* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Regulation
Coronary artery disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
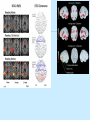
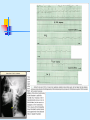
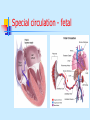
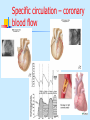
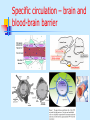
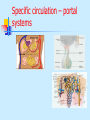
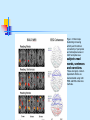
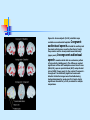
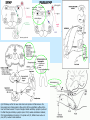
Special circulation - fetal Fetal circulation birth Changes in pressure closure of foramen ovale • Umbilical artery ligation 2x increase of peripheral resistance increase of blood pressure in left heart and systemic circulation • Lung inflation + vasodilatation 5x decrease of resistance decrease of blood pressure in right heart Changes in pO2 closure of ductus arteriosus • pO2 from 20 to 100 mm Hg vasoconstriction closure 1-8 days later + fibrotization after 1-4 months Vascular spasm closure of ductus venosus Change HbF into HbA Relative blood distribution Specific circulation – coronary blood flow Specific circulation – brain and blood-brain barrier Specific circulation – portal systems Specific circulation – countercurrent mechanism Specific circulation – liver and intestine Hepatic sinuses Blood supply to enterocytes The goals of regulation To increase blood flow where necessary (working muscle, digestion, gland secretion etc) To regulate temperature skin vasodilatation/vasoconstriction resulting in heat spare/loss To maintain constant blood flow where necessary and/or functional (brain, heart, … kidney, lungs) principles heart (cardiomotor) inotropy, bathmotropy, chronotropy, dromotropy blood (volume) vasomotor vasodilatation x vasoconstriction β-2 adrenergic receptor↑Gs activity → ↑AC activity → ↑cAMP → ↑PKA activity → phosphorylation of MLCK → ↓MLCK activity → dephosphorylation of MLC ↑α1 adrenergic receptorActivation of Gq --> ↑PLC activity --> ↑IP3 and DAG --> activation of IP3 receptor in SR --> ↑intracellular Ca2+ Regulation of blood circulation Mechanisms of regulation: Local Humoral (chemical) – O2, CO2, H+ Nervous Enzymatic and hormonal General/systematic Fast = short-term (regulate blood pressure) Slow = long-term (regulate blood volume) – several days Local chemical regulatory mechanisms The most obvious in the heart and the brain Goal: autonomic regulation of resistance by organ based on its metabolic needs Principle: accumulation of products of metabolism (CO2, H+, lactic acid ) or consumption of substances necessary for proper function (O2) directly affects smooth muscles of vessels and induce vasodilatation Figure 1: Brain maps illustrating increasing activity and functional connectivity of perisylvian and extrasylvian areas in both hemispheres as subjects read words, sentences and narratives. These emergent, contextdependent effects are demonstrated using both fMRI and EEG coherence methods. Figure 44: Across-subjects (N=10) z-statistic maps overlaid on an anatomical template. Congruent audiovisual speech activated the auditory and the visual cortical areas, as well as the inferior frontal, the premotor and the visual-parietal areas bilaterally (upper panel). speech Incongruent audiovisual caused a similar but more extensive pattern of brain activity (middle panel). The difference reached significance in three left hemisphere areas: Brocat’s area (BA44/45), superior parietal lobule (BA7) and prefrontal cortex (BA10) (lower panel). In the contrast ’Congruent > Incongruent’ no statistically significant voxels were detected. Activation images were thresholded using clusters determined by voxel-wise Z>3.0 and a cluster significance threshold of p<0.05, corrected for multiple comparisons. Local nervous The most obvious in the skin and mucous Goal: central regulation of blood distribution Principle: Autonomic nervous system Sympaticus Vasoconstriction – activation of α receptors in vesselsnoradrenalin (glands, GIT, skin, mucous, kidneys, other inner organs) Vasodilatation – activation of β receptors in vessels – adrenalin (heart, brain, skeletal muscles) Parasympaticus - Acetylcholin Vasoconstriction – heart Vasodilatation – salivatory glands, GIT, external genitals Local enzymatic and hormonal Platelets Endothelium balance Thromboxan A – vasoconstriction Prostacyclin – vasodilatation Endothel-derived relaxing factor = NO (arginin =>nitric oxid synthetase=>NO=>G-cyclase =>cGMP => vasodilatation) Endothelin1 most potent vaso/venoconstrictor, receptors in smooth muscles, besides