* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download I. Neurons are the anatomical elements of neural systems
Neurotransmitter wikipedia , lookup
Node of Ranvier wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Process tracing wikipedia , lookup
Eyeblink conditioning wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Synaptic gating wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Optogenetics wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Neural engineering wikipedia , lookup
Neuroanatomy wikipedia , lookup
Development of the nervous system wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Circumventricular organs wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Synaptogenesis wikipedia , lookup
Axon guidance wikipedia , lookup
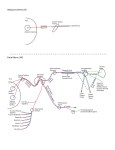
1 The Nerves of the Eye and Orbit Optic nerve (II) Oculomotor nerve (III) Trochlear (IV) Trigeminal (V) Abducens (VI) Facial (VII) I. Neurons are the anatomical elements of neural systems a. neuron= a single nerve cell, usually generates an action potential, but several nerve cells in the retina DO NOT, they produce graded potentials b. typically bipolar—receive input from one end and provide outputs at the other end c. dendrites= small branches of neuron that receive inputs d. axon= a single long process that provide the output e. cell body contains metabolism apparatus and protein synthesis f. action potential= brief change in the electrical polarity of the cell’s membrane that can be propagated from one end of the cell to the other without the amplitude being diminished II. Neural circuits consist of neurons linked mostly by unidirectional chemical synapses a. synapse= site of close approximation between two neurons, or between neuron and effector (cell to cell connections acting as communication sites) b. neurotransmitter= chemical released by a pre-synaptic swelling that interacts with chemical receptors on the dendrites of the second neuron c. presynaptic cell= cell that releases the neurotransmitter d. postsynaptic cell= cell on which the neurotransmitter acts e. the effect is to excite or inhibit the electrical activity in the target cell f. chemical synapses are unidirectional= info flows from the presynaptic to the postsynaptic cell, but not vice versa g. “recurrent connections” (common in retina) act as a feedback mechanism to presynaptic cell h. Gap Junctions – create bidirectional ion flow III. The direction of neural information flow distinguishes between sensory and motor nerves a. optic nerve fibers, as well as pain touch, cold and hot receptors of the eye and orbit conduct signals from the eye to the brain, but not vice versa (sensory nerves) b. information from the brain to the eye occurs by other sets of fibers (motor nerves) IV. Motor outputs are divided anatomically and functionally into somatic and autonomic systems VS 112 Ocular Anatomy Udpated 10/07 Page 1 of 12 2 The Nerves of the Eye and Orbit a. autonomic nervous system= output of this system is to smooth muscles and glands b. somatic (voluntary) nervous system= cell bodies of this system are contained within the brain and spinal cord and connect to striated muscle V. The autonomic nervous system is subdivided into the sympathetic and parasympathetic systems a. sympathetic NS (fibers enters eye by passing through the sympathetic root of ciliary ganglion, no synapsis present)= uses norepinepherine as a neurotransmitter (FIGHT or FLIGHT) b. parasympathetic NS= uses acetylcholine as a neurotransmitter, cell bodies of nerve close to target organ (ciliary & Meckal’s ganglia) c. the two systems of neurons often innervate the same targets, but usually with antagonistic effects VI. In the optic nerve, the location of axons from retinal ganglion cells corresponds to their location on the retina a. optic nerve= CRANIAL NERVE II, eye’s main sensory nerve b. contains about 1 million nerve fibers, all of which are axons of the ganglion cells that form the innermost cellular layer of the retina c. bundle of axons exits through the optic foramen as the optic nerve d. optic nerves from each eye join at the optic chiasm e. ganglion cells in the superior retina have axons in the superior half of the nerve f. axons in the inferior part of the nerve are form ganglion cells in the inferior retina g. Figure 5.3 , temporal retinal fiber begin segregated into superior and inferior bundles but coalesce at the chiasm, the