* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download New Concepts in Ocular Surface Infection and Inflammation
Survey
Document related concepts
Transcript
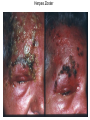
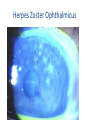
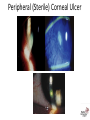
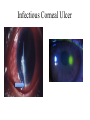
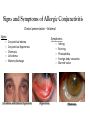
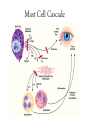
Oral Pharmaceuticals in Anterior Segment Disease Blair B Lonsberry, MS, OD, MEd., FAAO Diplomate, American Board of Optometry Pacific University College of Optometry [email protected] OSDs are Difficult to Tell Apart: Overlapping Signs/Symptoms Signs Hyperemia Chemosis Lid Swelling Symptoms Foreign Body Sensation Burning Dry, Gritty Ocular Surface Itchy Eyes Photophobia Tearing CASE Case • 20 year old male presents with a red painful eye – Started that morning when he woke up – reports a watery discharge, no itching, and is not a contact lens wearer • SLE: – See attached image with NaFl stain Herpes Simplex Keratitis: Clinical Features • Characterized by primary outbreak and subsequent reactivation • Primary outbreak is typically mild or subclinical • After primary infection, the virus becomes latent in the trigeminal ganglion or cornea • Stress, UV radiation, and hormonal changes can reactivate the virus • Lesions are common in the immunocompromised (i.e. recent organ transplant or HIV patients) Dendritic Ulcers 6 Pediatric HSV Keratitis • pediatric herpes simplex keratitis has an 80% risk of recurrence, a 75% risk of stromal disease, and a 30% rate of misdiagnosis • 80% of children with herpes simplex keratitis develop scarring, mostly in the central cornea – results in the development of astigmatism – 25% of children have more than 2 D of astigmatism, most of which is irregular • consider pediatric HSV when a patient has unilateral recurrent disease in the anterior segment Herpes Simplex Keratitis Management • Topical: – Viroptic (trifluridine) q 2h until epi healed then taper down for 10-14 days. • Viroptic is toxic to the cornea. – Zirgan (ganciclovir) available, use 5 times a day until epi healed then 3 times for a week (US only) Anti-Viral Medication Drug Mechanism of Action Acyclovir Bioavailability Dosing Side Effects Acyclovir interferes with 10-30% gets DNA synthesis inhibiting absorbed viral replication Short ½ life *Metabolized in kidneys Simplex: 400 mg 5x/day Zoster: 800 mg 5x/day Overall very safe Nausea, vomiting, headaches, dizziness, confusion Valacyclovir Acyclovir pro-drug Equivalent to acyclovir but better for pain management Simplex: 500 mg tid Zoster: 1 g tid Same as acyclovir Famciclovir (Famvir) Inhibits DNA chain Superior to elongation acyclovir* It is metabolized to penciclovir where it is active 10-20x as long as acyclovir Simplex: 250 mgTID Zoster: 500 mg TID Same as acyclovir 95% converted to acyclovir* Better bioavailability and longer 1/2 life HSV Stromal Disease • HSV Stromal disease is an immune-mediated disease • Increased risk of scarring and high risk of poor visual prognosis • Requires corticosteroids (HEDS: corticosteroid reduced risk of progression by 68%) – Without epithelial defect: corticosteroids and prophylactic anti-viral dosage – With epithelial defect: active infection anti-viral dosage with judicious corticosteroids How much to dose steroid? • HEDS used QID of prednisolone phosphate • Current Recommendations: – Mod – severe (especially with neo): 1% Prednisolone or Lotemax QID to 6x/day – Want the lowest dose needed to control the inflammation – AAO EBM Treatment Guideline 2014 • Topical steroid for 10 weeks (this is based on HEDS results) with oral antiviral Herpes Simplex Epithelial Keratitis • Treatment Regimen: – Zirgan 5x/day until the ulcer heals, then 3x/day for one week – Oral Valtrex 500 mg 3x/day for 7-10 days – Artificial tears – L-Lysine 2 grams daily? • Proven to “slow down” and retard the growth of the herpes virus and inhibit viral replication – Debride the ulcer? • Prior to topical antiviral therapy debridement was treatment of choice • Generally try to avoid use of sharp instruments and use of cotton swab and anesthetic • RTC 1 day, 4 days, 7 days Herpes Simplex Keratitis • Prophylactic Treatment: – Reduces the rate of recurrence of epithelial and stromal keratitis by ≈ 50% • Acyclovir 400 mg BID • Valtrex 500 mg QD • Famvir 250 mg QD • L-lysine 1 