* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download RHINITIS, SINUSITIS
Survey
Document related concepts
Transcript
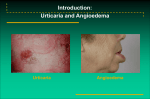
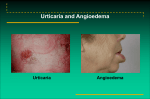
Urticaria and Angioedema 101 Scot Laurie, MD Allergy and Asthma Center at NorthPark Assistant professor, University of Texas Southwestern Medical Center Case Presentation Jim S. is a 45 y/o who presented for evaluation of his urticaria. He has been suffering with hives for the past 4 months. He is unable to tell what triggers his hives. His hives are generalized and an individual hive will last a few hours; he has had several episodes of lip swelling as well. He might have had a similar episode 10 years ago and his doctor told him he was allergic to penicillin Case presentation He has visited his primary care physician who suggested he take Claritin He returned when his hives persisted and the doctor told him that he was allergic to something and suggested an allergy evaluation. Case presentation Past medical history – Hypothyroidism Medications – levothyroxine – Ibuprofen prn Review of systems – Occasional headaches; otherwise negative Physical exam Case presentation How would his hives be classified? What is causing his hives? Are his medical conditions or medications contributing to his hives? What tests should be done to evaluate his hives? How are his hives best treated? URTICARIA & ANGIOEDEMA DESCRIPTION – Urticaria Raised, erythematous, blanching Pruritic Lesions well-circumscribed; typically coalesce – Angioedema Subcutaneous swelling Predilection to areas of loose connective tissue, such as the face or mucus membranes involving the lips or the tongue Urticaria or “Hives” Urticaria and Angioedema Clinical features: Urticaria – Repeated occurrence of short-lived cutaneous wheals accompanied by erythema and pruritus Wheals range in size from a few millimeters to several centimeters Wheals may coalesce to form larger lesions Individual wheals typically last less than 24 hours Urticaria may occur anywhere on the skin – Mucus membrane involvement is rare Lesions should resolve without any residual marking Urticaria and Angioedema Clinical features: Angioedema – Approximately 50% of patients with chronic urticaria have angioedema as well – Episodes of short-lived deep dermal and subcutaneous or submucosal edema – Like urticaria, symptoms generally last less than 24 hours Larger swellings may take longer to resolve – Pruritus does not consistently accompany angioedema, and may not occur at all. Mediators of hives and swelling Source Mast cells (cutaneous) Factor Histamine Prostaglandin D2 Leukotrienes C and D Platelet Activating Factor Complement system Hageman factordependent pathway Mononuclear cells Anaphylatoxins C3a, C4a, C5a: histamine Bradykinin Histamine-releasing factors, chemokines Urticaria and Angioedema Classification – Acute: < 6 weeks Allergic Infectious Idiopathic – Recurrent acute – Chronic: > 6 weeks Idiopathic Autoimmune Physical URTICARIA CLASSIFICATION Acute: < 6 weeks – Affects as many as 10-20% of the population at some point in their lives – Etiology frequently identified Food allergy Drug allergy Stings/venoms Infection – Viral infection leading cause of urticaria in children Urticaria Classification Recurrent acute (intermittent) – Episodes of urticaria lasting days or weeks with intervals of days, weeks, or months in between episodes Chronic: > 6 weeks – Idiopathic – Physical urticarias URTICARIA ETIOLOGIES Common – Idiopathic – Medications – Stings – Foods – Infection – Physical urticarias Rare Causes – Neoplasms – Collagen vascular disease – Endocrine – Urticarial vasculitis Urticaria etiologies Urticaria is rarely, if ever the presenting or sole symptom of an underlying disease A complete Review of Systems will suggest or identify any systemic disease in which the urticaria occurs URTICARIA ETIOLOGIES Medications – Any drug has the potential to elicit an allergic reaction Antibiotics in general, and penicillins specifically, are most often indicated Aspirin/NSAID’s Considered second most common cause of acute drug allergic reactions Frequently exacerbate chronic urticaria and angioedema URTICARIA ETIOLOGIES Foods Important cause of acute urticaria – Primary allergens are peanuts, tree