foveal bundle of ganglion cell nerves are temporal as the exit the globe but centered at the chiasm VII. Axons from the two optic nerves are redistributed in the optic chiasm a. after the two optic nerves pass through their respective optic canals and exit the sphenoid bone, they merge as the optic chiasm, where optic nerves combine, from which the bilateral optic tracts arise b. axons from the nasal hemiretinas cross to the opposite side of the brain (the contralateral projection) c. temporal retinal axons remain on the side from which they originated (ipsilateral side) d. not all of the crossing axons take the most direct and shortest route from one side to the other i. some cross the midline and turn anteriorly and then loop back ii. other nasal axons remain on the ipsilateral side and then change direction to cross the midline at the back of the chiasm iii. between these extremes, are axons that run directly through the center of the chiasm iv. Figure 5.5 VS 112 Ocular Anatomy Udpated 10/07 Page 2 of 12 3 The Nerves of the Eye and Orbit e. the fovea is represented bilaterally in both optic tracts VIII. Spatial ordering of axons changes in the optic tracts a. retinotopic= the pattern of projection of axons such that neighboring areas on the retina remain neighbors in the target nuclei b. such an arrangement suggests that a small bundle of axons in a particular part of the tract will be from corresponding parts of the two retinas and therefore correspond to the same region of the visual field IX. In the lateral geniculate nuclei, which are primary targets in the optic tracts, inputs from the two eyes are separated into different layers a. lateral geniculate nuclei= Main output of retina, large six-layered nuclei in the midbrain to which most retinal ganglion cell project, main relay to cortex b. neurons here send axons to the primary visual cortex via the optic radiations c. layers 1,4, and 6 receive inputs from the contralateral eye d. layers 2,3, and 5 receive inputs from the ipsilateral eye e. left LGN receives axons from the left temporal retina and the right nasal retina (right half of the visual world) f. right LGN receives axons from the right temporal retina and the left nasal retina (left half of the visual world) X. Axons terminating in the lateral geniculate nuclei are spatially ordered a. ganglion cells that are neighbors in the retina will have their terminals as neighbors in the LGN b. destruction of a particular part of the LGN will always produce a scotoma (an area of relative or complete blindness) in the same part of the visual field c. the fovea and surrounding areas are over-represented spatially in the LGN (the large # of foveally derived axons is evenly spread across the LGN, and because XI. Some axons leave the optic tracts for other destinations a. some retinal ganglion cells do not contribute to the primary visual pathway and are not directly involved in visual perception b. some projections appear to have signals that convey info to secondary targets and are used for other purposes (i.e. reflex eye movements) c. Superior colliculus, olivary nuclei, accessory optic nuclei, supraoptic nucleas. XII. Lesions of the optic nerves and tracts produce defects in the visual fields a. Figure 5.12 b. any lesion between the chiasm and the eye will affect the visual field of only one eye VS 112 Ocular Anatomy Udpated 10/07 Page 3 of 12 4 The Nerves of the Eye and Orbit c. lesions of the chiasm or the optic tracts will affect both monocular fields d. if one optic tract were completely severed, the scotomas would be hemianopias, in which half of each monocular field is blind XIII. Lesions in the secondary visual pathways can be observed only as motor deficits a. it is possible to interrupt the primary visual pathway, so as to produce complete while certain visual behaviors, such as the pupillary light reflexes, remain intact and normal b. brain lesions that involve one or more of the subsidiary pathways without affecting the primary visual pathway will not produce visual field defects The Trigeminal Nerve: Signals for Touch and Pain A. Two of the three trigeminal divisions carry signals from the eye and surrounding tissues. a. Trigeminal Nerve (Cranial Nerve V) differs from other cranial nerves because it collects the cell bodies of its neurons in a large ganglion, the gasserian (semilunar) ganglion, outside the brainstem b. Connected to the brainstem via the sensory