* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download development
Cell culture wikipedia , lookup
Embryonic stem cell wikipedia , lookup
Cellular differentiation wikipedia , lookup
Dictyostelium discoideum wikipedia , lookup
Regional differentiation wikipedia , lookup
Regeneration in humans wikipedia , lookup
Cell theory wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Somatic cell nuclear transfer wikipedia , lookup
State switching wikipedia , lookup
Drosophila melanogaster wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Fertilisation wikipedia , lookup
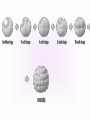
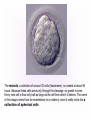
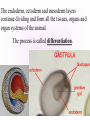
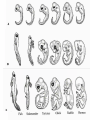
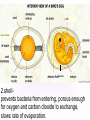
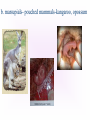
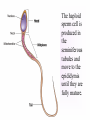
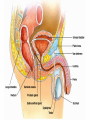
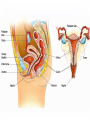
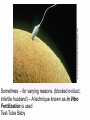
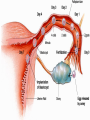
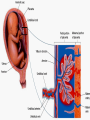
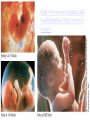
KEY QUESTIONS FOR THIS UNIT What effects do estrogens and testosterone have on males and females? What are the main functions of the male reproductive system? What are the main functions of the female reproductive system? What are some of the most common STDs? What takes place during fertilization and early human development? What important events occur during the later stages of human development? After fertilization, embryonic development in animals begins. It follows a well-defined pattern of growth and differentiation. It is controlled – most part – by genes – the hereditary material from the parent cells. In some animals, development is external. Yet, in others – like humans – it occurs within the body of a parent. After fertilization of an egg, the zygote is formed. This is the first in a series of complex events that conclude with the birth of a full-grown organism. Following fertilization, the zygote begins a series of mitotic cell divisions know as cleavage. Cleavage- Cells don't grow, just divide; therefore, cell size decreases 1. Series of cell divisions after fertilization 2. Mitosis 3. Embryo-development of the zygote (one cell) Stages of Cleavage- the number of cells doubles at each division but no growth occurs. 1. Morula-developing embryo is solid ball of cells 2. Blastula-development of hollow center filled with fluid-blastocoel 3. Gastrulation-"horse shoe stage" when blastula reaches several hundred cells 1. Morula-developing embryo is solid ball of cells The process begins when the zygote divides into two identical cells by mitosis. The two cells then divide into four smaller cells, which in turn divide into eight smaller cells. This process continues and a solid ball of cells called the morula is formed. Zygote (approximately 16-20 hours after insemination) Four-cell embryo (approximately 45 hours after insemination). Two-cell embryo (approximately 24 hours after insemination). Eight-cell embryo (approximately 72 hours after insemination). The morula, a collection of around 30 cells (blastomere), is created at about 96 hours. Because these cells arise only through the cleavage, no growth is seen. Every new cell is thus only half as large as the cell from which it derives. The name of this stage comes from its resemblance to a mulberry, since it really looks like a collection of spherical cells Blastula-development of hollow center filled with fluidblastocoel On the 4th day after insemination an epithelial cellular layer forms, thicker towards the outside, and its cells flatten out and become smaller. Fluid filled inside sphere Yolk filled end opening The blastula stage is followed by the formation of the gastrula. During the formation of the gastrula, one side of the blastula pushes inward forming a second, inner, layer of cells. The inner cell layer is called the endoderm. The outer cell layer is called the ectoderm. A third cell layer, the mesoderm, then forms between the endoderm and ectoderm. The endoderm, ectoderm and mesoderm layers continue dividing and form all the tissues, organs and organ systems of the animal. The process is called differentiation. Growth and Differentiation 1.Differentiation-series of changes that transforms the unspecialized embryonic cells into specialized cells, tissues, and organs 2. Growth-increasing number of cells Ectoderm Nervous system, epidermis, sweat glands, hair and nails, lining of mouth, nostrils and anus Mesoderm Bones & muscles, blood, blood vessels & heart, reproductive and excretory systems, inner layer of skin Endoderm Lining of the digestive tract, lining of the trachea, bronchi and lungs, liver & pancreas, thyroid, parathyroid, and thymus, urinary bladder https://www.youtube.com/watch?v=k_9MTZgAhv0 Control of Development A. Nucleus 1. DNA-contains hereditary information. a. Controls cellular activity b. encodes for the production of cellular proteins B. Cytoplasm -receives instructions from the DNA in the nucleus. Which came first? https://www.youtube.com/watch?v=1a8pI65emDE DEVELOPMENT A. External in water 1. Nourishment is supplied by the yolk stored in the egg 2. No parental care B. External on land- production of egg and shell, some parental care 1. Extra embryonic membranes- 4 membranes outside of the embryo a. Chorion-outermost membrane-aids in gas exchange b.allantois-exchange of oxygen and carbon dioxide, stores wastes until egg hatches c. amnion-fluid filled sac that surrounds the embryo cushion, shock absorber d. yolk sac- surrounds the yolk- source of food for embryo Example of organism-lizards, birds, and snakes yolk (Part of white) chorion 2.shellprevents bacteria from entering, porous enough for oxygen and carbon dioxide to