* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Fluids & Electrolytes Part 1
Cushing reflex wikipedia , lookup
Cardiac output wikipedia , lookup
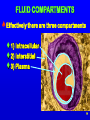
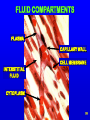
Intracranial pressure wikipedia , lookup
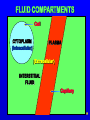
Electrophysiology wikipedia , lookup
Circulatory system wikipedia , lookup
Common raven physiology wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Hemodynamics wikipedia , lookup
Countercurrent exchange wikipedia , lookup
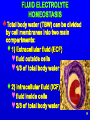
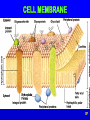
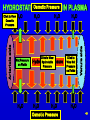
ADVANCED PHYSIOLOGY FLUID & ELECTROLYTES Part 1 Instructor Terry Wiseth NORTHLAND COLLEGE 1 FLUID ELECTROLYTE HOMEOSTASIS In a healthy individual fluid volume and electrolyte concentrations are maintained within strict homeostatic limits through the interaction of several organ systems 2 FLUID ELECTROLYTE HOMEOSTASIS Total body water (TBW) can be divided by cell membranes into two main compartments: 1) Extracellular fluid (ECF) fluid outside cells 1/3 of total body water 2) Intracellular fluid (ICF) fluid inside cells 2/3 of total body water 3 FLUID ELECTROLYTE HOMEOSTASIS The ECF is further divided into: 1) Blood plasma (80%) 2) Interstitial fluid (20%) These two ECF compartments are separated by a capillary membrane Interstitial fluid 4 FLUID COMPARTMENTS Effectively there are three compartments 1) Intracellular 2) Interstitial 3) Plasma 5 FLUID COMPARTMENTS Cell CYTOPLASM (Intracellular) PLASMA (Extracellular) INTERSTITIAL FLUID Capillary 6 ELECTROLYTES Dissolved ions in the: Cell, interstitial fluid, blood Potassium (K) Sodium (Na) Calcium (Ca) Magnesium (Mg) Chlorine (Cl) Bicarbonate (H2CO3) Proteins (Pr) 7 ELECTROLYTES There are three key concepts in consideration of fluid and electrolyte management: 1) Cell Membrane Permeability 2) Osmolarity 3) Electroneutrality 8 CELL MEMBRANE PERMEABILITY Refers to the ability of a cell membrane to allow certain substances to pass freely Other substances like charged ions (Na+) cannot cross the membrane and are trapped on one side of it H2O Na+ H2O H2O H2O Na+ H2O Na+ H2O Na+ Na+ H2O Na+ H2O Na+ Na+ 9 CELL MEMBRANE PERMEABILITY In other words “No Trespassing” Cell membranes allow some things to pass and blocks passage of others 10 OSMOLARITY Osmolarity is a property of particles in solution If a substance can dissociate in solution, it will contribute to the osmolarity of the solution 11 OSMOLARITY In other words “Water, water every where but not a drop to drink” If you are thirsty, you cannot drink salt water 12 ELECTRONEUTRALITY The principle of Electroneutrality means that the overall number of positive and negative charges balances For instance, in conditions like renal tubular acidosis where HCO3- is lost, chloride is retained Cl13 ELECTRONEUTRALITY In other words “Cells do not make good batteries” Positive and negative charges inside and outside the cell must be equal Click to show a charged + battery + + + + + + + + - 14 ELECTROLYTES When the body is in “fluid balance” it means that the various body compartments (cells, tissues, organs) contain the required amount of fluids to carry out normal bodily functions 15 ELECTROLYTES Fluid balance and electrolyte balance are inseparable In a healthy individual, the volume of fluid in each compartment remains stable 16 ELECTROLYTES Loss of electrolytes can have serious consequences for the body In severe dehydration, the loss of electrolytes can result in circulatory problems such as tachycardia (rapid heart beat) and problems with the nervous system such as loss of consciousness and shock 17 ELECTROLYTES