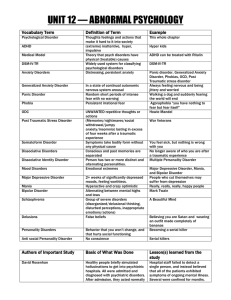
unit 12 — abnormal psychology
... Random short periods of intense fear with no warning Persistent irrational fear UNWANTED repetitive thoughts or actions (Memories/nightmares/social withdrawal/jumpy anxiety/insomnia) lasting in excess of four weeks after a traumatic experience Symptoms take bodily form without any physical cause Con ...
... Random short periods of intense fear with no warning Persistent irrational fear UNWANTED repetitive thoughts or actions (Memories/nightmares/social withdrawal/jumpy anxiety/insomnia) lasting in excess of four weeks after a traumatic experience Symptoms take bodily form without any physical cause Con ...
DSM Powerpoint - Incoming Student Resources
... outbursts that are grossly out of proportion in intensity or duration of the situation - Occur three more times each week for one year or more (on average) ...
... outbursts that are grossly out of proportion in intensity or duration of the situation - Occur three more times each week for one year or more (on average) ...
histrionic personality disorder
... Being easily influenced by other people. Being overly concerned with their looks. Needing to be the center of attention. Not think before acting. Quickly changing emotions, which may seem shallow to others. http://www.youtube.com/watch?v=p_1U2VpDZL8 ...
... Being easily influenced by other people. Being overly concerned with their looks. Needing to be the center of attention. Not think before acting. Quickly changing emotions, which may seem shallow to others. http://www.youtube.com/watch?v=p_1U2VpDZL8 ...
Vanessa Price Trauma Informed Responses in Specialty Courts
... The Psychotic Disorders • Schizophrenia – a chronic illness, but it can occur in episodes and have remissions. Usually overall functioning is lower than before onset of the illness. Marked by hallucinations, delusions, and/or thought disorder. • Schizoaffective disorder –Rather the person has episo ...
... The Psychotic Disorders • Schizophrenia – a chronic illness, but it can occur in episodes and have remissions. Usually overall functioning is lower than before onset of the illness. Marked by hallucinations, delusions, and/or thought disorder. • Schizoaffective disorder –Rather the person has episo ...
A condition in which people have an inflated sense
... Parents who teach that vulnerability is unacceptable may grow up not being able to feel empathy towards others. ...
... Parents who teach that vulnerability is unacceptable may grow up not being able to feel empathy towards others. ...
Bipolar Disorder - Boston Evening Therapy Associates
... individual to experience the severity of either depressive and or manic symptoms; and improve overall functioning and quality of life. Researchers are unclear as to the direct cause of this brain disorder, but note that the onset of the disorder begins between the ages of 18-25. Severe stress can o ...
... individual to experience the severity of either depressive and or manic symptoms; and improve overall functioning and quality of life. Researchers are unclear as to the direct cause of this brain disorder, but note that the onset of the disorder begins between the ages of 18-25. Severe stress can o ...
Abnormal Psychology
... episodes. • Manic episodes involve feelings of high energy (but they tend to differ a lot…some get confident and some get irritable). • Engage in risky behavior during the manic episode. ...
... episodes. • Manic episodes involve feelings of high energy (but they tend to differ a lot…some get confident and some get irritable). • Engage in risky behavior during the manic episode. ...
Psychobehavioral
... of 1.5-2.0 mEq/L. Dehydration, salt restriction, diuretic use, childbirth and infection predispose patients to these side effects. Which of the following is NOT one of these side effects? A. Diarrhea B. Vomiting C. Drowsiness D. muscular weakness E. lack of coordination ...
... of 1.5-2.0 mEq/L. Dehydration, salt restriction, diuretic use, childbirth and infection predispose patients to these side effects. Which of the following is NOT one of these side effects? A. Diarrhea B. Vomiting C. Drowsiness D. muscular weakness E. lack of coordination ...
