* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Glaucoma
Fundus photography wikipedia , lookup
Contact lens wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Keratoconus wikipedia , lookup
Vision therapy wikipedia , lookup
Macular degeneration wikipedia , lookup
Diabetic retinopathy wikipedia , lookup
Retinitis pigmentosa wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
Corneal transplantation wikipedia , lookup
Visual impairment wikipedia , lookup
Eyeglass prescription wikipedia , lookup
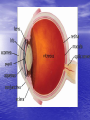
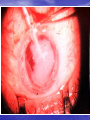
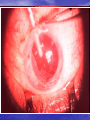
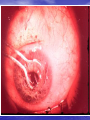
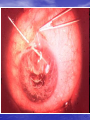
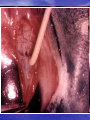
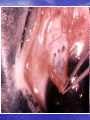
Lecture 4 CATARACT & GLAUCOMA Lecture is delivered by Ph. D., associate professor Tabalyuk T.A. Classification of cataracts: By age: congenital, juvenile, age-related (senile) By location opacities in the lens as seen with slit beam: cortical, nuclear, anterior subcapsular, posterior subcapsular By maturity: early, immature, mature, hypermature (Morgagnian cataract) By pattern: cuneiform (typical senile type), zonular, polar, pyramidal (congenital types) DIFFERENTIAL DIAGNOSIS The same sign is progressive (not acute) painless visual loss CATARACT Sign Visual acuity Field vision GLAUCOMA MACULAR DEGENERATION is decreased of is not damaged constriction of nasal may be visual field, Bjerrum’s scotoma scotoma Intraocular pressure normal, increased normal Lens opaque transparent, transparent, Fundus If is seen, damaged. if increased-secondary phakogenic glaucoma central if opaque– complicated if opaque– complicated cataract cataract not optic disc changes - degenerative patches dislocation of vessels, in central area If damaged - pale colour, increased complicated cataract cupping Artificial lenses Artiphakia is a condition of eye with artificial lens (IOL). Aphakia is a condition of eye without lens. The visual acuity without correction is very poor – 0,02-0,04. Iridodenesis (iris vibration) is typical. Thick plus glasses are needed for vision: for far distance – sph convex 10,0-12,0 D for near distance – sph convex 13,0-15,0 D. Secondary cataract occurs eventually in about 20 % cases after cataract surgery. It is opacity of natural posterior capsule. It can be treated by YAG laser capsulotomy. Attention! The term «complicated cataract» is used to describe a lens opacity which occurs as a result of some other disease of the eye. Longstanding uveitits, an untreated retinal detachment or an intraocular tumour are all examples of an associated disease. CONGENITAL CATARACTS : I degree – visual acuity is 0,3 and more; the size of opacity is less then 1,5 mm; the surgery may be done at the age of 14-16 years. II degree– visual acuity is 0,05-0,2; the surgery is usually done at the age of 3-4 years. III degree– visual acuity is less then 0,05; the surgery must be done during first year of life. Ectopia lentis (displacement of the lens) may be partial (subluxation) or complete (luxation). Aethiology: trauma, familial ectopia lentis (may be associated with ectopic pupil), associated with other ocular disprders (aniridia and buphtalmos), Marfan’s and Weill-Marchesani syndromes, metabolic (homocystinuria and hyperlysinaemia). Clinical features: iridodenesis (vibration of iris) and not proportional depth of anterior chamber. Marfan’s syndrome: tall person with partial displacement of the lens (subluxation), fragile bones and arachnodactyly. Video – phakoemulsification The outflow pathways of aqueous humor: 1. Main: posterior chamber - pupil - anterior chamber trabecular meshwork - Schlemm’s canal (scleral sinus)vorticose veins – scleral venous plexus. Additional: 2. Perivascular spaces of iris. 3. Suprachoroidal space - perivascular spaces – through sclera into the tenon’ s space. 4. Perivascular spaces of central retinal vessels. The IOP is maintained by a balance between aqueous inflow and outflow & usually measures between 16-26 mm Hg (using tonometr of Maklakov) & 10-20 mm Hg (using tonometr of Goldman) Noncontact pneumatic autotonometry Not every increasing of IOP is glaucoma. It may be ocular hypertension, caused, for example, by using corticosteroids, intoxication or climax. Typical for ocular hypertension are: absence of structural and functional changes; lasting existence without complaints; symmetrical increasing of IOP. So, ocular hypertension is a symptom, glaucoma is a syndrome. Glaucoma is such increasing of IOP, which is accompanied by specific visual defects (constriction of nasal visual field, Bjerrum’s scotoma) and specific optic disc changes (dislocation of vessels, increased cupping