Electrolytes serve three general functions to maintain: 1) Normal metabolism 2) Proper fluid movement between compartments 3) The acid-base balance 18 ELECTROLYTE COMPOSITION OF PLASMA AND INTERSTITIAL FLUID (meq/liter) PLASMA INTERSTITIAL FLUID Na+ 140.0 145.5 + K 4.5 4.8 Ca++ 5.0 2.8 ++ Mg 1.5 1.0 Cl 104.0 116.6 HCO324.0 27.4 PROTEIN 14.0 8.0 19 ELECTROLYTES Protein HCO3ClMg++ INTERSTITIAL FLUID PLASMA Ca++ K+ Na+ 0 50 100 150 200 20 ELECTROLYTES Na+ K+ Ca++ PLASMA Mg++ ClHCO3Protein INTERSTITIAL FLUID 21 IONS AND MOLECULES Ions are charged atoms ex: Na+, Cl-, Mg++ Na+ Cl- Molecules are formed when two or more atoms or ions are combined ex: H2O, C6H12O6, NaCl 22 MOVEMENT OF BODY FLUIDS Fluid moves between the compartments of the body through various mechanisms Substances leave and enter capillaries via three mechanisms: 1) Vesicular transport 2) Diffusion 3) Bulk flow 23 VESICULAR TRANSPORT AND DIFFUSION Vesicular transport and diffusion are associated with the movement of solutes (electrolytes) 24 BULK FLOW Bulk flow is the most important process for the maintenance of relative volumes (fluids) of blood and interstitial fluid Bulk flow involves the movement of both solvent (fluids) and solute into the interstitial space 25 MOVEMENT OF IONS AND MOLECULES Ions and molecules pass through membranes by: Simple Diffusion Passage through channels Facilitated Diffusion Active Transport (Na-K pump) 26 CELL MEMBRANE 27 FLUID COMPARTMENTS Describes the distribution of water in the body Fluid compartments are separated by semipermeable membranes Capillary wall separates the plasma and the interstitial fluid Cell membrane separates the cytoplasm and interstitial fluid 28 SEMIPERMEABLE MEMBRANE 29 SEMIPERMEABLE MEMBRANE 30 FLUID COMPARTMENTS PLASMA CAPILLARY WALL CELL MEMBRANE INTERSTITIAL FLUID CYTOPLASM 31 FLUID SHIFTS Fluid shifts may occur as the result of disease or injury 32 FLUID SHIFTS Accumulations of fluids in a tissue or in a body cavity is called third space compartment Ex: liver disease may lead to significant accumulations of fluid in the peritoneal cavity Represents a fluid loss as it is trapped 33 FACTORS CONTROLLING EXCHANGES OF FLUIDS 1) Diffusion 2) Filtration a) Hydrostatic Pressure b) Osmotic (Oncotic) Pressure 34 DIFFUSION Water, small molecules and ions Movement of molecules from areas of higher concentration to areas of lower concentration Click to View Animation 35 FILTRATION Net flow of water is due to overall effect of pressure on both sides of a membrane Fluid is filtered out of capillaries in response to changes in: 1) Hydrostatic Pressures 2) Oncotic (Osmotic) Pressures 36 HYDROSTATIC PRESSURE (HP) Fluid pressure Ex: blood pressure in the capillaries H2O H2 O H2O H2 O H2O H2O H2O H2O H2O H2O H2O 6 4 8 6 H2O 37 HYDROSTATIC PRESSURE (HP) Fluid pressure Ex: blood pressure in the capillaries Ex: pressure exerted by interstitial fluid H2O H2O H2 O H2 O H2O H2O H2O 8 6 H2O H2O H2O 6 4 H2O H2O 38 HYDROSTATIC PRESSURE IN PLASMA Blood Pressure at Arterial end of capillaries is 30 mm Hg Blood Pressure at Venous end of capillaries is 10 mm Hg Difference in pressure forces fluid out of plasma to the interstitial fluid 39 Pressure IN PLASMA HYDROSTATICOsmotic PRESSURE H2O Net Pressure on Fluids H2O H2O H2O Click to View Hydrostatic Hydrostatic Pressure Pressure H2O H2O Osmotic Pressure H2O Netto Click Pressure View Net on Fluids Pressure on Fluids Venule side Arteriole side Click to View Osmotic Pressure H2O 40 HYDROSTATIC PRESSURE IN INTERSTITIAL FLUID The lymphatic system drains interstitial fluid creating a negative interstitial pressure Hydrostatic pressure in interstitial space is - 6 mm Hg Supplies a pulling force (suction) drawing fluid out of the