* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download CNS Infections
Gastroenteritis wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Onchocerciasis wikipedia , lookup
Neonatal infection wikipedia , lookup
Marburg virus disease wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Oesophagostomum wikipedia , lookup
West Nile fever wikipedia , lookup
Leptospirosis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Meningococcal disease wikipedia , lookup
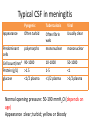
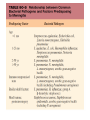
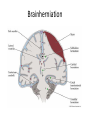
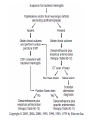
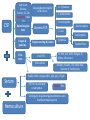
Central nervous system infection Dr. Koukeo Phommasone CNS infection • • • • Meningitis Encephalitis Myelitis Focal Central Nervous System Syndrome – Brain abscess – Subdural empyema – Epidural abscess ¦¾À¹©¢º¤ CNS infection • Virus: EV, HSV, VZV, CMV, Mumps, JE, Dengue • Bacteria: HIB, S. pneumoniae, N. meningitidis, S. suis, M. tuberculosis… • Fungi: Cryptococcus • Protozoa • Parasites: Angiostrongylus cantonensis, … ຶ່ຶ ງທ ຶ່ີ ຶ່ບແມ ຶ່ີ ັ້ ອທ ນອກນັັ້ນຍັງມ ຶ່ ນພະຍາດຊ ີ ສາຍເຫດຈານວນໜ ຶ ມເຊ ຶ່ ັ ນ: Neoplastic diceases, ພາໃຫ ັ້ ີມອາການຄ CNS infection ເຊ intracranial tumors and cysts, medications, collagen vascular disorders, and other systemic illnesses º¾¡¾¦½Á©¤¢º¤²ະຍາດ • • • • • headache; photophobia; stiff neck; Kernig’s and Brudzinski’s signs +; opisthotonus Ä¢É (fever) À¥ñ®¹ö¸ (headache) ¦½ªò®Ò©ó (altered mental status) Focal neurologicdeficits Meningismus ຶ່ີ ເວ ັ້ າມາຂ ອາການທ ັ້ າງເທ ຶ່ ນ nonspecific, ມັນຂ ີ ງນ ີ ັ້ ແມ ຶ ັ້ ນ ກັບ pathogenesis, infectious agents and area of CNS involvement and age of the patient Meningitis vs Encephalitis Meningitis • • • • Fever Headache Meningismus Altered mental status Encephalitis • Fever • Headache • Altered mental status Mental status changes early in the disease course, prior to coma Both share many • Focal or diffuse features neurologicsigns (seizures and hemiparesis) Meningoencephalitis Definitions of WHO Bacterial meningitis • Clinical description – Acute onset of fever (usually >38.5 rectal, >38 axillary) – Headache and – One of the following signs: neck stiffness, altered consciousness or other meningeal signs Acute encephalitis syndrome (AES) • Clinical case definition – Acute onset of fever and at least one of: • Change in mental status (including symptoms such as confusion, disorientation, coma, inability to talk • New onset of seizure ( including simple febrile seizure) Meningitis and encephalitis • Life-threatening disease • Signs and symptoms are not specific • Physical examination may not be sufficient to accurately identify patient with meningitis, especially in infants and young children • Lumbar puncture result may be difficult to distinguish bacterial meningitis from viral meningitis • Suspected bacterial meningitis is a medical emergency and need empirical antimicrobial treatment without delay • Physicians who prescribe the initial dose of antibiotics should be aware of guidelines for antibiotics and adjunctive steroids Focal neurological signs, papilloedema, falling level of consciousness with abscess) falling pulse, rising BP and/or vomiting LP contraindication • Mass in the brain (eg. Brain tumor or causing raised intracranial pressure • Skin or soft tissue sepsis at the proposed LP site • Severe coagulopathy or severe thrombocytopenia Risk for either mass or raised ICP recent head injury a known immune system problem localizing neurological signs evidence on examination ofraised ICP MRI or CT brain prior to LP Brainherniation Typical CSF in meningitis Pyogenic Often turbid Tuberculosis polymorphs mononuclear mononuclear Cell count/mm3 90-1000 Protein (g/L) >1.5 10-1000 1-5 50-1000 <1 glucose <1/2 plasma >1/2 plasma Appearance Predominant cells <1/2 plasma Often fibrin web Viral Usually clear Normal opening pressure: 50-190 mmH2O (depends on age) Appearance :clear; turbid; yellow or bloody LP • Cell count: 0-5/mm3 in children and adult, maybe up to 32/mm3 (mean of 8-9/mm3) in neonates – False positive eleviation of CSF white bloodcell counts : traumatic LP, intracerebral or subarchnoidhemorrage LP done at Mahosot • Physicians decide to do Lumbar Puncture according to clinical symptoms/signs • No contraindication for LP • Informed written consent LP doneatMahosot • Lab staff assist the physician for LP • CSF drop on agar plate, • CSF collection in 3 tubes: • adult: 8ml • children: 