* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download What Is This Virus Called Hepatitis C?
Chagas disease wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Ebola virus disease wikipedia , lookup
West Nile fever wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Schistosomiasis wikipedia , lookup
Henipavirus wikipedia , lookup
Leptospirosis wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Marburg virus disease wikipedia , lookup
Neonatal infection wikipedia , lookup
Antiviral drug wikipedia , lookup
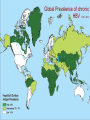
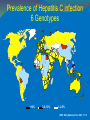
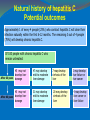
Frances Cieslak Victorian Viral Hepatitis Educator [email protected] Impact of Hepatitis Hepatitis can be caused by: Harmful consumption of alcohol Some chemicals and drugs Viruses – 5 known A, B, C, D & E Inflammation of the liver – natural response to injury Scar tissue = Fibrosis Extensive scarring = Cirrhosis HBV & HCV require long term monitoring One in 12 people worldwide are living with chronic hepatitis B or C World Hepatitis Alliance Chronic hepatitis B & C are responsible for over 80% of the worlds liver cancer (HCC) ASHM/NSWCC 2008 Hepatitis B At A Glance ASHM/CCNSW 2008 2 billion people infected world wide (350 million chronic) 1 million HBV related deaths each year A leading cause of hepatocellular carcinoma (HCC) Screening people at risk is critical Treatment is available to control the virus Vaccination prevents NEW cases but will not impact on current chronic hepatitis B burden Global Prevalence of chronic HBV CDC 2006 Chronic Hepatitis B in Australia Low prevalence (<2%), but high in some populations: Eg. People from China & Vietnam; sub-Saharan Africa & Indigenous Australians ~ 50-65% of chronic HBV (in Aus) – in people born in Asia ~ 160,000 Australians have chronic HBV (Gidding 2007) ~ 45,000 people with chronic HBV in Victoria ~1500-2000 new cases notified in Victoria each year (Cowie 2008) Transmission of HBV Percutaneous or mucosal exposure to: infected blood & body fluids Semen, vaginal secretions, saliva & breast milk* Mother to child Globally – perinatal transmission is most common *HBIG & vaccine should eliminate theoretical risk of acquisition through breast feeding Foetal scalp monitoring should NOT be used No evidence that mode of delivery (vaginal or caesarean) affects risk of infection CHB - Who Should Be Screened? GESA Chronic Hepatitis B Recommendations 2008 HIGH risk populations Any person born in/parents born in an endemic country Indigenous populations IDU’s (previous or current) Household/sexual contacts of HBsAg positive person History of HCV or HIV All pt’s undergoing chemo/immuno-suppressive therapy Those on renal dialysis Antenatal screen for ALL pregnant ♀ (RANZCOG) Pre & Post test discussion Natural History of HBV Acquired at Birth Digestive Health Foundation 2000 HBV DNA ( pg/mL) CHRONIC HEPATITIS CIRRHOSIS (30%) HCC ALT HBeAg + + + + + + + ++ + --------------- Clearance phase ALT normal range 10 Immune tolerant Replicative phase 20 AGE (years) 30 40 Immune escape Immune control Immune clearance ReactivationImmuno-active phase Low replicative phase Pre-core mutant Diagnosis & Treatment Mum: HBV Serology & LFT’s Infant: If mum HBV+ HBV serology & LFT’s – at 2-6 mnths S100 medications - Currently Liver biopsy required Pegylated interferon (weekly injection)–**side effects** Antiviral medication – (tablets) Long term – usually well tolerated, viral resistance is possible Mum – Preferably NOT treated during pregnancy but may be if high viral load – resistance is an issue Infant – Not usually treated due to disease phase, viral resistance , need for further research in children Vaccination Advised for ALL people at risk of contact with blood or body fluids Funded for some groups – encourage IDU’s Can ↓ perinatal transmission risk from 90% to 5% if HBIG (12hrs) &1st HB vaccination (24hrs no > 7 days) (when mum has active HBV markers - HBsAg + and HBeAg) Adult – 3 injections – Now, 1 & 5 months later Infants – 4 injections – birth, 2, 4 6 (or 12 months) Hepatitis C at a glance ~ 170 million people chronically infected globally (3-4 million new infections each year) WHO ~ 284,000 Australians infected with HCV ~ 211,700 people chronically infected (~ 17,444 people are living with HIV) NCHECR 2009 NO VACCINE – However treatment is available & CURE is possible A leading cause of liver transplant in Australia NCHECR 2008 Slow acting virus – often asymptomatic Prevalence of Hepatitis C infection 6 Genotypes >10% 2.5–10% 1–2.5% WHO. Wkly Epidemiol Rec 2002; 77: 41 Transmission of HCV - Blood to blood Risk Factors Sharing injecting equipment Recipient of blood products < 1990 History of incarceration Unsafe tatooing & body piercing (traditional practices) Place of birth – mass vaccination programs Sharing of blood contaminated household items Mother to child - 5% risk - Foetal scalp NOT to be used No - Mode of delivery – no affect on risk - Breastfeeding OK except if nipples cracked Natural history