capillaries 41 OSMOTIC (ONCOTIC) PRESSURE Drawing force resulting from the pressure created by presence of protein dissolved in the: Cytoplasm Plasma Interstitial fluid Pressure which develops when there is net movement of water across a membrane (osmosis) 42 OSMOTIC (ONCOTIC) PRESSURE Pressure created is directly proportional to solute concentration Thus osmotic pressure is dependent on the concentration of urea, glucose, amino acids, electrolytes and proteins Oncotic pressure defines pressures which are the result of protein concentration differences 43 OSMOTIC (ONCOTIC) PRESSURE Click to View Change Semi-permeable membrane Solute Solvent HIGH OSMOTIC PRESSURE LOW OSMOTIC PRESSURE 44 ONCOTIC PRESSURE IN PLASMA Oncontic pressure at the arterial end of capillaries is 28 mm Hg Oncotic pressure of interstitial fluid is 5 mm Hg Due to a higher protein concentration in plasma (albumin) Pr Pr Capillary Pr Pr - H2O H O Pr 2 Pr PrPr Pr PrPr Pr- Pr- Pr- Pr- Pr- Pr- Pr- Pr- PrPr- 45 ONCOTIC PRESSURE Capillary PROTEIN (OP) H2 O INTERSTITIAL FLUID PROTEIN (OP) H2 O Opposing oncotic pressure (OP) inside and outside of a capillary. A higher protein concentration in plasma as compared to interstitial fluid, thus it has a 46 greater oncotic pressure CAPILLARY-INTERSTITIAL FLUID EXCHANGES Hydrostatic and osmotic (oncotic) pressures create opposing inward and outward forces on the capillary Capillary Hydrostatic Pressures Osmotic Pressures 47 OUTWARD FORCES Arterial end of capillary exerts hydrostatic pressure (30 mm Hg) Capillary 30 Hydrostatic Pressures 48 OUTWARD FORCES Interstitial fluid oncotic pressure (5 mm Hg) Negative interstitial fluid pressure (-6 mm Hg) Total outward pressure 41 mm Hg Capillary Osmotic 5 Pressures Hydrostatic 30 Pressures 6 Interstitial Fluid (Pull) 49 INWARD FORCES Plasma oncotic pressure (28 mm Hg) Capillary 28 Osmotic Pressures 50 INWARD FORCES Net outward filtration of 13 mm Hg results in plasma fluid loss 41 mm Hg - 28 mm Hg = 13 mm Hg Capillary Osmotic 28 Pressures Osmotic 5 Pressures Hydrostatic 30 Pressures 6 Interstitial Fluid (Pull) 51 Opposing forces that influence fluid shifts across the capillary wall. The net effect is outflow of fluid (41 - 28) with a net pressure of 13 Arterial end of capillary 30 mm Hg (HP) Interstitial fluid - 6 mm Hg (HP) 28 mm Hg (OP) 5 mm Hg (OP) Total pressure drawing fluid out Inward drawing force 52 ABNORMAL CAPILLARY DYNAMICS Loss of protein and fluid from plasma to interstitial fluid is provided a return to the circulatory system by way of the lymphatic system 53 ABNORMAL CAPILLARY DYNAMICS Increased capillary fluid loss occurs when there is: 1) Increased Capillary Hydrostatic Pressure 2) Increased Interstitial Fluid Oncotic Pressure 3) Decreased Plasma Oncotic Pressure Accumulations of fluid in interstitial spaces is called edema 54 CONDITIONS FOR EDEMA Increased HP Capillary - HP OP OP Interstitial fluid Increased capillary Hydrostatic Pressure (HP) 55 CONDITIONS FOR EDEMA Capillary HP - HP Decreased OP OP Interstitial fluid Decreased plasma Oncotic Pressure (loss of protein) 56 CONDITIONS FOR EDEMA Capillary HP - HP OP Increased OP Interstitial fluid Increased Oncotic Pressure in interstitial fluid 57 EDEMA Various liver diseases that result in decreased protein synthesis lead to edema Noxious gases, inflammation (pneumonia), or respiratory burns may cause increased permeability of pulmonary capillaries with loss of proteins and fluid Cause of pulmonary edema in these cases may be a combination of factors 58 CAUSES FOR EDEMA I) Malnutrition II) Capillary wall damage III) Obstructed lymph flow IV) Fluid accumulation in the lungs V) Left ventricle heart failure VI) Congestive heart failure VII) Glomerulonephritis