* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Slide 1 - The University of Sydney
Survey
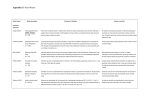
Document related concepts
Drug design wikipedia , lookup
Pharmacognosy wikipedia , lookup
Drug discovery wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Prescription costs wikipedia , lookup
Drug interaction wikipedia , lookup
Neuropharmacology wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Transcript
Cannabis © 2009 University of Sydney Module learning outcomes To be able to: • Describe the mechanism of action, pharmacology • Describe its desired and undesired effects • Describe the therapeutic uses of cannabis • Describe the prevalence of cannabis use • Assess cannabis use clinically, predisposing factors, and associated harms • Understand the management of cannabis use disorders Case study: Mark • Mark is a 34 year old who comes for help with his cannabis use. He is smoking 10 cones a day. He has tried to cut down on several occasions but finds he can’t bear his edginess and poor sleep when he stops. • Is there such a thing as cannabis withdrawal? • Would you say Mark is addicted to cannabis? • What harm is Mark’s cannabis use likely to cause? • Are there treatments available for cannabis dependence? Historical perspective • Cannabis cultivated in China 6000 yrs ago • American Indians widely used cannabis 1000 yrs ago • Multipurpose and hardy crop yielding – – – – Cooking oil Edible seeds Animal fodder Hemp fibre • Psychoactive drug Courtwright, Forces of Habit, 2001 Pharmacology and mechanism of action What are cannabinoids? • Group of >60 dibenzopyran chemicals found in leaves and flowering tops of female cannabis plant (Cannabis sativa and Cannabis indica) • Some common cannabinoids are: In the plant: In your body (endogenous): Synthetic: Δ9 – THC 2-arichidonyl glycerol (2 – AG) CP 55,940 Δ8 – THC anandamide HU – 210 cannabidiol and cannabinol Structure of THC and synthetic analogs Lipophilic side chain Most potent analog: 100s times more potent than THC Mode of cannabis action • Two specific cannabinoid receptors – CB1 - brain and peripheral tissues – CB2 - immune system • Linked to G-proteins with diverse downstream signalling pathways • Euphoria results from stimulation of mesolimbic dopaminergic neurons, like other drugs of abuse Neurotransmitter Receptor Influences nt release Neurotransmitter Receptor Post-synaptic release of endog. cannabinoid Central mediation of some of the effects of cannabinoids Cannabinoid receptor antagonists • SR 141716 (Rimonabant), LY320135 and AM281 • All have marked selectivity for CB1 receptors over CB2. Myths: for & against • Harmless, and safer than the licit drugs • You can’t get addicted to cannabis • It’s a gateway drug (leads to ‘hard drugs’) • Rising potency in recent years, leading to more harms • ‘it causes schizophrenia’ Commonly used terms • Cannabis is the preferred general term. • Other terms: marijuana, ganga, mull, grass, hash, pot, weed, dope • Types of cannabis, in increasing strength – Leaf << Head << Oil/resin • Diverse methods of smoking – joint = cigarette of cannabis, typically 0.5g – cone: smoked via a water pipe (bong), typically 0.25g – bucket bongs – vaporisers (increased ammonia levels via this method) Is high potency a problem? • For naive users: – higher risk of dysphoric & psychotic symptoms • higher rates of discontinuation? – higher rates of accidental injury? • For regular users: – lower respiratory risk, if users titrate dose – higher risk of dependence? • especially among adolescents – more cognitive impairment? THC content: 1990 - 2008 United States Non-normalized average THC % vs year of confiscation 12 10 THC % 8 6 4 2 0 90 91 92 93 94 95 96 97 98 99 00 01 02 03 04 05 06 07 08 Year National Institute on Drug Abuse, Potency Monitoring Project Quarterly Report, No. 100, 2008. Effects of Cannabis Why do people use cannabis? • To experience euphoria or perceptual distortions • Because others do so • To relieve mental symptoms – negative symptoms of schizophrenia – anxiety • To relieve physical symptoms – eg nausea, anorexia, cancer & HIV Typical effects of cannabis • Mental effects – Euphoria, relaxation and wellbeing – Increased appetite (‘munchies’) – Talkativeness, disinhibition • Physical effects – Vasodilator (systemic and portal) – Bronchodilation (short-term effect only) • Highly variable – Many people dislike it and discontinue use – Influenced by surroundings Prevalence of Cannabis Use Patterns of cannabis use in Australia 2007 National Drug Strategy Household Survey Lifetime illict drug use cannabis 33.5 inhalants 3.1 meth/amphetamine 6.3 hallucinogens 6.7 ecstasy 8.9 heroin 1.6 cocaine 5.9 0 5 10 15 20 25 30 35 40 Percent AIHW, 2008 Changes in drug use over time (ever used) 2007 National Drug Strategy