* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Learning and Sleep - University of Illinois Archives
Personality disorder wikipedia , lookup
Excoriation disorder wikipedia , lookup
Panic disorder wikipedia , lookup
Autism spectrum wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Bipolar disorder wikipedia , lookup
Depersonalization disorder wikipedia , lookup
Conversion disorder wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Asperger syndrome wikipedia , lookup
Restless legs syndrome wikipedia , lookup
Mental disorder wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Conduct disorder wikipedia , lookup
Abnormal psychology wikipedia , lookup
History of psychiatry wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Spectrum disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Idiopathic hypersomnia wikipedia , lookup
Classification of mental disorders wikipedia , lookup
History of mental disorders wikipedia , lookup
Circadian rhythms
Circadian rhythms ("circa," about; "dia," day) are those that occur on a 24 hour daily
cycle.
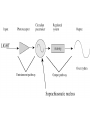
A variety of studies in animals supported by human clinical studies indicate that the
suprachiasmatic nucleus, in the hypothalamic region of the brain is the highest level
pacemaker, with an intrinsic rhythm of about 24 hours' duration. This intrinsic
rhythm in turn becomes entrained by environmental cues, typically the light-dark
cycle.
The psychiatric disorder that appears to be most closely related to circadian
rhythmicity is seasonal affective disorder (listed as bipolar 1 disorder, bipolar II
disorder or major depressive disorder, recurrent, “with seasonal pattern”), a
cyclothymic (depressive) disorder that tends to occur in the fall or winter as
daylength shortens.
Seasonal affective disorder often goes into full remission (or a change from
depression to mania or hypomania) as daylength increases in the spring. This is
often diagnosed when there are regular seasonally-occuring depressive episodes (at
least twice) and no other periods of depression. This disorder often responds to
lithium treatment or lithium combined with other antidepressants.
However, it has also been shown that SAD can be treated by exposure to bright lights
that contain the ultraviolet spectrum. As yet, the effects of light therapy on
depressed patients with other etiologies have not been thoroughly evaluated, so
specificity to this disorder is uncertain.
Physiology and Behavior of Non-REM and
Autonomic Regulation:
Cerebral Blood Flow
Brain Temperature
Body Temperature Regulation
Respiration
Heart Rate
Skeletal Musculature:
Muscle Tone
Knee Jerk Reflex
Body Twitches
Eye Movements
Cognition:
Neural Activity:
Cerebral Cortex Unit
EEG
REM Sleep
Low
Reduced
Normal
Slow
Slow
High
Increased
Impaired
Variable
Variable
Reduced
Normal
Infrequent
Infrequent, slow,
nonconjugate
Gone
Inhibited
Frequent
Rapid, conjugate
Wandering, vague Vivid dreams
Reduced activity, Increased activity,
phasic
tonic
Slow large waves, High frequency, waking-like
delta
REM Sleep as a Percent of Total Sleep by Age
SLEEP DISORDERS
Dyssomnias: True disorders of sleeping
* Intrinsic (e.g., intrinsic insomnias, hypersomnias, narcolepsy, sleep apneas, limb
movement disorder)
* Extrinsic (e.g., altitude insomnia, stimulant-dependent sleep disorder, alcoholdependent sleep disorder)
* Circadian rhythm (e.g., time zone change (jet-lag), shift-work, delayed or advanced
sleep phase syndrome)
Parasomnias: Abnormal behaviors that interrupt sleep
* Arousal disorders (e.g., sleep walking, sleep terrors [non-REM, vs. nightmares])
* Sleep-wake transition disorders (e.g., sleep talking, nocturnal leg cramps)
* Parasomnias of REM sleep (e.g., nightmares)
* Other parasomnias (e.g., sleep enuresis, SIDS)
SLEEP DISORDERS (cont'd.)