gram/day: – Proven to “slow down” and retard the growth of the herpes virus and inhibit viral replication • Frequent debilitating recurrences, bilateral involvement, or HSV infection in a monocular patient Prophylaxis?? • Pitfalls to Prophylaxis: – Reduction of recurrence does not persist once drug stopped – Resistance???? • van Velzen, et. al., (2013) demonstrated that longterm ACV prophylaxis predisposes to ACV-refractory disease due to the emergence of corneal ACVR HSV-1. Herpes Zoster Herpes Zoster Ophthalmicus 18 Herpes Zoster • Presents with: – pain and tingling in region of skin supplied by V few days before lesions, – malaise and fever, – papulomacular then pustular rash, – mucopurulent conjunctivitis, – uveitis, glaucoma, episcleritis, keratitis, and retinitis can all occur. – neurological complications include cranial nerve palsies and optic neuritis. Herpes Zoster • Associated factors include increasing age, immune deficiency and stress. • Only people who had natural infection with wild-type VZV or had varicella vaccination can develop herpes zoster. • Children who get the varicella vaccine appear to have a lower risk of herpes zoster compared with people who were infected with wild-type VZV. • A person's risk for herpes zoster increases sharply after 50 years of age. • Almost 1 out of 3 people in the United States will develop herpes zoster during their lifetime. • A person’s risk of developing post-herpetic neuralgia also increases sharply with age. Herpes Zoster • Management includes: – oral antivirals: • 800mg acyclovir 5x/day • valacyclovir (Valtrex) 1g TID, • famciclovir (Famvir) 500 mg TID – effectiveness of therapy is best started within 72 hours • Valacyclovir and famciclovir are preferred because of better bioavailability and convenience – Pain management: • tricyclic antidepressants, • Gabapentin • oral steroids Herpes Zoster Ophthalmicus (HZO) • Topical ganciclovir 5 times a day until healed, and then twice daily for 2 to 4 weeks is effective for dendriform keratitis, even in cases that have been unresponsive to oral antivirals • Topical corticosteroids: 41 – management of stromal keratitis and uveitis, – often need to be continued at a low-dose chronically and – require close monitoring for safety and efficacy Herpes Zoster Ophthalmicus (HZO) • Secondary glaucoma (16% to 56%) can occur because of inflammation or topical corticosteroids. • Neurotrophic keratopathy: – complicated by persistent epithelial defects, – corneal melting with or without perforation, and – microbial superinfection – challenging to manage Vaccine (Zostavax®) • The Advisory Committee on Immunization Practices (ACIP) recommends zoster vaccine (Zostavax®) for people aged 60 years and older. • The vaccine reduced the overall incidence of shingles by 51% and the incidence of PHN by 67% • Even people who have had herpes zoster should receive the vaccine to help prevent future occurrences of the disease. • In adults vaccinated at age 60 years or older, vaccine efficacy wanes within the first 5 years after vaccination, and protection beyond 5 years is uncertain Corneal Ulcers • • Infective bacterial and fungal corneal lesions cause severe pain and loss of vision Signs and Symptoms: – Pain, photophobia, tearing – Mucopurulent discharge with generalized conjunctival injection – Decreased VA (esp if on visual axis) – Possible AC reaction and hypopyon – Dense infiltrate – Satellite lesions around main lesion may indicate fungal infection Associated Factors • Contact lens wear, especially soft and extended wear lens • Recent history of corneal trauma • Topical steroid use • History of exposure to vegetative matter (fungal etiology) When to culture? • 1,2,3 Rule: • • • • • • 1 mm from visual axis 2 infiltrates (or more) 3mm or greater in size Nosocomial infections Immuno-compromised patient Post-surgical Sterile vs Infectious Infiltrates Peripheral (Sterile) Corneal Ulcer Infectious Corneal Ulcer Corneal Ulcers • The Steroids for Corneal Ulcers Trial (SCUT) • Conclusions: – no overall difference in 3-month BSCVA and no safety concerns with adjunctive corticosteroid therapy for bacterial corneal ulcers – researchers did find significant vision improvement for one specific subgroup of the study by using steroid therapy on patients with severe ulcers • Application to Clinical Practice: – Adjunctive topical corticosteroid use does not improve 