* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download older adults
Survey
Document related concepts
Schizoaffective disorder wikipedia , lookup
Alzheimer's disease wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Lifetrack Therapy wikipedia , lookup
Mental disorder wikipedia , lookup
Abnormal psychology wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Biology of depression wikipedia , lookup
Externalizing disorders wikipedia , lookup
Major depressive disorder wikipedia , lookup
Memory disorder wikipedia , lookup
Transcript
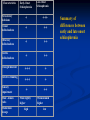
Geriatric Psychiatry: An Introductory Overview Carl I. Cohen M.D. Distinguished Service Professor & Director Division of Geriatric Psychiatry email: [email protected] Case of Ms Jones Ms Jones is a 76-year-old African American woman who presents with a history of not seeing her friends, loss of interest in sewing and gardening, and some forgetfulness. She has some difficulty hearing and also complains of arthritic pain. She has hypertension, hyperlipidemia, and type 2 diabetes. She takes medications for these conditions. Several of her friends died in recent years, and her daughter has moved to New Jersey. She has always been a very independent woman, but now feels more helpless. On examination she is found to memory deficits and mild difficulties in executive functioning. She meets 3 of 9 DSM IVTR depression criteria. Laboratory tests and physical examination are within normal limits, except for a BP of 155/95 and elevated cholesterol. She was initially treated for depression with medication and psychotherapy. She showed some improvements in mood and cognitive functioning initially. However, she never completely remitted, and three years later she showed evidence of early dementia, with impairments in cognition and daily functioning. Principles of Geriatric Psychiatry 1. Older adults are the most heterogeneous group in the population. 2. The demographics of aging are shifting. 3. Assessment is different in older age. 4. Disorders may present differently. 5. Treatment may be different. 6. The course of disorders may be different. 7. Aging is characterized by both longstanding conditions and late-onset conditions that may become chronic. 8. Nearly all older adults with psychiatric disorders will have comorbid conditions, although not all comorbity is alike. 9. There is continuity in personality. 10. Psychiatric illness must be understood within a social and biological context. 11. The prevalence of psychiatric disorders in older adults and mental disorders are best viewed on a continuum. 12. It is essential to view the treatment goals for older adults with mental illness in the context of a life course trajectory. 13. Disorders overlap with respect to neuropathology and symptoms. 14. Mental illness in older age is complex. Question 1 Older adults are extremely heterogeneous and have little in common with each other? Answer: False 1. Older adults are the most heterogeneous group in the population. Older persons differ dramatically in their physical and mental health, functional abilities, social networks, political and religious beliefs, and so forth. Although we often categorize aged persons based on chronological age –e.g., the census bureau defines “older adults” as aged 55 to 64, and elderly as 65 and over—there are marked differences in biological aging. This is especially true among persons with chronic schizophrenia who may have health problems more characteristic of persons who are 10 or 15 years older. Although older adults are heterogeneous they do share some common life experiences that may have psychosocial ramifications (so called “cohort effects”). However, with the increasing number of older persons reaching very old age, the number of cohorts within the aging population has grown. Persons born before 1930 came of age during the Great Depression and World War II, whereas those born after the war came of age during more prosperous times and included the cultural and social turmoil of the 1960s. The oldest African Americans grew up during periods of marked racial segregation and discrimination, whereas “young-old” African Americans came of age during the period of the civil rights and black power movements Clinical Implications Mental and physical health care to older adults should not be determined solely by chronological age because of the marked diversity within this age group. However, living through similar historical periods can provide a common background context for older adults of the same age. Question 2: The 1 percent Which group is part of the 1%: The percentage of persons aged 90 and over or persons in gangs? Answer: Persons aged 90+; however, persons in gangs (currently 1%) are one of the fastest growing segments of society (40% in past 3 years) 2. The demographics of aging are shifting. The baby boomers (people born between 1946 to 1964) will first turn 65 beginning 2011. The older population is projected to nearly double from 38 million (12.6 %) in 2008 to 72 million (20%) in 2030. Persons over aged 85 and over are the most rapidly growing segment of our population and their numbers will double over the first quarter of the century and more than quadruple over the first half the century (to over 19 million persons). The older population is also growing