* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Matherly, K
Survey
Document related concepts
Transcript
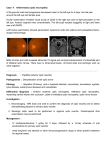
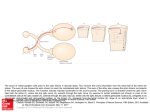
The Demyelinating Dilemma: An Atypical Presentation and Prognosis of Optic Neuritis 36YO WM with a history of MS presented with NLP of the left eye, with initial head MRI revealing no enhancement of the optic nerve. Diagnosis of optic neuritis was confirmed after dedicated orbital MRI. I CASE HISTORY Demographics *36 year-old caucasian male Chief complaint *Onset of blur OS and associated periorbital ache the day before with complete loss of vision OS upon awakening that morning Ocular history *Retrobulbar optic neuritis OD secondary to Multiple Sclerosis (MS) diagnosed in 2010; presented with BCVA: 20/80, which fully recovered to 20/20 after treatment. Medical history/family medical history *Aggressive Multiple Sclerosis diagnosed in 2010 after first episode of optic neuritis OD -Poorly controlled symptoms- had multiple sessions of IV steroids to control his symptoms, which have alternated between right- sided and left-sided weakness, numbness/tingling, and spasticity. -Has been on four different disease-modifying therapies but continues to develop new lesions evident on MRI. -Overview of MRIs: multiple enhancing and non-enhancing lesions of the brain and cervical spine; several non-enhancing lesions of the thoracic spine; new lesions have been noted on every MRI scan since baseline in 2010. *Father died at age 42 due to complications from MS. *Paternal aunt died from progressive MS complications. *Two siblings have not been diagnosed with MS. Current Medications *fingolimod 0.5mg QD *cholecalciferol 2,000 units QD II PERTINENT CLINICAL FINDINGS Clinical *VA: 20/20-2 OD, NLP OS *Pupils: equal & round OU, direct response intact OD, no consensual response OD; no direct response OS, consensual response intact OS; 4+APD OS *EOMs: full with no pain on eye movement *Color vision: 12/14 plates Ishihara OD, unable to test OS *Contrast sensitivity: 1.28 OD, unable to test OS *SLE: mechanical ptosis OS- mildly thickened and erythematous upper eyelid without hordeolum/chalazion; normal cranial nerve testing; no fatigue of ptosis on upgaze *Optic nerves: flat with distinct margins OU; temporal pallor OD, no definitive pallor OS Ocular Imaging (images available) *RNFL OCT OD: severe RNFL thinning ST, T, IT, IN, which is stable to baseline (1/6/11); borderline RNFL thinning SN & N, which is newly noted compared to baseline OS: severe RNFL thinning ST, T, IT, which is stable to baseline (1/6/11) *Macular OCT: normal foveal contour; no CME OU *Humphrey visual field OD: reliable, superior partial arcuate defect OS: complete field loss Radiology studies (images available) *1st MRI: -Brain: No active enhancing lesions seen along the cerebral white matter and no evidence of optic neuritis; several non-enhancing lesions stable to previous MRI -Spine: Elongated lesion involving the upper cervical cord at C2 level with no active enhancement; smaller foci of T2 hyperintensity along the dorsolateral aspect of the cord extending from C3-C6 with no enhancement nd *2 MRI: -Orbit: Mild asymmetric enhancement of the intraorbital left optic nerve, which can be seen in the setting of optic neuritis Laboratory studies *Serum NMO-IgG = negative *Aquaporin 4 receptor antibody = negative *Lyme, toxo, HIV, syphilis = negative III DIFFERENTIAL DIAGNOSIS PRIMARY: *Retrobulbar optic neuritis *Neuromyelitis optica (Devic’s disease) SECONDARY: *Infectious optic neuropathy *Inflammatory optic neuropathy *Toxic/nutritional optic neuropathy *Anterior ischemic optic neuropathy *Leber’s hereditary optic neuropathy *Central artery occlusion *Compressive lesion/tumor IV DIAGNOSIS & DISCUSSION Optic neuritis secondary to MS is characterized as an idiopathic, demyelinating inflammation of the optic nerve, which is typically associated with decreased vision, pain on eye movement, dyschromatopsia, reduced contrast sensitivity, visual field loss, and optic nerve edema in one-third of patients. According to the Optic Neuritis Treatment Trial study (ONTT), only 3% of patients diagnosed with optic neuritis presented with no light perception of the affected eye, making our patient’s presentation atypical. There is also evidence of spontaneous visual recovery in >90%, and the patient maintains NLP vision three weeks post-onset. Two weeks after presentation, the patient reported “pinpoint lights/sparkles” that were most noticeable inferiorly and superiorly. He also reported that vision was more “gray/translucent” in the temporal half of his visual field. He continues to monitor his vision daily by directing a flashlight at different angles and attempting to perceive hand motion, but vision has remained stable. Poor visual recovery at one month follow-up is a poor prognostic sign, and it has almost been one month. Initially, MRI of the brain did not show enhancement of the left optic nerve, which was unexpected. MRI of the orbit was needed to visualize the small, subtle enhancement of the left intraorbital optic nerve. The minimal enhancement in the setting of profound vision loss suggested the possibility of inflammation extending into the optic canal, which has been associated with worse visual prognosis in some studies. The extent of the lesion usually correlates with vision at the time of diagnosis and visual prognosis. A more obvious, extensive lesion would be expected in the