of hepatitis C Potential outcomes Approximately 1 of every 4 people (25%) who contract hepatitis C will clear their infection naturally within the first 6-12 months. The remaining 3 out of 4 people (75%) will develop chronic hepatitis C. Of 100 people with chronic hepatitis C who remain untreated: 45 may not develop liver After 20 years damage 47 may develop mild to moderate liver damage 45 may not After 40 years develop liver damage 31 may develop mild to moderate liver damage 7 may develop cirrhosis of the liver 20 may develop cirrhosis of the liver 1 may develop liver failure or liver cancer 4 may develop liver cancer or liver failure Hepatitis C is a highly stigmatised condition Support from health professionals is important Disclosure In most situations there is no legal obligation to disclose Examples of discrimination & lack of knowledge: Mum wearing ‘colored’ arm band & baby’s cot labelled ‘universal precautions’ Labelling expressed breast milk “Hepatitis C” Education is key Diagnosis Antenatal screen for recommended in pregnant ♀ (RANZCOG) Pre & Post test discussion Mum: HCV serology (Ab’s + Virus) & LFT’s Infant: Counselling – Implications of testing Can check for virus with PCR test > 2 months Can check Ab’s > 18mnths due to maternal If Mum positive for virus – refer to liver clinic If infant positive – refer to paediatric gastroenterologist Treatment S100 Medications - NOT during pregnancy or breast feeding Pegylated Interferon - weekly S/C injection **side effects** Ribavirin = tablets BD - teratogenic – contraception! Infants not usually treated – some children - compassionately Aim: Sustained Virological Response (SVR) 100% - undetected virus 80% - > 6 months = CURE 60% 40% 80% 24 weeks 50% 48 weeks 20% 0% Genotype 1 Genotype 2/3 How can you help? Educate Transmission & prevention (including vaccination) Tests available Treatments available to control (HBV) & cure (HCV) Importance of monitoring for possible liver damage & HCC Refer To GP for screening/testing – refer on to specialists For ongoing monitoring for liver damage & HCC For counselling – mental health, drug & alcohol services Thank you Any questions or comments? Education and Support Services Victorian Viral Hepatitis Educator Information for Health Professionals 0407 865 140 or 9288 3586 [email protected] Hepatitis C Victoria Ph: 9380 4644 InfoLine 1800 703 003 Refer to Commonwealth Infection Control Guidelines (ICG) The Australian Immunisation Handbook Key Documents B Positive: all you wanted to know about hepatitis B – A guide for primary care providers (2008) Produced & funded by: ASHM & The Cancer Council NSW C Change - Report of the enquiry into hepatitis C related discrimination Anti-discrimination board of NSW 2001 Giles, M.L, Pedrana, A, Jones, C, Garland, S., Hellard, M. and Lewin, S.R. ‘Antenatal screening practice for infectious diseases by general practitioners in Australia’ Australian and New Zealand Journal of Obstetrics and Gynaecology 2009, 49, 39-44 Hepatitis viruses and the newborn: Clinical manifestations and treatment, http://www.uptodate.com Uptodate January 2009 – American Continued Medical Education Program – Royal College Association of Physicians HIV, Viral hepatitis and STI’s – A guide for primary care ASHM 2008 HIV/Aids, Viral Hepatitis and Sexually Transmissible Infections in Australian Annual Surveillance Report NCHECR 2008 Key Documents Impact – Information about Heptatits C 5th Ed. Hepatitis Victoria 2008 National Hepatitis C Resource Manual 2nd Ed. Dept. of Health & Ageing 2008 Overview of hepatitis B virus infection in children Uptodate January 2009 – American Continued Medical Education Program – Royal College Association of PhysiciansVictorian Infectious Diseases Bulletin 11 (3) Sep 2008 DHS Victoria Temple-Smith, M., Jenkinson, K., Lavey, J., Gifford, SM & Morgan, M. Discrimination or discretion? Explorying dentists’ views on treating patients with hepatitis C Australian Dental Journal 2006 51 (4) 918-929 Wiseman, E., Fraser, MA, Holden, S, Glass, A, Kidson, BL, Heron, LG, Maley, MW, Ayres, A, Locarnini, SA, Levy, MT Perinatal transmission of hepatitis B virus: An Australian Experience MJA ‘Research’ 2009 190: 489-492 Wallace, J., McNally, S., & Richmond, J. (2007) National Hepatitis B Needs Assessment ARCSHS Latrobe University Hepatitis Treatment Centres •Geelong Liver Clinic •Maroondah Hospital Bayside Hepatitis Clinic (Cheltenham) •Monash Medical Centre - Clayton Aubury / Wodonga – by appt - Springvale Liver Clinic Austin Hospital - Cranbourne Liver Clinic Ballarat Liver Clinic • Northern Hosp. Liver Clinic Bairnsdale Hospital • Royal Melbourne Hospital Bayside Gastroenterology (Frankston) • St. Vincent’s Hospital Bendigo Health Infectious Diseases •St. Kilda – First Step Liver Clinic • Warrnambool – Western Region Box Hill Hospital Alcohol and Drug (WRAD) centre Fitzroy – Inner Space • Werribee Hepatitis Clinic Footscray – Western Hospital Frankston – Peninsula Liver Clinic Alfred Hospital - Prahran Frances Cieslak Victorian Viral Hepatitis Educator