and motor roots i. Ophthalmic division (V1): Has three major branches 1. Nasociliary nerve: Only one of the three to innervate the eye 2. Frontal nerve: Has two dependent branches-the supratrochlear and supraorbital nerves both of which go to the skin of the brow and forehead 3. Lacrimal nerve-has only a single branch which is the route used by parasympathetic fibers going to the lacrimal gland via the lacrimal nerve ii. Maxillary division (V2): Extend to the teeth and gums in the upper jaw, the lips and facial skin, and the mucosa of the maxillary sinus 1. Zygomatic nerve: the major branch that enters the orbit and runs beneath the orbit floor to innervate the skin of the lower eyelid and face 2. Zygomatio-facial and zygomatico-temporal nerves are small branches that exit the orbit through small foramina in the zygomatic bone to the skin of the cheek iii. Mandibular division (V3): Has numerous branches that innervates the teeth, gums, and skin of the lower jaw B. All somatosensory information from the eye is conveyed by the nasociliary nerve to the ophthalmic division of the trigeminal a. Two long ciliary nerves exit the posterior sclera on either side of the optic nerve, and they run medially to join the nasociliary nerve. b. Several short ciliary nerves exit the sclera all around the optic nerve. They are mixed nerves containing sensory, sympathetic, and parasympathetic VS 112 Ocular Anatomy Udpated 10/07 Page 4 of 12 The Nerves of the Eye and Orbit C. D. E. F. G. H. I. 5 fibers and they all run from the eye to the ciliary ganglion that lies on the lateral side of the optic nerve Sensory nerve fibers from the cornea, conjunctiva, limbus, and anterior sclera join to form the long ciliary nerves. a. In the general classification of sensory receptors they are nociceptors, activated by noxious or potentially noxious stimuli including mechanical pressure, which is perceived as pain, and substances that are released by damaged cells or inflammatory reactions. b. The majority of nerve endings are in the cornea where they end in the epithelium c. Nerve fibers from the cornea, iris, limbus, and ciliary body join on either side of the eye to run within the choroids as two long ciliary nerves. They exit the sclera on either side of the optic nerve, running back and medially to join the nasociliary nerve. d. Majority of fibers in the long ciliary nerves are from the cornea Stimulation of corneal or conjunctival nerve endings elicits sensations of touch or pain, a blink reflex, and reflex lacrimation Other sensory fibers from the eye are conveyed by the short ciliary nerves and the sensory root of the ciliary ganglion a. The sensory fibers in the short ciliary nerves run directly through the ganglion without synapsing and they exit as a single fiber bundle called the sensory root Most other branches of the ophthalmic nerve carry somatosensory fibers from the skin of the eyelids and face a. The merging of the anterior ethmoidal and infratrochlear nerves form the nasociliary nerve b. The anterior ethmoidal nerve innervates the nasal mucosa and skin at the tip of the nose c. The posterior ethmoidal nerve innervates the nasal mucosa and joins the nasociliary just after it enters the orbit d. Supratrochlear and supraorbital nerves, two branches of the frontal nerve that innervates the upper eyelid and forehead A few branches of the maxillary nerve pass through the orbit from the facial skin and maxillary sinus a. Zygomatico-temporal and zygomatico-facial join the zygomatic nerve from the skin overlying the cheek bone b. Pterygopalatine ganglion (sphenopalatine, or Meckel’s) carry parasympathetic fibers for the lacrimal gland Lesions in the branching hierarchy of the ophthalmic nerve produce anesthesia that helps identify the lesion site a. Retrobulbar block: an injection of anesthetic behind the eye Viral infection of the trigeminal system can produce severe corneal damage Extraocular Motor Nerves VS 112 Ocular Anatomy Udpated 10/07 Page 5 of 12 The Nerves of the Eye and Orbit 6 A. The three cranial nerves that innervate the six extraocular muscles contain axons from clusters of cells in the brainstem that arise from the nuclei of motor neurons. Their cell bodies have extensive dendritic processes a. Oculomotor (III) to the superior rectus, medial rectus, inferior rectus, and inferior oblique; also the levator muscle b. Trochlear (IV) to the superior oblique c. Abducens (VI) to the lateral