* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Full paper
Survey
Document related concepts
Transcript
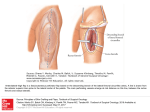
ACTUAL VERSUS EXPECTED LASIK FLAP THICKNESS USING THE MORIA M2 130 MICROKERATOME HEAD Abd El Monem Mohamed Hamed, MD. * Shereef Abd El Wahab ,MD.** Maha Attia ELFayoumy,MD.*** * Assistant professor of ophthalmology Benha Faculty Of Medicine * * Lecturer of ophthalomology Benha Faculty Of Medicine *** Lecturer of ophthalomology Benha Faculty Of Medicine AIM: To evaluate actual versus expected laser in situ keratomileusis (LASIK) flap thickness using the Moria M2,130 microkeratome head. METHODS: 50 eyes of 25 patients scheduled for LASIK surgery for myopia where enrolled in this study. Patients were prepared for surgery. On the day of surgery they were admitted to the LASIK room where the lids were sterilized and draped. A suction lid speculum was applied to one eye after instilling one drop of Benox into the conjunctival sac, the eye was then washed with balanced salt solution BSS and the suction of the lid speculum activated to assure there was no excess BSS in the conjunctival sac then a final preoperative ultrasonic central corneal pachymetry reading using the sterile probe of the Tomey AL-2000 pachymer was recorded. The suction ring of the Moria M2 mikroketatome was centered on the cornea and immediately after the lasik flap was fashioned and the suction ring removed the flap was elevated then an intra operative central stromal bed pachmetry reading was recorded using the sterile Tomey AL-2000 pachymer probe. The actual flap thickness was calculated by subtracting the intra operative central stromal thickness from the preoperative central corneal thickness. SETTING: Out patient Lasik center in the period from January 2004 till beginning of February 2004. RESULTS: The mean actual flap thickness created by the Moria M2 130 head microkeratome for the first cut was 153.8 + 17 (range 120µm – 188µm) and for the second cut 148.4 + 15.82 (range 118- 185). The mean difference in flap thickness between the first and second cut was 4.4µm + 1.7µm with the tendency of the second flap to be slightly thinner than the first. This difference was found to be statistically insignificant (P>0.05, paired t test). The mean difference between the actual and expected flap thickness was 9.9µm + 1.7 and this was found to be statistically significant ( P <0.001 ). CONCLUSION: The difference between the actual and expected flap thickness using the Moria M2 microkeratome was statistically significant and care should be taken when making assumptions about flap thickness based upon the manufacturers labeling to calculate the residual bed thickness, having in mind that the flap may be thinner in some cases and thicker in others. The latter must be thought of well to avoid violating the rule of leaving at least 250µm of stromal bed after laser ablation, which may lead to postoperative ectasia , keratoconus and even intraoperative stromal penetration. It is recommended to do an intraoperative pachymetry in all LASIK cases if possible. INTRODUCTION Recently there have been multiple reports of ectasia after LASIK in cases which were supposed to have a residual corneal thickness of more than 410µm after the LASIK procedure1. Most researchers have agreed that a residual corneal thickness (RCT = residual stromal thickness after ablation + corneal flap thickness) of 410µm or more should not lead to post operative ectasia, provided that the postoperative residual stromal thickness (RST) would not be less than 250µm. A lot of surgeons follow the rule of leaving a postoperative corneal thickness of 410µm to be on the safe side and avoid the occurrence of postoperative ectasia 2. In spite of following this rule, there still are reports of cases of postoperative ectasia1. This fact lead researchers to revaluate the methods of preoperative 1 calculation of the RST, and thus the final RCT. Before LASIK the best means of estimating RST is to subtract the theoretical laser correction obtained from the laser computer and the expected flap thickness normally obtained with a given microkeratome system from the preoperative central corneal thickness3. Many surgeons make assumptions about flap thickness based upon the manufacturers’ labeling of the microkeratome when estimating the RST 4. This however may be unwise as previous