etc.) Congenital glaucoma (or hydrophtalmos) is caused by abnormal development of eye drainage system. The accumulation of aqueous in the eye due to elasticity of baby’s external coat causes the increasing of eye size. There are 2 clinical forms: I. Hydrophtalmos without stasis (megalocornea, stretching out of limbus, deep anterior chamber, increased eye, loss of vision, increased IOP, typical changes of optic nerve). II. Hydrophtalmos with stasis (all above mentioned signs + photophobia, blepharospasmus, mixt injection, corneal oedema, which is reliefed by 40 % glucosae). There are 4 stages: I. Early – D of cornea 12,0-12,5 mm, anterior-posterior distance of the eye is increased on 1,5-2,0 mm, N fundus. II. Advanced - D of cornea 13,0-14,0 mm, anterior-posterior distance of the eye is increased on 3,0-4,0, glaucomatous cupping of optic disc ophthalmoscopically. III. Far advanced - D of cornea is more then 14,0 mm, anterior-posterior distance of the eye is more then 30,0 mm, atrophy of optic disc ophthalmoscopically. IV. Terminal (or buftalm) – full blidness, scleral staphyloma. Methods of diagnostic of congenital glaucoma: General examination, especially of cornea & limbus Biomicroscopy or focal lighting Keratometry Tonometry Ultrasound biometry Ophthalmoscopy Methods of treatment of congenital glaucoma: Only surgical. Immediatly! Goniotomy Sinusotrabeculectomy Enucleation in buftalmos Classification of primary acquired glaucoma Clinical form Stage 1. Open-angle I – early 2. Close-angle II – advanced III – far 3. Mixt advanced IV - terminal Level of IOP A - compensated B - subcompancated C -decompancated Dynamics of visual functions stabile & nonstabile Stages of primary glaucoma (according to visual functions defects): I – visual field is consticted less then 10 degrees, physiological cupping is increased. II - visual field is consticted more then 10 degrees, edge excavation. III – tube visual field (15 degrees from the point of fixation), edge excavation. IV – visual field or visual acuity is zero, atrophy of optic disc. Depending on IOP (using tonometr of Maklakov) glaucoma is subdivided: A (compensated) – IOP is less then 27 mm Hg. B (subcompancated) – IOP is 28-32 mm Hg. C (decompancated) – IOP is 33 mm Hg and more. According to dynamics of visual functions during 6 month: stabile & nonstabile – constriction of visual field on 10 degree and more; in tube vision – on 2-3 degrees and more; increasing of scotomas size; increasing of size of optic disc cupping Open-angle glaucoma Pathogenesis – constriction or closing of openings in trabeculae & Schlemm’s canal as a result of endocrine, vascular or general diseases such as atherosclerosis, artery hypertension, diabetus mellitus etc. Clinical features: usually asymptomatic until significant loss of visual field has occured; the eye looks usual, only dystrophic iris changes may be revealed biomicroscopically; open anterior chamber angle on gonioscopy, may be excess pigmentation of trabeculae; & typical for glaucoma signs (elevated IOP+visual field loss,first of its nasal part +optic nerve damage). Methods of investigation: A. Functional – visometry, perimetry, campimetry, adaptometry. B. Objective – general examination, focal lighting, biomicroscopy, gonioscopy, ophthalmoscopy, tonometry. Close-angle glaucoma Pathogenesis –the closing (blockade) of anterior chamber angle by iris root as a result of excess anterior position of lens or functional pupil blockade (not organic, i.e. occlusio or seclusio pupille) due to excess near location of lens & iris. Clinical features: complaints for clouding of vision, haloes around lights in the morning, headache, pain in the eye etc.; frequent change of eye refraction & glasses prescribtion; sometimes begins from acute attack; signs of venous stasis – dilated scleral veins; flat anterior chamber & iris bombee biomicroscopically; narrow or close anterior chamber angle on gonioscopy; & typical for glaucoma signs (elevated IOP+visual field loss,first of its nasal part +optic nerve damage). Methods of investigation: A. Functional – visometry, perimetry, campimetry, adaptonetry. B. Objective – general examination, focal lighting, biomicroscopy, gonioscopy, ophthalmoscopy, tonometry. DIFFERENTIAL DIAGNOSIS CATARACT Sign Visual acuity Field vision CHRONIC GLAUCOMA RETINITIS PIGMENTOSA is decreased progressivly of is not damaged constriction of nasal concentric visual field visual field, Bjerrum’s narrowing scotoma Intraocular pressure normal, increased normal Lens opaque transparent, transparent, Fundus if is seen, damaged. if increased-secondary phakogenic glaucoma if opaque– complicated if opaque– complicated cataract cataract not optic disc changes – nasal dislocation of If damaged - vessels, glaucomatous complicated cataract cupping mid-peripheral perivascular “bonespicule” pigmentation, waxy disc pallor without nasal dislocation of vessels & glaucomatous cupping Medical treatment of chronic glaucoma: 1. Local hypotensive therapy. The antiglaucomatous drops are divided into two main groups: I. which improve outcome of aqeous humour Cholinomimetics - 1 % pilocarpini, carbachol; α, Β – adrenomimetics – dipinefrini, epinefrini; Analogs of prostaglandins F 2 α (which stimulate the uveo-scleral outflow) – latanoprost (xalatan), travoprost (travatan) II. which reduce production of aqeous humour Central agonists of α2- adrenoreceptors - klonidini; B-adrenoblockers: nonselective - timololi, arutimoli, & selective - betoptic; Carbonic anhydrase inhibitors – Azopt. 2. Vasodilatators – acidi nicotinici, cavintoni, trentali, halidori etc. 3. Nootrops – piracetami, nootropili, etc. 4. Stimulators of nerve conductivity – proserini. 5. Tissue therapy, vitamins. Laser treatment of chronic glaucoma: Laser peripheral iridotomies in primary angle-closure glaucoma; Laser trabeculoplasty in primary open-angle glaucoma. Surgery of chronic glaucoma: Filtration surgery in primary open-angle glaucoma, e.g. trabeculectomy. In primary angle-closure glaucoma radical surgery – phacoemulsification of cataract with IOL implantation; palliative surgery – iridectomy. Nonpenetreting filtration surgery: canaloplasty • Figure 1 (left). Introduction of the microcatheter into Schlemm's canal • Figure 2 (right). A 10-0 polypropylene suture being tied around the end of the microcatheter Nonpenetreting filtration surgery: viscocanalostomy The initial steps of viscocanalostomy are similar to those of trabeculectomy. Specifically, the surgeon creates a one-half– to two-thirds–depth superficial scleral flap, within the bed of which a deep scleral flap is made. The deep dissection begins 4 to 5 mm posterior to the limbus and advances toward the limbus in a tissue plane just above the suprachoroidal space. As the dissection advances anteriorly, the roof of Schlemm’s canal is removed. The surgeon then cannulates Schlemm’s canal and injects a bolus of viscoelastic material into each of the canal’s cut ends (as in the picture). This viscodissection is intended to dilate the canal and facilitate the subsequent drainage of aqueous. Laser surgery in glaucoma Differential diagnosis of acute close-angle glaucoma Symptom acute close-angle glaucoma iridocyclitis haloes around lights + - irradiation of pain + - injection (redness) mixt venous stasis pericorneal arterial cornea oedematous decreased sensitivity precipitates on endothelium normal sensitivity anterior chamber flat normal pupil mydriasis miosis, posterior synechia IOP increased normal or decreased Emergency in acute close-angle glaucoma: instillation of miotics (pilocarpini 1 or 2 %) every 15 minutes during first hour, every 30 minutes during next hour, then 4 times a day; analgetics (promedoli 2 % 1,0 ml s/cutaneous); diuretics (Diacarbi 0,5 or Hipothiasidi 0,1 per os, Lasix 1 % 2,0 ml i/m) If the attack of acute close-angle glaucoma doesn’t disappear during 12-24 hours, antiglaucomatous surgery is indicated. Suspicion of glaucoma may be in such cases: • IOP is 27 mm Hg and more (using tonometr of Maklakov) and 21 mm and more (using tonometr of Goldman); • complaints for clouding of vision, haloes around lights in the morning; • iris bombee, less depth of anterior chamber; • typical changes of optic disc; • the difference in right and left eye IOP is more then 5 mm Hg. All patients with suspicion of glaucoma must be observed in details in clinics. This diagnosis can exist only one year. Methods of investigation: A. Functional – visometry, perimetry, adaptonetry, campimetry. B. Objective – general examination, focal lighting, biomicroscopy, gonioscopy, ophthalmoscopy, tonometry. C. Necessary additional – diurnal tonometry, tonography, elastotonometry, provocative test. Secondary glaucoma is complication or outcome of some other eye diseases. It may be: 1. Uveal glaucoma – as a result of pupil occlusion. Management – treatment of uveitis. In deep anterior chamber– mydriatics. In flat anterior chamber – miotics. 2. Phacogenic – prodused by immature cataract or lens dislocation into the anterior chamber. Management – cataract surgery. 3. Phacolytic - prodused by hypermature cataract. Management – cataract surgery. 4. Vascular glaucoma as a result of central vein occlusion or neovascularization in diabetus mellitus. Management – treatment of main disease. 5. Posttraumatic as a result of burns, penetrating or blunt injury of eyeball. Management – miotics. 6. Neoplastic – as a result of intraocular tumours. Management–surgery (enucleation).