exchange, slows rate of evaporation. C. Internal Development 1. Placental mammals-blood vessels of embryo are in close contact with the mother's blood a. Placenta-structure produced by the uterus of the mother, which supplies nutrients to the embryo and removes wastes from the embryo. ** Gas & food exchange is accomplished between the mother and the embryo by diffusion and active transport through the placenta. No direct blood link exists between the mother and the fetus. b. Umbilical cord-attaches the embryo to the placenta of the mother in the uterus 2. Non placental mammals- 2 types a. egg laying mammals (monotremes) -duckbill platypus, spiny anteater b. marsupials- pouched mammals-kangaroo, opossum Aging: complex series of developmental changes which occur with the passage of time -- caused by both heredity & environment Death: irreversible cessation (end) of all brain functions Reproduction is the formation of new individuals The reproductive system could be thought of as the single most important system for the continuation of a species—without it, no species could produce another generation In humans, as in other vertebrates, the reproductive system produces, stores, and releases specialized sex cells known as gametes. These cells are released in ways that make possible the fusion of sperm and egg to form a zygote, the single cell from which all cells of the human body develop For the first six weeks of development, human male and female embryos are identical in appearance. Then, during the seventh week, major changes occur. The primary reproductive organs—the testes in males and the ovaries in females—begin to develop. The testes produce testosterone, a male sex hormone. Testosterone is required for sperm production and the development of male physical characteristics. The ovaries produce the female sex hormones estrogen and progesterone. Estrogen is required for the development of eggs and for the formation of female physical characteristics. Progesterone prepares the uterus for the arrival of a developing embryo Female Secondary Male Secondary Sex Characteristics Sex Characteristics •Development of breasts •Growth of beard and body hair •Changes in body form •Growth of body hair •Changes in body form •Lowered voice pitch The Male Reproductive System The main structures of the male reproductive system are the testes, the epididymis, the vas deferens, the urethra, and the penis. These structures work together to produce and deliver sperm. 1. Testes: make and store sperm Just before birth (and sometimes just after) the testes descend through a canal into an external sac called the (scrotum) -- saclike pouch which houses the testes, is 1-2 degrees Celsius below normal body temperature 2. Within each testis, are hundreds of tiny tubules called seminiferous tubules: carries/stores sperm from the testes 3. Epididymis: temporary storage organ for sperm at the beginning of the Vas Deferens The haploid sperm cell is produced in the seminiferous tubules and move to the epididymis until they are fully mature. 4. Vas Deferens: tube which carries the sperm past 3 lubricating glands 5. Cowper's gland, Seminal vesicle, prostate gland: -- 3 lubricating glands -- prostate produces an alkaline fluid which neutralizes the urine in the urethra -- prostate cancer kills many over 70 males -- treated with radiation and estrogen 6. Urethra: opening through the penis 7. Penis: releases the semen SEMEN: liquid loaded with sperms EJACULATION: Sperm are ejected from the penis by the contractions of smooth muscles lining the glands in the reproductive tract.the release of semen Note: because ejaculation is regulated by the autonomic nervous system, it is not completely voluntary. About 2 to 6 milliliters of semen, containing more than 200 to 600 million sperm, are released in an average ejaculation. Puberty in females starts when the hypothalamus signals the pituitary gland to release FSH and LH. FSH stimulates cells within the ovaries to produce estrogen, the female steroid sex hormone. Interactions of estrogen with target cells produce female secondary sex characteristics. Female Reproductive System The main structures of the female reproductive system are the: ovaries Fallopian tubes uterus vagina. In addition to producing eggs, the female reproductive system prepares the female’s body to nourish a developing embryo A. Ovaries - female gonads 1. Each ovary contains about 400,000 follicles (tiny egg sacs), which contain an immature egg Although a female is born with about 400,000 immature eggs (primary follicles)—and does not produce any new eggs during her lifetime—only about 400 eggs will actually be released. Roughly once a month, under the influence of FSH, a follicle gets larger and the egg passes through the early stages of meiosis. When meiosis is complete, a single large haploid egg and three smaller cells called polar bodies will be produced. The polar bodies have very little cytoplasm and soon disintegrate. 2. Ovaries also secrete estrogen (hormones) responsible for secondary sex characteristics 1. Site for fertilization B. Fallopian tubes or Oviduct - leads from each ovary (neither in contact) When a follicle has completely matured, its egg is released in a process called ovulation. The follicle breaks open, and the egg is swept from the surface of the ovary into the opening of one of the two Fallopian tubes. 