* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Human Development
Sex allocation wikipedia , lookup
Evolution of sexual reproduction wikipedia , lookup
Baby Gender Mentor wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Causes of transsexuality wikipedia , lookup
Human embryogenesis wikipedia , lookup
Drosophila melanogaster wikipedia , lookup
Developmental biology wikipedia , lookup
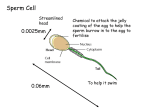
Human Biology (BIOL 104) Talk Ten: Human Development Chapter 17 How do we develop? • On ovulation day, egg and sperm fuse to form zygote. • Zygote divides, implants onto uterus and grows into Embryo and hangs out for about 9 months. • Embryo decides it is time to breathe air, fetal adrenal glands trigger contractions and out comes baby. • Baby grows grows grows into child, child undergoes puberty and becomes adult. • Adult lives, works, reproduces (perhaps), gets gray hair and croaks. REMEMBER!!!!!!!!! • If viable sperm contact an egg at the time of ovulation fertilization will occur. • This “typically” occurs on day 14. Remember Day 1 is first day of menstruation. • The fertilized egg will implant on day 6. • The new embryo will begin to produce HCG-Human Chorionic Gonadotripin. • HCG maintains the corpus luteum and allows the production of progesterone and estrogen until the placenta takes over this task. Remember - Fertilization • Egg must develop and be released on ovulation day. • Egg must be correctly positioned in the oviduct and attract sperm. • Vaginal tract must activate sperm. • Hormonal levels must be exact. • Ensure only one sperm joins with egg. Remember - Fertilization • Sperm must undergo capacitation--process of activation by substances in female vaginal tract fluids. • Sperm motor from vagina up through cervix, uterus, to the oviduct. • Many sperm attempt fertilization, only one succeeds (except for twins). Development before Implantation • Fertilization • Cleavage: successive rounds of cell division. A one cell zygote--2 cell--4 cell--8 cell-. • Cleavage occurs in the oviduct. • Morula: 16 cell stage--enters the uterus • . • Key cell differentiation step: – Trophoblast – Inner Cell Mass • • • • Development before Implantation Blastocyst Hollow ball of cells. Each cell is called a blastomere. Inner cell mass--become the embryo. • Trophoblast--Incredible Altruistic Cells! – Escape from the Zona Pellucida – Digest through Endometrium – Initiate HCG secretion – Form the Placenta Gastrulation • Truly the most important day of your life! • Process of forming 3 germ layers--this process requires cell movement. • Each germ layer forms specific tissues and organs – Ectoderm--(blue)--will form skin and nervous system. – Mesoderm--(red)--will form muscles, kidneys, connective tissue, and reproductive organs. – Endoderm--(yellow)--will form digestive tract, lungs, liver and bladder. Figure 12.8b Extraembryonic Membranes • Establishing extraembryonic membranes is critical. These membranes protect the embryo and link embryo to mother: – Amnion--provides fluid environment for fetus. – Chorion--becomes the placenta--site of gas and nutrient exchange with mother. – Allantois--becomes unbilical blood vessels The Placenta • Nutrient and Gas Exchange between fetus and mother. • Fetal side--from chorion. • Maternal side--from uterine tissue • Blood of fetus and mother do not mix. • Fetal chorionic villi project into maternal blood. • Exchange occurs across membranes. • Umbilical cord stretches between placenta and fetus. Pregnancy: • Fetal period – Week 8 through birth – Rapid growth – 5th month – skeletal muscles active – 6th month – gains weight The Prenatal Period – Last 3 months – fetal brain cells rapidly divide – GI and respiratory systems last to develop Overview of Human Development Mammary glands • Are present in both males and females. • Are not a component of the reproductive system. • Contain epithelial tissue that secrete milk. • Milk drains into a series of ducts opening at the nipple. Birth--Hormonal Control • Fetus--Hypothalamus—Cortisol Releasing Hormone • • Fetus--Anterior pituitary --ACTH • • Fetus--Adrenal Gland produces Cortisol and DHEAS. • Cortisol from fetus converted to prostaglandins in placenta--these begin contractions. • DHEAS from fetus converted to