* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Political abuse of psychiatry in Russia wikipedia , lookup
Autism spectrum wikipedia , lookup
Spectrum disorder wikipedia , lookup
Substance use disorder wikipedia , lookup
Conduct disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Conversion disorder wikipedia , lookup
Mental disorder wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
History of psychiatry wikipedia , lookup
Asperger syndrome wikipedia , lookup
Abnormal psychology wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Child psychopathology wikipedia , lookup
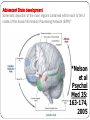
Adolescent Psychiatry Dr Nasima Matine Specialist Registrar in Child and Adolescent Psychiatry November 2010 Adolescent Disorders What is an adolescent? Adolescent development Psychiatric disorders in adolescence Talking to adolescents -CASC The Adolescent is travelling a long way without seeming to go very far………… ‘no man’s land’ Adolescence is..????? Adolescence = latin ‘growing up’ Covers age 13 – 19 Unique time between: Dependent child..................->Independent adult ‘no man’s land’- developing adult bodies; finding a role, acquiring more rights, finding balance independence and being somebody’s child Sturm and drang ‘storm and stress’or is this a myth???? Time of turmoil Inevitable conflict Parents / Society . It’s his / her Hormones doctor Necessary for Development Wayne and Waynetta What does it mean to be an Adolescent………..????? Drive Relationships Alcohol/ Drugs Sex / Pregnancy Exams Leaving home Work / University Adolescence Peers v Parents Voting Money What can you do, at what age??? Criminal responsibility- 10y Criminal responsibility- age may Gillick competence PT work- 14-16y FT work- 16y Sex gay /straight- 16y Drive- 17y Alcohol- 18y Smoke- 18y Vote- 18y Legal Adult-18y be raised Gillick Competence- accept not refuse treatment 2008- Channel 4 study: 1/3 15y sexually active Work- prevent child labour When women 1st got vote UK had be 30+y A right of passage North American Indians- Vision Quest Africa- traditionally learning skills manhood: hunting, physical stamina & strength, passage adulthood decided by Elders - (now changed) UK- age 18, party, alcohol, new legal rights Developmental Changes in Adolescence Emotional Physical 4 Domains of change Social Cognitive Spots, breasts, menstruation, hair, muscles, Sexual desire, the sex talk?………Embarrasing?????? PUBERTY PHYSICAL Changes Bodily Systems • ANS, liver metabolism • Consequences medication Brain Development • SYNAPTIC PRUNING • ? imbalance subcortical limbic & PFCx heightened Emotionality Adolescent Brain development Schematic depiction of the main regions contained within each of the 3 nodes of the Social Information Processing Network (SIPN)* *Nelson et al Psychol Med 35: 163-174, 2005 A schematic depiction of the main regions contained within each of the three nodes of the social information processing network (SIPN). Brain regions that make up the detection node include the fusiform face area, the superior temporal sulcus and the anterior temporal cortex. These regions are involved in carrying out basic perceptual processes on social stimuli and are highlighted in green. Brain regions that make up the affective node include the amygdala, hypothalamus, nucleus accumbens, and bed nucleus of the stria terminalis and are highlighted in red. These regions interact with the detection node to imbue social stimuli with emotional significance. Brain regions that make up the cognitive-regulation node include the dorsomedial prefrontal cortex and the ventral prefrontal cortex are depicted in blue. This node is involved in inhibiting motivated response tendencies and understanding the psychological perspective of other individuals as in theoryof-mind tasks. The gray arrows between the three nodes indicate that these nodes are interactive. Normal Neurocognitive Development Synaptic Pruning Neuronal Proliferation What architecture will be left to play with? 10 15 Age 20 25 2430 Complex abstract thought - Justice, Morality Body image Less concrete Discourse & Arguement Growing verbal ability Compare Self to others COGNITIVE Developing a Sense Self I am unique 12-19 Psychosocial Crisis Identity v Role Confusion Who am I? Where am I going? >11y Formal Operational thought Change egocentricity abstraction Thinking, Reason, Conceptualise Ethics & Justice Erikson Piaget COGNITIVE Freud Superego Socially appropriate behaviour Conscience: right & wrong Fit into society Developmental changes in adolescencecognitive development Christie, D. et al. BMJ 2005;330:301-304 Copyright ©2005 BMJ Publishing Group Ltd. Developing thought Piaget 2-7 years: Pre-operational stage [e.g. not getting the principal of conservation] 7-11 years: Concrete operational stage [getting conservation, but not abstract concepts] >11 