Household Survey 50.0 1991 1993 1995 1998 2001 2004 2007 37.5 % 25.0 12.5 .0 Cannabis Heroin Amphetamines Cocaine Ecstasy AIHW, 2008 Changes in recent drug use over time 2007 National Drug Strategy Household Survey 50.0 1991 1993 1995 1998 2001 2004 2007 37.5 % 25.0 12.5 .0 Cannabis Heroin Amphetamines Cocaine Ecstasy AIHW, 2008 Cannabis use across age groups 2007 National Drug Strategy Household Survey Ever used % Recent use 2007 National Drug Strategy Household Survey 60 50 Percent 40 30 20 10 0 14-19 20-29 30-39 40-49 50-59 60+ Age AIHW, 2008 Changing patterns of cannabis use • Weekly or more frequent use accounts for 96% of use • Earlier initiation of use: – increased risk of dependence • More use among vulnerable groups • remote indigenous people • persons with schizophrenia • conduct disordered adolescents Natural history of cannabis use in Australia • Initiation in mid teens • Most use intermittently – Surveys capture relatively low daily use • Discontinue in mid to late 20s – Impact of ‘marriage, mortgages & children’ • Persistent use relatively rare – Predicted by early initiation – Heavier use Drug use with increasing age Chen, K. & Kandel, D.B. 1995, Am J Pub Health, 85(1):41-47. © American Journal of Public Health. Reprinted with permission. To obtain the full article, reprints of the article, or subscribe to the American Journal of Public Health, visit www.ajph.org Concept of gateway drug use • Sequence of drug involvement – alcohol & tobacco precede cannabis, leading in turn to heroin & other drugs – harms derive from ‘hard drugs’ • BUT < 5% of those who’ve tried cannabis go on to use ‘harder’ drugs • Progression predicted by: – earlier initiation & heavier use – other psychosocial issues Why the association with other drugs? • Selective recruitment to use – at risk & troubled youth more likely to use • Peer networks – regular users affiliate with peers who use – peer culture supportive of drug use & crime • Drug markets – provide opportunities to use other illicit drugs • Genetic vulnerability to drug dependence? Harms of cannabis use Acute adverse effects • Anxiety, dysphoria, panic, paranoia – especially among naive users • Cognitive and psychomotor impairment while intoxicated • Psychotic symptoms (probably rare) – high doses of THC – vulnerability Accidental injury • Impaired performance on complex tasks • Reduced risk-taking (in contrast to alcohol) – awareness of impairment • Simulated driving impaired • Epidemiological evidence – dose related risk of MVA1 – measurement of impairment not reliable – confounding with alcohol 1Ramaekers, et al, 2004, DAD, 72: 109 -119 Adverse effects of chronic use • Chronic intoxication • Dependence • Effects on adolescent development and school performance • Motivation, learning, memory • Respiratory disease • Effects of maternal & paternal? use • Schizophrenia & psychosis Cannabis and adolescent development • Concerns – Effect on educational performance, especially in heavier users – Progression to “harder” drugs? • Issues – Heavy use uncommon – Causal attribution • Other drug use • User characteristics Respiratory effects Position statement of RACP • Cannabis is primarily smoked • Cannabis smoke similar to tobacco smoke • Most also smoke tobacco and the differential effects are difficult to study • There is every reason to believe that the long-term harms are similar to those of tobacco Taylor & Hall, 2003, Intern Med J. 33(7):310-3 Evidence • Cannabis-smoking causes chronic bronchitis in 20-30% (cough, sputum) • Histopathological changes in bronchi: acute and chronic bronchitis and dysplasia • Impaired immunological responses – pulmonary alveolar macrophages • Increased health service use • Decreased respiratory function not proven Public health impact of respiratory risks • In comparison with tobacco – Small in public health terms – Large in terms of personal risk • A consequence of smoking as a route – Encourage non-smoking use? • Most smoke tobacco also – amplification of respiratory risks Cannabis and psychosis • ‘Cannabis psychosis’ – Toxic psychosis i.e. as a direct result of the cannabis intoxication – Functional psychosis i.e. persists once cannabis no longer present • Cannabis as a risk factor for schizophrenia – Precipitation – Exacerbation • High prevalence of cannabis use – Especially at period of risk for psychosis – Complicates causal attribution ‘Cannabis Psychoses’ • i.e. as a direct result solely of heavy cannabis use • Conflicting opinions – clinical observations – limited case-control evidence • Probably exist but severe toxic pschosis rare – either require large doses of THC or vulnerability • Mild dose-dependent paranoia common • Can’t do a randomised controlled trial ! Cannabis Psychosis: NSMHWB Unadjusted OR: 2.86 95% CI: 1.37, 5.99 Adjusted OR: 2.39 95% CI: 