VIII) Nephrotic syndrome IX) Large doses of blood or salt sol. 59 I) MALNUTRITION Decreased or cessation of food intake leads to decreased synthesis of protein by the liver Resulting in marked lowering of plasma protein Decreased oncotic pressure causes a lowered tendency to draw water into the capillaries Thus fluids accumulate outside the capillaries 60 MALNUTRITION Normal Protein H2O Malnutrition Capillary Decreased Protein Decreased Protein H2O In malnutrition, there is a decreased synthesis of protein by the liver, resulting in a lowered protein level in plasma. A decrease in oncotic pressure causes a diminished tendency to draw water into capillaries. The net result is edema 61 KWASHIORKOR AND MARASMUS Reduced osmolarity from lack of protein in the diet results in a fluid shift, as more water moves out of the capillaries into the interstitial spaces like the peritoneal cavity 62 II) CAPILLARY WALL DAMAGE Damage which increases capillary permeability to proteins Ex: exposure to certain chemicals Venoms Bacterial toxins Inflammatory response Protein loss leads to decrease in capillary oncotic pressure 63 CAPILLARY WALL DAMAGE Capillary H2O H2O Normal Venom or Toxins (Increased Proteins) 64 III) OBSTRUCTED LYMPH FLOW Excess fluids and proteins in interstitial fluid are collected and returned to plasma by lymphatic vessels abdominal surgery mammogram Tumor or surgical removal of lymph nodes can obstruct flow which leads to edema 65 IV) PULMONARY EDEMA Fluid accumulates in alveoli of the lungs 66 PULMONARY EDEMA Pulmonary capillaries are more permeable to proteins than capillaries in other parts of the body Thus lungs are more susceptible to edema 67 PULMONARY EDEMA Tendency toward increased oncotic pressure (water drawing force) Interstitial fluid space is limited in lung tissue Alveoli RBC Interstitium Thus excessive fluid in the interstitial fluid space leaks readily into the alveoli interfering with gas exchange 68 ALVEOLAR EDEMA In this section of lung the alveolar walls are congested (arrow A) and the alveolar spaces are filled with pink fluid (arrow B). A few alveolar macrophages (arrow C) are present but there is no significant inflammation 69 PULMONARY EDEMA Factors which protect the lungs from fluid accumulations: 1) A high rate of lymph flow away from the lungs 2) Pulmonary capillary pressure that is lower than systemic capillary pressure Great deal of congestion is present as well as fluid in the alveoli 70 PULMONARY EDEMA Principles of water balance in the lungs are the same as in peripheral tissues Any condition that causes increased capillary hydrostatic pressure, decreased capillary oncotic pressure, or increased capillary permeability may lead to pulmonary edema 71 V) LEFT VENTRICLE HEART FAILURE Pulmonary edema is characteristic of various forms of heart failure If the left ventricle of the heart fails as a pump: 1) Pulmonary circulation is slowed and there is a buildup of blood in the pulmonary vessels 2) Blood pressure increases 72 HYDROSTATIC EDEMA pulmonary artery pulmonary artery This radiograph demonstrates pulmonary arteries that are much larger than their accompanying bronchi (A). In addition the bronchial walls are thickened. The patient was treated with diuretics and the subsequent scan (right) shows normal appearing bronchi (B) in which the bronchial walls are thin and the pulmonary artery and bronchus are the same size 73 VI) CONGESTIVE HEART FAILURE The heart fails as a pump coronary bypass Increased pulmonary venous and capillary pressure because of increased blood volume (increased hydrostatic pressure) 74 VII) GLOMERULONEPHRITIS Inflammatory kidney disease Edema is caused by fluid retention Thus there is increased