* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Co-occurring addiction and mental disorders
Deinstitutionalisation wikipedia , lookup
Political abuse of psychiatry wikipedia , lookup
Child psychopathology wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Moral treatment wikipedia , lookup
Schizophrenia wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Alcohol withdrawal syndrome wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
History of psychiatry wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Mental status examination wikipedia , lookup
Sluggish schizophrenia wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Abnormal psychology wikipedia , lookup
History of mental disorders wikipedia , lookup
Antipsychotic wikipedia , lookup
Addiction psychology wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
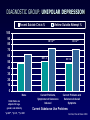
Co-occurring Addiction and Severe Mental Disorders Richard Ries MD Harborview Medical Center University of Washington Seattle, Wa Dr Ries speaks for: Lilly, Janssen, Pfizer, Forest, Zeneca, Bristol Myers, Abbot, States, counties, NAMI, mental health centers, addiction agencies, and others (even in prisons) DUAL DIAGNOSIS IS: TWO DIAGNOSES/ DISORDERS TWO SYSTEMS DOUBLE TROUBLE IN THE EYE OF THE BEHOLDER Examples of Dual Disorders: MENTAL DISORDERS Schizophrenia Bi-polar Schizoaffective Major Depression Borderline Personality Post Traumatic Stress ADDICTION DISORDERS Alcohol Abuse/Depen. Cocaine/ Amphet Opiates Marijuana Polysubstance combinations Prescription drugs CHARACTERISTICS OF THE DUAL DIAGNOSIS CLIENT IN KING COUNTY Severity of Chemical Dependency High LH HH 2 Severity of Psychiatric Condition 1 4 Low 3 HL LL Low High Dual Disorders for Everyone? If applied to all cases, Term has no meaning Both Mental and Addiction Disorders need to be over threshold Personality Disorders, other than Borderline not usually counted Substance Induced Disorders cause diagnostic confusion Drug Induced Psychopathology Drug States Withdrawal Acute Protracted Symptom Groups Intoxication Chronic Use Depression Anxiety Psychosis Mania Systems Problems Different Different Different Different Different Different Different Laws…commitment/confid. funding..audits etc personnel training certification sites Norms DOUBLE TROUBLE Hall Alterman Solomon Safer Drake Barbee Lyons Chen ’77 ’85 ’86 ’87 ’89 ’89 ’89 ’92 Poor out-pt attendance, discontinue Rx More mood changes, intensive staffing More noncompliance, arrests Over twice hosp. rate and criminal behav More hostility, noncompliance More psych symptoms More noncompliance, ER, jail, rehosp. Worse treatment course Likelihood of a Suicide Attempt Increased Odds Of Attempting Suicide Risk Factor Cocaine use Major Depression Alcohol use Separation or Divorce NIMH/NIDA 62 times more likely 41 times more likely 8 times more likely 11 times more likely ECA EVALUATION Therapy Plan Bio Psych Social Psych Labs Meds (antipsychotics etc.) 1:1 cog/beh Psychoeducation Groups etc Couples conf. D/C planning housing, etc. CD Labs Meds (withdrawal, craving, etc.) Step work Groups AA Meetings Intervention Sober housing Engaging the Chronically Psychotic Patient Noncoercive engagement techniques Assistance obtaining food, shelter, and clothing Assistance obtaining entitlements and social services Drop-in centers as entry to treatment Recreational activities Low-stress, non-confrontational approaches Outreach to patient’s community Coercive engagement techniques Involuntary commitment Mandated medications ( parole etc) Representative payee strategies CSAT TIP 1994 CHARACTERISTICS OF THE DUAL DIAGNOSIS CLIENT IN KING COUNTY Severity of Chemical Dependency High LH HH 2 Severity of Psychiatric Condition 1 4 Low 3 HL LL Low High CURRENT SUBSTANCE USE PROBLEMS in acute psychiatric inpatients % None % Current but low SI sx % Current and high SI sx 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Bipolar, Depressed Comtois, Ries & Russo 2004 Bipolar, Manic Unipolar Depression Schizophrenia/Schizoaffective DIAGNOSTIC GROUP: BIPOLAR DEPRESSED Recent Suicide Crisis % 100 90 80 70 60 50 40 30 20 10 0 Lifetime Suicide Attempt % OR 2.1*** OR 2.5*** OR 1.5* OR 1.0 None Odds Ratios are adjusted for age, gender, and ethnicity *p<.05**, **p<.01, ***p<.001 Current Problems, Symptoms not Substance Induced Current Problems and Substance Induced Symptoms Current Substance Use Problems Comtois, Ries & Russo 2004 DIAGNOSTIC GROUP: BIPOLAR MANIC Recent Suicide Crisis % 100 90 80 70 60 50 40 30 20 10 0 Lifetime Suicide Attempt % OR 3.4*** OR 2.5*** OR 2.2** None Odds Ratios are adjusted for age, gender, and ethnicity *p<.05**, **p<.01, ***p<.001 Current Problems, Symptoms not Substance Induced OR 3.1*** Current Problems and Substance Induced Symptoms Current Substance Use Problems Comtois, Ries & Russo 2004 DIAGNOSTIC GROUP: UNIPOLAR DEPRESSION Recent Suicide Crisis % 100 90 80 70 60 50 40 30 20 10 0 Lifetime Suicide Attempt % OR 1.6*** OR 1.2 None Odds Ratios are adjusted for age, gender, and ethnicity *p<.05**, **p<.01, ***p<.001 Current Problems, Symptoms not Substance Induced OR 1.6*** OR 1.0 Current Problems and Substance Induced Symptoms Current Substance Use Problems Comtois, Ries & Russo 2004 CAGE QUESTIONS Cut Down (or stopped) Annoyed when asked drug/alc. use discussed Because symptoms worsened Because doctor or therapist suggested Annoyed, angry, fights when using Admitted to ER or hospital when using Guilty about use Guilty, depressed, suicidal when using Ever made a suicide attempt when using CAGE Questions Eye opener: taken drink or drug in AM to feel better Taken drink or drug with meds Not taken meds because of using drug/alc (forgot, avoid mixing, etc.) What are 2 or 3 reasons you use alc/drugs? What are 2 or 3 reasons you should stop or cut down? Substance Induced Mania Methamphet/Cocaine Ecstacy Halucinogens Alc/Benzo withdrawal? Med/Substance induced true Bipolar Dual Bipolar Video Bipolar vs Sub induced sytmptoms Types of substance Addiction vs Psych behavioral problems Denial Psych Substance Recovery Issues Meds 12 step, other groups Risk of Relapse in Patients With Schizophrenia Rate of relapse among patients treated with conventional antipsychotics for first-episode schizophrenia and schizoaffective disorder 16% at 1 year 54% at 2 years 82% at 5 years * Stable patients were allowed the option to discontinu antipsychotic medication after 1 year of treatment The risk for a first and second relapse was almost 5 times greater than when not taking medication* Risk is diminished by maintenance antipsychotic drug treatment Based on a survival analysis of relapse using medication status as a time-dependent covariate. Source: Robinson D, Woerner MG, Alvir JMJ, et al. Arch Gen Psychiatry. 1999;56:241-247. Barriers to Adherence to Antipsychotic Therapy Cognitive impairment Complex drug regimen (eg, BID dosing) Adverse events (eg, side effects, weight gain, EPS, diabetes ) Monitoring of selected adverse events (eg, ECG, blood, glucose, liver functioning, electrolyte, slitlamp testing) Cost of medication Source: Substance abuse Perkins DO. J Clin Psychiatry. 1999;60(suppl 21):25-30. Comorbid Substance Abuse Associated With Noncompliance in Schizophrenia P < 0.05 Nearly half of all patients in a prospective 4-year study (N = 99) were active substance abusers (n = 42) Patients who actively abused substances were significantly more likely to be noncompliant 67% % Noncompliant 80 60 47% 40 34% 20 0 No Past Past Current History History User Hunt GE et al. Schizophrenia Res. 2002;54:253-264. It may not be that the med(s) stopped working, but…… The patient stopped the med The patient stopped the med AND used drugs and/or alcohol…... OR lowered the med and used… OR used on top of the med…. OR used twice the dose on one day and nothing the next…. Stimulants ( cocaine/amphets) are most MSE destructive. Features of Schizophrenia Positive Symptoms Delusions Hallucinations Disorganized Speech Cognitive Deficits Attention Memory Executive Functions (e.g., abstraction) FUNCTION Work Interpersonal Relationships Self-care Negative Symptoms Affective Flattening Alogia Avolition Anhedonia Social Withdrawal Comorbid Conditions Depression Anxiety Aggression Substance use disorder DIAGNOSTIC GROUP: SCHIZOPHRENIA/SCHIZOAFFECTIVE Recent Suicide Crisis % 100 90 80 70 60 50 40 30 20 10 0 Lifetime Suicide Attempt % OR 1.8*** OR 1.5** None Odds Ratios are adjusted for age, gender, and ethnicity *p<.05**, **p<.01, ***p<.001 Current Problems, Symptoms not Substance