* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Immunity to infectious diseases
Gastroenteritis wikipedia , lookup
Social history of viruses wikipedia , lookup
Human microbiota wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Infection control wikipedia , lookup
Bacterial cell structure wikipedia , lookup
Virus quantification wikipedia , lookup
Introduction to viruses wikipedia , lookup
Viral phylodynamics wikipedia , lookup
Neonatal infection wikipedia , lookup
Marine microorganism wikipedia , lookup
Bacterial morphological plasticity wikipedia , lookup
Schistosoma mansoni wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Molecular mimicry wikipedia , lookup
History of virology wikipedia , lookup
Hepatitis B wikipedia , lookup
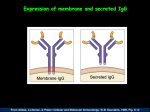
Immunity to infectious diseases. Prof. Mohamed Osman Gad El Rab. College of Medicine& KKUH. Acquired immunity. Classification of immunity. active. natural. artificial. infections. immuniz. passive. natural. artificial. Maternal IgG. immuno therapy. • Immunity to viral infections . • Innate (natural) immunity: many viruses induce : 1. production of type 1 interferons. ( INF- alpha & INF - beta.) 2. activation of NK - cells . dsRNA produced during viral replication induce the expression of interferons by the infected cells. * monocytes , macrophages & fibroblasts also synthesize interferons . Viruses initiate infection by binding to specific host - cell membrane molecules . • e.g. 1. influenza virus bind to cell membrane glycoproteins . 2. rhinoviruses bind to intercellular adhesion molecules (ICAMs). Mechanism of action : • Interferons bind to receptors that activate JAK-STAT pathways. These induce several genes . 1. One gene activate a ribonuclease that degrade viral RNA . 2. Other genes activate protein kinases which inhibit protein synthesis . 3. binding of INFs to NK-cells induce lytic activity . * IL-12 produced by macrophages also enhance NK-cell activity . Antibody- mediated immunity : • Anti-viral antibodies : 1. prevent spread during acute infection. 2. protect against reinfection . Protective functions of antibodies : 1. secretory IgA blocks viral attachment . 2. complement - fixing antibodies may cause lysis of enveloped viruses 3.IgM antibody agglutinate viral particles . Cell – mediated immunity is important for control & clearance of viral infections . CTL activity arises within 3 - 4 days, peak by 7-10 days & then decline when the infection is cleared . Viruses can evade defenses. host 1. Hepatitis C virus : overcome anti - viral effect of INFs blocking the action of protein kinase. 2.Adenoviruses & CMV : reduce surface expression of MHC-1. 3. Measles ,CMV & HIV : reduce MHC -11 levels . 4. A large no. of viruses cause generalized immunosuppression. . e.g. mumps , measles , EBV., CMV., & HIV. Influenza virus . Antigenic variation of influenza virus . • In 1918-1919 an influenza pandemic killed over 20 million people . The structure of the virus contain : Hemagglutinins (HA ). Neuraminidase (NA ). Shifting Nature of Influenza • Antigenic drift – small, ceaseless changes in the genetic structure. New strains continually replace old strains. • • Antigenic shift – major change, usually occurs when species hosting virus trade viral genes. Novel strain appears without natural immunity in host population. 1. Antigenic drift : gradual minor change in HA & NA. 2. Antigenic shift : sudden major change in HA & NA . ( new subtype emerge ) 1918 Hemagglutinin Causes Severe Lung Damage. M88/Hs p M88 Kobasa et al. Nature 2004;431:703 Example: If MHC X was the only type of MHC molecule MHC XX Pathogen that evades MHC X Survival of individual threatened Population threatened with extinction • Immunity to bacterial infections. • If the inoculum (dose ) is small and the virulence of the bacteria is low . Tissue phagocytes may eliminate the bacteria . The humoral response (antibody) is the main protective response against extracellular bacteria . • Antibodies act in several ways : 1. neutralize toxins . 2.activate complement . - generates anaphylatoxins. -release chemotactic agents . Protective functions of antibodies. Intracellular bacteria : • Initially activate NK – cells which provide early defense . Final control is by : cell - mediated immunity . ( this involve activated macrophages ) Cell-mediated immunity involve activated macrophages. Bacteria can by-pass host defense: • 4 steps in bacterial infections : 1. attachment .(adherence). 2. proliferation . 3. invasion of host tissues . 4. toxin - induced damage. Adherence Penetration into the Host Cell Salmonella entering epithelial cells via invasins Figure 15.2 1. Secretory IgA block attachment , but some bacteria secrete proteases that break IgA . 2. Opsonization & phagocytosis prevent proliferation , but some bacterial surface structures inhibit phagocytosis, ( polyssacharide capsule ,Strp.pneum.) Strep.pneumonae. Inhibit phagocytosis. 3. Some bacteria resist complement lysis . 4. Mycobacteria survive intracellularly by resisting oxidative attack ,some prevent lysosomal fusion . Complications of immune responses . In some cases disease is not caused by the bacteria but rather by the immune response. 1. Endotoxins of gram –ve bacteria activate macrophages which release high levels of IL-1, & TNF - alpha, these may cause : Septic shock . 