2. Eggs are not motile; they get pushed along the fallopian tube by cilia C. Uterus or Womb - site where the egg implants it's self if fertilized After a few days, the egg passes from the Fallopian tube into the cavity of an organ known as the uterus. The lining of the uterus is ready to receive a fertilized egg, if fertilization has occurred. The outer end of the uterus is called the cervix. D. Vagina - birth canal, leads to the outside of the body IMPLANTATION, DEVELOPMENT If an egg is to become fertilized, sperm must be present in the Fallopian tube. Sperm swim actively through the uterus into the Fallopian tubes. FYI: Although hundreds of millions of sperm are released during an ejaculation, only about one percent will reach the upper region of each Fallopian tube. If the egg and sperm meet in the Fallopian tube, the egg and sperm cell may fuse. The fusion of the sperm nucleus and egg cell nucleus is fertilization. Fertilization occurs in the upper portion of the oviduct (Fallopian Tube) The fertilized egg is known a a zygote (a newly formed diploid cell) If the egg is not fertilized within about 24 hours after ovulation, it breaks down and passes through the uterus, through the vagina in a process known as menstruation.. Sometimes - for varying reasons (blocked oviduct, infertile husband) – A technique known as in Vitro Fertilization is used Test-Tube Baby Cleavage of the zygote begins while the fertilized egg is still in the oviduct – about 36 hrs. after fertilization. Division continues & four days after fertilization, the embryo is a solid ball of about 50 cells called a morula Cells rearrange and about six or seven days after fertilization, the blastocyst attaches itself to the wall of the uterus. The embryo secretes enzymes that digest a path into the soft tissue. This process is known as implantation. This is the first phase of pregnancy The second phase – gastrulation and formation – is about 2 weeks after fertilization. The marks the actual beginning of pregnancy. Keep in mind events leading up to birth are sequential and follow a definite timeline. If the embryo implants somewhere other than the uterus – i.e.: oviduct, ovaries, cervix - this is termed an ectopic pregnancy Third Phase - Embryonic Period Period of primary organ differentiation Ends at about the 8th week Last phase – a.k.a. Fetal Period Characterized by rapid growth, changes in body parts & the final preparation for birth By the end of the third week of development, the nervous and digestive systems have begun to form. The chorion has grown into the uterine tissue to form a vital organ called the placenta. The placenta is the connection between mother and developing embryo. The developing embryo needs a supply of nutrients and oxygen. It also needs a means of eliminating carbon dioxide and other metabolic wastes. The Placenta also acts as a barrier for most microorganisms. However, certain viruses AIDS German measles chicken pox encephalitis Can pass through http://www.med.upenn.edu/ meded/public/berp/overvie w.mov Birth – Human gestation period is ~ 9 months (length of pregnancy . Development does not end but continues until death Aging is the term that is applied to the developmental changes that occur in an organism from birth until death. The causes of aging are not fully understood. It appears that aging involves both hereditary and environmental factors. 1. Multiple Birth. a. Identical - formed when 1 egg is fertilized and splits during the first division. b. Fraternal - formed when 2 eggs are fertilized at the same time The Human Menstrual Cycle A mature egg develops & is released approximately 28 days There are 4 stages to the menstrual cycle: 1. Follicle Stage - FHS (follicle stimulating hormone) secreted by pituitary causes follicles to develop in the ovaries. As follicle develops, it releases estrogen, which stimulates the uterine lining to thicken with blood (10-14 days). 2. Ovulation - FHS decreases, LH (lutenizing hormone) from the pituitary gland increases which causes a mature egg to release from the follicle & from the ovary. Occurs in the middle of the cycle (14 day). 3. Corpus Luteum Stage (yellow body stage) After ovulation the follicle fills with cells forming the corpus luteum. Corpus luteum secretes progesterone that maintains the continued growth of the uterine lining. 4. Menstruation - if fertilization does not occur, secretion of the LH decreases & the corpus luteum breaks down. Progesterone levels decrease & the lining of the uterus breaks down & is given off. Lasts 3-5 days. Menopause - The permanent cessation of the menstrual cycle that occurs approximately between 45-50 years of age. The menstrual cycle is regulated by something called a negative feedback mechanism. In its simplest terms, in a negative feedback mechanism, the level of one hormone in the blood stimulates or inhibits the production of another hormone. Some important human reproductive disorders: •Sexually Transmitted Disease (STD) Ex.: syphilis, gonorrhea, genital herpes, AIDS o http://www.cdc.gov/std/ o http://www.plannedparenthood.org/healthtopics/stds-hiv-safer-sex-101.htm o http://www.webmd.com/sexualconditions/default.htm •Epidemic in some geographic areas •May be transmitted by both males and females •Can cause sterility or death if not treated •Early treatment leads to recovery Prostate Enlargement – enlargement of prostate gland – common in males over 40 Breast Cancer – cancerous growth in both male in female breast tissue. Major cause of death in women 25 – 45 year old. Early detection and treatment very important in identifying and curing. \\hvfile1.harpursville.ad.southcentralric.org\staff$\JFrechette\My Documents\a.BIOLOGY 2012-2013\POWER POINTS\HUMAN REPRODUCTION\US Breast Cancer Stats 2011 to 2012.pdf Cervical Cancer - caused by several types of a virus called human papillomaviruses (HPV) •spreads through sexual contact •sometimes the virus leads to cancer •At higher risk if you smoke, have many children, use birth control pills for a long time, or have HIV infection. •A vaccine for girls and young women protects against the four types of HPV that cause most cervical cancers http://www.nlm.nih.gov/medlineplus/cervicalcancer. html