* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Interesting ECGs
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Transcript
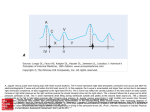
Interesting ECGs Sarah Gutman History of the ECG 1876 Marey uses the electrometer to record the electrical activity of an exposed frog's heart. 1878 British physiologists John Burden Sanderson and Frederick Page record the heart's electrical current with a capillary electrometer and shows it consists of two phases 1891 British physiologists William Bayliss and Edward Starling of University College London improve the capillary electrometer. They connect the terminals to the right hand and to the skin over the apex beat and show a "triphasic variation accompanying (or rather preceding) each beat of the heart". 1893 Willem Einthoven introduces the term 'electrocardiogram' at a meeting of the Dutch Medical Association. History of the ECG In 1924 Einthoven was awarded the Nobel prize in Physiology or Medicine for his discovery of the mechanism of the electrocardiogram. 60 year old woman with 3 hours of chest pain Acute Posterior MI ST depression in leads V1 - 3 tall R wave tall upright T wave in leads V1 -3 usually associated with inferior and/or lateral wall MI 80 year old with dizziness Digoxin shortened QT interval characteristic down-sloping ST depression Possible Effects of Digoxin on the ECG Depression or sagging of the ST segment which is concave in an upward direction; it looks as if the ST segment alone has been pulled down. These changes are more apparent in the lateral precordial leads, although they may also be seen in the limb leads. The T waves are often flattened and the QT interval (ST segment) shortened. Usually the PR interval is slightly prolonged as a result of an enhanced vagal effect upon the AV node. In some cases there are abnormalities of the U wave (prominent or inverted) which may be due to digitalis itself, or can be secondary to hypokalemia. Ventricular premature beats Atrial tachycardia (automatic, accelerated, or non-paroxysmal) Atrioventricular junctional tachycardia (automatic or non-paroxysmal) Accelerated junctional rhythm (automatic or non-paroxysmal) Accelerated idioventricular rhythm (automatic or non-paroxysmal) Ventricular tachycardia Bidirectional tachycardia (usually a junctional tachycardia with alternating right and left bundle branch block) Ventricular fibrillation Abnormal conduction due to digitalis toxicity includes the following: Sinus bradycardia Sinus pause or arrest Sinoatrial block First degree atrioventricular block Second degree atrioventricular block (Mobitz 1 or Mobitz 2) Third degree atrioventricular block Combined arrhythmia and conduction abnormalities due to digitalis toxicity include the following: Atrial tachycardia with atrioventricular junctional block (PAT with block) Sinus bradycardia associated with atrioventricular junctional tachycardia Accelerated junctional rhythm associated with underlying atrial fibrillation (atrial fibrillation with regularization) Atrial flutter, atrial fibrillation, and Mobitz type II second degree AV block are the least likely of all the possible abnormalities. 55 year old man – routine ECG in cardiology outpatients Heterotopic Heart Transplant two distinct QRS morphologies two distinct rates 36 year old lady with recurrent blackouts VT + AICD polymorphic ventricular tachycardia large deflection (arrowed) is the defibrillator discharging. Following the defibrillation a dual chamber pacemaker can be seen. A 75 year old lady with loud first heart sound and mid-diastolic murmur AF + RVH AF There is the suggestion of right ventricular hypertrophy.: tall R waves in the right precordial leads (V1 and V2 deep S waves in the left precordial leads (V5 and V6); a R:S ratio >1 in V1 and V2 is suggestive of RVH right axis deviation and RV1 >7 mm. The combination of Atrial Fibrillation and Right Axis Deviation on the ECG suggests the possibility of mitral stenosis. A 75 year old lady with loud first heart sound and mid-diastolic murmur P Mitrale and RVH P mitrale or left atrial enlargement is manifest as broad notched (M shaped) p wave in lead II, classically seen in mitral stenosis. The broad negative P wave in V1 is also indicative of left atrial overload. qR pattern in V1 with T wave inversions in anterior leads is suggestive of right ventricular hypertrophy. A 79 year old man with 5 hours of severe, central, crushing chest pain Acute myocardial infarction in the presence of left bundle branch block The sequence of repolarization is altered in LBBB, with the ST segment and T wave vectors being directed opposite to the QRS complex. These changes may mask the ST segment depression and T wave inversion induced by ischemia. On the other hand, the diagnosis of an acute MI or ischemia can occasionally be made in a patient with underlying LBBB if certain STT changes are seen, particularly if the ST-T vectors are in the same direction as the QRS complex as in the Sgarbossa criteria described below. The presence of deep T wave inversions