estriol in placenta--these promote oxytocin in mother. • Oxytocin (from Posterior pituitary) in mother begins labor. – Cervical stretching--positive feedback. Birth--Stages • Stage I: • water breaks • cervix dilates • Stage II: Birth--Stages • Contractions increase to every 12 min, baby emerges. • Episiotomy (cut vaginal orifice) can prevent ripping. Baby emerges, umbilical cord cut. Birth--Stages • Stage III: • Placenta is delivered about 15min after birth. • Remember our altruistic trophoblast cells! Twins/Multiple Births • Two types – Monozygotic • From one egg • Identical – Dizygotic • From two eggs • Fraternal • Not identical Identical twins • One zygote • Splits in 2 • No one knows why! • Completely random = does NOT run in families • Same exact DNA • Nature’s clones Fraternal Twins • 2 separate eggs get fertilized with 2 different sperm cells • More than one egg got released during ovulation • Siblings – Can be sisters – Brothers – Brother and sister • Tends to run in families Conjoined Twins • Used to be called “Siamese” twins • First well known case was in Siam • Identical twins that never completely separated during development • Sometimes can be separated, depending on what is shared. Birth Defects • 1 in 16 newborns (6.25 out of 100) born with birth defect. Many minor, but some serious or fatal. • 20% of defects (3.125 out of 1000) are genetic. • Causes: – neural tube closure problems--folic acid. – drugs--aspirin, caffeine, alcohol, vitamin A creams, cigarette smoke, cocaine, heroine, thalidomide,. – pathogens--rubella, HIV, STDs, listeria.. Genetic screening • Amniocentesis-remove fluid from amniotic cavity. • Analyze cells for genetic abnormalities. Performed 15th 17th week of pregnancy Genetic screening • Chorionic villi sampling--remove villi by suction, test for genetic abnormalities. • Performed 5th to 12th week of pregnancy, chance of risk for fetus Genetic screening • Screening eggs-obtain eggs and test a polar body (eggs “clone”). • If polar body is normal, fertilize and implant the egg. Sexual life cycles • Haploid Gametes join to form a zygote • Somatic cells divide by Mitosis to produce adult organism • Meiosis produces gametes in sex cells Genes on sex chromosomes determine Sex and sex-linked traits • Micrograph of the chromosomes of an organism paired and numbered. • Used to check for chromosomal abnormalities in individuals. Sex Determination • All embryos start on a neutral or "indifferent" path. The 4 week old embryo is indifferent • By 7 weeks, the SRY (sexrelated) gene encoded by the short arm of the Y chromosome begins to roar! • Testis determining factor (TDF) converts progesterone to testosterone Sex Determination • Testis-determining factor (TDF) is a general term for the gene (or product thereof) that results in maleness in humans and some other species. • Its expression directly or indirectly causes the development of primary sex cords, which will later develop to seminiferous tubules. • These cords form in the central part of the yet-undifferentiated gonad, turning it into a testis. • The testis then starts secreting testosterone and the Mullerian Inhibiting Substance Sex Determination • Indifferent embryos have two sets of ducts: • Müllerian ducts--will be come the future oviducts--thus female. • Wolfian ducts--will become the future vas deferens--thus male – dependent on testosterone for its continued development • The testes also produce an antiMüllerian hormone that promotes regression of the Müllerian ducts – without SRY, the indifferent embryo will naturally develop into a female Sex Determination Sex Determination DAX1 (dosage-sensitive sex reversal, adrenal hypoplasia critical region, on chromosome X, gene 1) is a nuclear receptor protein Encodes a protein that lacks the normal DNA-binding domain contained in other nuclear receptors. The encoded protein acts as a dominantnegative regulator of transcription of other nuclear receptors, including steroidogenic factor 1. This protein also functions as an anti-testis gene by acting antagonistically to SRY. Sex Determination •Two copies of DAX (double X) inactivate SRY, thus this individual would be genetically male, but look female. Sex Determination Sex Determination Figure 2.16 (3) Sex Chromosomal Disorders • Turner