capillary hydrostatic pressure 75 VIII) NEPHROTIC SYNDROME Urinary protein loss and decreased plasma protein Generalized edema as the result of lowered plasma oncotic pressure 76 IX) ADMINISTRATION OF LARGE AMOUNTS OF BLOOD OR SALT SOLUTIONS Pulmonary edema is the result of increased blood volume Thus increased hydrostatic pressure Individuals with heart or kidney disease are especially susceptible 77 INTERSTITIAL FLUIDCELLULAR DYNAMICS Water movement between cells and the interstitial fluids Electrolyte composition is a major factor in this exchange Osmotic pressure is the drawing force 78 ELECTROLYTE CONCENTRATIONS Interstitial Muscle Meq/liter Fluid Cells + Na 145.5 12 + K 4.8 150 Ca++ 2.8 0.0000001 Mg++ 1.0 7 Cl 116.6 3 HCO3 27.4 10 --PO4 2.3 116 Protein 8.0 40 79 PRINCIPLE ELECTROLYTE IN INTERSTITIAL FLUID Meq/liter + Na K+ Ca++ ++ Mg Cl HCO3--PO4 Protein Interstitial Fluid 145.5 4.8 2.8 1.0 116.6 27.4 2.3 8.0 Muscle Cells 12 150 0.0000001 7 3 10 116 40 80 MAIN INTRACELLULAR IONS Meq/liter + Na K+ Ca++ ++ Mg Cl HCO3--PO4 Protein Interstitial Fluid 145.5 4.8 2.8 1.0 116.6 27.4 2.3 8.0 Muscle Cells 12 150 0.0000001 7 3 10 116 40 81 ELECTROLYTE COMPARISONS 82 SIGNIFICANT IONS Na+ Cl- K+ PO4- - - 83 FLUID IMBALANCE Fluid imbalance may occur and result in either: Cellular dehydration Cellular hydration 84 CELL DEHYDRATION IN DIABETES Ex: diabetes Glucose concentrations increase in extracellular fluids Increased conc. gradients outside the cells draw water out of the cells by creating an osmotic pull H2 O glucose 85 CELL HYDRATION Na+ ions predominate in extracellular fluid Thus Na+ plays a major role in determining osmotic pressure Low Na+ in extracellular fluid creates an intracellular osmotic pull on H20 Na+ loss Click to View Animation Decreased solute concentration Hydration of cells Decreased osmotic pressure 86 CELL HYDRATION Low sodium levels can be caused by diuretics, vomiting or low Na+ intake If low sodium levels are combined with excess water intake Cell hydration is exaggerated Low sodium levels + Excess water intake = Cell hydration 87 EFFECTS OF IMBALANCE ON COMPARTMENTS Intravascular (plasma) compartment is the most likely to be affected by volume changes first Interstitial and intracellular compartments are less likely to be affected and thus represent fluid reservoirs 88 SUDDEN LOSS OR GAINS OF FLUIDS Sudden loss or gain of fluids affect only intravascular compartments ex: hemorrhage Both compartments share losses or gains equally if they occur over a period of hours Significant shifts of fluids between compartments require several hours 89 LOSS OF HYPOTONIC FLUID Loss of hypotonic fluid (solute concentration less than that of plasma) has a concentrating effect on extracellular fluid This results in an increase of osmotic pressure Water is drawn out of cells in response to increased extracellular osmotic pressure 90 FLUID BALANCE DISORDERS Total volume of water in the body is 60% of body weight Intracellular fluid === 67% Plasma =========== 8% Interstitial fluid ===== 25% 91 REGULATION OF FLUID INTAKE Thirst is a powerful regulator of fluid consumption 92 REGULATION OF FLUID INTAKE Thirst center in the hypothalamus is stimulated by: 1) Cellular dehydration 2) Decreased salivary production 3) Increased blood osmotic pressure 4) Decreased blood volume 93 THIRST 1) Cellular dehydration Inadequate intake of water Increase in extracellular solute concentration 94 THIRST 2) Decreased salivary production Dry sensation of the mucosa of the mouth and pharynx 95 THIRST 3) Increased blood osmotic pressure Stimulates osmoreceptors in the hypothalamus which in turn stimulate the thirst center of the hypothalamus 96 THIRST 4) Decreased blood volume (decreased blood pressure) Stimulates the release of renin by the kidney Renin promotes synthesis of angiotensin II which affects the thirst center of the hypothalamus 97 STIMULATION OF THIRST BY DEHYDRATION 1 2 3 decreased flow of saliva dehydration increased blood osmotic pressure dry mouth and pharynx stimulates osmoreceptors in hypothalamus decreased blood volume decreased blood pressure increased renin release by juxta-glomerular cells of kidney 4 stimulates thirst center in hypothalamus 5 6 7 increased angiotensin II production increases thirst increases fluid intake increases body water to normal level and relieves dehydration 98 REGULATION OF FLUID LOSS Fluid loss can be adjusted by: 1) Antidiuretic hormone (ADH) Vasopressin 2) Atrial natriuretic peptide (ANP) 3) Aldosterone 99 REGULATION OF FLUID OUTPUT ADH and aldosterone slow fluid losses ANP causes diuresis (increased urine production) 100 DEHYDRATION If the body is dehydrated: - Blood pressure falls - Glomerular filtration decreases Water is thus conserved 101 EXCESSIVE FLUID IN BLOOD Excessive fluid in the blood causes: - Increased blood pressure - Increased glomerular filtration Thus increased fluid output 102 OTHER FACTORS CAUSING EXCESSIVE FLUID RETENTION HYPERTENSION HYPERVENTILATION HEAVY PERSPIRATION Click to View Animation VOMITING EXCESSIVE FLUID RETENTION EXTENSIVE SKIN DESTRUCTION DIARRHEA FEVER 103 EFFECTS OF FLUID EXCESS Fluid excess initially affects the extracellular compartments Increased fluid volume can result in cerebral, pulmonary or generalized edema Usually the result of inadequate renal output rather than fluid intake 104 EFFECTS OF FLUID EXCESS If the retained water is hypotonic as compared to plasma the effect is to dilute the extracellular fluid This causes a decrease in osmolality When interstitial fluid is dilute as compared to intracellular fluid, water is drawn into the cells by osmotic pull Results in increased cellular volume and changes in cell function occur Most apparent in CNS tissue 105 INTRAVENOUS INFUSION If the total body water is increased by IV infusion of an isotonic solution the result will be: Increased extracellular volume With little or no effect on cellular volume Net result is no change in solute concentrations in plasma, interstitial fluids and intracellular fluid and no effect on cells 106 INTRAVENOUS INFUSION Infusion of a hypertonic solution results in: Diffusion of both solute and water into the interstitial fluid occurs This concentration of solutes in interstitial fluid is higher than normal Creates an osmotic drawing force Pulls water out of the cell 107 SUMMARY OF OVERHYDRATION OR WATER INTOXICATION 1) If the fluid is hypotonic 2) If the fluid retained is isotonic to plasma 3) If the excess fluid is hypertonic 108 HYPOTONIC 1) If the fluid is hypotonic Increase in extracellular volume A dilutional effect Subsequent cellular dehydration 109 ISOTONIC 2) If the fluid retained is isotonic to plasma Expansion of the extracellular compartment No effect on cells 110 HYPERTONIC 3) If the excess fluid is hypertonic Increased extracellular volume Cellular dehydration 111 CAUSES FOR OVERHYDRATION 1) Psychiatric disorder of compulsive water drinking (psychogenic polydipsia) 10 -15 liters/day 112 CAUSES FOR OVERHYDRATION 2) Forced water ingestion as a form of punishment (child abuse) 113 CAUSES FOR OVERHYDRATION 3) Inappropriate ADH secretion ADH also called Vasopressin Promotes water retention (reabsorption) by increasing permeability of the collecting ducts in the kidney 114 CAUSES FOR OVERHYDRATION ADH is also a powerful vasoconstrictor of arterioles Head trauma, lung cancers, pneumonia, CNS diseases, encephalitis Some types of tumors secrete