reports mentioned that there is a degree of variation in flap thickness, and flaps may actually be thinner or thicker than expected; the latter is potentially serious if laser ablation removes tissue to below the accepted standard of 250µm residual stromal bed. Many factors other than microkeratome model and head number such as mean preoperative pachymetry, size of suction ring, steepest K reading and order of surgery (first eye or second eye ) may lead to variability in flap thickness, however age, sex, average K readings, white to white oscillation and translation speed did not correlate with flap thickness 5. Several studies have been designed to compare the flap thickness produced by various mikrokeratomes. In our study we used one microkeratome, the Moria M2 ,with the 130µ head which the manufacturer expects to make a flap thickness of 160µm and we tried to avoid other factors that may influence the flap thickness by including eyes with a narrow range of difference in preoperative pachymetry (range 520µm-560µm). The mean preoperative steepest K reading was 42.95 + 1.12 (range 41.7 – 45) and the Moria Zero suction ring was used in all cases. Moria M2 has two translation speeds; a speed of 3.3 mm/sec was used in all cases. The collected data was used to see how close the expected flap thickness was to the actual flap thickness. PATIENTS AND METHODS Fifty eyes of thirteen females and twelve males were included in this study , all patient were myopes with a preoperative error of refraction ranging from -1 diopter to - 5 diopters . Preoperatively the following parameters were noted: uncorrected visual acuity, best corrected visual acuity, and manifest refraction. Soft contact lenses were discontinued two weeks before surgery; rigid contact lenses were discontinued four weeks before surgery. All patients had preoperative corneal topography (Tomey TMS-2N topographic modeling system) and ultrasound pachymetry (Tomey AL-2000 pachymeter). The preoperative corneal curvature was measured using automated keratometry (Nidek ARK7000A). All patients had a slit lamp examination and the preoperative intra ocular pressure IOP was recorded (Haag Streit applanation tonometer), followed by posterior segment indirect ophthalmoscopy. On the day of surgery the patients were admitted to the LASIK room where the lids were sterilized and draped. A suction lid speculum was applied to one eye after instilling one drop of Benoxinate (Oxybuprocaine hydrochloride 0.4%) into the conjunctival sac, the eye was then washed with balanced salt solution BSS and the suction of the lid speculum activated to assure there was no excess BSS in the conjunctival sac then a final preoperative ultrasonic central corneal pachymetry reading using the sterile probe of the Tomey AL-2000 pachymer was recorded. All LASIK procedures were performed using the Moria M2 microkeratome with the 130 head which is theoretically supposed to produce a 160 µm thick flap. All flaps were superiorly hinged and created after centering the properly sized Moria suction ring on the cornea and activating the vacuum–suction machine until clinical signs of high IOP were noticed ( pupil dilatation and blacking out of patients’ vision). Moria suction rings are available in five sizes, plus3, plus2, plus1, Zero and minus 1. The appropriate suction ring size is selected according to the steepest corneal keratometric (K) reading and to the table supplied by the manufacturer which specifies the size of the ring to be used and the stop position to be adjusted and the expected flap and hinge size in mm with every ring and K reading. The different suction rings for successive ranges of keratomertikc values increases the safety and reliability in different types of corneas, however in our study we had a narrow range of steepest K reading that allowed us to use one ring (The Zero ring) for all cases. After the flap was created, the suction was released and the ring removed, the flap was lifted and three accurate intraoperative pachmetry readings for the residual stromal bed thickness were recorded using the 2 sterile probe of the Tomey AL-2000 pachymer . Laser ablation was done using the Nidek EC-5000 machine, the flap was put back in place and the stromal bed was irrigated with BSS. The same steps were repeated with the other eye of each patient. A new blade was used for every patient. The first flap of every