* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Epidemology
Lyme disease microbiology wikipedia , lookup
Gastroenteritis wikipedia , lookup
Urinary tract infection wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Neonatal infection wikipedia , lookup
Human microbiota wikipedia , lookup
Chagas disease wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Infection control wikipedia , lookup
Schistosomiasis wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Transmission (medicine) wikipedia , lookup
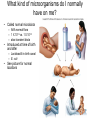
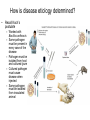
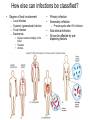
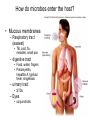
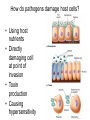
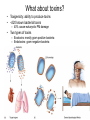
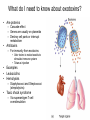
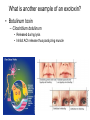
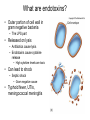
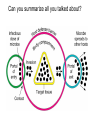
Principles of Disease What are some terms I should know? • Pathology • Etiology • Pathogenesis – Manner by which a _________ develops • Infection – Invasion of body by pathogenic microorganisms • Disease – Change from state of health • Epidemiology: when, where and how transmitted What are some epidemiological terms I should know? • CDC – US source for epi. Info. • Morbidity: incidence of notifiable diseases • Mortality What other epidemiological terms should I know? • Occurrence of disease – Incidence • Rate at which people contract a disease (new cases) – Prevalence • Total number who have the disease at a specified time • Includes old, continuing cases and new cases – Emerging infectious diseases: West Nile Virus What other epidemiological terms should I know? – Sporadic – – – – Outbreak: SARS Pandemic: influenza, 1918 Endemic: common cold Epidemic: HIV?, obesity… see next slide Trends in Overweight* Prevalence (%), Adults 18 and Older, US, 1992-2003 1992 1995 1998 Less than 50% 50 to 55% 2003 More than 55% State did not participate in survey *Body mass index of 25.0 kg/m2or greater Source: Behavioral Risk Factor Surveillance System, CD-ROM (1984-1995, 1998) and Public Use Data Tape (2003), National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention, 1997, 2000, 2004. What kind of microorganisms do I normally have on me? • Called normal microbiota – AKA normal flora – 1 X 1013 vs. 1 X 1014 – also transient biota • Introduced at time of birth and after – Lactobacilli in birth canal – E. coli • See picture for normal locations What do normal flora do for me? • Microbial antagonism – E. coli bacteriocins – Vaginal LAB (lactic acid bacteria) maintain low pH • Flora are symbiotic – Commensalism • Corynebacteria on eye – Mutualism • E. coli in large intestine makes vitamin K • But some microorgs can become pathogenic under certain conditions! – E. coli in urinary tract – Called opportunistic pathogens – Some exhibit parasitism and are not beneficial! How is disease etiology determined? • Recall Koch’s postulate – Worked with Bacillus anthracis – Same pathogen must be present in every case of the disease – Pathogen must be isolated from host and cultured (pure) – Cultured pathogen must cause disease when injected – Same pathogen must be isolated from inoculated animal Are there exceptions? • Yes – Some can’t be cultured (e.g. Treponema pallidum) – Thus, must use alternative methods • Legionellosis • Sometimes many bacteria cause same symptoms – Pneumonia • Sometimes one bacteria causes several diseases – Streptococcus pyogenes • Scarlet fever, strep throat, osteomyelitis How are infectious diseases classified? • Symptoms: subjective • Signs: objective – Syndrome: suite of symptoms or signs associated with a disease • Communicable disease • Contagious disease • Noncommunicable disease – C. tetani What else should I know about diseases? • • • • • Acute disease Chronic disease Subacute Latent disease Nosocomial infections Does vaccination help? • Yes! • If ~70% are vaccinated, low likelihood unvaccinated will contract disease – Called herd immunity How else can infections be classified? • Degree of host involvement – – – – Local infection Systemic (generalized) infection