Induced OR 1.7*** OR 1.7*** Current Problems and Substance Induced Symptoms Current Substance Use Problems Comtois, Ries & Russo 2004 Substance Induced Schizophrenia Methamphetamine/Cocaine Ecstacy Hallucinogens ( strong THC too) Alcohol Hallucinosis Meth vs Schiz Meth Later onset Clear regular heavy drug use Lifestyle More likely to preserve general function Usually paranoid and voices, but not many negative sx Schiz Earlier onset Prodrome of withdrawal, negative symptoms, few friends More global impairment, thought disorder May have drug use but usually much less Schizophrenia Patient video Positive and Negative features Substance effects Medications and side effects Social interactions Harborview Dual Dx Program Ongoing diagnosis and Rx adjustment Patient/Treatment matching (stage of change, women’s issues etc Bio-psycho-social approach incorporating psychiatric, addiction, and rehabilitation principles and staff Interactive with spectrum of care on-site, off-site resources, shelters, AA etc Consumer involvement Pre-vocational and vocational and housing incentives, Legal, as well as Social Security payeeship, etc. (carrot and stick) HARRP Program In MICA Patients: Diagnoses are complicated Presence of severe and persistent mental illness Compliance is a major problem Falling between the “cracks” of treatment systems Engaging the Chronically Psychotic Patient Noncoercive engagement techniques Assistance obtaining food, shelter, and clothing Assistance obtaining entitlements and social services Drop-in centers as entry to treatment Recreational activities Low-stress, non-confrontational approaches Outreach to patient’s community Coercive engagement techniques Involuntary commitment Mandated medications Representative payee strategies CSAT TIP 1994 The primary goals of PACT treatment Increase community tenure Lessen or eliminate debilitating psychiatric symptoms Prevent relapse of psychiatric symptoms Meet basic needs and enhance quality of life Reduce substance abuse and money management problems Improve functioning in adult social and employment roles/activities Lessen the family’s burden of providing care What are the Fundamental PACT Principles? Primary provider of services Fixed point of responsibility Community-based services Highly individualized services An ‘assertive’ can-do approach Continuous long-term services Counseling strategies….1:1 Problem identification, Addiction, housing, job, MOOD etc Treatment planning ASI domains…one of these is psych. Biopsychosocial What are availabilities of your site/agency Counseling strategies Social support/case management Linkage to onsite/offsite services 12 step facilitation Cog/behavioral Motivational Interviewing Couples/family Group Group Therapy What types of pts? only non-psychotic…only motivated, only female, only alcoholics…only noncompliant????? How often/week, how long/session Single or co-therapy Dual Group Therapy Process group , or theme/didactic Structured/ unstructured Pt co-therapist Activities/celebrating birthdays etc Using a “check-in” Name/ Addiction dx/sobriety date/what I’m doing to stay sober Psych dx/meds/what I’m doing to get better Dual Check In Using a “check-in” Name/ Addiction dx/sobriety date/what I’m doing to stay sober Psych dx/meds and compliance/ what I’m doing to get better How am I feeling on a 10 pt scale Relapse cues Do I need time in group for a current problem Harborview Co-occurring subprograms Different strokes for different folks Case management vs psychotherapy Mix of CD and MH Psychotic/Non-Psychotic Male/Female Homeless Residential/Therapeutic Community TWO DIMENSIONAL AXIS OF PSYCHIATRIC AND CHEMICAL DEPENDENCY Substance Abuse MICA Severe ACT Moderate Psychopatholog y Borderline Mild Rehab Mild Severe Moderat e Wingerson & Ries, 1999 CLINICAL SEVERITY OF PATIENTS BY TREATMENT TEAM ACT REHAB MICA BORDERLINE 12 10 8 6 4 2 0 Average # Lifetime Psych Hosp Average # Invol Lifetime Average # Incarcerations Psych Hosp Past 5 Yrs Wingerson & Ries, 1999 CONTINGENT BENEFITS STUDY-NIDA POWER: THEORETICAL ANALYSIS 100 Contingency effect 75 Multiple, weekly dispersals 50 25 Having Rx center be payee 0 Ries: Psych Serv 04 4. Substance use a. Total # of days/week use (if “0”, leave b,c,d blank) b. Specific Days Alcohol