rectus B. Most of the cells in the oculomotor nuclei send their axons into the ipsilateral oculomotor nerve and to the muscles on the ipsilateral side. EXCEPTION: the superior recti---the axons cross the midline between the two oculomotor nuclei to pass through the contralateral nucleus and enter the contralateral oculomotor nerve. (ie: RIGHT superior rectus innervated by axons originating in the LEFT oculomotor nucleas and vice versa) C. Severing ONE oculomotor nerve will still affect only the muscles on the ipsilateral eye D. Axons destined for different muscles run together in the oculomotor nerve until it exits the cavernous sinus just behind the orbit a. The superior branch of the oculomotor nerve innervates the levator and superior rectus b. The inferior branch innervates the medial and inferior recti and inferior oblique E. The oculomotor nerve contains parasympathetic fibers bound for the ciliary ganglion a. Motor root (of the ciliary ganglion): a small bundle of axons leaves the inferior oculomotor branch going to the inferior oblique and runs upward to the ciliary ganglion b. Edinger-Westphal nucleus: Lies in the brainstem near the ipsilateral oculomotor nucleus. Nerve fibers from these nuclei join the oculomotor nerve before they exit the brain stem F. Cells in the trochlear nerve (CN IV) nucleus a. innervate the contralateral superior oblique (only extraocular muscle with contralateral innervation along with superior rectus muscle b. the smallest and longest nerves going to the extraocular muscles making them vulnerable to trauma G. Abducens nerve cells (CN VI) a. innervate a single muscle ipsilateral lateral rectus b. lesions along the abducens nerve are confined to lateral rectus mainly c. most lateral of the extraocular nerves and is subject to damage associated with trauma to the side of the head H. Cavernous sinus- a large venous sinus alongside the sphenoid bone a. All of the oculomotor nerves pass through the cavernous sinus on their way to the orbit b. Carotid arteries pass through the cavernous sinuses c. The optic nerve does NOT pass through the cavernous sinuses VS 112 Ocular Anatomy Udpated 10/07 Page 6 of 12 7 The Nerves of the Eye and Orbit I. The extraocular motor nerves probably contain sensory axons from muscle spindles and tendon organs as well as motor axons Innervation of the Muscles of the Eyelids A. Three sets of muscles are associated with the eyelids B. The orbicularis oculi (striated muscle) is innervated by the facial nerve (VII) a. Contraction causes narrowing of the palpebral fissure to close eye b. Supplied by 2 branches of the facial nerve: upper and lower zygomatic branches of the facial nerve c. Lesions that irritate the facial nerve and produce unusual levels of activity in the nerve fibers going to the orbicularis muscle can produce blepharospasm d. Ectropian: may result do to failed transmission to orbicularis and muscle paralysis leading to this eversion of the lower lids C. Levator is innervated by the oculomotor (III) nerve D. The superior and inferior tarsal muscles are made of smooth muscle and are innervated by the sympathetic system E. Ptosis may result from either oculomotor or sympathetic lesions a. Normally the upper lid is held in position by the tonus in the levator and superior tarsal muscles. b. Lesion to CN III (oculomotor nerve) can affect innervation of levator or a sympathetic lesion affecting the superior tarsal muscle can result in ptosis (drooping upper lid) I. Autonomic Innervation of the Smooth Muscle within the Eye A. Sympathetic nerve pathway to the eye i. Most sympathetic fibers originate in superior cervical ganglion located in the upper part of the neck below the skull ii. Fibers run upward as the internal carotid nerves along with internal carotid arteries and begin branching at the carotid plexus (sympathetic plexus) iii. One of the bungles of sympathetic fibers becomes the sympathetic root of the ciliary ganglion which runs along the ophthalmic artery and enters the orbit at the optic foramen iv. The fibers run along the optic nerve and pass through the ciliary ganglion, but do not make synaptic connections with the ganglion v. While passing through, the bundle branches and enters the short ciliary nerves vi. The short ciliary nerves pass through the sclera to the choroid and branch to their target structures B. Dilator muscle of the iris has sympathetic innervation i. Drugs mimicking sympathetic