* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Controversy surrounding psychiatry wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Postpartum depression wikipedia , lookup
Major depressive disorder wikipedia , lookup
Alzheimer's disease wikipedia , lookup
Biology of depression wikipedia , lookup
Dementia praecox wikipedia , lookup
Behavioral theories of depression wikipedia , lookup
Dementia with Lewy bodies wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
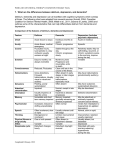
Master’s Advanced Curriculum (MAC) Project Field Instructor Training Acknowledgement: The development of this PowerPoint was made possible through a Gero Innovations Grant from the CSWE GeroEd Center’s Maser’s Advanced Curriculum (MAC) Project and the John A. Hartford Foundation. Learning Objectives At the end of this training participants will be able to: Identify two common changes related to the aging process that are part of normal aging. Identify 2 components of the presentation of depression in older adults. Identify 3 ways in which the presentation of dementia differs form the presentation of depression in older adults. Identify the role of function in the assessment of older adults. Effective Clinical Work with Older Adults: The Pathway to Our Future Introduction Social attitudes Regarding Older Adults Successful aging Physiology of normal aging Assessment of Problem Areas Functionality Cognition Ageism • Systematic stereotyping and discrimination against people because they are old • Result of a lack of information about older adults Aging Well Bad things in life don’t doom us Good people at any age facilitate an enjoyable old age Aging Well Keys to healing Gratitude Forgiveness Letting others in Aging Well A good marriage at age 50 predicted positive aging at 80 Alcohol abuse predicts unsuccessful aging Play, create, make younger friends Aging Well Health concerns okay if one feels well Motivations Generativity Keeping the meaning Normal Age-Related Changes Mobility Decrease in muscle mass Loss of bone strength Strategy Regular EXERCISE Autonomic Nervous System Impaired response to extremely hot and cold environmental temperatures Altered sleeping pattern Strategy Careful attention to weather conditions Good sleep hygiene Sensory Function Changes in vision Decrease in hearing taste smell The Brain Longer time to process new, complex information Difficulty remembering newly acquired information such as names The Brain Higher order thinking improves Intelligence based on experience and education improves The Brain Strategy Active & inquisitive lifestyle with stimulating environments Memory improvement strategies Regular EXERCISE Sexual Function Age-related changes do not diminish enjoyment or desire Incidence of HIV/AIDs infections growing fastest among older adult age group Assessment of Older Adults Function Cognition Function FUNCTION is the lens through which all assessments must be filtered Function Activities of Daily Living Self Care Eating Dressing and grooming Bathing Toileting Ambulation Transferring Function Instrumental Activities of Daily Living Meal preparation Laundry Shopping Arranging for transportation Money management Use of the telephone Cognition Domains of cognition Attention Orientation Language comprehension Expressive language Visual-spatial Memory Calculations Abstract reasoning Judgment Common problems that are NOT normal age related changes DEPRESSION DEMENTIA DELIRIUM Depression Depression is NOT a normal part of aging Depression in the elderly is quite treatable Depression in Older Adults Somatic concerns more prominent Focus on bowel or urinary dysfunction Peculiar tastes Dizziness Nonspecific aches and pains that do not align with any physical diagnosis Unshakeable belief of being ill Depression in Older Adults Dysphoria less prominent Older adults may be unaware or deny feelings of sadness, hopelessness or guilt Depression in Older Adults Depression can look like dementia “pseudo dementia” Inability to concentrate may be expressed as “failure” of memory Many complaints about loss of memory Depression in Older Adults High number of “I don’t know” responses Able to perform tasks Depression in Older Adults Medications Assess for depression as side effect to current medications Antidepressant medications Counseling Social supports Environmental modifications Dementia Global decline of mental functions in a conscious individual sufficient to interfere with the person’s daily functioning Loss or recent memory