M T W Th F Sa S c. Specific Days Drugs M T W Th F Sa S d. Unknown substance M T W Th F Sa S Weekly Substance Use Summary Code days 0=No use; 1=1 day; 3=2+ 5. Treatment Adherence a. Attendance (% of Rx plan) b. Medications (frequency/amount; % correctly taken) c. Enter lowest % of attendance or medication adherence Weekly Adherence Summary Code 0>80%; 1=60-79%; 3<60% 6. Money Management Budgets and spends payee money appropriately • Circle best response: 0-19% 20-49% Weekly Money Management Summary Code 50-79% 80-100% 0>80%; 1=50-69%; 3<50% Scoring: WEEKLY DECISION SUMMARY INSTRUCTIONS •If Weekly Status Sum=0, circle “0” in Decision Summary Score (below), congratulate, give gold award. •If Weekly Status Sum=1 or 2, circle “1” in Decision Summary Score (below), encourage better behavior, give silver award. •If Weekly Status Sum=3 or greater, circle “3” in Decision Summary Score (below), encourage better behavior, give red award. Weekly Decision Summary Score (circle one): 3 Type of Award Given (circle one): Gold 1 Red 0 Silver Preliminary Findings - 5/99 Contingent Benefits Study (Ries NIDA) 65% Cont. 51% p< .008 Non-Cont. 53% 51% alcohol weeks clean / total weeks = % Ries, Am J Addict 04 Medication monitoring and motivating Know who is on what and what for Know the prescriber if possible Sit in on med sessions now and then if possible Know something about meds…(Tech transfer centers summary, NEW CO-OCCURRING TIP) Ask the pt about taking or not/side effects, fears, biases, pressure from others..use motivational strategies Medications Essential to Treatment of Severely Mentally Ill Substance Use and Not-Taking Meds are the 2 top reasons for De-Comp Should be part of court orders Monitored by Case managers, nurses, doctors Anti-psychotics New: Clozaril, Zyprexa, Risperdal, Seroquel, Geodon, Abilify……better response, fewer side effects ( except wt gain) and better compliance. Consta = 2 week IM risperdal Old: Haldol, Prolixin ( both come as oral and as 2-4 week shots, called decanoate), others include Navane, Trilafon…….all cause more side effects Weight, Lipids, Diabetes…. …Isn’t that what being an American is all about ? HMHS: Body Mass Index (BMI) from Vital Exam: 44.8 45 40 % of Clients 35 29 30 23 25 20 15 10 5 3.2 0 Underweight Normal Weight Overweight Obese Mean=29.8 (sd=6.7), Median=29.1, Range from 14.4 to 49.9 BMI Categories: Underweight<18.5; Normal=18.5-24.9; Overweight=25-29.9; Obese>30 Cause of death in HMHS long term patients Cardiac…………………………. 50% profile average is 49 yo male Other medical illnesses and accidents…………………………25% Suicide …………………………..17% Other ………………………………8% Atypicals and Health issues Drug Weight gain Risk for diabetes Worsening lipid profile Clozapine +++ + + Olanzapine +++ + + Risperidone ++ D D Quetiapine ++ D D Aripiprazole* +/- - - Ziprasidone* +/- - - + = increase effect; - = no effect; D = discrepant results. *Newer drugs with limited long-term data. Source: Diabetes Care, February 2004 Anti-depressants Used for Major depressions Also used as auxillary meds in Bipolar, Schizophrenia, others SSRI’s include Prozac, Paxil, Zoloft, Celexa. Others: Serzone, Trazedone (sleep), Remeron, Effexor, Welbutrin Older ones: Elavil, Sinequan…more side effects Anti-Bipolar Meds Lithium..oldest, cheap Anticonvulsants : Depakote, Tegretol, Gabapentin, Lomotragine……gaining share…may also help impulse control….expensive Newer Antipsychotics…Zyprexa most researched, expensive, wt gain, but effective…also Geodon, Abilify- effective and NO Wt GAIN, also appear Diabetes/lipid neutral Ziprasidone: What about IM use? IM Ziprasidone has virtually replaced IM Haldol in ER’s at Harborview, the Seattle VA and on Harborview’s most intense, locked psychotic unit IM Haldol has been one of the most longstanding, unchanging, acute interventions in all branches of Medicine Dealing with SMI persons in court If clearly psychotic, agitated or confused,…use fewer more direct statements and questions, which don’t require complex responses Be Direct, for example: “Mr Smith, it appears that you might be having some difficult to understand experiences and that maybe these are causing you to get agitated and I therefore wonder if you might sit down” ………..versus……..”Please sit down and behave Mr Smith” Keep Calm