* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download hemodynamics
Cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
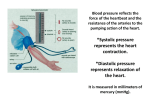
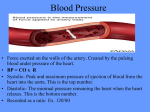
Cardiovascular Assessment II Yuriy Slyvka MD, PhD Cardiovascular Assessment Cardiac Output • Blood Pressure – Systolic / Diastolic • Pulse Perfusion Blood Pressure Systolic - Normal 95 - 140 mmHg Diastolic - Normal 60 - 90 mmHg Children vary with age Neonate 60 - 90 over 30 - 60 mmHg Systolic Maximum pressure exerted on arterial wall during ventricular contraction Diastolic Pressure in vasculature during ventricular relaxation Indirect Blood Pressure Measurement via Cuff Wrap blood pressure cuff around upper arm Auscultate over artery in antecubital fossa Inflate cuff rapidly Deflate cuff slowly while listening Mechanism Cuff inflated - occludes artery - no sound Slowly deflate cuff - first sound = systolic Continue to deflate cuff until sound disappears = diastolic Tapping sounds heard with each heart beat called Korotkoff’s sounds (Ko rot kof) Technique Usually use non-dominant arm Inflate to approx 160 mmHg Drop pressure approximately 3 mmHg/sec Standard adult cuff 5 inches wide Pediatric 3 inches wide Sources of Error Resulting in High BP Measurements Cuff too narrow • Width of cuff approx 40% circumference of arm Applied too tight or too loose Excessive cuff pressure • should start 30 mmHg above systolic Pressing stethoscope too tightly over artery will affect diastolic pressure Hypertension BP persistently > 140-160 / 90 Secondary means cause is known • May be a side-effect of medication Primary Hypertension means cause is unknown Hypotension BP < 95 / 60 Late sign of hypovolemia, cardiac failure, shock 90 / 60 not uncommon in young females Low blood pressure results in inadequate perfusion Brain Heart - (70% coronary artery perfusion occurs during diastole) (Diastolic pressure < 50 mmHg compromises perfusion of heart) Kidneys Low blood pressure a late sign of circulatory problems Normal compensatory mechanisms maintain blood pressure initially When these fail - pressure falls Use blood pressure to calculate Mean Arterial Pressure S-D+D 3 MAP is average pressure for circulation Indicator of adequate tissue perfusion Normally 70 - 105; 90 average Mean arterial pressure (MAP) MAP < 60 mmHg inadequate Resistance = Pressure gradient / Flow or re-arranged: MAP = C.0. x SVR Two factors determine blood pressure Cardiac output = stroke volume x heart rate Systemic vascular resistance (SVR) Stroke Volume (SV) determined by Preload Contractility Afterload Increased Preload Increases SV Preload = filling volume of ventricles Increased blood volume stretches muscle fibers Increases strength of contraction Requires longer time for ventricular filling Increased Contractility Increases SV Contractility = force of muscle contraction No change in muscle fiber length Increase force of contraction over same time period Inotropic drugs Decreased Afterload Increases SV Afterload = resistance ventricles contract against Primarily systemic vascular resistance Systemic vasodilation reduces afterload Factors afftecting Systemic Vascular Resistance Radius of arterioles Blood volume Blood viscosity (Hematocrit) Factors affecting Cardiac Output primarily affect systolic blood pressure Ex. Exercise using large muscle mass (legs) will require increase in cardiac output to supply more oxygen to working muscles Will see an increase in systolic Diastolic will stay the same or decrease since arteries of large muscle mass dilated Factors affecting Systemic Vascular Resistance will primarily affect diastolic pressure Ex. Exercise using small muscle mass (arms) Vasoconstriction of large muscle mass not being used Vasoconstriction increases vascular resistance Diastolic will increase Maximal Heart Rate correlates with Maximal O2 Consumption HR max = 220 - age 75% HR max ------ 60 % VO2 max 80 ------- 70 90 ------- 82 Aerobic exercise 75 - 80% HR max Heart Rate or Pulse - Evaluate for Rate Rhythm Strength Normal Heart Rate 60 - 100 Adults 90 - 120 Children 70 - 170 Newborns < normal = bradycardia > normal = tachycardia Tachycardia One of the cardinal signs of hypoxemia Increasing heart rate increases cardiac output Increase oxygen delivery to tissues Increasing HR increases C.O. Until HR > 150 C.O. decreases due to inadequate filling time Rhythm Regular or irregular Irregular beat may indicate arrhythmias Strength Bounding? • Arteriosclerosis Weak and thready? • shock Pulsus Paradoxus Strength decreases with spontaneous inhalation Increases with exhalation normal unless extreme Common in COPD Seen in 50% patients with pericarditis Pulsus Alterans Alternating strong and weak pulses May be sign of left ventricular failure Not related to respiratory disease Pulse Pressure Systolic - Diastolic Normal 35 - 40 mmHg < 30 mmHg pulse hard to detect Decreasing pulse pressure early sign of inadequate circulating blood volume Can estimate systolic blood pressure if can palpate Carotid pulse - then systolic is at least 60 mmHg Femoral 70 mmHg Radial 80 mmHg Pulse sites Radial Brachial Carotid Femoral Dorsalis pedis Check radial pulse before and after administering therapy Aerosol medication may produce side-effects First cardinal sign of hypoxemia is tachycardia After taking pulse, continue palpating pulse as count respiratory rate Assessment of Perfusion (microcirculation) Peripheral skin temperature • cold extremities indicate reduced perfusion Urine Output • one of the best indicators of C.O. and arterial pressure • < 20 ml/ hr oliguria ( o lig uria) Sensorium • Brain sensitive to lack of oxygen and/or lack of glucose • Both depend on blood supply to the brain - perfusion • Confusion may signal inadequate perfusion or hypoxemia Determine patient’s level of consciousness (LOC) Oriented to person - know who they are Oriented to place - know where they are Oriented to time - know what today is, what year Will typically see “Alert and oriented to PPT” in chart Summary Patient assessment includes evaluating patient’s cardiovascular system • Cardiac Output • BP/Pulse • Perfusion Many of the therapeutic interventions of respiratory care will affect the cv system