neurotransmitters (a common sympathetic neurotransmitter that is mimicked is norepinephrine) produce mydriasis (pupil dilation) NOT miosis (pupil constriction) ii. Dilation is the result of the contraction of the dilator muscle VS 112 Ocular Anatomy Udpated 10/07 Page 7 of 12 The Nerves of the Eye and Orbit II. 8 C. Sympathetic innervation of arterioles in the uveal tract produce vasoconstriction i. Most of the arterioles in the uveal tract (iris, choroid, and ciliary body) appear to receive innervation from sympathetic innervation ii. Allows choroidal blood flow to remain constant while arterial pressure increases iii. Under normal circumstances (when arterial and venous pressures on either side of the vascular bed are constant) the blood flow will be INVERSELY proportional to the resistance in the vascular bed 1. Ex: increase resistance = decreased flow (in choroid activation of sympathetic system reduces blood flow) D. Horner’s Syndrome i. results from an isolated lesion in the sympathetic pathway that could be far from the eye ii. Symptoms include: ptosis, miosis, and anhidrosis (lack of sweating) to the face and neck of the affected side iii. Other possible signs: decreased IOP, vasodilation of conjunctival blood vessels, and enophthamos (sinking of the eye into the orbit) E. Parasympathetic nerve pathway to the eye i. Preganglionic fibers originating in the Edinger-Westphal nucleus travel along the oculomotor nerve and motor root of the ciliary ganglion before reaching the ciliary ganglion, while postganglionic fibers originate in cell bodies of the ciliary ganglion and enter the eye by the short ciliary nerves 1. These fibers innervate the sphincter and ciliary muscles ii. Rami oculares are postganglionic fibers the orginate in the pterygopalatine ganglion and enter the orbit through the superior orbital fissure 1. They partially innervate the choroidal vasculature F. Pupil constriction is controlled by the parasympathetic system i. Retinal ganglion cells monitor the amount of light entering the eye and transmit information to the olivary pretectal nucleus (there are 2 olivary pretectal nuclei, 1 for each eye) ii. Olivary pretectal nucleus sends signals to both Edinger-Westphal nuclei iii. Edinger-Westphal nuclei innervate the sphincter muscle 1. Pupil constriction in the eye receiving light stimulus is direct reflex, constriction in other eye is consensual reflex G. Argyll Robertson pupil is characterized by partially constricted pupils (or pupil) without direct or consensual reflexes, but miosis with accommodation is present i. Lesion site is most likely between the olivary pretectal nuclei and Edinger-Westphal nuclei ii. Present in neurosyphili Innervation of the Lacrimal Gland VS 112 Ocular Anatomy Udpated 10/07 Page 8 of 12 The Nerves of the Eye and Orbit III. 9 A. Postganglionic parasympathetic fibers to the lacrimal gland originate from the pterygopalatine ganglion i. Pathway 1. pterygopalatine ganglion 2. zygomatic nerve 3. zygomatico-temporal nerve 4. communicating branch 5. lacrimal nerve ii. Axons terminate around secretory cells of lacrimal gland B. Sympathetic inputs are also present in the lacrimal gland, but pathway is unclear C. Preganglionic parasympathetic fibers to the pterygopalatine ganglion originate in a portion of the facial nerve nucleus i. Provides connection between innervation of the cornea and conjunctiva and lacrimal gland D. Lacrimal gland stimulation is associated with pain, emotional distress, and very intense light stimuli E. Lacrimal gland is also influenced by hormones F. Afferent or efferent pathway lesions prevent reflex weeping, but efferent pathway lesion also prevents tonic lacrimal gland stimulation thereby affecting basal tear production i. Efferent lesions could contribute to dry eye syndrome Issues in Neural development A. Specialized growth cones guide the extension of axons and dendrites i. Growth cones – specialized regions of developing neural processes that contain filipodia the crawl to a region where it will receive synaptic inputs or to the target cells to which it will be presynaptic B. Pathfinding by growth cones depends on recognition of local directions signs i. Neuroglial cells – supporting cells found throughout the nervous system that act as adhesives to guide growth cones on particular paths C. Target recognition and acquisition may require specific markers produced by the target cells i. Tropic factors guide developing