substances with ADH-like activity 115 DEHYDRATION Effects of a fluid deficit depend on: Volume Rate of loss Amount of electrolytes lost with water 116 HYPOTONIC LOSS Simple dehydration is sometimes called hypotonic loss Effects of hypotonic fluid loss (water loss exceeds solute loss) has a concentrating effect Results in increased osmolality and hypernatremia (increased Na+ concentration) 117 HYPOTONIC LOSS Water is drawn out of cells into the extracellular compartment Cell volume depletion stimulates the release of ADH (antidiuretic hormone) and aldosterone ADH mediates renal water retention Aldosterone favors Na+ and water retention 118 SUMMARY OF HYPOTONIC DEHYDRATION Immediate effect of water loss is hypernatremia Physiological responses to correct the imbalance: Movement of cellular water to extracellular compartments Hormonal responses that increase extracellular volume H2 O 119 CAUSES FOR DEHYDRATION 1) Excessive sweating 2) Insensible fluid loss 3) Diuresis 4) Diabetes insipidus 120 CAUSES FOR DEHYDRATION 1) Excessive sweating Sweat is hypotonic May result in hypernatremia with losses of electrolytes 121 CAUSES FOR DEHYDRATION 2) Insensible fluid loss From the skin or lungs 122 CAUSES FOR DEHYDRATION 3) Diuresis Solute cleared from the blood by the kidney and not reabsorbed remains in the glomerular filtrate This high solute concentration creates an osmotic pull that draws water in that direction Results in increased urine output and water loss 123 DIURESIS Mannitol (polysaccharide) is sometimes used in cerebral edema Non-reabsorbable solute and creates an osmotic pull on water promoting water loss 124 CAUSES FOR DEHYDRATION 4) Diabetes insipidus Deficiency of ADH Excessive urination and thirst 125 ELDERLY Older individuals have a decreased renal capacity to save water Significant if: Fluid intake is limited (decreased diet) Insensible fluid loss is increased (fever) 126 ELDERLY Elderly are also susceptible to water intoxication Increased ADH secretion (stress of surgery, pneumonia, meningitis) Reduction in renal blood flow Decreased urine volume and water retention Heart failure, liver disease, drug induced hypotension 127 INFANTS Infants have a greater surface area compared to weight Increased insensible fluid loss Infants have less renal concentrating ability than an adult 128 END FLUID AND ELECTROLYTES PART 1 129 MOVEMENT OF BODY FLUIDS Pressures acting to move substances out of the capillary include: Blood Hydrostatic Pressure (BHP) Interstitial Fluid Osmotic Pressure (IFOP) 130 MOVEMENT OF BODY FLUIDS Blood colloid osmotic pressure (BCOP) and interstitial fluid hydrostatic pressure act to push substances into the capillary At the arterial end of the capillary the sum of the outward moving pressures is dominant and substances move into the interstitial fluid (filtration) At the venous end the inward pressure is dominant and the substances move into the capillary (reabsorption) 131 MOVEMENT OF BODY FLUIDS The exchange of interstitial and intracellular fluid is controlled mainly by the presence of the electrolytes sodium and potassium Potassium is the chief intracellular cation and sodium the chief extracellular cation 132 MOVEMENT OF BODY FLUIDS Because the osmotic pressure of the interstitial space and the ICF are generally equal water typically does not enter or leave the cell A change in the concentration of either electrolyte will cause water to move into or out of the cell via osmosis 133 MOVEMENT OF BODY FLUIDS A drop in potassium will cause fluid to leave the cell whilst a drop in sodium will cause fluid to enter the cell Aldosterone, ANP and ADH regulate sodium levels within the body, whilst aldosterone can be said to regulate potassium 134