* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Keratitis - e
West Nile fever wikipedia , lookup
Sarcocystis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Henipavirus wikipedia , lookup
Trichinosis wikipedia , lookup
Gastroenteritis wikipedia , lookup
Leptospirosis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Anaerobic infection wikipedia , lookup
Marburg virus disease wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Hepatitis C wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Herpes simplex wikipedia , lookup
Oesophagostomum wikipedia , lookup
Hepatitis B wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Neonatal infection wikipedia , lookup
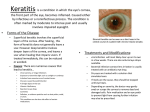
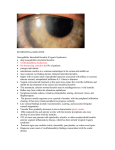
Keratitis Keratitis Classification and external resources An eye with non-ulcerative sterile keratitis. Keratitis is a condition in which the eye's cornea, the front part of the eye, becomes inflamed. The condition is often marked by moderate to intense pain and usually involves impaired eyesight.[1] Types Superficial keratitis involves the superficial layers of the cornea. After healing, this form of keratitis does not generally leave a scar. Deep keratitis involves deeper layers of the cornea, and the natural course leaves a scar upon healing that impairs vision if on or near the visual axis. This can be reduced or avoided with the use of topical corticosteroid eyedrops. Causes Keratitis has multiple causes, one of which is an infection of a present or previous herpes simplex virus secondary to an upper respiratory infection, involving cold sores. Pathogens Amoebic keratitis. Amoebic infection of the cornea is the most serious corneal infection, usually affecting contact lens wearers.[2] It is usually caused by Acanthamoeba. On May 25, 2007, the CDC issued a health advisory due to increased risk of Acanthamoeba keratitis (AK) associated with use of Advanced Medical Optics (AMO) Complete Moisture Plus Multi-Purpose eye solution.[3] Bacterial keratitis. Bacterial infection of the cornea can follow from an injury or from wearing contact lenses. The bacteria involved are Staphylococcus aureus and for contact lens wearers, Pseudomonas aeruginosa. Pseudomonas aeruginosa contains enzymes that can digest the cornea.[4] Fungal keratitis (cf. Fusarium, causing recent incidences of keratitis through the possible vector of Bausch & Lomb ReNu with MoistureLoc contact lens solution) Viral keratitis Herpes simplex keratitis (dendritic keratitis). Viral infection of the cornea is often caused by the herpes simplex virus which frequently leaves what is called a 'dendritic ulcer'. Herpes zoster keratitis Onchocercal keratitis, which follows O. volvulus infection by infected blackfly bite. These blackfly usually dwell near fast-flowing African streams, so the disease is also called "river blindness".[5] Other Exposure keratitis — due to dryness of the cornea caused by incomplete or inadequate eye-lid closure. Photokeratitis — keratitis due to intense ultraviolet radiation exposure (e.g. snow blindness or welder's arc eye.) Ulcerative keratitis Contact lens acute red eye (CLARE) — a non-ulcerative sterile keratitis associated with colonization of Gram-negative bacteria on contact lenses. Severe allergic response may lead to corneal inflammation and ulceration (i.e. vernal keratoconjunctivitis).[6] Feline eosinophilic keratitis — affecting cats and horses; possibly initiated by feline herpesvirus 1 or other viral infection.[7] Diagnosis Effective diagnosis is important in detecting this condition and subsequent treatment as keratitis is sometimes mistaken for an allergic conjunctivitis. Treatment Treatment depends on the cause of the keratitis. Infectious keratitis can progress rapidly, and generally requires urgent antibacterial, antifungal, or antiviral therapy to eliminate the pathogen. Treatment is usually carried out by an ophthalmologist and can involve prescription eye medications, systemic medication, or even intravenous therapy. It is inadvisable to use over-the-counter eye drops as they are typically not helpful in treating infections, also using them could delay correct treatment, increasing the likelihood of sight threatening complications. In addition, contact lens wearers are typically advised to discontinue contact lens wear and replace contaminated contact lenses and contact lens cases. (Contaminated lenses and cases should not be discarded as cultures from these can be used to identify the pathogen). Antibacterial solutions include Quixinex (levofloxacin), Zymar (gatifloxacin), Vigamox (moxifloxacin), Ocuflox (ofloxacin — available generically). Steroid containing medications should not be used for bacterial infections, as they may exacerbate the disease and lead to severe corneal ulceration and corneal perforation. These include Maxitrol (neomycin+polymyxin+dexamethasone — available generically), as well as other steroid medications.. One should consult an ophthalmologist or optometrist for treatment of an eye condition. Some infections may scar the cornea to limit vision. Others may result in perforation of the cornea, (an infection inside the eye), or even loss of the eye. With proper medical attention, infections can usually be successfully treated without long-term visual loss.