nuts, shellfish, fish, eggs, milk Chronic urticaria typically unrelated to food allergy Infection Common cause of acute urticaria – Viral infection most common cause in children – Episodes are self-limited Rare cause of chronic urticaria INSECT BITES & STINGS Generalized urticaria/angioedema – Indicates systemic reaction – Requires allergist evaluation for possible immunotherapy Urticaria in children does not require immunotherapy – Hymenoptera bees, wasps, yellow jackets, hornets Fire ants URTICARIA ETIOLOGIES Aeroallergens – Rarely, if ever, cause urticaria Animals may cause contact urticaria Inhaled latex may result in systemic allergic reaction ? seasonal pollens Contact Urticaria – Nonimmunologic cinnamic acid, benzoic acid Diagnosed by open patch test – Immunologic (Allergic) Latex, fruits, vegetables Diagnosed by applying material to eczematous or scratched skin Urticaria etiologies Endocrine/autoimmune – Thyroid disease Urticaria and angioedema has been associated with hypo- and hyperthyroidism Possible association with the presence of thyroid autoantibodies (antithyroid peroxidase and antithyroglobulin) – Thyroid autoimmunity has been demonstrated in 12-26 % of subjects with chronic urticaria – Thyroid autoimmunity occurs in 3-6% of the population URTICARIA ETIOLOGIES Chronic urticaria – Most common etiology is idiopathic – 30-60% of patients exhibit a wheal-and-flare with autologous serum skin testing Thought to be due to a complement-activating, histamine-releasing autoantibody (IgG) against the αchain of the high-affinity IgE receptor (FcεRI) – These autoantibodies are able to trigger mast cell or basophil histamine release through direct crosslinking of adjacent receptors – Can cause histamine release in healthy subjects Treatment implications: urticaria may be more difficult to control Plasma of patients with chronic urticaria shows signs of thrombin generation, and its intradermal injection causes wheal-and-flare reactions more frequently than autologous serum J Allergy Clin Immunol 2006;117:1113-7. Chronic urticaria: etiologies 51/96 (53%) patients had positive ASST 61/71 (86%) patients had positive APST Prothrombin fragment F(1+2) (marker of thrombin generation) was higher in patients than in controls – Levels directly related to severity of urticaria Chronic urticaria: etiologies Conclusions – Suggests role of the activation of the extrinsic coagulation pathway with thrombin generation in chronic urticaria Thrombin increases vascular permeability (edema) May trigger mast cell degranulation – Possible therapeutic use of anticoagulants (heparin/warfarin) Natural history: Chronic Urticaria Up to 50% patients resolve within 3-12 months Another 20% of patients resolve in 12-36 months or 36-60 months Up to 1.5% of patients persist for 20+ years 50% of patients with chronic urticaria will have recurrences Physical urticarias tend to last longer, as do more severe forms of chronic urticaria PHYSICAL URTICARIAS Symptomatic dermographism Cholinergic Delayed pressure Cold Aquagenic Solar Vibratory adrenergic PHYSICAL URTICARIAS Dermographism – Very common- affects 2-5% of population Small fraction of these patients will seek treatment – Stroking of the skin results in linear wheals which may persist as long as 30 minutes patients may complain of generalized pruritus or “skin crawling” PHYSICAL URTICARIAS Cholinergic urticaria – Likely the most common of the physical urticarias- 30% of the physical urticarias – Occurs primarily in teenagers and young adults – Pruritic, small macules and papules occur in response to heat, exercise, or emotional stress May occur with wheezing May occur without visible skin lesions (cholinergic pruritus) Physical urticarias Cold urticaria – Characterized by the rapid onset of pruritus, erythema, and swelling after exposure to a cold stimulus Holding cold objects: hand swelling Eating cold items: lip swelling/ oropharyngeal edema Swimming, with total body immersion, can result in massive mediator release, resulting in hypotension – Risk factor: oral symptoms with ingestion of cold items URTICARIA EVALUATION Acute urticaria and angioedema – History to ascertain for possible triggers: food, drug, sting, infection – Exam to confirm diagnosis – May refer to board-certified allergist for select skin