PSYCHOSIS IN CHILDHOOD AND ADOLESCENCE
... MENTAL STATE ASSESSMENT N.B. Will often not volunteer psychotic symptoms. Thought Disorder “Trouble with thinking clearly” Hallucinations “Strange experiences recently, hearing voices when no one there, people talking about you” Delusions “unusual events recently monitored in any way, strang ...
... MENTAL STATE ASSESSMENT N.B. Will often not volunteer psychotic symptoms. Thought Disorder “Trouble with thinking clearly” Hallucinations “Strange experiences recently, hearing voices when no one there, people talking about you” Delusions “unusual events recently monitored in any way, strang ...
DSM-IV-TR in Action Powerpoint
... Anxiety and Obsessive-Compulsive Spectrum Disorders Will also include trichotillomania and possible other conditions Obsessions to be described as urges rather than impulses Term “impulses” is problematic as how do you distinguish them from impulse control disorders, so will change term ...
... Anxiety and Obsessive-Compulsive Spectrum Disorders Will also include trichotillomania and possible other conditions Obsessions to be described as urges rather than impulses Term “impulses” is problematic as how do you distinguish them from impulse control disorders, so will change term ...
Major Mental Illnesses
... inappropriately in social situations, and have trouble concentrating. Symptoms of psychosis are also present, and the person’s behaviour is markedly different from usual. ...
... inappropriately in social situations, and have trouble concentrating. Symptoms of psychosis are also present, and the person’s behaviour is markedly different from usual. ...
Document
... “A distinct period of abnormally and persistently elevated, expansive, or irritable mood, lasting at least one week (or for any duration if hospitalization is necessary)” (p.362). ...
... “A distinct period of abnormally and persistently elevated, expansive, or irritable mood, lasting at least one week (or for any duration if hospitalization is necessary)” (p.362). ...
AbnormalPsych - WordPress.com
... have experienced. This is normal; happens with medical students, too! Note, though, that all psychological disorders involve exaggerations of normal tendencies. If you can answer, “no” to the question, “Is this out of the norm for me?”, then you probably do not have a disorder! ...
... have experienced. This is normal; happens with medical students, too! Note, though, that all psychological disorders involve exaggerations of normal tendencies. If you can answer, “no” to the question, “Is this out of the norm for me?”, then you probably do not have a disorder! ...
Mental Disorders and Addictive Behavior
... real or imagined fears occur so often they prevent a person from enjoying life. • Phobias are an example. ...
... real or imagined fears occur so often they prevent a person from enjoying life. • Phobias are an example. ...
Bipolar Disorder
... Mood disturbance sufficiently severe to cause marked impairment in occupational functioning or in usual social activities or relations with others, or to necessitate hospitalization to prevent harm to self or others At no time during the disturbance have there been delusions or hallucinations for as ...
... Mood disturbance sufficiently severe to cause marked impairment in occupational functioning or in usual social activities or relations with others, or to necessitate hospitalization to prevent harm to self or others At no time during the disturbance have there been delusions or hallucinations for as ...
Mental Illness and Therapy - Agajanian-Psychology
... events experience the original event in forms of dreams and flashbacks. ...
... events experience the original event in forms of dreams and flashbacks. ...
Psychological Disorders
... 1. Dissociative disorders 2. Mood disorders 3. Schizophrenia 4. Anxiety Disorders DISSOCIATIVE DISORDERS ...
... 1. Dissociative disorders 2. Mood disorders 3. Schizophrenia 4. Anxiety Disorders DISSOCIATIVE DISORDERS ...
DSM-5 Condensed Training
... Purpose: Assist trained clinicians in Dx of Mental Dis’ as part of case formulation assessment that leads to a fully informed (cultural/social) Tx Plan for each individual. Manual makes NO recommendations for Tx or ForensicsCompentency/Criminal Resp./Disability Dx Criteria Sets: Summarize characteri ...
... Purpose: Assist trained clinicians in Dx of Mental Dis’ as part of case formulation assessment that leads to a fully informed (cultural/social) Tx Plan for each individual. Manual makes NO recommendations for Tx or ForensicsCompentency/Criminal Resp./Disability Dx Criteria Sets: Summarize characteri ...