more diverse. In 2000, 16% of population were nonwhites (Blacks, Hispanics, Asians, Native Americans) or 5.8 million persons. In 2050, 36% of population will be non- white or 29.5 million persons. Thus, there will be a 5-fold increase in the number of minority elders over the first half of the 21st century. Clinical Implications Mental health providers can expect to be working with increasingly older and more diverse populations They must possess appropriate clinical skills and cultural knowledge if they are to deliver competent care. Question 3 Emergency rooms are an ideal place to examine older adults? Answer: False 3. Assessment is different in older age The assessment of older adults must take into account communication difficulties in vision and hearing, physical handicaps, and cognitive difficulties. Clinical Implications Clinicians should generally assess cognitive and physical dysfunction on the initial examination Continue to closely monitor for the effects of treatment on the patient’s mental & physical functioning. Another key difference from younger persons is the likelihood that caregivers, both formal and informal, will be more involved in providing information and treatment. Question 4 Depressive symptoms in later life are similar to those in younger persons False 4. Disorders may present differently Like physical disorders, the clinical presentations of psychiatric disorders may differ in older persons. Examples: Depression may present with fewer signs of sadness and with more symptoms of social withdrawal, somatic concerns, motor disturbances, and apathy. Sometimes described as:“Depression without sadness” or a “depletion syndrome” manifested by withdrawal, apathy, and lack of vigor. Also may see more executive dysfunction, which may be due to vascular depression (see figure re: vascular depression). Major Depression Similar across lifespan but there may be some differences. Among older adults: •Psychomotor disturbances more prominent (either agitation or retardation), •Higher levels of melancholia(symptoms of noninteractiveness, psychological motor retardation or agitation, weight loss) •Tendency to talk more about bodily symptoms •Loss of interest is more common •Social withdrawal is more common •Irritability is more common •Somatization (emotional issues expressed through bodily complaints)is more common Vascular depression (depression due to vascular lesions): more common in late-onset disease. Evidence that cerebrovascular disease seemingly plays a role in depression beginning in late life. Vascular lesions include periventricular hyperintensity, deep matter hyperintensity, and subcortical gray matter hyperintensity. Disruption of prefrontal systems may be responsible. Symptoms include greater levels of apathy, psychomotor retardation and disability, and less agitation,psychoses, family history of psychiatric illness, guilt, and insight versus other older depressed persons. Vascular Depression Hypothesis (Krishnan & McDonald, 1995;Sneed & Cuslng-Reimlieb, 2011) Risk Factors •Age •Hypertension •Hyperlipidemia •Smoking •Diabetes Artherosclerosis Deep white matter lesions ( vulnerability to late onset depression) Negative life events Poor social support Vascular depression with executive dysfunction Disorders may present differently (cont.) Late-onset schizophrenia—onset after age 40 or 45(about 15-20% of all schizophrenia)--tends to occur disproportionately more in women, to have more persecutory delusions, fewer negative symptoms, and formal thought disorders (see chart comparing early and late disorders) Characteristics Early-Onset Schizophrenia Late-Onset Schizophrenia Persecutory delusions + +++ Visual hallucinations + ++ Olfactory hallucinations + ++ Tactile hallucinations + ++ Thought disorder +++ + Affective blunting +++ + + ++ Sensory impairment Male –female ratio Medication dosage Male slightly higher high Women much higher low Summary of differences between early and late onset schizophrenia Clinical Implications Clinicians must be vigilant for more atypical symptoms in older adults. Question 5 All drug metabolism is appreciably affected by aging False 5. Treatment may be different With increased age: There are declines in the absorption rate of medications, although amount of medication absorbed does not change Distribution of drugs as a result of an increase in adipose tissue relative to lean body mass Diminished metabolism in the liver Declines in renal clearance Clinical Implications Dosages of medications may need to be lower than in younger persons, and considerations of side effects and drug interactions become more relevant. Must be cautious in prescribing drugs that are apt to affect the Cytochrome P450 metabolic pathways in the liver (Phase I hepatic metabolism), and if used, their potential interactions with other medications should be reviewed. Some pathways such as CYP1A2 and CYP3A4 are most affected by aging. It is best to use drugs that do not undergo Phase I hepatic metabolism, but only Phase II hepatic metabolism (conjugation), since this process is not affected by aging. Because of changes in the distribution of drugs in the body, the fat soluble drugs, which includes many of the drugs used in psychiatry, tend to remain in the body longer and may cause toxicity. Conversely, water soluble drugs such as lithium need