* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lessons Learned From Root Cause Analysis Activity
Survey
Document related concepts
Transcript
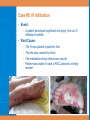
In Search of the Root Cause: Patient Safety at UCSF Adrienne Green, MD Associate CMO Clinical Professor of Medicine Kathy Radics, RN, MPA Patient Safety Manager GME Grand Rounds October 19, 2010 Case Presentation A 45 y/o M underwent a cardiac catheterization. While in the recovery area, he complained of feeling lightheaded and had labile blood pressure. He was therefore transferred to the Limited Stay Unit for overnight observation. The attending physician was unaware of the patient’s admission. The next morning he complained of severe abdominal pain. The LSU nurses had difficulty identifying a provider to evaluate the patient. Case Presentation The patient was hypotensive, CBC with H/H of 7.2/21.4. He was taken to the ED CT scanner where he arrested. A code was called and the patient was taken to the OR. The code was called before surgical intervention. The patient died of an unrecognized retroperitoneal bleed. Objectives • Review the role of RCA in promoting patient safety • Describe the RCA process – Background – UCSF process – Evidence for RCA effectiveness • Review recent UCSF events • Review strategies for disclosure/what do after an event Patient Safety- some definitions • Sentinel Event – A preventable error leading to death, serious physical or psychological injury, or risk of such injury • Adverse Event – A preventable error leading to any level of injury • Active Error – Occurs at the point of human interface with a complex system • Latent Error – Failures of system design Strategies to Improve Patient Safety • Root Cause Analysis – Introduced to medicine in early 1990s – Mandated in 1997 by The Joint Commission for all sentinel events • Failure Mode Effects Analysis- prospective • Incident Reporting Systems • Patient Safety Rounds • Culture of Patient Safety Surveys Root Cause Analysis • safe, blame-free, protected • structured retrospective analysis for identifying causal factors • multidisciplinary • focuses on systems and processes, not individual performance • ask why at each level of cause and effect • identify and implement improvement actions to prevent recurrence • Also at UCSF – assign accountability for action items and timely follow up – discuss disclosure to patient/family – discuss bill waivers Root Cause Analysis What happened? Why did it happen? What do we do to prevent it from happening again? Not allowed at an RCA: • “it’s okay, the patient was really complex and sick anyway” • “that MD/RN/pharmacist just wasn’t doing his/her job” • finger pointing RCA at UCSF • Conducted as part of the UCSF Patient Safety Committee (PSC), a multidisciplinary Medical Staff Committee – RN, MD, Pharmacy – Adult and Children’s Hospital – Leadership/Administration – Risk Management – Front line providers – Content experts What kind of events lead to RCA at UCSF? • “Never events” • Sentinel events • Errors resulting in patient harm • Near misses • Other events requiring multidisciplinary review 2010 Example Event Type 2009 Procedural Complications 35.5% 38.5% Esophageal Intubation Medication Errors 22% 27 % Insulin pen used for 2 patients Device Events 8% 0 Thermal Injury (burn) due to cooling device Q1-3 Specimen Issues 6.6% 0 Incorrect number of path specimens sent from OR to path Treatment Delay 6.6% 11.5% Delay in appt to f/u on abnl PSA Nosocomial Infection 6.6% 4% Hospital acquired H1N1 Wrong Site Surgery 4% 0 Wrong eye Retained Foreign Body 4% 7.5 % Retained sponge Other 6.6% 11.5 % Fall with injury RCA Actions and Follow-up • Identify and implement improvement actions to prevent recurrence – assign accountability for action items – team leaders report to PSC on progress Hierarchy of Actions Stronger Actions – – – – – Physical plant changes Engineering control (forcing functions) Simplify the process and remove unnecessary steps Standardize equipment, process, caremaps Leadership in support of patient safety Weaker Actions – – – – Double checks Warnings and labels New procedure, memorandum, policy Training Intermediate Actions – – – – – – Increase staffing/decrease workload Software modifications Eliminate/reduce distractions Checklist/cognitive aid Read back Enhanced documentation/communication http://www4.va.gov/ncps/CogAids/RCA/index.html#page=page-14 Actions: Strong or Weak? Action Items: Themes Corrective Action Plan Types Adequacy of technological support Oct - Dec 09 Jan - March 10 April June 10 July - Sept 10 1 1 2 1 3 1 6 7 1 1 6 2 2 Availability of information Behavioral assessment process Care planning process 6 Communication among staff members Communication with patient / family 1 Competency assessment / credentialing 2 1 Continuum of care 1 3 Equipment maintenance / management 3 4 3 Medication management 2 6 5 4 Orientation and training of staff 3 3 2 2 Policies 2 1 1 2 Staffing levels 2 2 2 1 Patient identification process Patient observation procedures Physical assessment process Physical environment Supervision of staff Total 1 22 34 19 24 Could This Happen To One of Your Patients? Case #1: Attending Oversight A 45 y/o M underwent a cardiac catheterization. While in the recovery area, he complained of feeling lightheaded and had labile blood pressure. He was therefore transferred to the Limited Stay Unit for overnight observation. The next morning he complained of severe abdominal pain. The patient was hypotensive, CBC with H/H of 7.2/21.4. He was taken to the ED CT scanner where he arrested. A code was called and the patient was taken to the OR. The code was called before surgical intervention. The patient died of an unrecognized retroperitoneal bleed. Case #1: Root Causes • The attending physician was unaware of the patient’s admission. • The LSU nurses had difficulty identifying a provider to evaluate the patient. • While in the LSU the patient had an acute change in condition – there was confusion by the nursing staff about whom to call for assistance. – the attending physician was not notified • There was a failure to recognize a potential retroperitoneal bleed Case #1: Actions • Attending oversight guidelines developed • Education on post-cath complications for involved providers and units • LSU developed clear protocol for escalation • Could this happen to one of your patients? – Are you comfortable calling an attending with questions regarding patient care? – Are you familiar with your service’s attending oversight guidelines? Guidelines for Attending Oversight on the Pediatric Medical Services Department of Obstetrics, Gynecology and Reproductive Sciences Trainee/Attending Communication Guidelines June 2010 Case #2: Medication Error A 6 mo baby with ALL received chemo including methotrexate. 