neurons to their final position; the final position is dependent upon the timing that the tropic factors are being produced D. Many early neurons are eliminated as mature patterns of connectivity are established E. Adult connectivity patterns are not always complete at birth, and postnatal development is subject to modification i. Critical periods – times in which the nervous system can be extensively modified 1. Pathfinding is completed early in life VS 112 Ocular Anatomy Udpated 10/07 Page 9 of 12 The Nerves of the Eye and Orbit 10 2. Synapse establishment and maintenance persists for considerably longer, and could persists, on some level, throughout life F. Ocular albinism is associated with a pathfinding error in the development of optic nerve axons G. Anomalous innervation of the extraocular muscles may be the result of pathfinding or target recognition errors H. Some forms of amblyopia may be related to problems with postnatal establishment and maintenance of synaptic connections i. Amblyopia – reduced visual acuity that is not accounted for by refractive error or pathology I. Innervation of the extraocular muscles begins early in gestation sensory innervation much later IV. Postnatal Neuron Growth and Regeneration A. Most postnatal neuron growth is interstitial growth i. Interstial growth – neuron growth that occurs when growth cones disappear and lengthening is no longer needed, neurons get larger and a new cell membrane is formed B. Neurons do not undergo mitosis postnatally i. We are born with all neurons that our body will ever form C. Spinal neurons in peripheral nerves can regenerate after being damaged D. Central nervous system neurons do not regenerate following major damage E. Corneal nerve endings will regenerate following local damage i. Damaged corneal nerve fibers initially degenerate, but eventually regenerate to innervated damaged area; also, fibers from undamaged regions provide innervation to damaged area ii. Nerve endings in cornea can regenerate because only a small, uncomplicated area of the pathway is damaged F. Neuronal degeneration can affect other, undamaged neurons i. Transneuronal atrophy – degeneration of nerve tissue that arises because the nerve from which the tissue received signals is no longer functional G. Parasympathetic nerve pathway to the eye originate in the ciliary or the pterygopalatine ganglion (Fig. 5.26) i. Pre-ganglionic fibers originating in the Edinger-Westphal nucleus travel along the oculomotor nerve and motor root of the ciliary ganglion before reaching the ciliary ganglion. ii. Post-ganglionic fibers originate in the cell bodies of the ciliary ganglion and enter the eye by the short ciliary nerves. 1. These fibers innervate the sphincter and ciliary muscle iii. Rami oculares are post-ganglionic parasympathetic fibers also that originate in the pterygopalatine ganglion. 1. From the facial nerve synapse, the fibers pass through the superior orbital fissure, form a plexus around VS 112 Ocular Anatomy Udpated 10/07 Page 10 of 12 The Nerves of the Eye and Orbit 11 the carotid artery, bypass the ciliary ganglion, and innervate the choroid. H. Pupil constriction is controlled by the parasympathetic innervation of the sphincter (Fig 5.28) i. Retinal ganglion cells monitor the amount of light entering the eye then leave the optic tract and run to the pretectal nucleus cells (there are 2 PNCs one for each eye). ii. Olivary pretectal nucleus sends signals to both EdingerWestphal nuclei that accounts for the direct and consensual reflex. (the path for OPN to the contralateral Edinger-Westphal nucleus passes through the posterior commissure. iii. Edinger-Westphal nuclei innervate the sphincter muscle and cause pupillary light reflexes. I. Argyll Robertson pupil i. Characterized by constricted pupils with no direct or consensual reflex. ii. Caused by lesions between the olivary pretectal nuclei and Edinger-Westphal nuclei. iii. Retention of miosis occurs despite loss of pupil reflex iii. Found many times in syphilis patients (Whore's pupilaccommodation but no reflex) Innervation of Lacrimal Gland (Fig 5.27 and 29) A. Postganglionic parasympathetic fibers in the lacrimal gland originate from the pterygopalatine ganglion (same area as Rami oculares) i. Pathway: Leave pterygopalatine ganglion and join the maxillary nerve briefly before branching off to the zygomatico-temporal branch. The fibers then leave via the communicating branch to