is the hallmark symptom Dementia Alzheimer’s disease is most common form Multi-infarct or vascular dementia caused by many small strokes and is second most common form Dementia Early symptoms • Forgetfulness • Confusion and disorientation • Impaired judgment • Personality changes Diagnosis includes ruling out all treatable conditions and includes physician workup and evaluation Dementia Concerns include • Proper diagnosis and treatment • Future planning of legal and financial concerns • Caregiver arrangements • Safety and supervision • Behavior management Delirium Sudden, REVERSIBLE change in mental status Infection or illness Medications Delirium is A MEDICAL EMERGENCY Medical treatment should be sought immediately Delirium Disturbance in consciousness with • reduced ability to focus, sustain or shift attention • change in cognition • agitation • perceptual disturbance that occurs over short periods of time and tends to fluctuate over the course of the day Sudden onset The Distinction Between Depressive Dysfunction and Alzheimer’s Depressive Dementia Alzheimer’s Clinical Course Onset dated only within Onset can be dated with some precision. Symptoms of relatively short duration. History of previous psychiatric illness of similar kind common. Relatively rapid progression of symptoms after onset. Family usually very aware of the dysfunction and its severity. broad limits. Symptoms of longer duration before medical help sought. Previous psychiatric history unusual. Slow progression of symptoms throughout course. Family usually unaware of the dysfunction and its severity. Clinical Features Depressive Dementia Alzheimer’s Patient complains much of cognitive loss. Patient complains little of Patient makes detailed complaints. Complaints usually vague. Patient emphasizes disability. Patient conceals disability. Patient highlights failure. Patient delights in Patient makes little effort to perform even simple tasks. cognitive loss. accomplishment, however trivial. Patient struggles to perform tasks. Patient does not try to keep up. Patient usually communicates strong sense of distress. Patient relies on notes, There is pervasive affective change. Patient often appears Nocturnal accentuation of dysfunction uncommon. diaries and calendar to keep up. unconcerned. Features of Cognitive Dysfunction Depressive Dementia Alzheimer’s “Near miss” and wrong answers frequent. Memory gaps for specific periods of events common. Memory gaps for specific periods unusual. Marked variability in performing tasks of similar difficulty. Consistently poor performance on tasks of similar difficulty. “Don’t know” answers typical. Summary Our attitudes, beliefs and knowledge base will guide how we assess older adults Evidence guides the comprehensive geriatric assessment Bio Psycho Social Summary Understanding of normal and successful aging guides assessment to help us recognize when problems exist Diagnosis is the first step to securing treatment and remedy Treatment is available for common geriatric syndromes including the 3 “Ds” Depression, Dementia and Delirium Summary Functional status will guide needed services and interventions to a far greater degree than diagnosis or age Assessing functional status is crucial for helping older adults maintain independence and the guide for viable planning Summary Markers for successful aging can guide psychotherapeutic interventions Provide guidelines for Reminiscence, Cognitive and other reflective therapies with older adults For More Information Services and Programs • Huntington Senior Care Network, Resource Center 837 S. Fair Oaks Ave Suite 100 Pasadena, Ca 91105 (626) 397-3110 www.seniorcarenetwork.com For More Information Alzheimer’s Association 5900 Wilshire Blvd # 1100 Los Angeles, CA 90036 (323) 938-3379 www.alz.org For More Information Los Angeles Caregiver Resource Center (800) 540-4442 www.losangelescrc.org References Mezey, M.D. (Ed.). (2001). The Encyclopedia of Elder Care. (26). New York, NY: Springer Publications. Vaillant, G.E. (2002). Aging Well. New York: Little Brown & Company. Carstensen, L. L., Edelstein, B.A. & Dornbrand, L. (Eds.). (1996). The practical handbook of clinical gerontology. Thousand Oaks, CA: Sage Publications. Fitten,J., & Brothers, L. (1986, April). The Sepulveda GRECC METHOD No 10, Depression. Geriatric Medicine Today, 5(4). Young, R.C, Manley, M.W., & Alexopoulos, G.S. (1985). “I Don’t Know” Responses in Elderly Depressives and in Dementia. Journal of the American Geriatrics Society, 33(4), 253–257.