2 days later she developed fevers and was empirically started on zosyn. Due to poor mtx clearance with high levels, the pt developed mucositis requiring TPN and prolonged hospitalization. Medication Error: Root Cause and Actions • The ordering MD was unaware that PCNs are contraindicated until mtx levels decline Weak – Education and training • The fever occurred at night and the signout/handoff did not indicate which abx the pt could or could not have – Peds Onc sign-out modified to include list of meds to avoid • The pharmacy did not catch the drug interaction because mtx was no longer on the pt’s med profile – A “fake order “ was developed and implemented by pharmacy to maintain mtx on pharmacy profile until levels decline Strong Case #3: Wrong Site Surgery A patient was consented for a left eye surgery. The left eye was marked in the pre-op area. The pt was prepped and draped in the OR. The initial incision was made on the right. A member of the team then mentioned that a time out had not been performed and that the surgery was to be on the right. The correct surgery was then performed. Wrong Site Surgery: Root Cause and Actions • The correct site was marked in the pre-operative area but draping covered the site marking – Ophthalmology changed practices w/r/t marking and draping • A time out was not performed – Re-education re: universal protocol and checklist – Staff empowered to escalate noncompliance Could this happen to one of your patients? • Are you using the correct checklist form? • Do you perform a comprehensive timeout before each procedure? Does your time out include the entire team? Case #4: Equipment Not Sterilized • Dirty equipment was re-used in an outpatient clinic procedure Dirty Area Clean Area Equipment Not Sterilized: Root Cause and Actions • Sterilization equipment in procedure room; dirty and clean equipment in close proximity – Sterilization moved to SPD – Extra equipment purchased to enable this new practice • Sterilization procedures and competencies not standardized b/w SPD and clinics – Sterilization practices and competencies standardized b/w clinic staff and SPD Case #5: IV Infiltration • Event: – A patient developed significant skin injury from an IV infiltrate of nafcillin • Root Cause: – – – – The IV was placed in patient’s foot The site was covered by kerlix The medication being infused was caustic Patient was unable to have a PICC placed in a timely manner IV Infiltration: Root Cause and Actions • Action: – A multidisciplinary taskforce convened to establish standard practices/guidelines for IV placement, including escalation to more skilled providers and a PICC if necessary – Education re: caustic meds – Establish procedures for response to IV infiltrates • Could this happen on your team? – Do you order PICC lines when appropriate? – Do you know how to care for an IV infiltrate? – Do you know which medications are caustic and should not be infused through a PIV? Device Fire • Event: – An x-ray developer caught fire • Root Cause: –Equipment was old with unclear history of inspection and maintenance –Difficulties with response to fire • Action: –New digital developers were ordered –Complete fire safety assessment of the site –Staff re-training re: fire and safety • Could this happen on your team? –Have you reviewed fire safety responses recently? –Do you red tag faulty equipment to be sent to biomedical engineering for repair? RCA Effectiveness • 3 studies show improved outcomes from single RCAs (improved mortality, graft survival) • 8 studies measure process outcomes (compliance with new process, survey perception of improvement) • Retrospective VA study (119 actions/26 RCAs) – 39% actions fully implemented (74% of those effective) – “stronger” actions more likely to be implemented, 75100% – more “weak” actions recommended but <30% implemented Percarpio et al. Joint Comm Journal July 2008 Hughes. NCPS Topics in Pt Safety 2006 RCA Effectiveness at the VA Root Cause/Contributing Factor Pre-RCA Post-RCA None 10% 0 Patient Behavior 43% 10% Course of Disease 40% 3% Systemscommunication, equipment etc. 37% 100% Bagian et al. Journal on Quality Impr. 2002 RCA Effectiveness at UCSF: Sustainability • Analysis of actions from 2007 and 2008 • Random selection of 10% of actions from top 3 action categories (med management, communication, orientation/training) • Action completed and sustained 58% • Action completed and abandoned 17% • Completed but recurrent event 17% What do I do if an error occurs in one of my patients? • Call your attending • Speak with the patient and family – Express empathy and apology – Inform of the facts but don’t speculate – Let pt/family know that the event will be investigated and identified problems fixed – Let pt/family know that you will stay in contact as you learn more • Document objectively • Call Risk Management (353-1842) • File an Incident Report RCA at UCSF: Opportunities for Improvement • Implement improvements beyond the location of the primary event • Demonstrate sustainability of improvement activities • Disseminate learnings and themes beyond the location of the primary event Summary • RCA is an important tool for improving patient safety What happened? Why did it happen? What do we do to prevent it from happening again? • UCSF has a robust and improving RCA process • Recent events highlight the importance of: – Resident:attending communication/oversight – Medication management – Universal Protocol • Help is available if an error or adverse event occurs in one of your patients Suggestions and Comments • Adrienne Green [email protected] • Kathy Radics [email protected]