circulation in kidney GFR. Activated by Angiotensin-II, catecholamines etc Local enzymatic and hormonal Plasma protein - Kinin ↑ = vasodilatation bradykinin and kallikrein A role in inflammation, coagulation, pain and gland secretion (sweat, salivatory, pancreas -> increases blood flow locally) Hormones of adrenal medula: adrenalin (vasodilatation), noradrenalin (vasoconstriction) General fast & slow regulatory mechanisms General fast (short-term) regulatory mechanisms Nervous autonomic reflexes Baroreflex glomus caroticum, glomus aorticum Afferentation: IX and X spinal nerve Centre: medulla oblongata, nucleus tractus solitarii Efferentation: X spinal nerve (ps), sympathetic fibers Effectors: heart (atriums), vessels Effect: After acute increase of blood pressure – activation of receptors – decrease of blood pressure (vasodilatation, decrease of effect of sympathetic nerves) SYMP PARASYMP right: Pathways within the lower brain stem and spinal cord that subserve the baroreceptor and chemoreceptor reflex control of the sympathetic outflow to the heart and blood vessels. The open triangles indicate excitatory synaptic inputs and the filled triangles inhibitory synaptic inputs. CVLM, caudal ventrolateral medulla; IML intermediolateral cell column in the spinal cord; KF, Kölliker-Fuse nucleus in pons; NTS, nucleus tractus solidarus. Carotid sinus massage Purpose Sinus, in this case, means an area in a blood vessel that is bigger than the rest of the vessel. This is a normal dilation of the vessel. Located in the neck just below the angle of the jaw, the carotid sinus sits above the point where the carotid artery divides into its two main branches. Rubbing the carotid sinus stimulates an area in the artery wall that contains nerve endings. These nerves respond to changes in blood pressure and are capable of slowing the heart rate. The response to this simple procedure often slows a rapid heart rate (for example, atrial flutter or atrial tachycardia) and can provide important diagnostic information to the physician. Description The patient will be asked to lie down, with the neck fully extended and the head turned away from the side being massaged. While watching an electrocardiogram monitor, the doctor will gently touch the carotid sinus. If there is no change in the heart rate on the monitor, the pressure is applied more firmly with a gentle rotating motion. After massaging one side of the neck, the massage will be repeated on the other side. Both sides of the neck are never massaged at the same time. General fast (short-term) regulatory mechanisms Humoral mechanisms Adrenalin – β receptors → vasodilatation → ↓ peripheral resistance → blood from skin and GIT to skeletal muscles, heart and brain → ↑ minute heart volume Noradrenalin – α receptors → vasoconstriction → ↑ blood pressure Renin-angiotensin – activated by ↓ pressure in vas afferens slow (long-term) Regulatory mechanisms of water and electrolytes exchanges autoregulation of total blood volume by kidneys Increase of ADH (vasopressin) When ↓ blood volume → ↓ of filtration pressure in glomeruli → ↓ production of urine → ↑ volume of circulating blood → ↑ blood pressure ↑ ADH → ↑ of the permeability of collecting ductus for the water → water is reabsorbed → ↑ volume of circulating blood → ↑ blood pressure Increase of Aldosterone ↑ aldosterone → ↑ reabsorbtion Na+ and water → ↓ volume of urine → ↑ volume of circulating blood → ↑ blood pressure Intracardial regulatory mechanisms (2) Ionotropic effect of heart rhythm ↑ heart frequency → ↑ amount of Ca2+ that goes into heart cells → ↑ Ca2+ available for tubules of sarkoplasmatic reticulum → ↑ Ca2+ that is freed by each contraction → ↑ strength of contraction Intracardial regulatory mechanisms (1) Frank-Starling’s law = initial length of the fibers is determined by the degree of diastolic filling of the heart, and the pressure developed in the ventricle is proportionate to the total tension developed. The developed tension increases as the diastolic volume increases until it reaches a maximum, then tends to decrease. Ganong: Review of Medical Physiology Myocardium – correlation length x tension beta receptor activation blockage Frank-Starling’s law = initial length of the fibers is determined by the degree of diastolic filling of the heart, and the pressure developed in the ventricle is proportionate to the total tension developed. The developed tension increases as the diastolic volume increases until it reaches a maximum, then tends to decrease. Ganong: Review of Medical Physiology