to be used cautiously because of the diminution of total body water with age. Finally, some psychotropic drugs remain active (e.g. lithium, gabapentin, rivastigmine) until they are cleared by the kidney, and doses may need to be adjusted in older adults. Question 6 Prognosis for depression in later life is no worse than younger persons False 6. The course of disorders may be different In schizophrenia There is a diminution in positive symptoms with age. Levels of co-occurring depression may remain the same or increase. Mild cognitive problems that present earlier in life may worsen due to normal effects of the aging process.Thus, older persons may be at the level of a mild dementia. In depression: More subtypes (e.g. vascular depression; and depression with cognitive deficits/dementia also known as “pseudomentia”) that may be more resistant to treatment. There is some evidence that older persons with major depression may be more prone to relapse and relapse sooner than their younger counterparts. Clinical Implications In treating persons with schizophrenia need to be aware of changes in symptoms that occur with aging, and to adjust treatment accordingly. In treating older adults with depression, it is important to determine the subtype of depression, because prognosis varies considerably depending on the etiology of the depression. 7. Aging is characterized by both longstanding conditions and late-onset conditions that may become chronic. Depression in older adults is often chronic, and more than half of persons with clinical depression in later life remain syndromally depressed and an additional 30% have some residual symptoms (subsyndromal or subthreshold depression). Even under the most ideal treatment conditions (e.g., medication and psychotherapy), about onethird of older persons with new –onset depression relapse on 2-year follow-up (Reynolds et al, 2006). Two-thirds relapse without medications. The line between reversible and irreversible illness may become less distinct. Examples: Late-onset depression may be a prodromal symptom of dementia. It is estimated that twofifths of late-onset depression with some cognitive problems (so called “pseudodementia”) may eventually progress to a true dementia, despite there having been an initial resolution of depression. Persons with vascular depression are more prone to dementia. Clinical Implications Although treatment can help reduce recurrence and levels of symptoms, the complex interaction of psychiatric and physical conditions may make full recovery less likely. Treatment of late-onset depression may benefit (i.e., reduced likelihood of dementia) from a combination of an SSRI and cholinesterase inhibitor such as donepezil (Aricept), although depression recurrence may be higher. While the ultimate goal for all patients may be the remission of symptoms, sometimes treatment goals will have to be adjusted, and like some chronic physical disorders, persons may have to live with a modest level of symptoms. Question 7 Comorbid illnesses are important determinants of outcome in older adults True 8. Nearly all older adults with psychiatric disorders will have comorbid conditions, although not all comorbity is alike Some comorbid conditions can contribute substantially to disability and functional decline (e.g., severe osteoarthritis, severe heart disease, neurocognitive disorders), whereas other conditions have minimal effects on functioning (e.g., controlled hypertension or hypercholesterolemia). There is a reciprocal interaction between depression and many physical disorders. Depression may result in higher occurrence of certain physical illnesses, and physical disorders may increase levels of depression e.g. mortality rates are higher among postmyocardial infarct patients with depression Depression and anxiety often co-occur, and having more anxiety symptoms (e.g. half of persons with depression have anxiety), is a poor prognostic indicator in depression. One of the more significant health challenges involve persons with some combination of chronic pain , dementia, depression, anxiety, bereavement, multiple losses, social isolation and poor nutrition. Clinical Implications There is some evidence that treating depression can improve health outcomes and that improving physical health can improve depression and anxiety. Unfortunately, the ability to successfully treat depression is less robust in older persons with concomitant physical disorders. Question 8 There are considerable changes in personality over time False 9. There is continuity in personality Each older person is a product of the lifelong effects of physiological, environmental, and psychological factors. With respect to psychological factors, although some changes occur across a lifespan, various personality traits (e.g., coping , sense of control, self-esteem, interpersonal skills) tend to be fairly stable over time, and they will affect how one deals with late-life stressors. Clinical Implications On the positive side, continuity means that most older persons have been able to successfully use various coping strategies to manage their stressors over the life course. Therapists must help to gird up these formerly successful coping mechanisms, and in turn, improve the sense of self-esteem. However, with increasing age and disability, formerly successful