2. In staphylococcal food – poisoning , enterotoxins act as superantigens and cause direct massive T-cell activation . This may cause: Toxic shock syndrome . Endotoxin Contrast the nature and effects of exotoxins and endotoxins. Figure 15.4b Exotoxins Figure 15.4a 3.Complications of streptococcus pyogenes infections throat • 1. Rheumatic fever :antibodies formed against antigen in the strep. cell wall cross –react with the sacrolemma of Human heart .Granuloma form in the heart (Aschoffs nodules). 2. Rheumatic heart disease :repeated attacks by strep. with different M types can result in damage to the heart valves.( certain children have a genetic predisposition to this immune-mediated disease ). ( high A.S.O. titer ). • 3. Acute glomerulonephritis : antibodies to strep . components combine to form immune- complexes which then deposit in the kidney glomeruli . 4. In chronic intracellular infections e.g. T.B. excessive CMI responses lead to granuloma formation . Granuloma formation ( T.B. ) The balance between TH1 & TH2 is important in immunity. It determine the clinical presentation of the disease . 5. Immunological response in leprosy : The response decide the type of disease : 1.In tuberculoid leprosy the patient mount an effective cell-mediated response.Macrophages destroy the bacilli and contain the infection . 2. In lepromatous leprosy : the patient is unable to produce a cell-mediated response and organisms multiply and spread in the tissues > • Immunity to parasitic infections: • A. Protozoal diseases . These are unicellular organisms . e.g. malaria , trypansomiasis , toxoplasma, * They have complex life - cycles. some stages are free in the blood , other stages are intracellular. The type of the immune response depend on the location of the parasite in the host . In the blood antibodies may be effective In the intracellular stage CMI may be effective. Immunity to Malaria: • Caused by genus Plasmodium. • P.falciparum is the most virulent & prevalent. • Infect 10% of the population. • Causes 1 – 2 million deaths every year. • Have a complex life – cycle . Life cycle of malaria : 3-stages. During the life- cycle, many antigens appear : • Infection begin with mosquito bite. • Sporozoites enter the blood & disappear within 30 min. * Migrate to the liver & after 1 week release merozoites which infect RBCs. Sporozoites stay for only 30 min. in the blood, therefore induce a poor immune response. • The intracellular stage in the liver cells and RBC ,reduce the degree of immune activation generated by the pathogen. In endemic areas: • Only 22% of the children have detectable antibodies to sporozoites. • In adults 84% have such antibodies. • In general, the degree of immunity to Malaria is not complete . Trypansomiasis ( sleeping sickness). • As the parasite multiply , an effective antibody response develop to the glycoprotein coat called variant surface glycoprotein (VSG). These antibodies eliminate most of Parasite from the blood by : the 1. complement lysis. 2. opsonization & phagocytosis . Trypansomes, (T. cruz,) However , 1% of the parasite with different antigen (VSG ) escape the antibody response. These proliferate and a new wave of parasites invade the blood . • This is called : antigenic shifts. (a characteristic feature of Trypansomes ). Immunity to parasitic worms (helminths): • Helminths are large multicellular organisms e.g. Schistosoma (Bilharzia ). • Have complex life- cycle . • Cercaria enter the blood stream and become schistosomules which enter capilleries.then pass to the lungs & liver. then become adult worms. Immune responses are not sufficient to eliminate the adult worms . • Adult worms evade immune responses by coating themselves by host glycoproteins . Humoral immune responses to parasites are characterized by : 1. elevated IgE. 2. blood eosinophilia . Eosinophils mediate ADCC to damage the parasite. A chronic state develop in which adult worms persist and induce cell-mediated delayed hypersensitivity reactions This eventually result in the formation of large granulomas . • Immunity to fungi . • Fungal infections of man fall into 4 types: 1.superficial mycoses . 2.subcutaneous mycoses. 3.respiratory mycoses. 4.candida albicans . • Recovery is based on cell-mediated immunity. • There is also evidence for neutrophil involvement In immunity to some respiratory mycoses. Immunology quiz no 4. A. • A12-year old girl has been receiving cytotoxic drugs for Acute leukemia. Although there is evidence that the leukemia is responding, she has become neutropenic ( neutrophils were less than 0.5 x10 ml ) .Early in the evening she was found to have fever, within half an hour she collapsed and was found to have features of sock (tachycardia and hypotention ). Blood was taken for culture which later grew E. coli. She was started on antibiotics and fluid replacement .She gradually improved during the next 12 hours . 1. What is the diagnosis of this patient ? 2. What is the predominant cell involved in this condition ? 2. Describe the underlying immunopathology.? B. • What is the recommended childhood immunization schedule in Saudi Arabia ? What are the indications for passive immunization ? Mention 2 infectious and 1 non-infectious condition for which passive immunization may be required ? Practical points : • Routine tests in microbial serology . 1. Widal test for diagnosis of typhoid fever. standard tube agglutination test (STA) -patient serum in dilution mixed with salmonella suspension . 2.A.S.O. test. anti- streptolysin O test. -toxin –anti-toxin neutrallization test for diagnosis of streptococcal infections . (patient serum neutralize toxin therefore indicator R.B.C . not lysed ) 3. T.P.H.A.test. • Treponema pallidum hemagglutination test. -for diagnosis of syphilis. Trypansomes,life –cycle.