years: Formal operational thought [concepts, ideals, ethics, justice…] c.50% of population probably never achieve formal operational thought. Identifying emotions Who do I talk to?? Complexity Emotions Controlled Listened to Lonely Respected Angry Judged Criticised Rejected Frustrated EMOTIONAL Cared for Supported Capacity regulate emotionsmaturity Sense of Identity Exploratory Behavior - drugs / alcohol Emotional Separation from parents SOCIAL Peer identification Changes nature relationships Parents Partners Education Communicating with adolescents Useful questions to gauge developmental level What degree parental separation achieved? What identities are evolving? How is past/future perceived? Do they perceive themselves as responsible for self? Can they weigh consequences of choices? How are sexual/affectionate interests expressed? Communicating with adolescents . • See young people by themselves as well as with their parents- make sure to document that you’ve asked if they want to be seen alone, if refuse. • Be empathic, respectful, and non-judgmental, • Assure confidentiality in all clinical settings- be aware when confidentiality may need to be broken, tackle this with sensitivity • Be yourself. Don't try to be cool or hip—young people want you to be their doctor, not their friend • Try to communicate and explain concepts in a manner appropriate to their development- think about what words you use. Face - to - Faceness Authenticity Working Adult-Adolescent interface Rapidly shifting positions No jargon Energy Coping Dunno, Boring… Working with Adolescents Honesty Validation- self validation Hope- chance to alter the trajectory Why is a knowledge of adolescent development important ? Background of developmental changes: impacts upon: Nature/ presentation of illness Consequences of illness Relationship between the adolescent patient and healthcare providers Is the presentation age appropriate???? Think LD, sexualised behaviours Psychiatric disorder and development in adolescence Disorder delay aspect of development e.g. Anorexia delays puberty Delay in development/difficulty negotiating tasks of adolescence Disorder e.g. Delay in puberty predisposes to anxiety/depression Dysfunctional System surrounding the adolescent disorder and difficulties negotiating developmental tasks eg. Chaotic family leads to academic/social delay-school refusal or conduct disorder Psychiatric disorder in adolescence How do we differentiate from normal functioning? Impact Persistence Duration Eg- on emotions/relationships/school/biological symptoms depression Trajectory and Vulnerability Social Function and the Time-critical nature of Adolescence Social Function Independent living skills Educational qualifications Etc. Available Support Complexity of social and emotional challenges Adolescent “Discomfort Zone” MENTAL DISORDER Time 11yrs 18 yrs Mental Health Problems and disorders in adolescents Common: Depression Anxiety ADHD conduct disorder substance misuse disordered eating (inc eating disorders) risky behaviours e.g. Self harm Less common: Psychoses PTSD Autism Epidemiology psychiatric disorders: Isle of Wight Study Classic study 2303 14 and 15 y olds. Rutter 1976. Main conclusions have stood test of time: 1. Definite psychiatric disorders in 10% of sample. Another 10% self reported marked ‘misery’ 2. Most were emotional and conduct disorders. Depression: 2% (42% M; 48% F misery). 3. Just under ½ with disorders at 14 had them at 10y. 4. Only minority were alienated from parents. Commoner if psychiatric disorder. Management: Bio-Psycho-Social Best choice takes into account individual and family: Medications Psychological treatments: CBT, DBT, IPT, Family therapy, group therapy Educational liaison/support Behavioural management: parents/children Case 1 JM is 16. Took overdose ibuprofen. Sexually abused by uncle at 8. Been in CAMHS services since age 11. Problems: recurrent depression, impulsive behaviour-self harm/fire setting/ alcohol. School refusal- lost over 50% last year. Problems with relationships Mum and dad incapacitated-mum abdo problems, dad depression/physical problems. Acts as ‘carer’ in the home; fiercely protective of sibs Factors to consider Therapeutic alliance: trust and choice Previous treatments Family system-maintaining factors Cognitive sophistication ? Developing diagnoses Harm reduction strategies SIRSE: Symptoms, Impact, Risk, Strengths, Explanatory model Management Antidepressants Psychology-CBT/IPT Psycho-education Family work Sexual abuse-specialist work e.g. New Beginnings School liaison Case 2 LG 15 y old hardworking girl. Perfectionist traits, difficulty fitting in, social anxiety. Sibling issues: rivalry, dieting. BMI 16. Eating minimally. Calorie counting. Body image problems. Missed 2 periods. Very weak/fatigued. Fainted before. Poor concentration-grades falling behind. Issues to consider Willingness to engage: where on cycle of change Family context: sister dieting, parental value Peer and social ideas about food/being accepted Physical health complications: menstruation/bone loss/hypotension/lethargy/electrolytes. Education Psychological functioning. Management options Psycho-education Physical: weight monitoring and restoration, blood tests and physical checks. Psychological challenge: motivational enhancement work Family work CBT/antidepressants-anxiety School liaison Case 3 14 y old girl with polysubstance misuse. GP asks ‘does she have underlying schizophrenia?’