* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Antibiotic-Associated Diarrhea/C. difficile Colitis
Public health genomics wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Dental emergency wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Antimicrobial resistance wikipedia , lookup
Antibiotic use in livestock wikipedia , lookup
Focal infection theory wikipedia , lookup
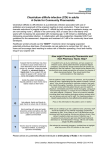
January 2016 Antibiotic-Associated Diarrhea/C. difficile Colitis Paul Feuerstadt, MD and Randy Johnson PA-C Antibiotic-associated diarrhea What is antibiotic-associated diarrhea? Antibiotic-associated diarrhea describes an increase in the frequency of bowel movements and/or watery bowel movements that occurs as a result of antibiotic therapy used to treat bacterial infections anywhere in the body. Generally, this is a benign, selflimited diarrhea caused by changes to the composition and function of intestinal flora; the constellation of microorganisms that live in your intestinal tract. What are the symptoms of antibiotic-associated diarrhea? The symptoms of antibioticassociated diarrhea includes loose stools with or without increased bowel movement frequency. The changes in bowel habits can happen rapidly, even after one dose, though most commonly occurs five to ten days after starting antibiotics. Some individuals can have a “delayed onset” which can occur up to 8 weeks after the initial antibiotic exposure. Though most patients will have a mild form, some might develop severe antibiotic-associated diarrhea characterized by frequent watery diarrhea, fever, blood in stool, pus in stool, abdominal pain and cramping. One should contact their doctor if they have any of these signs of severe symptoms as it may represent something more serious. How do antibiotics cause antibiotic-associated diarrhea? Antibiotics are used to treat infections caused by harmful bacteria and choice of antibiotics varies depending on the location and severity of the infection as well as the cause. While a specific antibiotic works to treat the underlying disease (e.g. urinary tract infection, pneumonia, sinus infection, skin infections, etc) it may also affect the balance, composition, and function of the intestinal flora. When the good bacteria are inadvertently suppressed by the antibiotics, the bad bacteria can overgrow causing the changes in bowel habits and diarrhea. Which antibiotics most commonly cause Antibiotic-associated diarrhea? • Cephalosporins, including cefixime (Suprax), Ceftriaxone (Rocephin), and cefpodoxime (Vantin) • Clindamycin (Cleocin) • Erythromycin (Erythrocin, E.E.S., others) • Penicillin Drugs, such as amoxicillin (Larotid, Moxatag, others) and ampicillin • Quinolones including ciprofloxacin (Cipro) and levofloxacin (Levaquin) • Tetracyclines, such as doxycycline (Vibramycin, Periostat, others) and minocycline (Minocin, Solodyn, others) What characteristics place a patient at risk for antibiotic-associated diarrhea? • Any previous episode of antibioticassociated diarrhea • Age greater than 80 • Female gender • Antacid use/Proton pump inhibitor use Some individuals can have a “delayed onset” which can occur up to 8 weeks after the initial antibiotic exposure. . • Recent or extended (> 7 days) stay at a hospital or skilled nursing facility • Recent surgery on the digestive tract • Severe underlying disease of the digestive system (e.g. colon cancer, inflammatory bowel disease) How do we diagnose antibioticassociated diarrhea? If symptoms are mild the medical practitioner might be able to diagnose this disease by asking questions and taking a history alone. If symp- toms are severe the medical practitioner might obtain a stool sample and/or bloodwork to evaluate for a more serious condition and assess for severity of the process. What are common treatments of antibiotic-associated diarrhea? Treatment will depend on the severity of the illness and this should only be assessed by a medical practitioner. Mild symptoms will usually resolve within a couple of days following completion of antibiotic treatment. In mild cases home remedies such as drinking plenty of fluids, eating soft, easy to digest foods (e.g. bananas, rice, applesauce), and avoiding irritating foods (e.g. fatty, spicy or fried foods) can help to alleviate the symptoms. In more severe cases the medical practitioner might advise stopping the antibiotic. In addition, recent studies have shown that the probiotics, healthy bacterial supplements, such as S. boulardii (Florastor), Lactobaccilus (Culturelle) and Bifidobacterium (Align), if given with antibiotics, can reduce the risk of the onset or severity of the diarrhea. Patients should always consult their medical provider before considering taking medications that constipate (e.g., loperamide [Imodium A-D]) since these medications can hinder the body’s ability to eliminate the infection and lead to more serious complications. C. Difficile Infection: A specific type of Antibiotic-Associated Diarrhea What is C. difficile Infection? C. difficile infection is a common and more severe type of antibiotic-associated diarrhea. It is estimated that approximately one-third of cases of antibiotic- associated diarrhea are caused by C. difficile. C. difficile is a bacterium that is most commonly acquired in the hospital or skilled nursing facility setting. Some individuals who develop this infection might have had no exposure to medical facilities or medical care at all. Treatment will depend on the severity of the illness and this should only be assessed by a medical practitioner. • Poor hand hygiene (e.g., not washing hands with soap and water) • Having a roommate or someone in the same home/living environment who has the infection • Living in a skilled nursing facility or spending an extended amount of time in a hospital How is C. difficile infection diagnosed? C. difficile infection is diagnosed by stool studies that are obtained by your physician. The study usually takes less than 24 hours to obtain results and if positive, therapy should be started immediately. How does C. difficile cause diarrhea? How is C. difficile infection treated? Following acquisition of the C. difficile bacterium, patients might be exposed to specific antibiotics for various reasons which then alter the delicate balance of bacteria in the colon allowing the C. difficile infection to proliferate. This causes C. difficile colitis or “Pseudomembranous colitis.” Most patients who acquire C. difficile infection will have been exposed to antibiotics within 1-3 months of the start of their symptoms, although some may have not received antibiotics at all. C. difficile infection is treated with antibiotics including metronidazole (Flagyl), vancomycin (Vancocin) or fidaxomicin (Dificid). The choice of antibiotics is based upon the severity of illness and should be discussed with your health care providers. One of the challenges with this infection is recurrence after the infection is treated and thought to be cleared from a patient. Although studies have shown mixed results it is believed that the probiotic S. boulardii (Florastor) might prevent C. difficile infection if given with antibiotics and reduce repeat infections if given at the same time as the primary treatment of C. difficile. If several recurrences occur, then a fecal microbiota transplantation should be considered for more definitive therapy. What characteristics leave a patient at risk for C. difficile-associated diarrhea? • Age> 65 • Woman • Any immune weakening including chronic kidney disease, solid organ transplant, diabetes mellitus, HIV infection • Any antibiotic exposure • Chronic usage of proton pump inhibitors • Chronic usage of narcotics • Any gastrointestinal surgery What is fecal microbiota transplantation (FMT)? FMT is a procedure where stool from a healthy donor is transferred to the colon of an individual suffering from a disease that is known to respond to this. In C. difficile infection, it is known that alterations to the bacteria in the colon are a significant risk factor for acquisition of the infection. Studies have shown that by replacing the bacteria in the colon of a patient with C. difficile infection, we are able to treat those who have had multiple repeat episodes that were previously unable to be cured with antibiotics alone. This treatment is typically only considered for patients who have had at least 2 recurrences or 3 total episodes of the infection. Our center is one of the only centers in the state of Connecticut who is currently performing this sometimes life-saving procedure. Summary Antibiotic-associated diarrhea is, generally, a benign, self-limited diarrhea caused by changes to the composition and function of intestinal flora by an- tibiotics. It is treated with supportive measures and probiotics most of time. Sometimes, a more severe form called C. difficile is present which requires treatment by a medical provider.