patient was always created by a brand new blade while the second flap was always created by a blade than has already been used once. The actual flap thickness was calculated by subtracting the central intraoperative stromal bed thickness from the central immediate preoperative corneal thickness. The actual flap thickness measurements of every created flap and the expected flap thickness measurements were exported to windows Microsoft Excel and statistically analyzed using the student t test. RESULTS: A total of 50 eyes were reviewed. Sex distribution was 52% females and 48% males there was no statistical significance between the number of males and females (P>0.05), the mean age was 36 years + 8.9 (SD). 50% of the procedures were in the first eyes and 50% in second eyes. The mean preoperative pachymetry measurement was 542.7 + 13.3µm (range 520 – 560 µm) and the mean steepest K reading was 42.95 + 1.12 (range 41.75 – 45). The mean white to white measurement was 11.5 + 0.4 and the mean scotopic pupillary diameter was 5.5 + 0.9. The mean actual flap thickness created by the Moria M2 130 head microkeratome for the first cut was 153.8 + 17 (range 120µm – 188µm) and for the second cut 148.4 + 15.82 (range 118- 185). The mean difference in flap thickness between the first and second cut was 4.4µm + 1.7µm with the tendency of the second flap to be slightly thinner than the first. This difference was found to be statistically insignificant (P>0.05, paired t test). The mean difference between the actual and expected flap thickness was 9.9µm + 1.7 and this was found to be statistically significant ( P <0.001 ) Chart 1 shows the actual first cut flap thickness in respect to the expected flap thickness. Thickness inmicrons Actual First Cut Flap Thickness In Respect to expected flap thickness 200 150 expected for first cut 100 first eye flap thickness 50 28 25 22 19 16 13 10 7 4 1 0 number of eyes CHART 1 Chart 2 shows the actual second flap thickness in respect to the expected flap thickness 3 Thickness in microns Actual Second Flap Thickness In Respect To The Expected Flap Thickness 200 150 second eye flap thickness 100 expected for first cut 50 28 25 22 19 16 13 10 7 4 1 0 Number of eyes CHART 2 Chart 3 shows actual first and second cut flap thickness in comparison to each other Thickness in microns Actual First And Second Cut Flap Thickness In Comparison To Each Other 200 150 first eye flap thickness 100 second eye flap thickness 50 28 25 22 19 16 13 10 7 4 1 0 Number of eyes CHART 3 DISCUSSION: Laser in situ keratomileusis continues to be the most common corneal refractive surgery performed worldwide6. It offers rapid visual recovery, low risk for corneal haze, and reliable results for correction of nearsightedness, farsightedness, and astigmatism. It is performed by first creating an anterior corneal flap with a microkeratome. The purpose of the microkeratome in LASIK is to create a corneal flap of a desired thickness, thus exposing the stroma for laser ablation, the lack of precision in reproducing flap thickness with actual microkeratomes is an important drawback of these instruments 7.In this study we examined the actual flap thickness produced by the Moria M2 keratome in 50 consecutive eyes and compared it to the manufacturers presumed flap thickness for the same microkeratome. The Moria M2 is an automated microkeratome designed to produce a surface-parallel keratectomy of a preset flap diameter and a uniform flap thickness, the 130 head of the microkeratome which was used in this study is supposed to produce a flap of 160µm thick 4 according to the manufacturers manual. The device was evaluated in this study after excluding the other factors that are known to affect the flap thickness such as variation in preoperative central corneal pachmetry, size of the suction ring, and steepest K reading by selecting cases with a narrow range of difference in preoperative pachymetry and K readings, we also used one rig size (The Zero ring) for all cases. Solomon et al 5 reported a significant difference in flap thickness between the first and second cuts done by the same micrikeratome blade and thus we recorded the flap thickness obtained after the first cut and that obtained after the second cut for each case. In this study the mean actual flap thickness created by the Moria M2 130 head microkeratome for the first cut was 153.8 + 17 and