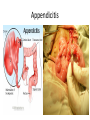
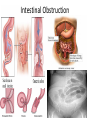
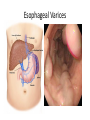
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File - Emergency Assessment Skills
Survey
Document related concepts
Transcript
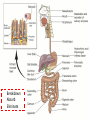
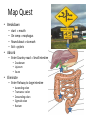
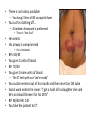
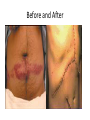
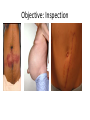
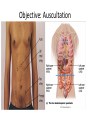
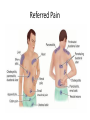
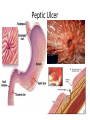
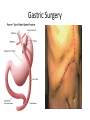
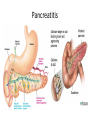
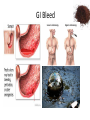
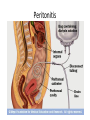
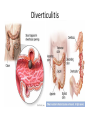
Acute GI Part 1 and 2 Statistics • What percentage of patients presenting to emergency departments offer abdominal pain as their chief complaint? • 31.8% or 5.8 million people (1999-2000) • This number increased to 7 million (20072008) • Of the 7 million cases between 2007 and 2008 what percent arrived by ambulance? • 26.9% CDC.gov Breakdown Absorb Eliminate Map Quest • Breakdown – – – – start = mouth On ramp = esophagus Round about = stomach Exit = pyloris • Absorb – Enter Country road = Small intestine • Duodenum • Jejunum • Ileum • Eliminate – Enter Parkway to large intestine • • • • • Ascending colon Transverse colon Descending colon Sigmoid colon Rectum Digestion • Mouth – Chewing and swallowing (CNS) • Stomach – – – – Hydrochloric Acid Pepsin Intrinsic Factor B12 absorption Peristalsis outward • Small intestine – Duodenal secretions • Amylase, Lipase pancreatic enzymes (bicarbonate) • Bile from liver to gallbladder via common bile duct – Fat/protein/carbohydrates – Nutrients & Vitamins absorbed • Large intestine – Ileocecal valve colon – Bacteria breakdown remaining waste – Slow peristalsis water and electrolytes reabsorbed Case Study • “After every time I eat a meal within 20 minutes I have the immediately go to the bathroom. I also become very bloated and "gassy" almost nauseous, but never threw up, only go to the bathroom and it goes away until I eat again. At first I thought I was lactose-intolerant (because my sister 22, just developed a severe case out of no where) but it isn't just dairy that causes this, it is with any food. My brother of 25 also suffers from very similar symptoms.” WebMD Forum Case Study • A 67 year old male involved in an MVC. Witnesses say he drifted into oncoming traffic on Ridge Road and struck another vehicle head-on. • He was a restrained driver, there was significant passenger side compartment intrusion. The passenger, an elderly woman, remains trapped in the vehicle, Mercy Flight is en route to the scene • The patient is hypotensive with 2 BP readings in the 70’s. His HR is 140. He is still awake, moaning in pain. – Based on Trauma Activation Criteria and Level I Trauma Alert is issued • • • • An OR is prepped A cooler of type O negative is prepared A CT scanner is held The Trauma Team Assembles • The patient arrives to ED. – What is you first priority? • There is no history available – You hang 2 liters of NS via rapid infuser • You cut his clothing off… – A bedside ultrasound is preformed • There is “free fluid” • He vomits • His airway is compromised • He is intubated • • • • BP= 60/40 You give 2 units of blood BP: 70/40 You give 2 more units of blood – The CT tech yells out “we’re ready” • You suction emesis out of his mouth and then insert an OG tube • Social work enters the room: “I got a hold of his daughter she said he’s on blood thinners for his DVTs” • BP: 80/60 HR: 130 • You take the patient to CT Group Work • The CT scan reveals a liver laceration. The patient is taken to the OR. The surgery went well and the damage was repaired. The patient was extubated and is hemodynamically stable. He was transferred to a floor. His sister, the elderly passenger, is still in the ICU. • You are the nurse assigned to this patient Before and After Triage • Anticipate/Coordinate/Evaluate (ACE) – Is this new or old? – Is this expected or unexpected? – What is the patients “normal”? – Is this life threatening? – Can the cause long-term harm? – Is this time sensitive? • BP/HR/RR/Sat/T + pain score • What are the physiological signs of pain? Subjective Data • • • • • • • • OLDCART Onset Location Duration Characteristics Aggravating Factors Relieving Factors Treatments • Focused History – – – – – – – – – – Abdominal Pain Dyspepsia Gas Nausea Vomiting Diarrhea Constipation Fecal incontinence Jaundice Previous GI disease • http://www.youtube.com/ watch?v=UM-HWkbnDfg Objective: Inspection Inspection Surface/contour/movement • Scars – Describe (length/location/character) • Striae – Pink-purple = Cushings • Dilated veins – Cirrhosis or inferior vena cava obstruction • • Rashes/Lesions Contour – – – – – – – • Flat/rounded/protuberant ascites pregnancy hernia