* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Embryonic stem cell wikipedia , lookup
Cell culture wikipedia , lookup
List of types of proteins wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Induced pluripotent stem cell wikipedia , lookup
Nerve guidance conduit wikipedia , lookup
Microbial cooperation wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
State switching wikipedia , lookup
Neuronal lineage marker wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Cell theory wikipedia , lookup
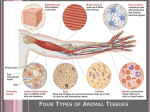
Tissues -four primary tissue types: 1. Epithelial 2. Connective 3. Muscle 4. Neural -however: all tissues in the body develop from three germ layers 1. ectoderm - epithelial + neural 2. mesoderm - connective + muscle + some epithelial 3. endoderm – organs + some epithelial Epithelial Tissue = lining epithelium & glands •multiple functions of epithelial tissue: 1. protection - from dehydration, pathogens 2. synthesis 3. regulation - e.g. body temperature 4. excretion - e.g. waste 5. immune response • lining epithelium = line body surfaces and cavities • glandular epithelium = secretion Lining Epithelium Functions 1. Physical protection: are found on exposed surfaces of the body -protection from abrasion, dehydration, and entrance by toxins 2. Control permeability: every substance that enters the body must cross an epithelial tissue first -permeability varies from location to location -contain pores, channels, transporters and other machinery required for selective permeability -function can be modified by stimuli e.g. hormones can increase ion transport e.g. stress can alter the physical structure and thus permeability 3. Sensitivity: innervated by sensory nerves -many epithelial tissues can detect differences in the environment (e.g. heat, pressure) -convey these changes to the nervous system -one type of specialized sensory epithelium = neuroepithelium -found in special sense organs (ear, eyes, tongue) Epithelial characteristics 1. Cellularity 2. Polarity 3. Attachment 1. to each other 2. to connective tissue 4. Avascularity 5. Regeneration Epithelial characteristics 1. Cellularity: composed almost entirely of cells held together by cell junctions -very little extracellular matrix 2. Polarity: possesses an exposed surface the faces the exterior of the body - apical face -also has an attached base which is anchored to other tissues basal face -the organelles are not uniformly distributed Epithelial characteristics 3. Attachment: attached to underlying tissues via the basement membrane -BM is produced by the basal surface of the cells & connective tissue - comprised of collagen type IV and laminin -the BM is comprised of two layers a. closest to epithelial cell = basal lamina (glycoproteins, laminin and actin) -acts as a barrier to transport b. furthest from the epithelial cell = reticular lamina -collagen IV bundles produced by the underlying connective tissue cells -provides strength Epithelial characteristics characteristics Epithelial 1. Tight junctions: lipid portions of PMs are bound together by interlocking membrane proteins -very tight union - prevents passage of water and solutes between the two cells 3. Attachment: also form extensive connections between each other Epithelial characteristics characteristics Epithelial 2. Gap junctions: two cells held together by proteins called connexons -connexons are channel proteins -materials can freely move between the two cells -passage of materials helps to coordinate the activities of the two cells e. g beating rhythm of cilia 3. Desmosomes: comprised of cellular adhesion proteins/CAMs and proteoglycans -also form plaques and contain cadherins -the plaque attaches to the intermediate filaments of the cytoskeleton (keratin) -several types known: belt, hemi, button -hemidesmosome: attaches the cell to the basement membrane of the tissue -link to a basement membrane protein = laminin Epithelial characteristics 4. Avascularity: do not contain blood vessels -must obtain nutrients via diffusion or absorption 5. Regeneration: damaged cells are replaced through differentiation of stem cells located deep within the tissue -rate of renewal depends on rate of cell death -stem cells = germinative cells -these cells are found closest to the basement membrane -migrate towards the surface and differentiate Classification of Epithelia • catagorizing epithelial tissue types A. # of layers simple = 1 layer stratified = multiple **pseudo = 1 layer B. Cell shape columnar cuboidal squamous Simple Epithelium -relatively thin -cells have the same polarity - nuclei are generally aligned -very fragile - cannot provide mechanical/physical protection -line internal compartments -relatively permeable - absorptive surfaces, secretion, filtration Stratified Epithelium -thicker due to multiple layers -found in areas subject to mechanical and chemical stress e.g. skin, mouth -tougher than simple epi. -organelles do not align Pseudostratified Epithelium -appears to be stratified -yet the basal surface of every cell contacts basement membrane -apical surface of the cells may possess cilia (ciliated epithelium) -often has glandular epithelial cells embedded in it - cells secrete mucus -found lining absorptive organs e.g. respiratory epithelium Squamous Epithelium -tile-like cells - cells are thin, flat and irregular in shape -cells interlock like tiles -simple squamous - most delicate tissue in the body -found in protected regions -many types: mesothelium - lines ventral body cavity (i.e. peritoneum of the abdomen) endothelium - lines heart and vessels Squamous Epithelium -stratified squamous - where mechanical stresses are severe -cells on exposed surfaces (exposed to air) contain keratin an intermediate filament protein that reduces water loss and provides strength = keratinized epithelium -non-keratinized epithelium is tough but must be kept moist e.g. lining of mouth Transitional Epithelium -permits stretching -located in walls of the bladder, renal pelvis and the ureters e.g. bladder wall - when empty the epi. looks as if it has several layers -actual number of layers can be seen upon distension Cuboidal Epithelium -cells are cubes -nucleus is in the center of the cell – very round -simple cuboidal: regions of secretion and absorption e.g. kidney tubules pancreas & salivary glands – secretion of buffers & enzymes thyroid follicles – secretion of thyroid hormones Cuboidal Epithelium -stratified cuboidal: relatively rare -ducts of sweat glands and mammary glands NOT ON PRACTICAL Columnar Epithelium -height is greater than their width -nuclei is close to the BM -simple columnar: provides some protection -also in areas of absorption and secretion Simple columnar epithelium microvilli -usually lines organs involved in secretion and absorption -located in the gallbladder, larger ducts of exocrine glands, gastric pits of stomach, lining of the small intestine -basally located nuclei aligned with one another -frequently the apical face is modified with cellular extensions e.g. microvilli – intestinal lining = brush border -short-lived cells – replaced every 4 to 5 days -frequently found with Goblet cells (intestine and stomach) wandering lymphocytes Columnar Epithelium -stratified columnar: relatively rare -two to multiple layers -only outer layer contains truly columnar cells -protection role NOT ON PRACTICAL Stratified columnar epithelium Columnar Epithelium -pseudostratified columnar: only a single layer -every cell contacts the BM -nuclei are at varying levels - appearance of multiple layers -exposed apical surface typically bears cilia e.g. respiratory epithelium Pseudostratified -these tissues are generally ciliated Type: Description: Function: Simple squamous single layer, flattened cells filtration, diffusion, osmosis lungs, linings of blood vessels single layer, cube-shaped cells secretion, absorption ovaries, kidneys, certain glands single layer, elongated cells protection, secretion, absorption linings of uterus, stomach and intestines single layer, elongated cells protection, secretion, movement of mucus linings of respiratory passages and reproductive multiple layers, flattened cells protection outer layer of skin, oral cavity, throat Location: Simple cuboidal Simple columnar Pseudostratified columnar Stratified squamous Stratified cuboidal Stratified columnar protection multiple layers, cube-shaped cells multiple layers, elongated cells protection, secretion larger ducts of sweat glands salivary glands and pancreas vas deferens, parts of pharynx Glandular Epithelium • epithelial cells specialized to produce and secrete substances •gland = single epithelial cell OR multiple cells •two types of glands: 1) exocrine = secrete into ducts e.g. sweat glands 2) endocrine = secrete directly into bloodstream e.g. thyroid, pituitary ** one gland is mixed - e.g. pancreas •exocrine gland structure: • Unicellular: single-celled glands e.g. goblet cells •Multicellular glands – multiple cells grouped together •Can be classified based on: •1. Mode of secretion •Merocrine •Apocrine •Holocrine •2. Consistency of secretion •Serous •Mucus •Mixed •3. Structure •shape of the secretory portion •branching pattern of the duct • simplest multi-cellular gland is a secretory sheet •e.g. gastric epithelium SIMPLE COLUMNAR with GOBLET CELLS -goblet cells = unicellular exocrine glands that secrete mucus •exocrine gland types 1. serous - watery fluid that contains enzymes e.g. saliva – parotid salivary gland •exocrine gland types 2. mucous - glycoproteins called mucins that absorb water to form a slippery mucus •exocrine gland types 3. mixed - more than one type of gland cell -produces different types of secretions - mucus and serous e.g. submandibular salivary gland Connective Tissue • provides support • binds structures together • fills cavities • produces blood • protects organs •components: matrix + cells -matrix: non-cellular support material -comprised of extracellular protein fibers – mainly collagens e.g. 1. collagen fibers (white) – type I 2. elastic fibers (yellow) 3. reticular fibers – collagen type III 4. fibronectin -plus a ground substance = water + hyaluronan (sugar), proteoglycans and glycoproteins -cells: secrete the matrix -some have become very specialized and make a very specialized matrix Connective Tissues -cell types found in connective tissues: A. fibroblasts: immature cell type found in basic connective tissues -secrete the extracellular matrix -secrete main component of matrix = collagens -also produce hyaluronan = glycosaminoglycan (sugar) that gives the ground substance a viscous quality -also produces the other components of the ground substance e.g. proteoglycans B. adipocytes: mature cell type of adipose tissue -more specialized type of fibroblast – fat storage -fill with lipid upon maturation C. melanocytes: synthesize and secrete melanin -dark, brown pigment that absorb light Connective Tissues D. Macrophages (Fixed): engulf damaged and dead cells by phagocytosis -immune cell -derived from monocytes E. free macrophages: wander rapidly through the connective tissue -called monocytes when circulating in blood F. mast cells: another immune cell -synthesize and secrete histamine - inflammation response -synthesize and secrete heparin - inflammation response G. lymphocytes - immune cells (T and B cells) -differentiate into plasma cells (type of B cells) - antibodies -differentiate into T cell subtypes - assist B cells Connective tissue Matrix fibers: collagen, reticular and elastic 1. Collagen fibers: long, straight and unbranched fibers made of CN type I -very concentrated and dense in tendons and ligaments -long chains of collagen protein subunits forming a triple helix -these helices are wound together - “rope” or a bundle = fibril -fibrils are then stacked together = collagen fiber -triple helix – three subunits = 2 alpha 1 chains + 1 alpha 2 chain e.g. CNI - 2 chains of CNIa1 and one chain of CNIa2 -there are nineteen types of collagen in the body = 80-90% are CNI, CNII, CNIII & CIV Connective tissue: fibers 2. Reticular: made of collagen type III -2 collagen III a1 + 1 collagen III a2 subunits = reticular fiber -reticular fibers interact in a different way – 3D network rather than bundles -thinner than collagen type I fibers - more flexible -abundant in the walls of hollow organs -form a supportive stroma (3D network) that supports the functional cells of these organs 3. Elastic: primarily made up of the proteins fibrillin & elastin -branching and wavy in appearance Classification Embryonic: first to appear = mesenchyme -derived from mesoderm germ layer -cells are star-shaped -matrix - fine protein filaments -Mucus connective tissue - jelly-like, many regions of embryo The way I organize Connective tissues • • • • Loose – areolar CT, fat & reticular Dense – dense (regular, irregular), elastic Supportive – bone & cartilage Fluid – blood (& lymph) Types: 1. Loose 2. Dense 3. Adipose 4. Reticular 5. Elastic 6. Cartilage 7. Bone 8. Blood 9. Lymph Type: Description: Loose connective Cells in fluid-gel matrix Function: Adipose Cells in fluid-gel matrix Reticular Cells in fluid-gel matrix Binds organs together, holds tissues, fluids Protects, insulates and stores Supports Dense Cells in fluid-gel matrix Binds organs together Elastic Cells in fluid-gel matrix Provides elastic quality Hyaline cartilage Cells in solid-gel matrix Elastic cartilage Cells in solid-gel matrix Bone Cells in solid matrix Blood Cells in fluid matrix Supports, protects, provides framework Supports, protects, provides flexible framework Supports, protects, provides framework Transports gases, defends against disease, clotting Loose connective tissues: types 1. Loose Areolar tissue -cells: are mainly fibroblasts, spaced far apart -matrix: sparse collagen I fibers, elastic fibers, mostly ground substance -cushions and can be distorted due to loose organization e.g. beneath the dermis 2. Adipose tissue = fat -cells: adipocytes (fat storing fibroblasts) -matrix: small amounts in between the adipocytes (mainly CNIV) -cushions joints and organs -stores energy -insulates liposuction: suction assisted lipoplasty -removal of SQ fat 3. Reticular tissue: -matrix: thin collagen III/reticular fibers woven into a 3D network – fibers are secreted by reticular cells (specialized fibroblasts) -supports walls of certain organs – e.g. liver, spleen, lymph nodes e.g. liver, spleen NOT ON PRACTICAL Dense connective tissues: types -most of the tissue is densely packed extracellular matrix fibers of collagen type I -often called fibrous or collagenous tissue -type types: 1) dense regular – densely packed collagen I and elastic fibers e.g. tendons, ligaments 2) dense irregular - interwoven meshwork of fibers of CNI and elastic -e.g. dermis of skin, perichondrium of joints and periosteum of bone 1. Dense Regular: -cells: few fibroblasts - matrix: multiple, closely packed collagen fibers – collagen type I -PLUS - fine network of elastic fibers – harder to see e.g. tendons, ligaments 1. Dense Irregular: -cells: few fibroblasts - matrix: similar to dense regular but with little to no organization -gives the tissue strength and flexibility in multiple directions e.g. dermis of the skin Dense irregular tissue • Found in the deepest layers of the dermis = also called the reticular layer (don’t confuse it with reticular tissue) 2. Elastic: -yellow, elastic fibers in parallel or branching networks -walls of larger vessels, airways, hollow organs NOT ON PRACTICAL Supportive Connective tissues: types -cartilage & bone 1. Cartilage: -cells = chondrocytes -matrix = collagen fibers embedded in a gel-like ground- substance -collagen type II -ground substance - water + proteoglycans -proteoglycans - protein + sugars e.g. chondroitin sulfate glucosamine -functions in support, attachment, protection -in developing child - model for future bone (endochondral bone) -avascular tissue - produces anti-angiogenic chemicals (inhibits growth of blood vessels) -therefore diffusion is the main mode of transport Proteoglycan -3 types: 1) Hyaline - most common - “glass” - ends of bones, within joints (synovial, articular), - end of nose, supports respiratory passages 2. Elastic - flexible cartilage - external ears and parts of larynx 3. Fibrocartilage - very tough -> more collagen fibers - shock absorber e.g. intervertebral discs meniscus of the knee Supportive Connective tissues: types 2. Bone = osseous tissue -most rigid connective tissue -cells = osteoblasts, osteocytes -matrix = collagens, proteoglycans, other specialized bone proteins -secreted by osteoblasts – as an unmineralized matrix = osteoid -mineralized as the cells mature into osteocytes -cells are held in lacunae -matrix is laid in concentric circles = lamellae -if lamellae surrounds a central canal = Haversian canal, containing vessels -two types of bone – when the matrix classified by histology 1. Compact - shaft of long bones, outer layer of short, flat and irregular bones -very dense appearing bony matrix -matrix is made up of units called osteons 2. Spongy - ends of bones, middle layer of short, flat and irregular bones -thin bars or “plates” (called trabeculae) of bone separated by irregular spaces filled with red marrow -lighter than compact – yet stronger Fluid Connective tissue: Blood -cells suspended in a fluid matrix = plasma -plasma ~ 55% blood volume -inorganic salts -organic substances - e.g. sugars, proteins -cells: 1) RBCs - biconcave, disc-shaped -contains hemoglobin - 4 globin proteins + heme group (iron) 2) WBCs - fight infection = leukocytes - many types: a. monocytes/macrophages b. lymphocytes - T and B cells c. basophils - histamine d. neutrophils - 1st at infection e. eosinophils - allergic response 3) platelets - blood clotting response Membranes -superficial epithelial sheet + underlying connective layer (called a lamina propria) -cover & protect -four types: 1. serous 2. mucous 3. cutaneous 4. synovial Muscular Tissue •specialized for contraction •very distinct organelles within the cells •3 types •1. skeletal – voluntary muscle •2. cardiac – involuntary muscle •3. smooth – involuntary muscle 3 types: 1) striated/skeletal – voluntary nervous control -repeating banding patterns of actin & myosin = striated appearance -mature cells = multi-nucleated cells – made from fusion of hundreds of muscle cells called myocytes -cells are very long – sometimes called muscle fibers -cannot divide – but new cells form from differentiation of myogenic stem cells = satellite cells -attached to bones via tendons 3) cardiac - involuntary control - only found in heart -cells are striated but uninuclear = cardiomyocytes -incapable of dividing – PLUS there are no satellite cells -therefore damaged heart muscle cannot be regenerated -cells are connected end to end by intercalated discs -these discs are areas of communication between cardiomyocytes through gap junctions -the discs also help channel the forces of contraction 2) smooth – involuntary control -lines blood vessels, airways and organs -non-striated -control their own rate of contraction through action of pacemaker cells -nervous system can also control contraction -slow, sustained contraction -spindle shaped cells - single nucleus/uninucleated -many types of smooth muscle cells found in many organs (i.e. not the same in every organ) -many kinds of smooth muscle cells incapable of division – no stem cells SMOOTH DENSE -you could confuse dense irregular connective tissue and smooth muscle – so be careful!! -there are more cells/nuclei in smooth muscle Neural Tissue (Nervous Tissue) •specialized for the conduction of electrical impulses from one body region to another •two types of neural cells: 1) neurons 2) glial cells 1) glial cells: astrocytes, oligodendrocytes, microglia -supportive function to neurons 2) neuron: cell body, dendrites, axon with an axon terminal -therefore cell has polarity -dendrite receives and/or generates signal -cell body = soma -axon - conducts the nerve impulse -forms a synapse with: another neuron or a muscle cell