for the second cut 148.4 + 15.82 and the difference in flap thickness between those created after the first or second cut was found to be statistically insignificant (P>0.05, paired t test).The mean flap thickness for flaps created after first cut, in this study ranged from 120µm – 188µm, while those created after the second cut ranged from 118- 185µm. No flaps thinner than 118 µm or thicker than 188µm were encountered throughout the study. Four out of the fifty (8%) eyes enrolled in the study had an actual calculated flap thickness of 160µm which was exactly equal to the manufacturers expected flap thickness, while 46 eyes (92%) had an actual flap thickness that ranged from 118µm to 188µm.This was found to statistically significant (P>0.05).The results of this study are close to the results of Miranda 8 who studied the flap thickness reproducibility using the Moria Carriazo Barraquer (CB), the Moria M2 and the Hansatome microkeratome, and found the Moria M2 to be of the greatest reproducibility with a mean actual flap thickness of 157+ 40µm .The difference in thickness between the first and second cut flaps was also found to be present but of no significance when using the Moria M2 microkeratome in contrast to other microkeratomes such as the Hansatome, Summit Krumeich-Barraquer microkeratome (SKBM),and Amadeus microkeratomes which showed a significant difference between first and second cut 5 . The results also correlate to the results of Javaloy 9 who found a difference between the desired and actual flap thickness when using the Moria M2 microkeratome with a mean flap thickness of 150.13µm + 20.42 ranging from 109µm to 189µm. The actual flap thickness in this study ranged from 118µm to 188µm this differed from the results of Solomon 5 who reported a range of flap thickness of 84µm – 204µm, this wide range was not seen in our study may be because only 50 eyes were included, in comparison to the number of eyes included in the study of Solomon 5, 1634 eyes, in which they used the Moria M2 on 140 eyes the big number of eyes they studied may explain the wide range they encountered. In conclusion the difference between the actual and expected flap thickness using the Moria M2 microkeratome was statistically significant and care should be taken when making assumptions about flap thickness based upon the manufacturers labeling to calculate the residual bed thickness, having in mind that the flap may be thinner in some cases and thicker in others. The latter must be thought of well to avoid violating the rule of leaving at least 250µm of stromal bed after laser ablation, which may lead to postoperative ectasia , keratoconus and even intraoperative stromal penetration. It is recommended to do an intraoperative pachymetry in all LASIK cases if possible. REFRENCES : 1. Miyata K, Tokunaga T, Nakahara M, Ohtani S, Nejima R, Kiuchi T, Kaji Y, Oshika T. Residual bed thickness and corneal forward shift after laser in situ keratomileusis. J Cataract Refract Surg. 2004;30:1067-72. 2. Wang Z, Chen J, Yang B. Posterior corneal surface topographic changes after laser in situ keratomileusis are related to residual corneal bed thickness. Ophthalmology. 1999 Feb;106(2):406-9; discussion 409-10. 3. Flanagan GW, Binder PS. Precision of flap measurements for laser in situ keratomileusis in 4428 eyes. J Refract Surg. 2003 Mar-Apr;19(2):113-23. 5 4. Giledi O, Mulhern MG, Espinosa M, Kerr A, Daya SM. Reproducibility of LASIK flap thickness using the Hansatome microkeratome. J Cataract Refract Surg. 2004;30:1031-7. 5. Solomon KD, Donnenfeld E, Sandoval HP, Al Sarraf O, Kasper TJ, Holzer MP, Slate EH, Vroman DT; Flap Thickness Study Group.Flap thickness accuracy: comparison of 6 microkeratome models. J Cataract Refract Surg. 2004;30:964-77. 6. Probst LE, Machat JJ. Mathematics of laser in situ keratomileusis for high myopia. J Cataract Refract Surg. 1998;24:190-195. 7. Jacobs BJ, Deutsch TA, Rubenstein JB. Reproducibility of corneal flap thickness in LASIK. Ophthalmic Surg Lasers. 1999;30:350-353. 8. Miranda D, Smith SD, Krueger RR. Comparison of flap thickness reproducibility using microkeratomes with a second motor for advancement. Ophthalmology. 2003 Oct;110(10):1931-4. 9. Javaloy Estan J, Vidal MT, Quinto A, De Rojas V, Alio JL. Quality assessment model of 3 different microkeratomes through confocal microscopy. J Cataract Refract Surg. 2004;30:1300-9. 6