distended bladder AAA Mass Peristalsis – Observe for several minutes if you suspect obstruction – Increased waves with obstruction • Pulsations – Aortic aneurysm (AAA) Objective: Auscultation Auscultation • Listen prior to percussion/palpation • Bowel sounds – one spot RLQ is usually sufficient – 5 to 34 per minute normal – Altered with diarrhea, intestinal obstruction, paralytic ileus, and peritonitis • Bruits – Suggest vascular occlusive disease – Listen over aorta, iliac arteries, femoral arteries – May be heard in systole normally, having a bruit in diastole is more indicative of arterial insufficiency/partial occlusion • Borborygmi – “stomach grumble” normal in transient waves • Listen for friction rubs over the liver and spleen – Tumor/infection/infarction Objective: Percussion Percussion • Helps determine the amount and distribution of gas • Identifies masses (solid or fluid filled) • Liver/spleen boarders • Tympany + dullness – Check all 4 quadrants – Tympany = gas – Typanitic = intestinal obstruction • Dullness = fluid/feces – Can be related to a mass in the abdomen Objective: Palpation Palpation • Light palpation – Superficial, relaxes patient, identify areas of pain • Deep palpation – Can delineate abdominal masses • Peritoneal Inflammation – Have the patient cough, ask where it hurts, use one finger to touch – Rebound tenderness = peritoneal inflammation • “does it hurt more when I push down or let go?” • “did the pain get worse with the bumps in the road” • Be aware of referred pain Specialty Exams • Percussing to establish the liver boarders • Palpating the liver boarders – Hooking technique • • • • Percussing the spleen Palpating the spleen Palpating the kidneys CVA (costal vertebral angle) tenderness Referred Pain Acute GI Part 2 Jason Morgan RN, BS Roberts Wesleyan Inspection Surface/contour/movement • Scars – Describe (length/location/character) • Striae – Pink-purple = Cushings • Dilated veins – Cirrhosis or inferior vena cava obstruction • • Rashes/Lesions Contour – – – – – – – • Flat/rounded/protuberant ascites pregnancy hernia distended bladder AAA Mass Peristalsis – Observe for several minutes if you suspect obstruction – Increased waves with obstruction • Pulsations – Aortic aneurysm (AAA) Auscultation • Listen prior to percussion/palpation • Bowel sounds – one spot RLQ is usually sufficient – 5 to 34 per minute normal – Altered with diarrhea, intestinal obstruction, paralytic ileus, and peritonitis • Bruits – Suggest vascular occlusive disease – Listen over aorta, iliac arteries, femoral arteries – May be heard in systole normally, having a bruit in diastole is more indicative of arterial insufficiency/partial occlusion • Borborygmi – “stomach grumble” normal in transient waves • Listen for friction rubs over the liver and spleen – Tumor/infection/infarction Percussion • Helps determine the amount and distribution of gas • Identifies masses (solid or fluid filled) • Liver/spleen boarders • Tympany + dullness – Check all 4 quadrants – Tympany = gas – Typanitic = intestinal obstruction • Dullness = fluid/feces – Can be related to a mass in the abdomen Palpation • Light palpation – Superficial, relaxes patient, identify areas of pain • Deep palpation – Can delineate abdominal masses • Peritoneal Inflammation – Have the patient cough, ask where it hurts, use one finger to touch – Rebound tenderness = peritoneal inflammation • “does it hurt more when I push down or let go?” • “did the pain get worse with the bumps in the road” • Be aware of referred pain Nursing Process • Define this condition • What physical exam findings would you expect? • What subjective data/complaints would you expect? • What’s the plan for your patient? • What are your nursing diagnoses? • What would you teach your patient? Content Overview 1. 2. 3. 4. 5. 6. 7. 8. Appendicitis Intestinal Obstruction Esophageal varices Peptic ulcers Pancreatitis Upper/lower GIB Peritonitis/NG tubes Diverticulitis http://www.youtube.com/watch?v=9RFYqH4DnHU Acute Abdomen • • • • Severe pain Rigid, board-like on exam Muscle spasms r/t peritoneal irritation DX problem – Peritonitis – Bowel rupture – Bleeding • Testing • Aggressive pain management - OR Assessment findings of common disorders • Right lower quadrant (RLQ) – Appendicitis – Perforated duodenal ulcer • Cecal volvulus • Strangulated hernia – Left lower quadrant (LLQ) • Ulcerative colitis • Colonic diverticulitis – Right upper quadrant (RUQ) • • • • • Liver hepatitis Acute hepatic congestion Biliary stones, colic Acute cholecystitis Perforated peptic ulcer – Left upper quadrant (LUQ) • Splenic trauma • Pancreatitis • Pyloric obstruction Appendicitis Appendicitis • Assessment: – Severe sudden epigastric pain – Pain increases w/ movement, breathing – Pain may radiate to shoulder or back – Indigestion – Acute Abdomen – Psoas sign – Obturator sign • Vital signs? • Testing – Lab work (WBC) – X-ray (free air series) – CT scan – contrast • Treatment – Surgery (endoscopic) • Complications – Rupture – SBP • Nursing Care – – – – – PIV IVF NPO OR prep NG Intestinal Obstruction Intestinal Obstruction • Partial or complete obstruction in the small or large intestine • Impairs absorption – Electrolyte abnormalities • Cause – – – – – Hernia Adhesions Tumor Paralytic ileus Neuromuscular disease • Assessment – – – – Distended ABD N/V, constipation Pain Hyperactive bowel sounds or absent • Testing – – – – Labs X-ray CT scan U/S • Treatment – Can be conservative such as bowel rest – Surgical option • Nursing Care – IV/IVF/NPO/NG/Pain medications Obstruction SBO = copious vomiting/ hyperactive BS Large Intestine = uncommon emesis /decrease or absent BS Esophageal Varices Esophageal Varices • Risk – Liver disease • Portal hypertension – Portal system engorged • Rupture – High mortality – Vomiting bright red blood – Hemodynamic monitoring – Banding via endoscope • Treatment – – – – Gastric decompression Sclerotherapy Endoscopic band ligation Esophogogastric balloon tamponade – ETOH withdrawl – Transjugular intrahepatic portosystemic shunting (TIPS) Peptic Ulcer Peptic Ulcer • HPI – Severe sudden epigastric pain – Pain increases w/ movement, breathing – Pain may radiate to shoulder or back – Indigestion – Acute Abdomen • PMH? • Medications? • Objective Data – – – – – X rays - Free air series CT Endoscopy CBC Coagulation studies • PT/PTT • INR • Treatment – PPI/H2 blocker Gastric Surgery Gastric Surgery • Open vs. closed (laparoscopic) – Indication related to diagnosis – Maintain NPO status – ABX on-call to OR – Lab work • CBC • Chemistry panel • Coags • Type and screen – Pre-op EKG (cardiology clearance) • POST-OP considerations Complications ◦ Include typical post-op complications (bleeding, infection, pain, ileus) ◦ Dumping syndrome Rapid emptying into small intestine Water rushes into intestine causing nausea, diarrhea, sweating, palpitations, syncope May result in malnutrition, weight loss, inability to travel from home • With in 30 minutes of eating – – – – – Tachycardia Palpitations N-V Dizziness May be delayed up to 90 minutes after a meal. Abdominal Trauma • • • • • • • • Blunt force trauma Sheering injuries Rapid deceleration Penetrating wounds MVC and pregnancy Seat Belt sign Liver/spleen/kidney laceration Hemodynamic monitoring Pancreatitis Pancreatitis • Acute inflammation resulting in auto-digestion – Inflammation delays enzyme release which damages the organ • Gallstones and alcohol abuse account for 80 to 90% of cases • Assessment – Sudden onset of sharp, twisting, deep ,upper abdominal pain – Symptoms include anorexia, hypoactive bowel sounds, abdominal distention, as well as nausea and vomiting. • Management – – – – IVF Pain management NPO (block stimulation of enzymes) 3 days to 7 weeks for recovery • ERCP (endoscopic retrograde cholangiopancreatography) – Endoscopic approach to view structures such as the bile duct • Gallstones can be removed this way • MRCP – MRI to see biliary tree and pancreatic ducts GI Bleed Upper GI Bleed Causes ◦ Ulcers, varices, trauma, Mallory-Weiss tears, ingestion of foreign bodies ◦ Only 5% GIBs originate in small bowel Nursing considerations ◦ ◦ ◦ ◦ ◦ ◦ NPO Isotonic IVF, blood products Gastric and airway suction Left lateral (side) decubitus (lying) position Endoscopy within 24h Post endoscopy complications: Spasm, perforation Decreased BS, abd distension Mediastinis, fever Lower GI Bleed Causes – – – – – – – – Ulcerative colitis Diverticulitis Hemorrhoids Colon polyps Cancerous tumors Crohn's disease Trauma Foreign object insertion / ingestion Nursing considerations – NPO – Isotonic IVF, blood products – Guiaic stools until LGIB confirmed – Prep for colonoscopy • Oral prep • Enemas contraindicated – Post colonoscopy complications: • Perforation • Decreased BS, abd distension • Infection, fever Peritonitis Peritonitis • Inflammation of the peritoneum – – – – – – • • • • Usually related to bacterial exposure May be from an injury or trauma Appendicitis Perforated ulcer Diverticulitis Bowel perforation Remedy problem (above) Watch hemodynamics (shock?) IVF/ABX Improvement – – – – Decrease in temp/HR ABD softens (+) BM/flatus (+)BS Diverticulitis Diverticulitis • A diverticulum is a saclike herniation that extends through the muscle wall of the bowel • 95% are in the sigmoid colon • When food or bacteria are retained in the pouches inflammation occurs – – – – Perforation Abscess formation Peritonitis Obstruction • Typical DX occurs through colonoscopy • CT scans • X-ray (free-air series) • Labs – CBC – ESR • Treatment – PERC drain for abscess – Resection – Colectomy Review: Nasogastric and Nasointestinal tubes • Know why the tube is placed • Know how to check placement – What are the gold standards? – What have you been taught in clinical? • Know the common complications – – – – Nasal breakdown Low intermittent vs. continuous suction Aspiration Discomfort