1.21, 4.72 Those with cannabis dep. 2.4 times more likely to report psychosis symptoms. Hall & Degenhardt, 2000, ANZJP Cannabis and Schizophrenia Consistent evidence that: • Cannabis use can precipitate schizophrenia – Four longitudinal studies in 3 countries – Consistent RR ~ 2 and AR ~ 13% • Cannabis can exacerbate schizophrenia – – – – Clinical evidence Retrospective studies Prospective studies Interventions studies • But were these people susceptible and likely to develop this illness in time anyway? Role of endocannabinoid system in schizophrenia • Schizophrenics have heightened levels of anandamide in their CSF than controls • Schizophrenics (that have never taken cannabis) have increased CB1 receptors in their forebrain compared to matched controls. Evidence for Precipitation • • • • Swedish conscript study N = 50,000 N times used cannabis by age 18 Diagnosis of schizophrenia next 15 years Andreasson et al, 1987, Lancet, 330 Evidence for Precipitation 10.0 7.5 RR 5.0 2.5 .0 No use 1-10 times 11-50 times 50+ times Risk of diagnosis of schizophrenia 2.4 times higher in those who tried cannabis before 18 years Dose Response which decreased but persisted after adjustment for psych history Evidence against self medication Andreasson et al, 1987, Lancet, 330 Further Evidence for Precipitation • Two New Zealand birth cohort studies: • Dunedin1 N = 759 • Christchurch2 N=900 • Both studies found that cannabis use • Predicted psychotic symptoms RR ~ 2 • Stronger prediction for early onset cannabis use 1Arsenault et al, 2002, BMJ, 325 2Fergusson et al, 2003, Psych Med, 33 Public health model for prevention of problem cannabis use • Development of credible health education – Young are sceptical about ‘scare tactics’ – Parallels with the effects of alcohol & tobacco: • respiratory risks, MVA, dependence, psychosis • Prevention of problem use in young people is a broader issue than drug education: – e.g. sense of belonging and purpose, sense of self-worth, and independent decision making all influence drug use and require many community changes Suggested Message • Communicate the risk while honestly acknowledging the uncertainties that remain – people with psychosis or a first degree relative with psychosis avoid using cannabis – one in seven people who use cannabis report unpleasant, psychotic-like symptoms; avoid use – discouraging young people from using cannabis daily or near daily Disorders of cannabis use Assessment and Treatment Assessment of cannabis use • Quantity and frequency of use – Route (Cones v Joints) and their number – Estimated amount (grams) – $ spent per day or week • Also gives estimate of economic impact of use • Presence of dependence • Predisposing factors, e.g. psychiatric illness, other substance misuse • Complications : physical, psychological and social Clinical features of dependence • Withdrawal syndrome: common in users seeking help • Compulsive use: common in problem users – Impaired control – Strong desire to use • Tolerance • Large amounts of day spent using (salience) • ?? Continued use despite clear evidence of harm: – less common than for alcohol • May continue use despite self reported paranoia, or past exacerbation of schizophrenia; despite social conflict arising from use, wheeze; all known to be associated with use Prevalence of dependence • 2-4% of the general population – ECA study (USA in 1980s) – Australia: National Survey of Mental Health and Well Being • 9% of lifetime users (NCS study) • 33-50% of daily users become dependent Withdrawal • Symptoms worse in first week • Symptoms (rarely life-threatening): – irritability, anger – restlessness, anxiety – sleep difficulties, including strange dreams – craving, weight/appetite change, depressed mood, physical discomfort • To some extent still controversial • No validated rating scale Adverse consequences of dependence – Withdrawal – Physical complications: e.g. respiratory symptoms – Impaired memory – Poor work performance – Criminal involvement – Social disapproval Demand for treatment • Fewer than 10% seek any treatment • Why so few? – high rates of remission? – fewer short term consequences? – existing treatment services unattractive? Treatment options • • • • • Self-help Mutual support Brief interventions Psychotherapy Pharmacotherapy for withdrawal? – Diazepam (e.g. 5 mg tds x 3-5 days) for troublesome withdrawal? Limited evidence for a role – Short course of Lithium - ongoing RCT at USyd – Cannabis antagonist ineffective; trials abandoned Goals of psychotherapy • Reviewing benefits of cutting down/stopping • Reviewing harms of continued use • Identifying likely risk times for using • Discussing means of avoiding risk situations • Setting realistic goals Medical uses of cannabinoids • Antiemetic agent – Better than placebo but not as good as most