. Threatened family with knife. Talking to herself at times. Chaotic behaviour. Prostituted self. Risky situations. Parents extremely worried about safety. Think underlying anxiety disorder Social services crisis team involved. Issues to consider Motivational level to change behaviour Willingness to engage Safety issues Family issues: 5 y old brother, mum ‘nervous breakdown’ Underlying problems: previous notes and treatments School work Management options Psycho-education: drugs, sex and risk Inter-agency working: substance misuse team, social services key worker to ensure safety Underlying illnesses-explore School liaison Psychological work-motivational enhancement Practical monitoring: drugs diaries Parental support Further reading BMJ series of ABC Adolescence CASC 1A Eating Disorder Lucy is a 14 year old girl She is a national championship swimmer and wants to be in the Olympic Team Her mother is her coach Her GP refers her, as he is concerned she is loosing weight Take a history to elicit signs and symptoms of an eating disorder CASC 1a –Key points FOOD METHODS WL Current eating pattern – ‘take me through what you’d eat through the day?’ Avoidance fatty foods Rules about eating- can sometimes be quite OCD in nature Binging Over exercise- sit ups, running spot, up & down stairs Restriction Vomiting Laxatives, diet pills Rate W/L BODY IMAGE Feel overweight, other people say I’m not Do you feel need to loose more weight PHYSICAL Ammenorrhoea, cold, chest pain, SOB, exhausted, hair, nails, dry skin MOOD Often co-morbid depression Suicide CASC 1b Eating Disorders You have just assessed Lucy You have a made a diagnosis of Anorexia Nervosa Please speak with her mother and explain the diagnosis and management options to her mother You have Lucy’s permission to speak to her CASC 1b Eating Disorders AN: morbid fear fatness, distorted body image self induced WL AIMS Weight restoration Treat physical complaints – monitor weight, bloods Managing anorexic thoughts Improve level functioning Support family TREATMENT OPTIONS OP – Dietician / Psychoeducation, CBT, FT / Meal support IP – Unable to restore weight Physical complication, rapid WL, psychiatric risk CASC 2a Overdose Mike is a 16 years old He recently split up with his boyfriend and felt that he didn’t want to live anymore He took an overdose of 20 paracetamol tablets with some of his mother sleeping pills Take a relevant history Perform a risk assessment CASC 2a Overdose Details OD Planned / spontaneous, how get medication, note, did weight until his was left alone, how did get AE How does feel now? Regret, Active/ Passive suicidal ideation, self harming thoughts Previous OD Psychiatric: Mood, Psychosis Relationships –friends, parents (abuse??), partners Support Drugs / Alcohol Ask if it’s ok to speak with his parents?? CASC 2b Overdose You have just seen Mike Please present your findings to your Consultant Discuss your plan CASC 2b Overdose Succinct summary age, name, what happened, any psychiatric illness, risk Plan discuss whether manage OP or IP, think about criteria for this If OP, what does he need? Frequency OPA, Psychological input, medication Risk management plan for him: CAMH in hrs, out of hrs AE / out of hrs GP service; identify friends /family member to say ‘I struggling’ Think about importance liaising with family- CASC 3a Fire Setter Georgie is a 15 years old She is a looked afterchild and lives in a care home She recently set fire to the paper bin in her bedroom The police were called and she was brought to AE The staff are very concerned and say she has been behaving oddly Please take a history CASC 3a Fire Setter This is a station about being sensitive to the needs of the individual and taking a careful history & also think about risk Georgie is a LAC child, she was brought into the care system aged 13, after it was found out that her stepfather was sexually abusing her. Her mother knew this was happening. Her emotions switch rapidly, she cuts to relieve distress, she often feels really angry. Sometimes she hears a voice telling her to harm herself but there is no clear evidence of psychosis She has set fire to a bin once before, after seeing her mother It was recently her birthday and her mother sent her a card