strategies may not be working and therapy must address some of the physical, cognitive, and social losses that occur in later life. 10. Psychiatric illness must be understood within a social and biological context The importance of material and emotional resources as well as physiological conditions (co-occurring illness, medications) must be considered. It is said that aging is a bit like gambling: “The longer you go on, the more likely you are to lose.” Thus, older adults have to confront and deal with various losses, perhaps best summarized by the 4D’s of Aging: disability, dependency, desertion (e.g., loss of close relationships as people move away or dying), and death (e.g., one’s own mortality and the death of others). Clinical Implications For some adults who are physically healthy and have strong social resources, a useful strategy might be to encourage activities and engagement following losses of kin or friends or in the context of life stressors. On the other hand, for persons with more disabilities and fewer resources, encouraging too much engagement may be unrealistic and further exacerbate their feelings of worthlessness and depression. 11. The prevalence of psychiatric disorders in older adults and mental disorders are best viewed on a continuum Official psychiatric disorders may not accurately reflect psychiatric distress in the aging community because: Older adults may present atypically, Co-morbid physical and cognitive disorders may make fulfillment of the diagnostic criteria more difficult, Older adults with psychiatric disturbances may cluster in certain settings so that they may not be adequately sampled (e.g., natural occurring retirement communities, assisted living facilities, and nursing homes). Thus, we may need to view illness on a continuum and looking at subsyndromal or subthreshold disorders with respect to depression, anxiety disorders, psychoses, and neurocognitive disorders. Prevalence of Depression The National Comorbidity Survey-Replication (NCS-R) allowed for the most comprehensive examination of psychiatric disorders among older adults in the United States. The 12-month prevalence of depressive mood disorders for persons aged 55+ was 4.9%. There was a steady decline in prevalence across each decade, with the highest rates in the 55 to 64 year old group (7.6%) and the lowest rates in the 85 and over group(2.4%). Age pattern 55 75 85 Prevalence of Anxiety The 12 -month prevalence for anxiety disorders in older adults was 11.6%. However, in this case, while the youngest group (age 55-64) had the highest levels(16.6%), the 75-84 year old age group had lower rates(6.0%) than the oldest age (85+) group (8.1%) 55 Age pattern 85 75 Age differences By comparison, in the national sample, across all age categories (age 18+) the 12 –month prevalence for any mood disorder or anxiety disorder was 9.5 % and 18.1%, respectively (Note the much higher rates in younger than the older groups). In all age groups, major depression was the most common mood disorder and specific phobia were the most common anxiety disorder. Subsyndromal Depression and Anxiety If non-DSM criteria are used, rates of clinical or “syndromal” depression (based on meeting symptom prevalence and severity criteria) is about 12%(range 816%) and may be as high as 24% for subsyndromal (“subthreshold” ) depression. Thus, about one-third of older adults may meet criteria for syndromal or subsyndromal depression. Clinical depression is about 25% in medically ill. Likewise, syndromal and subsyndromal anxiety may be found in slightly over 15% of the older population These findings are important because subyndromal depressive and anxiety disorders have been found to be associated with higher rates of functional impairment, disability, medical illness, and mortality. Prevalence of Psychoses Prevalence rates of psychoses are especially difficult to determine because of the clustering of persons with psychoses in more supported environments or perhaps their unwillingness to consent to interviews. The Epidemiologic Catchment Area study found only 0.3% of persons aged 65 and over had a lifetime history of schizophrenia . The National Comorbidity Study (NCS)-R has not provided age data on non-affective psychoses, although the general population was found to have a 1.5% lifetime prevalence. If one views psychoses on a continuum, NCS-R data indicated that lifetime prevalence of psychotic symptoms in the older adults in the general population is 11%, or over 7 times the lifetime prevalence of the formal diagnostic category for psychotic illness. Prevalence of Dementia and Mild Cognitive Impairment The prevalence rates of dementia have been found to range from 5 to 10%. The prevalence rate is about 1% at age 65, but there is a doubling of prevalence rates every 5 years until age 90, when the rates may continue to increase but more slowly. “MA9” ----Mnemonic for Neurocognitive Disorders (formerly known as dementia & mild cognitive disorder) Based on concern of pt/informant of significant cognitive decline and one or more of the following: Memory & learning impairment Attention impaired(sustained, selective, divided) Aphasia (expression, naming, understanding) Agnosia/Apraxia/Art & visuospatial tasks Appropriate social cognition impaired (emotional recognition, empathy) Abstraction and other executive functioning impaired (planning, decisions, flexibility) --- PLUS--Absence of delirium Ability to function is impaired Causes of Dementia (and most defining features) 1. Alzheimer’s disease 60-70% (insidious onset; memory deficits early; consistency in loss of various cognitive functions) 2. Vascular 10-30% (sudden onset,stepwise; less consistency (“patchy”) in cognitive deficits) 3. Mixed (AD + Vascular) 10% 4. Lewy Body 10-25% (central feature: dementia & 2 of 3 core sx: parkinson sx; fluctuating cognition with variations in attention and alertness; visual hallucinations; also suggestive: neuroleptic sensitivity; REM sleep behavior; also milder cognitive deficits; falls; visuospatial deficits; 5. Depression 5-15% (‘pseudodementia’). 