join the lacrimal gland. ii. Parasympathetic axons terminate around the secretory cells of the glands. iii. Sympathetic inputs are unclear B. Preganglionic parasympathetic fibers to the pterygopalatine ganglion originate in a portion of the facial nerve nucleus i. Provides connection between innervation of the cornea and conjunctiva and lacrimal gland C. Other inputs on the parasympathetic pathway can lead to lacrimal gland stimulation and tear production. i. Inputs can be pain, emotional distress, and very intense light. D. Lacrimal gland can also be stimulated by local and nonlocal hormones. E. Lesions in the afferent and efferent pathway can prevent reflex weeping i. Efferent lesions are more serious because they eliminate all tonic innervation of lacrimal gland ii. A possible causative agent for dry eye VS 112 Ocular Anatomy Udpated 10/07 Page 11 of 12 12 The Nerves of the Eye and Orbit I. Neural Development A. Once neurons differentiate, they grow processes that become axons and dentrites. Growth originates at the cell body. i. Growth cones- specialized region that contain filipodia that allow developing processes to crawl to specific regions. ii. Dentrites find the region where it will receive synaptic input and axons find the presynaptic region of target cells. B. Pathfinding of growth cones has several factors. Laminin on the surface of neuroglial cells act as stepping stones that guide the growth cones along particular paths. b) The first neurons to reach their destinations act as “pioneer” cells that make it easier for later neurons to reach their destinations. a) a) b) c) C. Growing neurons must recognize when they have reached their targets. Tropic factors are specific markers produced by target cells. Axons grow towards these markers. Tropic factors are produced at different times. This is how one neuron can innervate several cells. D. Many more neurons are produced than are needed. a) Fine tuning the pattern of connectivity requires the elimination of neurons with poor connections to target cells. b) This establishes mature patterns of neuron connective E. Adult connectivity patterns are not always complete at birth. Critical periods are times when neurons are susceptible to modification. a) Critical period for pathfinding happens early and ends when the target is acquired. b) Critical period for synapse establishment and maintenance is much longer. Some capacity for synapse modification may persist throughout life. F. Developmental abnormalities that involve errors in pathfinding, target recongnition, and synapse establishment, can interfere with normal neuron interactions. a) Ocular albinism is associated with errors in pathfinding in the development of the optic nerve axons. This misrouting occurs at the chiasm. b) Recognition errors can cause inaccurate innervation of the extraocular muscles that result in improper function of those muscles. c) Amblyopia that is not accounted for by refractive error or pathology is associated with postnatal synaptic establishment and maintenance anomalies. II. Post natal Neuron Growth and Regeneration A. Once target is reached by developing neurons, the growth cones disappear and subsequent increase in size is by interstitial growth. b. Peripheral nerves retain a capacity for interstitial growth for many years. c. Growth in central neurons does not last as long. Brain reaches adult size earlier than the rest of the body B. Neurons do not undergo mitosis postnatally. We are born with all the neurons that are body will ever have. This is why there is an overproduction of them in the embryo. C. Because neurons are unable to reproduce, ability to regenerate depends on where the damage is. a) Spinal neurons in peripheral nerves can regenerate after damage. Axons can grow to reach the target structure again, but the innervation is never as good as the original. b) Central neurons do not regenerate at all after damage. Intricate pathways and need for precision may prevent it. c) Corneal nerve ending will regenerate if damage is confined. Fibers from undamaged regions provide innervation to damaged area. Regeneration is possible because only a small, uncomplicated pathway area is damaged. Neuronal degeneration after damage can affect other neurons causing transneuronal atrophy. Neurons that used to receive signals from the damaged nerve, will no longer function and will degenerate too. VS 112 Ocular Anatomy Udpated 10/07 Page 12 of 12