Medical-Psychiatric Sleep Disorders:
* Associated with mental disorders (e.g., mood disorders, anxiety, schizophrenia)
* Associated with neurological disorders (e.g., Dementia, Parkonsonism, sleep-related
epilepsy)
* Associated with other medical disorders (e.g., sleeping sickness, nocturnal cardiac
ischemia)
CHRONIC INSOMNIA
* 20% to 30% of the adult population complains of trouble sleeping.
* Most common: persistent difficulty in getting to sleep (>45 min., > 3 X / week, > 3 weeks)
Most Common Causes:
* Emotional style (anxiety, depression, hyperaroused-restless)
* Conditioned poor sleep: loss of "confidence" in the ability to sleep (often following events that
disrupt sleep for several nights)
* Drugs: Use or withdrawal from cigarettes, alcohol (induces sleep but with "rebound" @ 3-4
hrs.), diet pills, prescription drugs (benzodiazepines can reduce delta sleep; cyclic antidepressents
reduce REM sleep); consumption of coffee
* Medical-psychiatric disorders (Recall major Mood Disorders)
* Intrinsic sleep disorder (periodic limb movement disorder, sleep apnea)
If an intrinsic disorder is suspected, a polysomnogram (PSG) or clinical sleep recording from a
sleep lab is warranted.
*
EEG, eye movements
*
Chin, limb EMG (tone; sleep movement disorders)
*
Respiration (sleep apneas)
TREATMENTS FOR SLEEP DISORDERS
* Psychotherapy (control of negative thoughts, etc.)
* Pharmacotherapy (short-term, not chronic!)
(benzodiazepines: Halcion, Restoril)
* Behavioral (e.g., progressive relaxation, biofeedback,
thought stopping)
* Sleep hygiene (regular schedule, minimize light and noise,
eliminate non-prescription drugs, exercise, etc.)
Disorders of Excessive Daytime Somnolence
(Falling asleep at a desk or IN CLASS!)
Insufficient Sleep Syndrome: pressures of work, being on call, late partying. Treatment:
induce common sense; revamp the practice of medicine.
Sleep Apneas: Daytime sleepiness due to sleep disturbance. Mostly middle-aged, older
males with obstructive sleep apnea, a breathing disorder. May be associated with obesity,
excess alcohol or drug use. Other apneas of central origin also are seen, but rare.
Obstructive sleep apnea may be treated by sleep position training, weight loss, alcohol
reduction, mechanical devices to improve breathing, or surgery (e.g., tonsillectomy).
Narcolepsy: Pathological daytime sleepiness. Diagnosed by absence of apneas, rapid
onset of REM. Multiple sleep latency test (5 daytime naps at 2 hr intervals following the
nighttime PSG) to see if REM onset is rapid during the day. Can be treated with stimulant
drugs.
Parasomnias
Disorders such as sleepwalking and sleep terrors tend to occur in children and adolescents
and to disappear in adulthood. Sleepwalking may occur/recur in adults under stress.
Sleep Deprivation Effects
Mild: increased irritability, difficulty in concentrating, disorientation (particularly in the
morning), impaired sensory-motor coordination and performance.
Severe: Hallucinations, "bizarre" behaviors can result
Recovery from deprivation: Compensatory increases in REM and delta sleep occur during
subsequent sleep cycles; "intensity" of rapid eye movements and other sleep characteristics
may increase.
Intense exercise, e.g. marathons, increase sleep time, particularly deep non-REM delta sleep.
Learning and Sleep
Learning during sleep: it happens, especially in the lighter stages of sleep, but it is not a
particularly efficient way to learn.
There is evidence for a relationship between REM sleep and memory formation:
*
REM sleep increases following learning and in rats in enriched environments
*
Material learned before a night's sleep is better remembered in the morning than
a list learned prior to 8 hours waking before recall testing.
*
REM deprivation in advance impairs learning
*
REM deprivation after learning: data equivocal




















![Final_Exam_Study_Guide[1].](http://s1.studyres.com/store/data/010111588_1-cbc32fd81262c5db5d7117680859ab3a-150x150.png)