6. Frontotemporal 5-10% : executive or language (semantic/primary progressive aphasia) prominent early; memory less impaired early in disorder. Three types of cellular inclusions: a. Tar-DNA binding protein of 43kDa (TDP-43) --most common b. Tau c. Fused in sarcoma (FUS) protein Both Tau and TDP are associated with diverse pathologic subtypes including CBD, Pick’s, PNP ALS,PD types and semantic dementia 7. Other 10-20% e.g. Parkinson’s disease (movement disorder early--1-yr before dementia) Mild Neurocognitive Disorder (Mild Cognitive Disorder) As with other disorders, a subsyndromal category, “Mild Cognitive Impairment,” has been identified that consists of various objective cognitive deficits (same categories as major cognitive disorder), usually in memory, but daily functioning remains largely intact and self/observer identified decline is “mild”. It is estimated that about 10% of persons aged 70 to 79 have MCI, and this rate is about 20% in the 80 to 89 year old category . Clinical Implications Psychiatric symptoms among older adults are common and may cause dysfunction, even when they do not meet DSM IV criteria. Perhaps even more so than in any other age category, it is important to not overly rely on strict diagnostic criteria and to focus on the clinical symptoms that are causing distress. DSM Disorders in age 65+ (in order of frequency) 12 -month prevalence Anxiety Disorders (phobic disorders,gen anx, panic) 6%-12% female>male Dementia 5-10% female>male Major depression 1-2% female>male Dysthymic disorder 2% female>male Alcohol abuse /dependence 1% male>female Schizophrenia 0.3 -0.5% male=female Bipolar 0.3% male=female Any DSM disorder 12% female>male 12. It is essential to view the treatment goals for older adults with mental illness in the context of a life course trajectory. It is now recognized that the outcome for certain symptoms of schizophrenia in later life are more favorable than previously believed: One-half of persons attain clinical remission (cross-sectional data) as defined as having mild or no symptoms in positive and negative symptoms, Nearly half may attain social recovery. Depression outcome Older persons with depression do less well than previously believed, with roughly half continuing to have clinical depression on follow-up, and perhaps another 30% may have appreciable residual symptoms. Thus, only one-fifth may be in full remission on long-term follow-up. However, with more aggressive and creative treatment strategies, outcome can be improved. Outcome Across Lifespan For persons with severe mental illness, the ideal life trajectory can be viewed as a process moving from diminishing psychopathology and impaired functioning to normalization to positive health and well-being. Psychopathology Community IntegrationSuccessful Aging The initial part of this trajectory may be conceptualized as “recovery,” whereas the latter part may be conceptualized as “successful aging.” Successful aging can be viewed as a state involving the absence of disability accompanied by high physical, cognitive, and social functioning. It is a state that older adults may aspire towards, but often do not achieve. Even among the general aging population, only one-fifth attain “successful aging.” However, among persons with schizophrenia, only about 1 in 50 persons attain this status. Clinical Implications We now recognize that for many persons with schizophrenia, middle and older age is associated with better outcomes than previously believed, and that as some of the more severe symptoms relent, and certain social pressures diminish (e.g. need to have full-time work or marry), it may be an optimal time to make strides toward greater recovery. For older persons with depression, complete and permanent recovery is difficult, and the clinician needs to recognize that depression in later life is often a chronic disorder that requires more patience and clinical efforts than previously believed. In some instances depression may be a prodrome of dementia or neurological disorders (e.g. Parkinson’s disease) 13. Disorders overlap with respect to neuropathology and symptoms We now recognize that many of the dementia disorders share neuropathology Overlap among Various Dementias •Pure AD and VaD may be rare. Pure PD Pure AD •AD is multifactorial. •Similar risk factors: cholesterol, APOE4, DM, HTN. •Vascular pathology may contribute to cholinergic abnormalities in both disorders(cholinesterase inhibitors may help with both). Pure LBD Pure VaD Vascular Dementia All have cholinergic deficits in cortex AD (often with EPS)(40 -65%), PDD(75%), LBD(60-90%) Psychotic depression Many disorders share symptoms Schizophrenia with depression depression psychosis Schizophrenia with cognitive deficits PDD, LBD, AD, VaD with psychotic sx med conditions & drugs Depression with dementia (“pseudodementia”) Vascular depression with mild cognitive impairment (MCI) MCI with depression dementia Dementia with depression PD with depression movement disorders Schizophrenia with movement disorders PDD, LBD, PD+ with cognitive deficits PDD, LBD, AD with movement sx Examples: 1. Prevalence of Neuropsychiatric Symptoms (i.e., Psychiatric and Behavioral Problems) in AD Psychoses: Hallucinations:24% about half Delusions:50% Mood disturbances(depression,tearfulness):29% About one-quarter 2. Hallucinations in PD, DLB, PDD ¼ Parkinson’s Disease ½ Dementia Lewy Body ¾ Parkinson’s Disease Dementia Note: In PD and PDD medications may contribute to psychotic sx 3. Depression and Parkinson’s Disease In Parkinson’s disease about 40-50% have depression; about 1/3 have anxiety disorder Depression precedes motor dysfunction in 12 to 37% of PD patients Clinical Implications Because symptoms and pathology overlap, obtaining good histories and conducting comprehensive evaluations are necessary to determine the diagnosis. Obtaining a good history is critical Psychoses Cognitive Impairment Depression Movement Disorder Recent Onset Primary Mental Illness: Depression (mood congruent delusions) Secondary to physical illness or drugs: Delirium Psychoses Depression Longer duration Primary Mental Illness: Schizophrenia (bizarre delusions, auditory hallucinations more common, psychoses precedes depression & any movement sx); Delusional disorder (circumscribed delusion; mild hallucinations, depressed mood secondary to delusions) Psychiatric sx are secondary: Alzheimer’s disease (dementia depression psychoses movement disorders); Lewy Body Dementia ( psychoses and dementia and movement disorder within 1 year) Parkinson’s Disease (movement disorder psychoses dementia Five “Ds” of Psychiatric Disease in Older Adults Think of these possibilities and consider course: Delirium: days to weeks Drugs: days to months Disease: days to months Depression: weeks to months Dementia: months to years 14. Mental illness in older age is complex Items 2 through 13 suggest a high degree of complexity with respect to the interaction of age and mental illness. In later life there is a complex interaction between depression, anxiety, physical illness, cognitive impairment, personality factors, and life stress. Although aging is associated with a multitude of stressful events, older adults do not develop more psychiatric disturbances. For example, the prevalence of major depression is lower in elderly persons than young and middle-aged adults . Many elders have physiological, psychological, and environmental resources that modify these processes and avert unfavorable outcomes. Clinical Implications A good clinician must recognize the biopsychosocial factors influencing the mental state. Care of the older adult, each biological, psychological, and social element is likely to be more complex than in younger adults because their longer life has provided more experiences as well as more chances for interactions among these elements. •Importantly, older adults are survivors, having outlived many of their original age cohorts, and they have strengths that must be recognized along with any shortcomings. Important : Use these questions to study for examination Test yourself on Alzheimer’s disease(AD) and dementia— True or False? 1.Memory loss must always be present in dementia true 2. Depression is found in about ½ of AD patients false 3. Dementia is occurs about 5-10% of the elderly population true 4. Mild cognitive impairment includes memory problems and functional impairment false 5. Plaques and tangles may be found in AD, PD, and LBD 6. Psedodementia is usually not a prodrome of dementia 7. LBD is characterized by visual hallucinations, EPS, and cognitive sx true false true Test yourself on depression and anxiety—true or false? 1. About one-fourth to one-third of community elders have syndromal or subsyndromal depression true 2. Among older adults, the highest rates of DSM depressive disorders are found in the 85+ group false 3. About ¼ of medically ill persons suffer from depression true 4. Mortality rates are not greater among post MI pts with depression false 5.Social withdrawal is rare among older depressed pts 6. Vascular depression is associated with apathy false true 7. Elders with major depression are more likely to show social withdrawal true 8. Elders with major depression are more likely to talk about physical symptoms true false 9. Anxiety and depression rarely occur together 10. It is best to use drugs that undergo phase 1 and phase 2 metabolism in older adults false 11. Anxiety disorders are the most common disorders in elderly persons true Test yourself on schizophrenia-true or false? 1. About ¾ of schizophrenia begins before age 40 true 2. Compared to early onset cases, persons with late-onset true schizophrenia are more likely to have visual hallucinations, to be more paranoid, and to be women 3. Psychotic symptoms generally do not improve over the life course of schizophrenic persons false Congratulations—you are now an expert in geriatric psychiatry