* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File - rmhEDucation
Fundus photography wikipedia , lookup
Photoreceptor cell wikipedia , lookup
Corrective lens wikipedia , lookup
Contact lens wikipedia , lookup
Retinal waves wikipedia , lookup
Diabetic retinopathy wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Cataract surgery wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
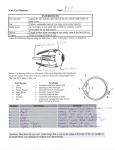
POINT OF CARE ULTRASOUND – OCULAR Aim To present common indications for ocular ultrasound (US) in the emergency department. Background Ocular US enables visualisation of the entire globe and optic nerve. It is especially useful in assessing the posterior segment when there is opacification of the anterior segment (eg dense cateract, hyphema). Or in the patient with significant eyelid swelling where visualisation of the posterior chamber is difficult. US should be used with caution in patients where pressure on the globe is contraindicated (eg penetrating trauma). Indications in the Emergency Department: 1. Trauma: - Pupillary response to light if too much eyelid swelling - Lens dislocation - Retinal detachment - Optic nerve sheath diameter for increased ICP 2. Visual disturbance - Retinal detachment - Posterior vitreous detachment - Vitreous haemorrhage - Optic nerve sheath diameter for increased ICP Anatomy of the eye Anatomy of the eye 1. Cornea 2. Iris 3. Ciliary body AC: anterior chamber PC: posterior chamber: posterior to iris 4. Vitreous 5. retina (yellow) choroid (orange) sclera (grey) ON: optic nerve Lens US image of the eye 1. cornea 2. Anterior chamber 3. Iris 4. lens 5. Vitreos 6. Retina, choroid, sclera 7. Optic nerve 9. Optic disc Technique Linear (vascular) probe Sterile gel Tegaderm over eyelid to stop conjunctival contamination with gel Longitudinal (saggital) and Transverse (axial) views Can also get pt to look to R, L and up and down to better define any pathology: annotate eye position on screen Longitudinal and Transvere Tips The anterior chamber and vitreous should appear black in the normal eye The lens always sits symmetrically behind the iris (usually has a thin hyperechoic posterior wall) Try to get an anatomical view of the globe (as above) and then angle the probe superiorly and inferiorly in transverse, and from nasal to temporal in longitudinal to image the entire globe Have the focus just beneath the area being examined (on the sonosite done by changing depth to keep the area being examined in the middle of the screen) Decrease gain to visualise the optic nerve Increase gain to visualise pathology in the posterior chamber Pathology Pupillary response Place the probe as anteriorly on the eye as possible with the patient looking down. Aim the probe caudally angling the probe until the iris is seen. Image from Wiswell J and Bellamkonda-Athmaram V. Sonographic Consensual Pupillary Reflex. West J Emerg Med. 2012 Dec; 13(6): 524 Shine a light in the contralateral eye and watch for constriction of the pupil. Lens The lens is lentiform shaped. It has a hyperechoic wall and a hypoechoic centre. The anterior wall is usually less well visualised. It lies summetrically behind the pupil. Lens dislocation The lens may be subluxed (still attached in some form to the ciliary body) or dislocated (not attached to the ciliary body). When dislocated, it will appear as a lentiform shape with a hyperechoic rim lying somewhere within the vitreous. A subluxed lens is usually anterior to the vitreous, but is no longer centred symmetrically behind the iris (see below). The patient should be imaged in different positions (eg sitting up, log roll) to ensure lens is attached. Axial view of the globe a. lens in normal position b subluxed lens Dislocated lens sitting in the vitreous image from http://sonodigest.blogspot.com.au/2015/07/posterior-dislocation-of-ocularlens.html Cateract Centre of the lens appears hyperechoic. Retina In the normal eye, the retina cannot be distinguished from the choroid/sclera on US. The retina is attached anteriorly at the ora serrata (curved arrow; see below) and posteriorly at the optic nerve. Retinal Detachment To be confident that the detachment is retina and not vitreous: try to get the optic nerve in the image so that retinal attachment points can be visualised. When detached, the retina is seen as a hyperechoic mobile line bulging into the vitreous with lucent areas superiorly and inferiorly. Anteriorly, the extent of detachment never extends beyond the ora serrata and posteriorly it is always attached to the optic nerve. Extent of retinal detachment Typical V shaped of complete retinal detachment. Image from http://www.slredultrasound.com/ImageoftheMonth.html Smaller retinal detachment. Note the posterior attachment at the optic nerve. Note: sometimes subretinal haemorrhage may cause small hyperechoic shadows inferior to the retina. Studies show that US for retinal detachment has a high level of accuracyi. Vitreous detachment Appears similar to a retinal detachment ie hyperechoic mobile line projecting into the vitreous. However, as there is no attachment to the optic nerve, the line may pass over the optic disc. Vitreous Haemorrhage Hyperechoic shadows are seen within the usually hypoechoic vitreous. Initially the shadows will be fine and only slightly hyperechoic. You may need to increase gain to better visualise the haemorrhage. With organisation into a haematoma, the shadows will become more linear and more hyperechoic. a: acute vitreous haemorrhage (note, fine hyperechoic shadows) b. chronic vitreous haemorrhage. Raised ICP Visualise the optic nerve in longitudinal and transverse. Measure the diameter 3mm posterior to the optic disc. Measure in two planes for accuracy. vertical measurement to 3mm, then measure width of optic nerve >5mm optic nerve sheath diameter is 100% sensitive to CT diagnosed raised ICP and 84% sensitive for intracranial pathology secondary to traumaii. From: Ohle R, McIsaac SM, Woo MY Sonography of the Optic Nerve Sheath Diameter for Detection of Raised Intracranial Pressure Compared to Computed Tomography. J Ultrasound Med 2015. 34 (34) 1285-1294. In conclusion Ocular US has various applications. Many of these conditions are easily detected on US and studies show high sensitivities and specificities. However, many conditions require a careful examination of all parts of the eye. The accuracy will decrease with poor technique. Unless otherwise stated, all images from private collection or from De La Hoz Polo M, Lluís AT, Segura OP et al Ocular ultrasonography focused on the posterior eye segment: what radiologists should know. Insights Imaging (2016) 7:351–364. i Vrablik ME, Snead GR, Minnigan HJ, et al The Diagnostic Accuracy of Bedside Ocular Ultrasonography for the Diagnosis of Retinal Detachment: A Systematic Review and Meta-analysis. Ann Emerg Med 2015; 65 (2): 199-203. ii Whitson MR and Mayo PH. Ultrasonography in the emergency department. Crit Care 2016: 227