3ml • Blood collection: (haemoculture, glucose and serology) CSF Cell count, Glucose, Protein, GS, ZN, Auramine, India ink Bacteriological tests Classical bacteriological &TB culture H. influenzae S. pneumoniae N. meningitidis Bacteria PCR Murine typhus S. suis Scrub typhus Fungus & parasites Viral tests Cryptococcal Ag & culture Viral PCR Viral culture Rickettsia Spotted fever EV, HSV, VZV, CMV, Dengue, JE, Nipha, Influenxa A Mumps, measles, TBE, West Nile, Inluenza B, Panflavivirus Panbio ELISA: Dengue (NS1, IgM, IgG), JE IgM Serum RDT for murine and scrub typhus Malaria film Serology for Angiostrongyluscantonensis and Gnathostomaspinigerum Hemoculture • Total included patients 2003-2009: 840 patients • Few bacteria isolated from CSF: 6% (67% AB before LP) • virus positive samples : 15.3% Viral causes Tested POS % EV PCR 345 CSF 7 2% HSV PCR 344 CSF 3 0.9% VZV PCR 385 CSF 2 0.5% CMV PCR 243 CSF 4 1.6% Mumps PCR 344 CSF 2 0.9% JEV PCR 344 CSF 2 0.9% JE culture 200 CSF 1 0.5% JEV IgM 700 CSF 48 6.8% Dengue 344 sera 4 (3D1,1D4) 1.2% Treatment of meningitis Mahosot Microbiology Review • Antibiotic recommendation – Ceftriaxone 80-100 mg/kg/day divided into 2 daily doses (50kg adult 2g IV every 12 h) – Or in neonates: • Aged 0-7 days cefotaxime100-150 mg/kg/day (dose interval every 8-12h) or aged 8-28 days 150-200 mg/kg/day IV (dose interval 6-8h) Treatment of meningitis Mahosot Microbiology Review • And if Listeria is suspected (usually in infant < 1 month old) give ampicillin Age 0-7 days 8-28 days Daily dose IV 150 mg/kg/day 200 mg/kg/day 300 mg/kg/day 12 g/day Dose interval Every 8h Every 6-8h <15 y Every 6h >15 y Every 4 h Treatment of meningitis Mahosot Microbiology Review • If ceftriaxone is not available give chloramphenicol Age 0-7 days 8-28 days <15 y >15 y Daily dose IV 25 mg/kg/day 50 kg/day 75-100mg/kg/day 4-6g/day Dose interval 24h 12-24h 6h 6h If suspected rickettsial disease add in: oral doxycycline 4 mg/kg stat followed by 2mg/kg every 12h for 1 week. In adult doxycycline 200 mg loading dose followed by 100 mg every 12h Adjunctive treatment with dexamethasone • Neurological sequelae are common in survivors of meningitis (hearing loss, cognitive impairement, developmental delay) • Adjuvant therapy with dexamethasone reduces the mortality and neurological sequelae among adults with bacterial meningitis in the developed world • There have been few clinical trials in Asian patients – unclear whether should be given ? Systemic steroids (dexamethasone, 10 mg IV) are important adjunctive treatment for patients with suspected bacterial meningitis and should be given with the first dose of antibiotics and continued every 6 h for 4 days (but unclear whether beneficial in developing countries) Prevention • Viral meningitis: Immunoprophylaxis - JEV • Bacterialmeningitis:Vaccine available for Hib, 7 serotype of S. pneumoniae and N. meningitidis group A, C, Y and W135 • Chemoprophylaxis for bacterial meningitis patients/contacts – Haemophulus influenzae • Eradication of nasopharyngeal colonization of Hib – Rifampicin 20 mg/kg daily for 4 days (2 days of rifampicin is efficacious as 4 days’ treatment – Ampicillin and chloramphenicol, unlike ceftriaxone and cefotaxime, do not effectively eliminate nasopharyngeal colonization – Rifampicin is Not recommended in pregnant women • Chemoprophylaxis is not currently recommended for daycare contacts 2 y old or older unless two or more cases occur in the daycare center within 60 days-period • For children <2 y, the CDC recommends prophylaxis for daycare contacts – Neisseria meningitidis • Chemoprophylaxis: – Ceftriaxone IM 250 mg in adult and 125 mg in children – Ciprofloxacin 500 mg oral in adult single dose – in adults, rifampin 600 mg bid for 2 days. In children 1 month or older 10 mg/Kg and infant youngerthan 1 month 5m/kg • Chymoprophylaxis is recommended for household contacts, daycare center members, any person exposed to the patient’s oral secretion • Chemoprophylaxis is not recommended for school, work or transport contacts • High dose penicillin or chloramphenicol do not reliably eradicate meningococci from the nasopharynx of colonized patients – S. pneumoniae: the risk of secondary pneumococcal disease in contacts of infected patient has not been defined – Streptococcus agalactiae • All pregnant should be screenat 35-37 weeks gestation for anogenital colonization with group B streptococci Microbiology Laboratory Mahosot Hospital Thank you for your attention