (c) Venogram shows the inferior mesenteric vein draining into the splenic vein (portal system) (arrow). Arrowhead = occlusion of the proximal IVC. (d) Delayed venogram shows hepatic enhancement (arrow), which was due to the cavoportal collateralization. Figure 10. Caval-retroperitoneal-portal pathway. Diagram shows IVC obstruction and formation of retroperitoneal collateral vessels between the IVC and the superior mesenteric vein (SMV). RV = renal vein. RG • Volume 30 Number 1 Kapur et al 77 Figure 11. Intrahepatic collateral vessels in a 60-year-old man who underwent venography for evaluation for filter placement. (a) Venogram shows IVC occlusion by a web (white arrow) and an inferior hepatic vein (black arrow). (b) Venogram shows opacification of the IVC superior to the obstruction (white arrow). The opacification is due to intrahepatic collateralization between the inferior hepatic vein (arrowheads) below the level of the obstruction and the right and middle hepatic veins (black arrow). The flow in the inferior hepatic vein is retrograde, as evidenced by the higher opacity of the contrast material within it. The opacity of the contrast material in the right and middle hepatic veins is lower because they fill by means of collateral flow. Teaching Point 4. Caval-renal-portal and caval-retroperitonealportal pathways have mainly been reported with mid-IVC occlusion (13). In IVC obstruction, as in portal hypertension, the left renal vein can develop connections to the splenic vein via an inferior phrenic vein and the epiploic veins of the stomach. Other tributaries of the portal system such as duodenal, jejunal, and pancreatic veins may communicate with retroperitoneal branches of the renal or lumbar veins. These in turn are tributaries of the IVC and azygos system (Fig 10). The establishment of this collateral pathway may result in duodenal varices (13). As mentioned earlier, the cavoportal collateral pathway may result in enhancement abnormalities in the liver and hot spots during nuclear medicine studies (13). Two methods may be used to differentiate the commonly seen portocaval collateral vessels from the uncommon cavoportal collateral vessels: (a) Knowledge of the site of venous obstruction, whether caval or portal, can help determine the direction of flow within the collateral vessel. (b) The opacity or attenuation of contrast material in the collateral vessels is an important determinant, as the opacity or attenuation of contrast material in the collateral vessel matches the venous system from where the blood flows. Therefore, the opacity or attenuation of contrast material in the collateral vessel will match the cava in the case of cavoportal collateral vessels and will match the portal circulation in the case of portocaval collateral vessels (Figs 1, 8). It is also important to note the site of contrast material injection, whether the upper or lower extremity, as this will also determine whether the collateral vessel will enhance. Therefore, the degree of enhancement of the collateral veins, in conjunction with knowledge of the site of injection, can provide important information about flow direction in the collateral circulation (4). Intrahepatic Collateral Pathway Intrahepatic communications between the hepatic veins can be demonstrated at hepatic venography or in anatomic or autopsy studies. This pathway is unique in that it is seen only with obstruction of the intrahepatic cava or occlusion of the right or left hepatic venous orifice. Over time, patients with intrahepatic IVC obstruction will develop collateralization between the hepatic vein branch that drains into the IVC proximal to the obstruction and the hepatic vein branch distal to the obstruction (23,24). The blood from the IVC below the obstruction can then drain into the right atrium (Fig 11). The blood flow in the hepatic venous branch proximal to the obstruction is retrograde (23,24). These collateral vessels are usually insufficient to prevent Budd-Chiari syndrome (23). 78 January-February 2010 Conclusions Teaching Point The presence of systemic-to-pulmonary or cavoportal collateral vessels suggests SVC or IVC obstruction. Evidence of a right-to-left shunt and focal characteristic enhancement in the liver (pseudolesion) may be detected at contrastenhanced CT. Because the preferential collateral pathway is the azygos-hemiazygos pathway, that focal liver enhancement pattern is not commonly seen. If such focal liver enhancement is visualized at CT or a focal hot spot is seen on a nuclear medicine scan, a search for possible obstruction of the SVC or IVC should be made (7). The existence of collateral vessels and caval obstruction allows differentiation of these enhancement abnormalities from enhancement due to liver masses (13,17). If the shunting is considerable, the hepatic perfusion abnormality may also be demonstrated at angiography (12). From a practical point of view, care should be taken when interpreting a defect in segment IV of the liver at CT, especially in the presence of known or potential SVC or IVC obstruction. References 1.Wilson ES. Systemic to pulmonary venous communication in the superior vena caval syndrome. AJR Am J Roentgenol 1976;127(2):247–249. 