testing/challenge tests to suspected agents Urticaria evaluation Chronic urticaria – History and physical exam Confirm diagnosis of urticaria/angioedema – Laboratory studies Usually none required – No relationship has been found between the number of identified diagnoses and the number of laboratory tests performed Consider thyroid evaluation (TSH, thyroid autoantibodies) in patients who fail initial therapy If urticarial vasculitis suspected: – ANA, complement levels – Referral for skin biopsy Skin biopsy Indications – Individual urticarial lesion persists for >48 hours – Urticaria are less than moderately pruritic – Lack of significant response to “maximum” doses of antihistamines URTICARIA MANAGEMENT Goals – control symptoms & keep patient comfortable search for and treat underlying etiologies exclude serious diseases Avoidance – causative factor if identified – NSAID’s & ASA – excessive heat Supportive therapy – Reassurance – Patient education is most important Urticaria management Chronic idiopathic urticaria – Because there is no one specific causative agent that can be withdrawn, the hives cannot be “cured”. – Treatment is considered palliative, until the condition resolves on its own Goal is to maintain a patient’s quality of life, despite condition INITIAL URTICARIA PHARMACOTHERAPY Antihistamines: H1 receptor antagonists – Second generation (“Non-sedating”) equal in efficacy to first generation without as many side effects – cetirizine, levocetirizine, desloratadine, fexofenadine, loratadine – First generation Generally administered on a daily basis for preventative therapy – hydroxyzine, diphenhydramine, chlorpheniramine, etc. – dose at qhs initially to reduce daytime somnolence – May be used on a prn basis SECONDARY URTICARIA PHARMACOTHERAPY H2 antagonists – 15% of histamine receptors in the skin are H2 – May use in combination with H1 antagonists – Inhibits metabolism of hydroxyzine, resulting in higher plasma concentration of hydroxyzine Doxepin – Very potent H1 antagonist – H2 antagonist as well – May be very sedating- generally use at night Leukotriene antagonists – Zafirlukast and montelukast superior to placebo in the treatment of chronic urticaria Urticaria management Antihistamine “cocktail” – Begin with 2nd generation antihistamine once a day; if response unsatisfactory, – Double the dose (either split-dose twice daily, or full dose once daily); if response unsatisfactory, ADD – Doxepin 10-50 qhs (titrate over time to reduce sedation) Levocetirizine/cetirizine>fexofenadine>desloratadine/ loratadine SECONDARY URTICARIA PHARMACOTHERAPY Oral corticosteroids – Role of systemic steroids in the treatment of chronic urticaria is limited – Short-term use in special situations (e.g. control of symptoms prior to an important event.) – Prolonged treatment complicated by severe side effects along with worsening of urticaria upon withdrawal Alternative agents for refractory chronic urticaria Drug Leukotriene modifiers Dapsone Sulfasalazine Hydroxychloroquine Colchicine Calcineurin inhibitors Mycophenolate Omalizumab Level of evidence Ib IIb III Ib III Ib IIb III SECONDARY URTICARIA PHARMACOTHERAPY Immunomodulatory agents – Limited studies demonstrate efficacy of cyclosporine in improving urticaria along with decreasing dependence on prednisone. Suppressive effect on basophil and mast cell activation Requires monitoring of a patient’s blood pressure and renal function Cyclosporine Patients with chronic, severe urticaria with positive autologous skin test – 3-month course of treatment resulted in 80% totally or almost clearing their symptoms – Upon medication withdrawal at 3 months: 1/3 remained clear 1/3 relapsed mildly 1/3 relapsed to baseline Br J Dermatol 2000;143:368. Urticaria and angioedema Pearls – Urticaria and angioedema frequently is not an allergic condition – Urticaria does not respond to topical treatment – Urticaria in the setting of antibiotics use might be due to the infection, rather than the antibiotic – Almost all urticaria is responsive to antihistamines; if your initial dose does not work, use more – When all else fails, refer to your favorite fellowship-trained allergy and immunology specialist – Treatment references: N Engl J Med 2002;346:175-9 or Allergy and Asthma Proc 2004;25:143-149. I Need an Allergist!!