* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download document
Hemolytic-uremic syndrome wikipedia , lookup
Blood transfusion wikipedia , lookup
Schmerber v. California wikipedia , lookup
Autotransfusion wikipedia , lookup
Blood donation wikipedia , lookup
Jehovah's Witnesses and blood transfusions wikipedia , lookup
Hemorheology wikipedia , lookup
Men who have sex with men blood donor controversy wikipedia , lookup
ABO blood group system wikipedia , lookup
Biology 212
Anatomy & Physiology I
Dr. Thompson
Blood
Biology 212
Anatomy & Physiology I
Dr. Thompson
Blood
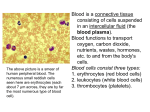
Blood:
Volume:
Components:
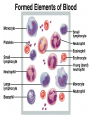
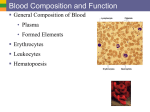
Formed Elements:
Plasma:
pH:
Buffered to remain stable
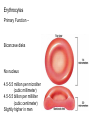
Erythrocytes
Primary Function –
Biconcave disks
No nucleus
4.5-5.5 million per microliter
(cubic millimeter)
4.5-5.5 billion per milliliter
(cubic centimeter)
Slightly higher in men
Hemoglobin
Each molecule:
4 large Globin proteins
Each surrounding an ironcontaining Heme Group
Oxygen
Erythrocyte formation =
Occurs
Developing erythrocytes =
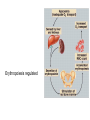
Erythropoiesis regulated
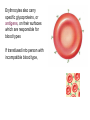
Erythrocytes also carry
specific glycoproteins, or
antigens, on their surfaces
which are responsible for
blood types
If transfused into person with
incompatible blood type,
Erythrocytes normally survive
Trapped and destroyed
Iron
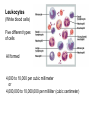
Leukocytes
(White blood cells)
Five different types
of cells
All formed
4,000 to 10,000 per cubic millimeter
or
4,000,000 to 10,000,000 per milliliter (cubic centimeter)
Each type has
specific functions,
but in general:
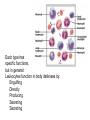
Leukocytes function in body defenses by:
Engulfing
Directly
Producing
Secreting
Secreting
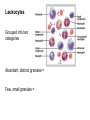
Leukocytes
Grouped into two
categories
Abundant, distinct granules =
Few, small granules =
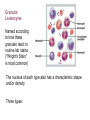
Granular
Leukocytes
Named according
to how these
granules react to
routine lab stains
("Wright's Stain"
is most common)
The nucleus of each type also has a characteristic shape
and/or density
Three types:
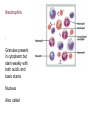
Neutrophils
.
Granules present
in cytoplasm but
stain weakly with
both acidic and
basic stains
Nucleus
Also called
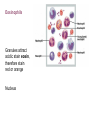
Eosinophils
Granules attract
acidic stain eosin,
therefore stain
red or orange
Nucleus
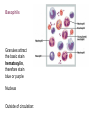
Basophils
Granules attract
the basic stain
hematoxylin,
therefore stain
blue or purple
Nucleus
Outside of circulation:
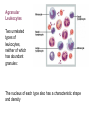
Agranular
Leukocytes
Two unrelated
types of
leukocytes,
neither of which
has abundant
granules:
The nucleus of each type also has a characteristic shape
and density
Monocytes
Nucleus
Stains
Cytoplasm
Outside of circulation:
Lymphocytes
Nucleus
Varying amounts of cytoplasm
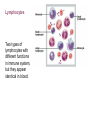
Lymphocytes
Two types of
lymphocytes with
different functions
in immune system,
but they appear
identical in blood:
All leukocytes formed in bone marrow, then enter blood
But:
Not particularly active when in the blood.
Most leukocytes are using the blood to get to other
tissues and organs, where they differentiate and
become active
Since they generally function outside of the circulatory
system, primarily in the connective tissues of other organs,
All leukocytes can leave (and most can also reenter) the
blood vessels by a process called
Therefore: All of the leukocytes, and the cells which they
mature into, are normally found in connective tissues
throughout the body
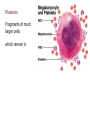
Platelets
Function
250,000 to 500,000 per cubic millimeter
or
250,000,000 to 500,000,000 per milliliter (cubic centimeter)
Platelets
Fragments of much
larger cells,
which remain in
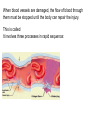
When blood vessels are damaged, the flow of blood through
them must be stopped until the body can repair the injury.
This is called
It involves three processes in rapid sequence:
Vasospasm
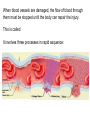
When blood vessels are damaged, the flow of blood through
them must be stopped until the body can repair the injury.
This is called
It involves three processes in rapid sequence:
Formation of a Platelet Plug
-
Under normal conditions, platelets do not stick to each
other or to the walls of blood vessels
-
When a blood vessel is injured, it releases chemicals
which cause platelets to attach to each other and to the
injured part of the vessel. This is
-
As new platelets attach, they also
When blood vessels are damaged, the flow of blood through
them must be stopped until the body can repair the injury.
This is called
It involves three processes in rapid sequence:
Formation of a Fibrin Blood Clot
-
This involves a series of sequential chemical reactions
in which the products of the first reaction serve as the
catalysts of the second reaction, whose products are the
catalysts of the third reaction, whose products are the
catalysts of the fourth reaction, etc.
-
This allows for a very rapid increase in the rate at which
the clot forms.
-
It also allows many chances to stop the process if it
began by mistake or gets too far away from where the
vessel was injured.
Formation of a fibrin
blood clot involves 13
"clotting factors".
Each of these is the
reactant for the next
of these sequential
reactions
Factor
Synonyms
Factor I
Fibrinogen
Factor II
Prothrombin
Factor III
Tissue Thromboplastin
Factor IV
Calcium
Factor V
Proaccelerin
Factor VI
Labile Factor
Factor VII
Prothrombin accelerator
Factor VIII Antihemophilic Factor A
Factor IX
Antihemophilic Factor B
Factor X
Stuart Factor
Factor XI
Thromboplastin Antecedent
Factor XII
Hageman Factor
Factor XIII Fibrin Stabilizing Factor
Formation of a fibrin
blood clot involves 13
"clotting factors".
Each of these is the
reactant for the next
of these sequential
reactions
Last reaction:
Once the fibrin clot has formed,
Over the next 30 to 60 minutes,
End result: Dense network of interconnected strands of
fibrin with platelets, erythrocytes, and leukocytes trapped
within it.
Over next few days, after vessel has time to repair itself:
Clot is dissolved and
removed by process
called
Plasma protein
converted to active
enzyme
which dissolves
fibrin.