case of NLP. If the left optic nerve had not shown an enhancing lesion on MRI, the diagnosis of optic neuritis would be less likely. It is estimated that 95% of patients diagnosed with optic neuritis show optic nerve enhancement on MRI. The patient’s severe presentation of presumed optic neuritis indicates that further investigation is needed to rule out Neuromyelitis optica (NMO). NMO is characterized as a severe demyelinating disease that predominately attacks the spinal cord and optic nerves. Several of the patient’s findings are consistent with NMO: 1)vision loss is typically more severe in optic neuritis secondary to NMO; 2)limb weakness/spasticity is a common feature; 3) spinal cord lesions are prominent on MRI, although the patient has not been diagnosed with longitudinally extensive acute transverse myelitis (lesions extending over 3 or more vertebral segments), which is a supportive criteria for diagnosis of NMO. 70% of patients with NMO express antibodies to the aquaporin-4 (AQP4) receptor. The absence of the AQP4 receptor antibody (NMO-IgG) does not rule out NMO, but its presence is diagnostic. The patient’s lab results were negative for NMO-specific autoantibodies. Early diagnosis and treatment of NMO is essential. Research shows that most patients with relapsing NMO have severe disability, and one-third died of respiratory failure. The patient’s diagnosis of MS remains unchanged at this time, due to multiple plaques on MRI of the brain that are more suggestive of MS, negative lab results for NMO-specific autoantibodies, and the patient’s symptoms, as well as age, race, and residence at a higher latitude. The patient had bilateral RNFL thinning OD>OS on his baseline OCT, and there were no changes in the left eye compared to baseline. Research shows that bilateral RNFL thinning is often detected in patients who have had ON in only one eye, and this is thought to be due to an optic neuritis attack that does not alter visual function enough for that particular patient to report it. Other possibilities include subclinical inflammation of the optic nerve, transsynaptic degeneration elsewhere in the visual pathway, or neurodegeneration in white matter that appears normal. V TREATMENT & MANAGEMENT *Neuro: -IV methylprednisone x 5 days -Discontinued fingolimod due to elevated liver enzymes and started beta interferon injections 3x/week, which is one of the only drug therapies that the patient has not tried -Continue IV steroid therapy as needed to control symptoms -Follow-ups every 3 months including MRI *Optometry: -Extensive education on the possibility of visual recovery, driving precautions, and returning for evaluation if the vision in the right eye worsens -Call the patient every week to monitor visual status -Follow up in 3 months with full dilated exam and OCT Sixty-seven percent of patients with optic neuritis secondary to MS who presented with NLP vision of the affected eye recovered vision that was 20/40 or better. Forty-four percent recovered peripheral visual field, but their vision remained worse than 20/400. Ninety-two percent of patients had persistent dyschromatopsia. Visual recovery is expected by 6 months, but more rapid recovery after IV methylprednisone is common within the first month. Other visual functions may continue to improve over the next two years, such as contrast sensitivity, color vision, and visual field. Bibliography: Beck, Roy W., et al. “A randomized, controlled trial of corticosteroids in the treatment of acute optic neuritis.” The New England Journal of Medicine, vol. 326(no. 9), Feb 27, 1992. Beck, Roy W., et al. “Multiple sclerosis risk after optic neuritis: final optic neuritis treatment trial followup.” Arch Neurol, vol. 65(no. 6), June 2008. Galetta, Steven L., et al. “Acute optic neuritis: unmet clinical needs and model for new therapies.” Neurol Neuroimmunol Neuroinflamm, 2(4): e135, August, 2015. Slamovitis, TL, et al. “Visual recovery in patients with optic neuritis and visual loss to no light perception.” Am J Ophthamol, 111(2): 209-14. Feb 15, 1991. Wingerchuck, Dean M., MD, FRCP(C), et al. “The clinical course of neuromyelitis optica (Devic’s syndrome).” Neurology, vol. 53, no. 5, 1107, September 1, 1999. More references available upon request VI CONCLUSION No light perception vision is an uncommon but possible presentation in optic neuritis secondary to Multiple Sclerosis. All other possible differentials should be considered and ruled out with an atypical presentation of presumed optic neuritis. If MRI of the brain does not show enhancement of the optic nerve, dedicated MRI of the orbit may be needed to help make the diagnosis. In a patient with recurrent episodes of optic neuritis and severe visual impairment, Neuromyelitis Optica should be considered and investigated through additional lab testing. Research suggests a good prognosis for visual recovery in most cases. The patients who maintain NLP vision after optic neuritis must be educated on the need to be more aware of the visual field on the side of the affected eye, especially when driving. Some monocular patients may not feel comfortable driving in certain conditions or may discontinue driving altogether. Safety glasses should be strongly recommended to protect the unaffected eye. These patients benefit from timely communication among a team of inter-disciplinary providers including their eye care specialist, neurologist, primary care physician, and possibly occupational therapist/physical therapist.