Focal infection Bacteremia • Sepsis: bacteria multiply in the blood • Toxemia • Viremia • • Primary infection Secondary infection – Pneumocystis after HIV infection • • Sub-clinical infection All can be affected by predisposing factors What are the stages of disease development? • Incubation period • Prodromal period • Period of illness • Period of decline • Period of convalescence During which stages can a disease spread? • Transmission can occur: – In any period, depending on pathogen • Infection reservoir is needed – Human • Those infected • Carriers also – Animal • zoonoses – Or nonliving • Soil: B. anthracis, Clostridium ssp. • Water: V. cholerae, S. typhi How are diseases transmitted? • Contact transmission – Direct – Indirect • Fomite: nonliving object that helps spread disease – Droplet:SARS • Vehicle transmission – Food, water, soil, air, blood, drugs, fluids, body parts • Vectors – Arthopods • Mechanical • Biological What about nosocomial infections? • Increased in last 30 yrs – 4th leading cause of death in US! • Three critical factors How can nosocomials be controlled? • Hand washing is most important • Clean respirators, humidifiers, bathtubs • Disposable tools, bandages, etc. Mechanisms of Pathogenicity How do microbes enter the host? • Mucous membranes – Respiratory tract (easiest) • TB, cold, flu, measles, small pox – digestive tract • Food, water, fingers • Poliomyelitis, hepatitis A, typhoid fever, shigellosis – urinary tract • STDs – Eyes • conjunctivitis How do microbes enter the host? • Skin – Sweat glands, hair follicles, on keratin • Parenteral route – Injured or penetrated barriers • Preferred entry route How many microbes does it take to cause disease? • Depends on virulence – ID50: infective dose for 50 percent of population – B. anthracis • Skin: ID50 = 10-50 endosopres • Inhaled ID50 = 10,000-20,000 • Gastro ID50 = 250,000-1,000,000 – Toxin potency = LD50 (lethal dose…) Bacterial pathogenic properties What happens after entry into the host? • Attachment – Usually via adherence • Stick to surface receptors (typically sugars) – Biofilm production • Dental plaque: mineralized biofilm – Rolling biofilm How do pathogens penetrate tissues? • Capsules – Prevents phagocytic cells from attaching – S. pneumoniae with capsule = virulent • Cell wall – S. pyogenes: m-protein • attachment and antiphagocytosis – N. gonorrhoeae: opa • Attachment, along with help from fimbriae – Mycobacterium tuberculosis • Cell wall waxes • Resist digestion after phagocytosis • animation How do pathogens penetrate tissues? • Enzymes – Coagulases • Clot fibrinogen • Protect against phagocytosis • Staphyloccocus – Kinases • Streptokinase (fibrolysin) Streptococcus pyogenes • Staphylokinase Staphylococcus aureus – Hyaluronidase • Digest matrix in connective tissue • Clostridium perfringens: gas gangrene How do pathogens damage host cells? • Using host nutrients • Directly damaging cell at point of invasion • Toxin production • Causing hypersensitivity What about toxins? • Toxigenicity: ability to produce toxins • ~220 known bacterial toxins – 40% cause eukaryotic PM damage • Two types of toxins – Exotoxins: mostly gram positive bacteria – Endotoxins: gram negative bacteria What do I need to know about exotoxins? • Are proteins – Cascade effect – Genes are usually on plasmids – Destroy cell parts or interrupt metabolism • Antitoxins – For immunity from exotoxins • Alter toxins to make toxoids to stimulate immune system • Tetanus injection • Examples • Leukocidins • Hemolysins – Staphylococci and Streptococci (streptolysins) • Toxic shock syndrome – Via superantigen T-cell overstimulation What is another example of an exotoxin? • Botulinum toxin – Clostridium botulinum • Released during lysis • Inhibit ACh release thus paralyzing muscle What are endotoxins? • Outer portion of cell wall in gram negative bacteria – The LPS part • Released on lysis – Antibiotics cause lysis – Endotoxins cause cytokine release • High cytokine levels are toxic • Can lead to shock – Septic shock • Gram negative cause • Typhoid fever, UTIs, meningococcal meningitis Can you summarize all you talked about?