3month vision in patients with bacterial corneal ulcers unless in the severe category Management • Infective ulcers need to be cultured! • If contact lens wearer, consider culture of contact lens • Intensive topical antibiotic regimen, consider fortified preparations, subconjunctival injections. – loading dose of Vigamox/Moxeza/Zymaxid/Besivance 2gtts q 15 min x 1 hour, – 1gt q 30 min x 6 hours, – 1 gt q 1 hr until f/u in 24 hours. ARMOR • Antibiotic Resistance Monitoring in Ocular Microorganisms (ARMOR) • Approximately 42% of isolates were determined to be MRSA • Newer fluoroquinolones have better activity than earlier generations • Besivance has the lowest MIC values of all the fluoroquinolones • Vancomycin is drug of choice if MRSA present • Azithromycin had very poor activity against Staph Anti-inflammatory effects • Degrade extracellular proteins • Tetracyclines inhibit MMPs • Anti-inflammatory Pseudomonas case report “Doxycycline as an adjunctive therapy…may help to stabilize corneal breakdown and prevent subsequent perforation.” AM. McElvanney 750 Anti-inflammatory Efficacy • Cortisol (hydrocortisone) is the standard of comparison for glucocorticoid potency and is given an anti-inflammatory score of 1 • All of the other medications are given relative scores that allow direct comparison – Prednisone has a relative anti-inflammatory efficacy of 4 • Much easier to compare for systemic medications than topical because of the vast differences in tear films, drop delivery, etc. Anti-Inflammatory Efficacy Generic Name of Medication Anti-Inflammatory Activity Equivalent Dose (mg) Relative Sodium Retaining Activity Hydrocortisone 1.0 20 mg 1.0 Prednisone 4.0 5 mg 0.8 Prednisolone 4.0 5 mg 0.8 Triamcinolone 5.0 4 mg 0.0 Methylprednisolone 5.0 4 mg 0.0 Dexamethasone 25.0 0.75 mg 0.0 Betamethasone 25.0 0.75 mg 0.0 Bioavailability of Systemic Steroids • Corticosteroids are readily absorbed from the intestinal tract which makes oral dosages very effective • They are metabolized by the liver (must consider function before prescribing) and excreted via the kidneys • Long term steroid treatment must be tapered to avoid side effects – Even at doses as low as 15 mg of prednisone if the patient has been dosed for several weeks • High dose oral steroids should be considered for initial therapy – 1 mg/kg therapy and continued until uveitis has resolved Systemic Corticosteroids • Prednisone – Available as Oral: 1, 2.5, 5, 10, 20, 50 mg tablets (1 and 5 mg/mL solution and syrup, if needed) • Ocular Treatment Guidelines – Mild to Moderate: Initial dose of 20-40 mg – Moderate to Severe: 40 – 60 mg – Severe: 60-100 mg • IV Methylprednisolone 250 mg IV q6hours for 12 doses for arteritic ischemic optic neuropathy (giant cell arteritis) • Similar dose given for active optic neuritis 2⁰ to MS Steroid Treatment Pearls • Specific type and location of inflammation determine route of administration • I.e. treat the problem! – Topical, Systemic, Periocular, Intravitreal, etc. • Must institute treatment immediately and at a high enough dose and frequency to suppress the inflammation Indications for oral and IV steroids • Inflammation of the posterior segment, optic nerve, or orbital tissues – – – – – – Stubborn anterior uveitis Posterior uveitis and/or chorioretinitis Scleritis Arteritic Ischemic Optic Neuropathy – temporal arteritis Optic neuritis Orbital inflammatory pseudotumor • Also recommended for hypersensitivity reactions – Contact dermatitis, etc Why Taper? • To prevent rebound inflammation – Corticosteroids reduce the quantity and activity of leukocytes – Stopping cold turkey causes these white cells to proliferate and increase the production of inflammatory cytokines – This means more steroids for a longer period of time which increases the risk of side effects What is the “right way” to taper oral prednisone? • Tapering is VERY case specific – no cookie-cutter method • If the inflammation is mild and a low dose oral steroid is prescribed for less than a week, tapering is usually not needed • Do NOT start tapering until the inflammation is resolved Medrol Dosepak • Methylprednisolone • Dosepaks have six 4 mg tablets that the patients takes on day one, with the number of tablets reduced by 1 each day over the next 6 days in a tapering schedule (21 tablets total) • Convenient dosing regimen with built in tapering Side Effects of Systemic