Specific Learning Disorder - American Psychiatric Association
... symptoms, such as difficulty in reading, are just symptoms. And in many cases, one symptom points to a larger set of problems. These problems can have long-term impact on a person’s ability to function because so many activities of daily living require a mastery of number facts, written words, and w ...
... symptoms, such as difficulty in reading, are just symptoms. And in many cases, one symptom points to a larger set of problems. These problems can have long-term impact on a person’s ability to function because so many activities of daily living require a mastery of number facts, written words, and w ...
Bipolar Disorder
... Mood disturbance sufficiently severe to cause marked impairment in occupational functioning or in usual social activities or relations with others, or to necessitate hospitalization to prevent harm to self or others At no time during the disturbance have there been delusions or hallucinations for as ...
... Mood disturbance sufficiently severe to cause marked impairment in occupational functioning or in usual social activities or relations with others, or to necessitate hospitalization to prevent harm to self or others At no time during the disturbance have there been delusions or hallucinations for as ...
Schizoaffective disorder

Schizoaffective disorder (abbreviated as SZA or SAD) is a mental disorder characterized by abnormal thought processes and deregulated emotions. The diagnosis is made when the patient has features of both schizophrenia and a mood disorder—either bipolar disorder or depression—but does not strictly meet diagnostic criteria for either alone. The bipolar type is distinguished by symptoms of mania, hypomania, or mixed episode; the depressive type by symptoms of depression only. Common symptoms of the disorder include hallucinations, paranoid delusions, and disorganized speech and thinking. The onset of symptoms usually begins in young adulthood, currently with an uncertain lifetime prevalence because the disorder was redefined, but DSM-IV prevalence estimates were less than 1 percent of the population, in the range of 0.5 to 0.8 percent. Diagnosis is based on observed behavior and the patient's reported experiences.Genetics, neurobiology, early and current environment, behavioral, social, and experiential components appear to be important contributory factors; some recreational and prescription drugs may cause or worsen symptoms. No single isolated organic cause has been found, but extensive evidence exists for abnormalities in the metabolism of tetrahydrobiopterin (BH4), dopamine, and glutamic acid in people with schizophrenia, psychotic mood disorders, and schizoaffective disorder. People with schizoaffective disorder are likely to have co-occurring conditions, including anxiety disorders and substance use disorder. Social problems such as long-term unemployment, poverty and homelessness are common. The average life expectancy of people with the disorder is shorter than those without it, due to increased physical health problems from an absence of health promoting behaviors including a sedentary lifestyle, and a higher suicide rate.The mainstay of current treatment is antipsychotic medication combined with mood stabilizer medication or antidepressant medication, or both. There is growing concern by some researchers that antidepressants may increase psychosis, mania, and long-term mood episode cycling in the disorder. When there is risk to self or others, usually early in treatment, brief hospitalization may be necessary. Psychiatric rehabilitation, psychotherapy, and vocational rehabilitation are very important for recovery of higher psychosocial function. As a group, people with schizoaffective disorder diagnosed using DSM-IV and ICD-10 criteria have a better outcome than people with schizophrenia, but have variable individual psychosocial functional outcomes compared to people with mood disorders, from worse to the same. Outcomes for people with DSM-5 diagnosed schizoaffective disorder depend on data from prospective cohort studies, which haven't been completed yet.In DSM-5 and ICD-9 (which is being revised to ICD-10, to be published in 2015), schizoaffective disorder is in the same diagnostic class as schizophrenia, but not in the same class as mood disorders. The diagnosis was introduced in 1933, and its definition was slightly changed in the DSM-5, published in May 2013, because the DSM-IV schizoaffective disorder definition leads to excessive misdiagnosis. The changes made to the schizoaffective disorder definition were intended to make the DSM-5 diagnosis more consistent (or reliable), and to substantially reduce the use of the diagnosis. Additionally, the DSM-5 schizoaffective disorder diagnosis can no longer be used for first episode psychosis.