Syndrome – XO only one sex chromosome • Short, thick neck and stature • Do not undergo puberty, or menstruate, • no breast development • Kleinfelter Syndrome – XXY • • • • • Testis and prostate underdeveloped No facial hair Brest development Long arms and legs: big hands and feet Can be mentally handicapped Androgen Insensitivity Syndrome • Androgen, also called androgenic hormones or testoids, is the generic term for any natural or synthetic compound, usually a steroid hormone, that stimulates or controls the development and maintenance of male characteristics in vertebrates by binding to androgen receptors. • This includes the activity of the accessory male sex organs and development of male secondary sex characteristics. • Androgens are also the original anabolic steroids and the precursor of all estrogens, the female sex hormones. • The primary and most well-known androgen is testosterone. Androgen Insensitivity Syndrome • The effects that androgens have on the human body --virilization, masculinization, anabolism, etc. --- are not brought about by androgens themselves, but rather are the result of androgens bound to androgen receptors • the androgen receptor mediates the effects of androgens in the human body. • Likewise, under normal circumstances, the androgen receptor itself is inactive in the cell until androgen binding occurs •Figure by Jonathan Marcus, based on an original drawing by Dr. Marianne D Sadar (Meehan KL, Sadar MD. Front Biosci. 2003 May Androgen Insensitivity Syndrome • Normal function of the androgen receptor. • Testosterone (T) enters the cell and, if 5-alpha-reductase is present, is converted into dihydrotestone (DHT). • Upon steroid binding, the androgen receptor (AR) undergoes a conformational change and releases heat shock proteins (hsps). •Figure by Jonathan Marcus, based on an original drawing by Dr. Marianne D Sadar (Meehan KL, Sadar MD. Front Biosci. 2003 May Androgen Insensitivity Syndrome • Normal function of the androgen receptor. • Phosphorylation (P) occurs before and / or after steroid binding. • The AR translocates to the nucleus where dimerization, DNA binding,and the recruitment of coactivators occur. • Target genes are transcribed (mRNA) and translated into proteins •Figure by Jonathan Marcus, based on an original drawing by Dr. Marianne D Sadar (Meehan KL, Sadar MD. Front Biosci. 2003 May Complete Androgen Insensitivity Syndrome • It is a genetic disorder that causes XY fetuses to become impassive to androgens or male hormones. • They are born appearing externally female even if they are genetically male. • Inside there is an undersized vagina with no uterus, fallopian tubes, or ovaries. • There are testicles in the abdomen or the groin area. • Complete androgen insensitivity syndrome is frequently confirmed at puberty when an individual is supposed to start menstruating but does not. Partial Androgen Insensitivity Syndrome • Characteristically leads in “confusing sexual organ.” • The clitoris is enlarged or, otherwise, the penis is undersized and exhibits hypospadias. – the opening of the urethra is situated on the underside of the penis instead of at its tip • Partial androgen insensitivity may possibly be fairly frequent, and has been recommended as the reason for sterility in a lot of men whose sexual organs are of characteristically male form. • People with confusing sexual organs have normally been subjected to surgery during infancy. – Surgery on the sexual parts is necessary only when it is essential for the health of the child. Issues of sex determination • So, clearly being Male or Female isn’t as cut and dry as people have been led to believe! • 17 out of 1,000 people are really neither – XY, but Female anatomy – XX, but Male anatomy – Both Female and Male anatomy • Other genes, such as testosterone receptor on chromosomes other than X and Y chromosomes have a role in sexual development Issues of sex determination • So, some people fall between Male and Female – Due to chromosomal variation – Variations in SYR gene – Testosterone receptor gene • All of the different variations are known as intersex – These people are altered surgically to make them conform to one sex or the other • Should there be five genders instead of two? The end! Any questions?