Corticosteroids • Incidence increases with long-term high-dose therapy • Length of use has greater link to developing side effects than dosage amount Side Effects of Systemic Steroids • Metabolic Effects: – – – – HYPERglycemia can occur Increased appetite, Weight Gain, and Redistribution of fat Decreased calcium absorption – leads to Osteoporosis Hyperlipidemia • Mineralocorticoid Effects: – Fluid Retention (Increased Sodium Retention) – Hypertension – Edema (If liver/kidneys can’t keep up) • CNS Symptoms: Euphoria, Insomnia, Psychoses, Depression, and Restlessness Therapy Considerations • Diabetes – Educate all Type 2 Diabetes patients that their blood sugar will likely become elevated – Educate all Type 1 Diabetes patients they made need to alter their insulin levels • Peptic Ulcers – Consider prescribing an H2 Blocker or a Proton Pump Inhibitor if prednisone dose ≥60 mg or ≥30 mg over 2 weeks • PPI’s: Omeprazole (Prilosec), Esomeprazole (Nexium), and Lansoprazole (Prevacid) • H2 Blockers: Cimetidine (Tagamet), Famotidine (Pepcid), and Ranitidine (Zantac) Steroid Considerations • Also use caution in patients with: – Any Infectious disease – Pregnancy (Orals are Category C) – Chronic renal failure – Congestive Heart Failure – Systemic Hypertension – Osteoporosis – Psychoses Allergic Conjunctivitis Prevalence of Allergic Conjunctivitis • Allergies affect as many as 40 to 50 million Americans • Incidence and prevalence of allergic conjunctivitis has been rising over the last 40 years Signs and Symptoms of Allergic Conjunctivitis Clinical presentation – bilateral Signs: – – – – – Symptoms: Conjunctival edema Conjunctival hyperemia Chemosis Lid edema Watery discharge Lid edema and bilateral hyperemia – – – – – Hyperemia Itching Burning Photophobia Foreign body sensation Blurred vision Chemosis Mast Cell Cascade Treatment • Ocular allergy sufferers need; – fast relief of signs and symptoms, – long-lasting therapeutic effects, – comfortable and safe topical drugs, – convenient treatment regimen • Therapeutic focus is mostly confined to the suppression of mast cells, their degranulation and the effects of histamine and other mast-cell derived mediators. Treatment of Ocular Allergy Medications: • Topical OTC drops • Oral antihistamines (prescription and OTC) • Topical NSAID drops • Topical antihistamines • Topical mast cell stabilizers • Topical steroid drops • Topical dual-action drugs (antihistamine/mast cell stabilizers) Oral Allergy Medications • Oral antihistamines (pills and liquids) ease symptoms such as: – – – – swelling, runny nose, itchy or watery eyes, and hives (urticaria). • Some oral antihistamines may cause dry mouth and drowsiness. • Older antihistamines such as diphenhydramine (Benadryl), chlorpheniramine (Chlor-Trimeton) and clemastine (Tavist) are more likely to cause drowsiness and slow reaction time. – these sedating antihistamines shouldn't be taken when driving or doing other potentially dangerous activities. OTC Allergy Medications Generic Brand Diphenhydramine Benadryl Chlorpheniramine Chlor-Trimeton Clemastine Tavist Loratadine Claritin Cetirizine Zyrtec Fexofenadine Allegra (both OTC and Rx) Prescription Allergy Medications Carbinoxamine maleate ARBINOXA, PALGIC (tabs, solution) Diphenhydramine HCI BENADRYL Injection Hydroxyzine HCI HYDROXYZINE HCL (tabs, syrup) Desloratadine CLARINEX (tabs, ODT, syrup) Fexofenadine HCl ALLEGRA (tabs, ODT, suspension) Levocetirizine dihydrochloride XYZAL (tabs, solution) Montelukast SINGULAIR (tabs, chew tabs, granules) Cromolyn sodium GASTROCROM (oral solution) Ocular Allergy Medication Options Tetrahydrazoline HCI VISINE*, MURINE* Plus Naphazoline HCI NAPHCON® eye drops, VASOCON* Phenylephrine HCI PREFRIN* Oxymetazoline HCI VISINE L.R.* Naphazoline/Antazoline VASOCON*-A Naphazoline/Pheniramine NAPHCON-A® eye drops Ketorolac ACULAR* Suprofen PROFENAL® solution Diclofenac VOLTAREN* * Trademarks are the property of their respective owners **Vexol is a trademark of N.V. Organon Levocabastine LIVOSTIN* Emedastine EMADINE® solution Loteprednol Rimexolone ALREX* VEXOL** suspension Cromolyn CROLOM*, MAXICROM™ solution Lodoxamide ALOMIDE® solution Nedocromil ALOCRIL*, TILAVIST* Pemirolast ALAMAST* Azelastine OPTIVAR*, LASTIN* Ketotifen ZADITOR*, ALAWAY*, ZYRTEC, CLARITIN Epinastine ELESTAT* Olopatadine PATANOL® PATADAY Bepotastine BEPREVE Alcaftadine LASTACAFT Thank You!!!