modern anti-emetics – Side effect of feeling stoned! – All data derived from medicinal preparations not available in Australia (but most patients use smoked cannabis) • Appetite stimulant – particularly in advanced HIV patients • Analgesic and antispasmodic • Dependencies (obesity, tobacco, alcohol) using antagonists (limited by depression) Should cannabis use be decriminalised? Putative harms caused by cannabis prohibition • A large scale cannabis black-market – – – – controlled by criminals unregulated and no quality control untaxed corruption of public officials • ‘Arms race’ in policing technology – helicopters and satellite surveillance – indoor hydroponic cultivation • ?Loss of individual liberty to use cannabis, esp. for medicinal uses Other harms of prohibition • Discriminatory law enforcement – only 1-2% of past year users are prosecuted – more often lower SES, unemployed indigenous males – most cannabis use goes undetected but majority of drug offences are for cannabis use • Brings law into disrepute among the young • Effects on convicted users – stigma of criminal record – no impact on cannabis use – disproportionate penalty for self-harm • Poor use of scarce police and criminal justice resources Options for reducing cannabis-related harms • Intensified enforcement of prohibition – US and Swedish models • Legalisation of cannabis use – de facto e.g. the Netherlands – or de jure • ‘Decriminalisation’: – prohibition with civil penalties – diversion into treatment or education Arguments in favour • Current laws ineffective – Fails to prevent widespread use – Criminalises 50% of our youth! – Discriminatory enforcement (young indigenous males are 10x more likely to be convicted of use) • A cautious step - easily reversed • Reduces – harms to users – discriminatory enforcement • Better use of scarce resources • Minimal impact on use Arguments against • • • • • Only desired by a minority in Australia (25%) Really an irreversible step Likely to increase heavy & regular use Contrary to international treaties Little or no effect on black-market (legal product taxed) • Inconsistent: – use not a crime but cultivation and sale would still be a crime • Symbolism – implies cannabis use is safe & acceptable Proposed changes in penalties for personal use • Removal of jail penalties for 1st offenders • Cautioning and diversion as an alternative – may increase number of users dealt with – a more proportionate response to self-harm • Reduce push for more radical reform – more reversible policy and – consistent with international agreements • Penalties for use when driving – to address most probable adverse effect on non-users Key points • Occasional use of cannabis is widespread, socially accepted and causes little harm • The legal status of cannabis use is likely to remain controversial • Disorders of cannabis use are increasingly recognised and contribute to loss of productivity, respiratory and mental illness • Management options are currently limited to counselling • Elucidation of the pharmacology of the endocannabinoid system offers new targets for drug therapy for many illnesses Self-test case: Paul • Paul presents with insomnia and feeling ‘on edge’. He gave up smoking cannabis late last week after a fight with his partner over his pot smoking. He had been smoking 7 bongs per day. Self-test case: questions 1. How long is his withdrawal syndrome likely to last? 2. What complications of his past cannabis use might you check for? 3. How might you reduce his risk of relapse? Self-test case: answers 1. Around one week 2. Respiratory complications (airways disease, wheeze); psychiatric complications (e.g. exacerbation of schizophrenia if ever present) 3. Brief intervention: reinforcing benefits of cutting down, identifying at risk periods Contributors University of Sydney • • • Dr Jonathon Arnold Associate Professor Kate Conigrave Professor Paul Haber University of Queensland • Professor Wayne Hall University of New South Wales • • Dr Anthony Arcuri, National Cannabis Prevention and Information Centre Professor Jan Copeland, National Cannabis Prevention and Information Centre • Professor Maree Teesson, National Drug Alcohol Research Centre All images used with permission, where applicable Further learning Latt, et al (eds.), Addiction Medicine, Oxford University Press, 2009. (Chapter 7, Cannabis) • Hulse et. al. (eds.), Management of Alcohol and Drug Problems, Oxford University Press, 2002 and companion workbook. • Hall WD. Drug Alc Review 28: 100-116, 2009. • NCPIC website (www.ncpic.org.au) • Free national information and helpline (1800 304050) • www.nida.nih.gov and nsw.health.gov.au • Courtwright, DT, Forces of Habit: Drugs and the making of the modern world , Harvard Press, 2001 • Booth, M. (2004). Cannabis: A history. Bantam Books, London.