in leads with a predominantly negative QRS complex (eg,V1-V3) is highly suggestive of evolving ischemia or MI. ST elevations in leads with a predominant R wave (as opposed to QS or rS waves) are also strongly suggestive of acute ischemia. Pseudonormalization of previously inverted T waves is suggestive but not diagnostic of ischemia. Attempts to Improve diagnosis of AMI in the presence of LBBB Serial ECG changes — 67 percent sensitivity ST segment elevation — 54 percent sensitivity Abnormal Q waves — 31 percent sensitivity Initial positivity in V1 with a Q wave in V6 — 20 percent sensitivity but 100 percent specificity for anteroseptal MI Cabrera's sign — 27 percent sensitivity overall, 47 percent for anteroseptal MI Cabrera's sign refers to prominent (0.05 sec) notching in the ascending limb of the S wave in leads V3 and V4. However, there may be a high degree of interobserver variability in accurate identification and their sensitivity is quite low. 78 year old woman with central chest pain radiating to jaw Second degree atrioventricular block: Mobitz type I (Wenckebach block) + inferior STEMI progressive PR interval prolongation preceds a nonconducted P wave The site of block is in the AV node in most cases (70 to 75 percent), with the remaining cases involving the His bundle, bundle branches, or fascicles Mobitz type I block (due to ischemia of the AV node) is not an uncommon complications of an inferior myocardial infarction (given the RCA supplies the AV nose in over 90% of individuals). 80 year old woman in pre-admission clinic for CABG and AVR in 2 weeks Bifasicular block Abnormal left axis deviation qR complex in the lateral limb leads (I and aVL) rS pattern in the inferior leads (II, III, and aVF) Bifascicular block refers to conduction disturbances below the atrioventricular (AV) node in which the right bundle branch and one of the two fascicles (anterior or posterior) of the left bundle branch are involved. In this case the left anterior fascicle is blocked and combined with the RBBB this is called a bifascicular block. Posterior Fascicular Block A 90 year old woman with syncope Trifasicular Block Complete right bundle branch block Left anterior hemiblock Long PR interval = bifasicular block with prolongation of the PR interval If the right bundle branch and both the anterior and posterior fasicles of the left bundle branch were blocked, this would be complete heart block. Progression to Complete Heart Block Probably infrequent Natural history of "high-risk" bundle-branch block: final report of a prospective study. N Engl J Med. 1982 – largest study, progression of 1% per year. Smaller studies report 16-75% 80 Year Old Woman with dizzy spells AF + Complete Heart Block Fibrillary waves of atrial fibrillation and no P waves Regular ventricular rhythm 19 Year Old Girl with Chest Pain Pericarditis Stage I (acute phase): Diffuse concave upward ST segment elevation in most leads, PR depression in most leads (may be subtle), and sometimes notching at the end of the QRS complex. 70 year old man with slow palpitations Atrial Flutter 5:1 Block 40 year old English Tourist with Central Chest Pain and Shortness of Breath Pulmonary Embolus Sinus tachycardia Incomplete right bundle branch block Possible old inferior myocardial infarction S1Q3T3 pattern consistent with acute pulmonary embolism (a large S wave in lead I, a Q wave in lead III, and an inverted T wave in lead III indicates acute right heart strain). The most common ECG finding in the setting of a pulmonary embolism is sinus tachycardia 54 year old farmer with hypertension LVH Criteria Cornell criteria: Add the R wave in aVL and the S wave in V3. If the sum is > 28 mm in males or > 20 mm in females, then LVH is present. Modified Cornell Criteria: Examine the R wave in aVL. If the R wave is > 12 mm in amplitude, then LVH is present. Sokolow-Lyon Criteria: Add the S wave in V1 plus the R wave in V5 or V6. If the sum is > 35 mm, then LVH is present. Romhilt-Estes LVH Point Score System: If score = 4, then LVH present with 30-54% sensitivity. If score > 5, then LVH is present with 83-97% specificity. Amplitude of largest R or S in limb leads >20 mm – 3 Amplitude of S in V1 or V2 > 30 mm – 3 Amplitude of R in V5 or V6 > 30 mm - 3 ST and T wave changes opposite QRS without digoxin – 3 ST and T wave changes opposite QRS with digoxin – 1 Left Atrial Enlargement – 3 Left Axis Deviation – 2 QRS duration > 90 milliseconds – 1 Intrinsicoid deflection in V5 or V6 > 50 millisecond - 1 26 year old international medical student practicing ECG technique Brugada pseudo-RBBB and persistent ST segment elevation in leads V1 to V3 40 year old man on frusemide and sotolol presents with collapse Torsades de pointes Polymorphic VT associated with a prolonged QT interval is termed torsades de pointes (TdP). TdP can occur in patients who have a congenital long QT syndrome or acquired QT prolongation from drug therapy, hypomagnesemia, or hypokalemia. 91 year old man with palpitations Sinus Tachycardia ST depression consistent with ischaemia