* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Joint Arthroplasty THR & TKR
Survey
Document related concepts
Transcript
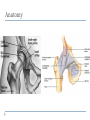
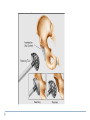
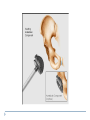
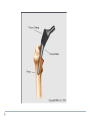
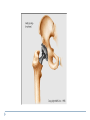
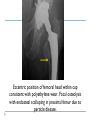
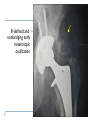
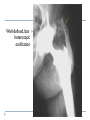
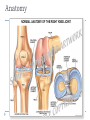
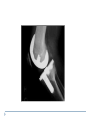
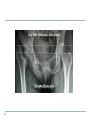
Joint Arthroplasty THR & TKR THR is one of the most successful orthopedic procedures performed today . It is estimated that over 300,000 total hip arthroplasties are performed each year in the United States alone . THA can relieve pain, can restore function, and can improve quality of life . Anatomy Definition THA is a procedure whereby the diseased articular surfaces are replaced with synthetic materials . THA is an elective procedure and should be considered as an option among other alternatives . the articular surfaces of both the acetabulum and femur are replaced . . . . Indication If there is Hip pain , that has been failed to be treated conservatively and cause a significant decrease in the activities of daily living . If there were No pain , Patients with significant deformity and limitation of motion may be candidates . Indications Osteoarthritis Rheumatoid arthritis Avascular necrosis Traumatic arthritis Certain hip fractures Benign and malignant bone tumors The aims are pain relief and improvement in hip function Contraindication Active infection (local or systemic) Preexisting significant medical problems (eg, recent myocardial infarction, unstable angina, heart failure, or severe anemia) Skeletal immaturity Paraplegia or quadriplegia Contraindication Permanent or irreversible muscle weakness , nerves or blood vessels that could endanger limbs. Joint disease which may require alternative reconstruction (osteotomy) Allergy to implants, particularly to metals (e.g.: cobalt, chromium, nickel, etc.) Pregnancy Contraindication Age itself is not a contraindication to proceeding with replacement. Because the joint replacement can fail with time, the revision rate is lower if surgery is delayed as long as possible. On the other hand, patients who elect surgery at a better level of functional status have better functional outcomes Complications INTRAOPERATIVE COMPLICATION 1. Perforation or fracture of the femur or acetabulum 2. Nerve and vascular injury , Injury to the sciatic nerve is most common vascular injuries that may be recognized postoperatively are arteriovenous fistulas, arterial thromboses, and pseudoaneurysms . Complications POSTOPERATIVE COMPLICATIONS 1. Thromboembolic disease , Without thromboprophylaxis, perioperative mortality from pulmonary embolus (PE) occurs in 2 to 3 percent. With thromboprophylaxis, there is a 0.1 percent rate of post-discharge fatal PE at 90 days postoperatively. 2. Infection , less that 1 % 3. Postop Dislocation , overall incidence of dislocation can reach 2% Complications 1. 2. 3. Osteolysis and wear Is the most common long-term complication seen in young and physical active pt the most frequent reason for implant failure. The process begins as wear particles from the hip implant are phagocytosed by macrophages that become activated. These activated macrophages release osteolytic factors and stimulate osteoclasts to dissolve surrounding bone Eccentric position of femoral head within cup consistent with polyethylene wear .Focal osteolysis with endosteal scalloping in proximal femur due to particle disease. Complications Aseptic loosening 1. The commonest cause of long term faliure 2. 10-20% after 10 years Heterotropic bone formation 1. In 20% after 5 years 2. is a process by which the soft tissues around the hip become ossified 3. (NSAIDs) and external beam radiation have been used most successfully in preventing HO . Ill-defined and nonbridging early heterotopic ossification Well-defined, late heterotopic ossification Total Knee replacement As of 2010, over 600,000 total knee replacements were being performed annually in the United States and were increasingly common Anatomy Definition is a surgical procedure whereby the diseased knee joint is replaced with artificial material. The end of the femur bone is removed and replaced with a metal shell. The end of the lower tibia is also removed and replaced with a channeled plastic piece with a metal stem. Depending on the condition of the patella, a plastic "button" may also be added under its surface. Indication 1. 2. 3. 4. Most commonly due to OA Pain limiting daily activities limited function or mobility Failure of other methods resting, weight loss, physical therapy, a cane or other walking aid, medications, braces and surgery Deformity Indication Total knee arthroplasty is performed in patients of all ages (except the skeletally immature) and better outcome were found in those less than 55 Patients should understand the risks as well as the benefits before making these decisions. Contraindications 1. 2. 3. 4. 5. Absolute contraindications: Active infection in the knee or anywhere in the body Extensor mechanism dysfunction Severe vascular disease Recurvatum deformity secondary to muscular weakness The presence of a well-functioning knee arthrodesis Contraindications 1. 2. 3. 4. 5. Relative contraindications: Medical conditions that preclude safe anesthesia and the demands of surgery and rehabilitation. Skin conditions within the field of surgery (e.g., psoriasis) Past history of osteomyelitis around the knee Neuropathic joint Obesity Complications 1. 2. 3. Thromboembolism without any prophylaxis has been reported at 40-88% Infection Patellofemoral complications Patellofemoral instability, patellar fracture, patellar component failure, and extensor mechanism tendon rupture Common reasons for reoperation Complications 4. 5. Neurovascular complications Arterial thrombosis following total knee replacement is a rare (ie, 0.03-0.17%) but devastating. Peroneal nerve palsy is the commonly reported nerve palsy Periprosthetic fractures Supracondylar fractures of the femur are not common following total knee replacement (ie, 0.21%) Complications 6. 7. Aseptic loosening Leads to the ultimate failure of the prosthesis and occurs at an approximate rate of 5-10% of patients at 10-15 years Arthrofibrosis Excessive scar tissue causing restriction of knee movement Occurs in less than 1% Postop & Follow up Physical therapy is an extremely important part of rehabilitation Patients can begin physical therapy 48 hours after surgery Some degree of pain, discomfort, and stiffness can be expected during the early days of physical therapy. Knee immobilizers are used in order to stabilize the knee while undergoing physical therapy, walking, and sleeping. They may be removed under the guidance of the therapist for various portions of physical therapy. Postop & Follow up Continuous passive motion (CPM) machine can help speed the recovery process. The CPM machine is first attached to the operated leg. The machine then constantly moves the knee through various degrees of range of motion for hours while the patient relaxes. Patients will start walking using a walker and crutches. Eventually, patients will learn to walk up and down stairs and grades. A number of home exercises are given to strengthen thigh and calf muscles. Postop & Follow up Most patients seem satisfied with their knee replacements. The majority of patients are able to return to lowimpact sporting activity. Long-term studies confirm satisfactory functional scores and show a 91-96% prosthesis survival rate at 14-15 years of follow-up. Cementless designs do not have the same length of follow-up, but studies at 10-12 years report a 95% prosthesis survival rate. Excision Arthroplasty - intractable joint infection - when previous operations have failed - the joint has been irremediably destroyed , EXCISION ARTHROPLASTY is the solution Excision Arthroplasty to excise the articular ends of the bone forming the joint , creating where movement can occur femoral head & neck are excised leaving a false articulation ( pseudoarthrosis ) between the upper end of the femur & the acetabulum The joint is obviously unstable , but because of local fibrosis & the effect of powerful surrounding muscles , the pt can still take weight on the side & can walk about though with marked limp Thank You