* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download the molecular basis of apoptosis
Survey
Document related concepts
Transcript
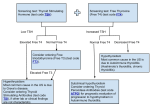
Hypothyroidism Diagnosis and Management dr Pandji M,SpPD, KEMD ,FINASIM Definition : Hypothyroidism is a clinical syndrome resulting from a deficiency of thyroid hormone which in turn results in generalized slowing down of metabolic processes. Etiology of Hypothyroidism Primary : 1. Hashimoto’s thyroiditis : a. With goiter b. “Idiopathic” thyroid atrophy, presumably end-stage autoimmune thyroid disease, following either Hashimoto’s thyroiditis or Graves’ disease c. Neonatal hypothyroidism due to placental transmision of TSH-R blocking antibodies. 2. Radioactive iodine therapy for Graves’ disease 3. Subtotal thyroidectomy for Graves’ disease or nodular goiter 4. Excessive iodide intake (kelp, radiocontrast dyes) 5. Subacute thyroiditis 6. Rare causes in the USA a. Iodide deficiency b. Other goitrogens (Adapted : Greenspan FS, 2001) Secondary: Hypopituitarism due to Pituitary Adenoma Pituitary Ablative Therapy or Pituitary Destruction Tertiary : Hypothalamic Dysfunction ( rare ) Peripheral resistance to the action of thyroid hormone Pharmacologic Hypothyroidism I. Thyroid Hormone Synthesis Inhibitor – Tionamide : MTU, PTU, Carbimazol – Perchlorat, Sulfonamid – Yodide (Expectoran, Amiodaron) – Lithium II. Thyroid Hormone Destruction – Phenitoin & Phenobarbital – Enterohepatic pathway inhibitor of thyroid hormone Colestipol, Colestyramin The Hypothalamic-Hypophysial-Thyroid Axis Hypothalamus TRH T3 Portal system Anterior pituitary T4 “Free” T4 T3 T3 + TSH Tissue + T4 Thyroid Grades of Hypothyroidism 200 TSH mU/L 100 40 10 (Adapted : Greenspan FS, 2001) FT4 pmol/L T3 nmol/L Individual and median values of thyroid function tests in patients with various grades of hypothyroidism. Discontinuous horizontal lines represent upper limit (TSH) and lower limit (FT4, T3) of the normal reference ranges. 4.0 15 12 9 6 3 0 2.5 2.0 1.5 1.0 0.5 0 Subclinical Hypothyroldism Mild Overt Hypothyroldism Hypothyroldism Pathogenesis Thyroid Hormones Synthesis of hyaluronate fibronectin and collagen by fibroblast Accumulation of glucosaminoglycans mostly hyaluronic acid in interstitial tissues Hydrophilic substance increase capillary permeability to albumin Interstitial edema Skin (Wiersinga, 2004: The thyroid and its disease) Many organs (heart muscle, striated muscle) Hypothyroidism in adult (myxedema) Physiologic Effect of Thyroid Hormone Endocrine Tissue growth Lipid & carbohydrate metabolism Brain maturity Heat production & Oxygen consumption Skeletal neuromuscular THYROID Gastrointestinal Cardiovascular Sympathetic Hematopoitic Pulmonary DIAGNOSIS HYPOTHYROIDISM Clinical Hypothyroidism FT4 TSH FT4 TSH FT4 N TSH FT4 TSH N/ FT4 N TSH N Primary Hypothyroidism Subclinical Hypothyroidism Secondary Hypothyroidism Normal TRH Test FT4 TSH FT4 TSH No Response Primary Hypothyroidism Tertiary Hypothyroidism Secondary Hypothyroidism Management of Hypothyroidism Pay attention to : 1. Initial dosage of thyroxin 2. The way to increase thyroxin dosage The Purpose of Hypothyroidism Treatment 1. To relief symptom and sign 2. To normalize metabolism 3. To normalize TSH, level but not supressed 4. To normalize T3 & T4 levels 5. Avoid risk and complications Principles to conduct thyroxine replacement therapy 1. The more severe the disease, the lower the initial and the slower the increase dosage of thyroxine 2. The older the patients should more pay attention especially in cases of angina pectoris, congestive heart failure, cardiac arythmia Thyroid Hormone available on the market: • L-Thyroxin (T4) Euthyrox L-Triiodothyronine (T3) Thyroid Extract The best is L-Thyroxin • Should be taken before meals • Dosage Recommendation : – L-T4 : 112 ug/d or 1,6 ug/kgB.W (RRJ : Djoko Moeljanto, 2002) – L-T3 : 25-50 ug Starting dose of thyroxin • There is no evidence base for determining how thyroxine therapy should be initiated, but it is customary to prescribe 50 ug daily, increasing to 100 ug daily after 3-4 weeks. • Measurement of serum T4 and TSH at two months after starting will dictate any further adjustment of dosage. • In the elderly, symptomatic ischemic heart disease, starting dose of 25 ug/d is advisable with increments of 25 ug/3-4 weeks. • A full replacement dose of 100-150 ug/d. (Toff AD, 2001; Thyroid International) The TSH level can be used as a guideline to establish the substitution dosage of thyroxin TSH level Thyroxin 20 uU/ml 50-75 ug/d 44-75 uU/ml 100-150 ug/d 90% Hypothyroidism cases used LT4 100-200ug (RRJ : Djoko Moeljanto, 2002) Variation in dosage of thyroxin Once thyroxin therapy is established it is good practice to review patients annually and measure serum TSH not only to ensure compliance but also to determine whether and adjustment of dose is required. Situation in which an adjustment of the dose of thyroxine may be necessary Increased dose required Use of other medication Phenobarbitone Phenytoin Carbamazepine Rifampicin *Sertraline *Chloroquine Cholestyramine Sucralfate Aluminium hydroxide Ferrous sulphate Dietary fibre supplements increased thyroxine clearance interference with intestinal absorption Pregnancy Oestrogen therapy increased concentration of serum thyroxine-binding globulin After surgical or iodine-131 ablation of Graves’ disease reduced thyroidal secretion with time Malabsorption e.g. coelic disease Decreased dose required Aging decreased thyroxine clearance Graves’ disease developing in patient with long-standing primary hypothyroidish switch from production of blocking to stimulating TSH-receptor antibodies * mechanism not fully established (Adapted : Toff AD, 2001) Suggested management of patients taking thyroxine replacement therapy, depending upon pattern of thyroid function test results and clinical symptoms TSH T4 T3 Symptoms Action normal normal or raised normal or raised normal none none normal present normal or raised normal or raised normal or raised normal none increase thyroxine by 25-50 g daily until serum TSH is suppressed but ensure T3 unequivocally normal none normal yes* normal < 0.05 mU/l < 0.05 mU/l < 0.05 mU/l high normal yes* or no or raised reduce thyroxine by 25-50 g daily to restore normal TSH reduce thyroxine by 25-50 g daily to restore unequivocally normal T3 Symptoms of possible undertreatment might include tiredness and weight gain * Symptoms of possible overtreatment might include unexplained atrial fibrillation and reduced bone mineral density (Adapted : Toff AD, 2001) Summary • • • • • • Some basic principles to remember that active hormone is free hormone. Cells metabolism are based on FT3 not FT4 Diagnosis established by symptom, sign, FT4 and TSH Should be careful to start and increase the dosage of thyroxine especially in case of angina pectoris,CHF,arythmia Drug of choice is L-thyroxine Target of treatment is normal TSH level