2.Cihangiroglu M, Lin BH, Dachman AH. Collateral pathways in superior vena caval obstruction as seen on CT. J Comput Assist Tomogr 2001;25(1):1–8. 3.Madan AK, Allmon JC, Harding M, Cheng SS, Slakey DP. Dialysis access-induced superior vena cava syndrome. Am Surg 2002;68(10):904–906. 4.Bashist B, Parisi A, Frager DH, Suster B. Abdominal CT findings when the superior vena cava, brachiocephalic vein, or subclavian vein is obstructed. AJR Am J Roentgenol 1996;167(6):1457–1463. 5.Holemans JA, Howlett DC, Rankin SC. Superior vena cava obstruction: unusual findings due to venous collaterals. Clin Radiol 1997;52(7):559–560. 6.Sonin AH, Mazer MJ, Powers TA. Obstruction of the inferior vena cava: a multiple-modality demonstration of causes, manifestations, and collateral pathways. RadioGraphics 1992;12:309–322. 7.Herbener TE, Basile V, Nakamoto D, Butler HE, Pickering SP. Focal liver enhancement on contrastenhanced CT scan caused by obstruction of the superior vena cava (SVC). AJR Am J Roentgenol 1997;169(1):250, 253–254. radiographics.rsna.org 8.Grayet D, Ghaye B, Szapiro D, Dondelinger RF. Systemic-to-pulmonary venous shunt in superior vena cava obstruction revealed on dynamic helical CT. AJR Am J Roentgenol 2001;176(1):211–213. 9.Kim HC, Chung JW, Park SH, et al. Systemic-topulmonary venous shunt in superior vena cava obstruction: depiction on computed tomography venography. Acta Radiol 2004;45(3):269–274. 10.Stockberger SM, West KW, Cohen MD. Right to left shunt from systemic venous to pulmonary venous system developing after SVC obstruction. J Comput Assist Tomogr 1995;19(2):312–315. 11.Ho HT, Horowitz AL, Ho AC. Systemic to pulmonary venous communication (right-to-left shunt) in superior vena cava obstruction demonstrated by spiral CT. Br J Radiol 1999;72(859):712–713. 12.Nguyen BD, Roarke MC. Superior vena cava obstruction with intrahepatic and systemic-pulmonary venous right-to-left shunts. Clin Nucl Med 2004;29 (8):491–493. 13.Dahan H, Arrive L, Monnier-Cholley L, Le Hir P, Zins M, Tubiana JM. Cavoportal collateral pathways in vena cava obstruction: imaging features. AJR Am J Roentgenol 1998;171(5):1405–1411. 14.Gallego C, Miralles M, Marín C, Muyor P, González G, García-Hidalgo E. Congenital hepatic shunts. RadioGraphics 2004;24(3):755–772. 15.Singh IB, Pal GP. Cardiovascular system. In: Human embryology. 7th ed. Chennai, India: Macmillan India Press, 2001; 250–252. 16.Edwards EA. Functional anatomy of the portasystemic communications. AMA Arch Intern Med 1951;88(2):137–154. 17.Fleming RJ, Seaman WB. Roentgenographic demonstration of unusual extra-esophageal varices. Am J Roentgenol Radium Ther Nucl Med 1968;103(2): 281–290. 18.Felson B, Lessure AP. “Downhill” varices of the esophagus. Chest 1964;46:740–746. 19.Lee KR, Preston DF, Martin NL, Robinson RG. Angiographic documentation of systemic-portal venous shunting as a cause of a liver scan “hot spot’’ in superior vena caval obstruction. AJR Am J Roentgenol 1976;127(4):637–639. 20.Dickson AM. The focal hepatic hot spot sign. Radiology 2005;237:647–648. 21.Yoshimitsu K, Honda H, Kuroiwa T, et al. Unusual hemodynamics and pseudolesions of the noncirrhotic liver at CT. RadioGraphics 2001;21(spec issue):S81–S96. 22.Baba Y, Miyazono N, Inoue H, et al. Altered flow dynamics of intravascular contrast material to the liver in superior vena cava syndrome: CT findings. Abdom Imaging 2000;25(2):146–150. 23.Kamba M, Ochi S, Ochi H, Maruyama S, Suto Y. Asymptomatic membranous obstruction of the inferior vena cava forming intrahepatic collateral pathways. J Gastroenterol 1995;30(6):783–785. 24.Salomonowitz E, Castaneda-Zuniga WR, Bass JL, Lund G, Cragg AH, Amplatz K. Transhepatic collateral pathway due to vena caval obstruction. AJR Am J Roentgenol 1984;142:1210–1212. This article meets the criteria for 1.0 AMA PRA Category 1 Credit TM. To obtain credit, see www.rsna.org/education /rg_cme.html. RG Volume 30 Number 1 January-February 2010 Kapur et al Where There Is Blood, There Is a Way: Unusual Collateral Vessels in Superior and Inferior Vena Cava Obstruction Sangita Kapur, MD, et al RadioGraphics 2010; 30:67–78 • Published online 10.1148/rg.301095724 • Content Code: Page 68 The presence of such collateral vessels results in a right-to-left shunt, subsequently leaving the patient susceptible to stroke, brain abscess, and a high cardiac output state (4). Page 68 The pathway consists of mediastinal connections between the innominate veins and the superior pulmonary veins via the bronchial venous plexuses around the airways, hilar vessels, and pleura (8) (Fig 2). Page 72 The complicated development of the cardinal system and the close relationship of its development with that of the vitelline and umbilical veins may explain the occurrence of congenital portosystemic anastomoses (14). Page 77 The opacity or attenuation of contrast material in the collateral vessels is an important determinant, as the opacity or attenuation of contrast material in the collateral vessel matches the venous system from where the blood flows. Page 78 Because the preferential collateral pathway is the azygos-hemiazygos pathway, that focal liver enhancement pattern is not commonly seen. If such focal liver enhancement is visualized at CT or a focal hot spot is seen on a nuclear medicine scan, a search for possible obstruction of the SVC or IVC should be made (7).